|
Research
Comparison of patients with asthma managed in general practice and in
a hospital clinic
Omar A Abdulwadud, Michael J Abramson,
Larry Light, Francis C K Thien
and E Haydn Walters
MJA 1999; 171: 72-75
See also Heard et al & Gibson
Abstract -
Introduction -
Methods -
Results -
Discussion -
Acknowledgements -
References -
Authors' details
-
-
More articles on Respiratory medicine
|
Abstract |
Objectives: To compare knowledge and attitudes
about asthma, self-management skills and impact of asthma on quality
of life between patients managed in general practice (GP) and in a
hospital clinic.
Design: Cross-sectional survey with six months'
follow-up.
Patients and setting: 105 adults with asthma: 61 from the
Alfred Hospital Asthma and Allergy Clinic, Melbourne, and 44 from
nearby general practices, in 1994-1995.
Main outcome measures: Patient sociodemographic and
clinical characteristics; patient knowledge, attitudes and
beliefs about asthma; self-management skills; and impact of asthma
on quality of life.
Results: GP patients were more educated (P = 0.04)
and more likely to smoke (P = 0.04) and to have mild asthma
(P = 0.04) than hospital patients; they were less likely to use
theophylline (P = 0.006) and to have exercise limitation
(P = 0.03), and had fewer previous hospital admissions (P
= 0.01). Impact of asthma on quality of life was greater in the
hospital group than in the GP group. At baseline, the GP group were less
likely to have written asthma action plans (P = 0.018), and
were less able to manage rapid onset attacks than the hospital group
(P = 0.02). More subjects in the hospital group than the GP
group felt their asthma was severe (P = 0.02) and were
optimistic about their asthma improving (P = 0.03). GP
patients increased their knowledge about asthma significantly
(P = 0.002) over six months.
Conclusions: Patients with asthma managed in general
practice and in hospital differ in clinical parameters, quality of
life and attitudes to asthma. Future educational initiatives should
take such differences into account.
|
| | Introduction |
Asthma is the third most common reason for consultations with general
practitioners (GPs) in Australia,1 but is both
under-recognised and undertreated.2 The finding that GPs were the
usual source of routine asthma treatment for 89% of the people who died
of asthma3 demonstrates that GPs have
the primary management role even in severe asthma.4 To guide both doctors and patients, in 1989 the Thoracic Society of
Australia and New Zealand developed the "six-point" Australian
Asthma Management Plan (AMP).5 This was adopted by the
National Asthma Campaign (NAC) at its inception in 1990. While the
Royal Australian College of General Practitioners is a partner in the
NAC, the plan was originally drawn up by hospital-based specialists.
There is concern among GPs that they do not have sufficient time and
knowledge to devise action plans and counsel patients about asthma
management,4 as suggested in the AMP.
The effectiveness of patient education about asthma as proposed in
the AMP has not been widely evaluated in general practice. Only one
such study has been reported,6 and only one nationwide
survey of selected GPs was conducted before the launch of the NAC
intervention.7
We aimed to examine patient knowledge about asthma and its
management, self-management skills, impact of asthma on quality of
life, and attitudes to asthma. We compared these between patients
managed in general practice and in a hospital clinic over a six-month
period that coincided with widespread advertising and
dissemination of the AMP.
|
| |
Methods |
| |
Design and setting | |
The study was a cross-sectional survey with six months' longitudinal
follow-up during 1994-1995. There was no intervention, and patients
received their usual care from their GPs or hospital specialists. The
study was conducted at the Alfred Hospital Asthma and Allergy Clinic,
Melbourne, Victoria, and at 13 general practices near the hospital.
Fourteen GPs were recruited by a practising GP (L L). The study was
approved by the Ethics Review Committee at the Alfred Hospital.
| |
Subjects |
Consecutive patients being seen for asthma at the participating
general practices were nominated by their GPs. Of 54 patients invited
to participate, 44 were recruited (nine refused or did not respond and
one died). Sixty-one patients were recruited from the Alfred Clinic.
Inclusion and exclusion criteria were reported
previously.8 All patients gave written
informed consent. Diagnosis of asthma was based on American Thoracic
Society criteria.9 | |
Assessments |
Clinical and demographic characteristics of patients were
determined by questionnaire. The term "priority asthmatic" was
given to asthmatics who had severe and precipitately acute attacks of
asthma; they had usually (but not necessarily) been admitted to an
intensive care unit. Forced expiratory volume in 1 second
(FEV1) was obtained from the records of the lung function
laboratory, and predicted FEV1 at baseline was
calculated for males and females separately, as suggested by Gibson
et al.10 The mean daily peak
expiratory flow (PEF) variability was estimated from patient
diaries.5 Severity of asthma was
classified as mild, moderate or severe based on medication use, as
reported previously.8 Medication was grouped into
generic categories.
| |
Outcome measures | |
Patients completed the Asthma General Knowledge,11 Quality of
Life,12 Self-Management
Skills,13 and Attitudes and
Beliefs14 questionnaires on entry
and six months later. Selection of these outcomes was based on the
asthma education targets and outcome measures proposed by the
National Asthma Campaign.15 | |
Statistical analysis | |
Data were analysed with the SAS for Windows statistical
package.16 Categorical variables
were summarised as percentages, and associations were tested in
contingency tables by χ2 tests. For continuous
variables that were normally distributed, differences in mean
scores were assessed by Student's t test. For continuous
variables that were not normally distributed, the Wilcoxon signed
rank and rank sum tests were used.
|
| |
Results |
| |
Participation |
Follow-up questionnaires were returned by 39 of the 44 (87%) GP
patients (with five of those with the most severe asthma lost to
follow-up) and by 47 of the 61 (77%) hospital patients (with the
remaining 14 either lost to follow-up or not responding).
| |
Subject characteristics | |
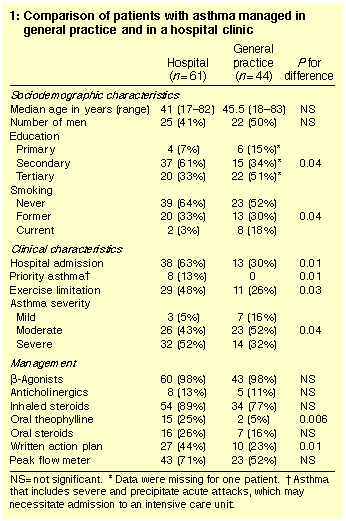
Characteristics of the two patient groups are shown in Box 1. They were
similar in age and sociodemographic characteristics, including
occupation (data not shown), except that the GP group had a
significantly higher proportion of tertiary-educated people and of
current smokers than the hospital group.
GP patients had less exercise limitation and milder asthma than the
hospital patients, and were less likely to have been admitted to
hospital and to have priority asthma. There was no significant
difference in lung function or other clinical parameters (data not
shown).
GP patients were significantly less likely to use theophylline and to
have a written asthma action plan than hospital patients.
Proportions using β-agonists, anticholinergics, and inhaled or
oral steroids and owning peak flow meters were not significantly
different in the two groups.
| |
Asthma outcome measures | |
Asthma knowledge: Asthma General Knowledge scores
did not differ significantly between the GP and hospital groups
either at baseline (means, 20.2 and 20.5 out of 31, respectively) or
six months later. Scores increased in both groups over the six months,
but the increase was significant only in the GP group (P =
0.002), which had a mean score increase of 1.66 (95% confidence
interval [CI], 0.58 to 2.76) compared with 0.83 (95% CI, 20.39 to 2.03)
in the hospital group.
Quality of life: Scores for impact of asthma on
quality of life are shown in Box 2. Impact at baseline was
significantly greater in the hospital group than in the GP group for
total quality of life and the subcategories of breathlessness,
social disruption, and concern for health, but not mood disturbance.
After six months, impact had significantly decreased in the hospital
group for all these parameters except mood disturbance, but there was
no significant change in the GP group. Despite the significant
decrease in the hospital group, impact was still significantly
greater than in the GP group for total quality of life (P =
0.03), social disruption (P = 0.008) and concern for health
(P = 0.04). None of the improvements in quality of life
differed significantly between the two groups over six
months.
Self-management skills: At baseline, the hospital group
had a significantly higher median score for knowledge about
self-management of a rapid onset asthma attack than the GP group
(P = 0.02), but the two groups had similar scores for a slow
onset attack (Box 3). After six months, the hospital group had
significantly improved its slow onset scenario score (P =
0.02), but the GP group had not. Overall, there was no difference in
the median change over six months in scores for either scenario
between the two groups.
Attitudes and beliefs about asthma: Patients' attitudes and
beliefs about their asthma are shown in Box 4. At baseline, hospital
patients were significantly more likely than GP patients to believe
that their asthma was severe, but also that it would improve in the
future. After six months, hospital patients were significantly less
optimistic (P = 0.03), and the difference in this parameter
between the two groups was no longer significant. The proportion of
patients who said they could do everything they wanted regardless of
the effect it might have on their asthma did not differ significantly
between the two groups at baseline, but at follow-up hospital
patients were significantly less likely to say this than GP patients.
More hospital than GP patients wished their doctor would talk more to
them about their asthma at both baseline and six-month follow-up, but
the difference was significant only at follow-up. Concomitantly,
fewer hospital patients than GP patients felt that their doctor had
told them everything they wanted to know about their asthma; the
difference was significant at both baseline and follow-up.
|
| |
Discussion |
We found that our samples of GP and hospital patients with asthma
differed in sociodemographic and clinical parameters, quality of
life, self-management skills and attitudes and knowledge about
asthma.
Some of our findings about the GP sample were more positive than
reported previously. Use of inhaled steroids was significantly
higher than found in random community samples,17,18 possibly
because our sample of GP patients had more severe asthma, or because of
industry promotion of these drugs.18 It is also possible that
this form of treatment has become more acceptable in our group of GPs,
many of whom had a particular interest in asthma. Use of peak flow
meters and prevalence of written action plans in the GP patients were
also higher than previously reported,17,18 but, once again, this
finding may be confounded by the group of GPs studied. Actual
prevalence of peak flow meter use and written action plans may be
substantially lower in more typical general practices.
There was some evidence from our study that implementation of the AMP
may have improved, especially in general practice, over the period of
our study. However, despite NAC recommendations, half of the
hospital patients and three-quarters of the GP patients had no
written asthma action plans; and about a third of the hospital
patients and half of the GP patients did not have access to a peak flow
meter. While our study sheds no light on the reasons for these
findings, it demonstrates that there was room for improvement in
asthma management in both settings, but particularly in general
practice.
Asthma knowledge among the GP patients was similar to that among the
hospital patients at baseline, but improved more over the six months
to follow-up. This was possibly due to the GP patients' higher
educational level, our interaction with them during the study or
better than average care from their doctors. As doctors had recruited
the patients to the study, they may have put more effort into educating
them before follow-up, although we have no evidence for this.
The absence of any significant improvement in quality of life among
the GP patients after six months suggests that insufficient
attention may be given to this aspect of asthma. Furthermore, the
potential selection bias towards milder disease and the loss to
follow-up of five of those with more severe asthma from the GP group may
have biased the results away from detecting improvement. Overall,
the general practice group had better quality of life than the
hospital group. This would be expected, as the GP group had milder
disease with fewer hospital admissions. It is surprising that mood
disturbance was the only category which did not differ between the two
groups at baseline. Possibly moods such as sadness, depression and
frustration are similar in all patients regardless of the severity of
asthma.
At baseline, the GP group was less able to manage the rapid onset
attack, perhaps because they were likely to have experienced fewer
such attacks. The hospital group improved their ability to manage
slow onset attacks significantly over six months. Maybe their
doctors educated them informally, although they did not have access
to the results of the questionnaires. Alternatively, participants
may have improved their answers with practice, but as this did not
happen in the GP group it is unlikely.
There was little difference in attitudes and beliefs about asthma
between groups. However, at six months, the hospital group was
significantly less optimistic about their asthma improving in the
future than the GP group. This could result from the difference in
asthma severity between the two groups, which resulted in hospital
patients having a more realistic appreciation of their poor
prognosis after education. At six months, more of the hospital
patients than GP patients also wished that their doctors would tell
them more about their asthma. Perhaps this reflects a low level of
communication between doctors and patients in the hospital asthma
clinic compared with general practice and requires further study.
This study has some limitations. The GP patients may not be
representative of the total general practice population, and
recruiting interested GPs may have biased results. In the absence of
any viable alternative strategy, evaluation focused on patients
rather than GPs. Despite potential sampling and selection biases,
the results highlight the impact of patient education among patients
attending general practices and the differences between GP and
hospital patients. Future educational initiatives should take such
differences into account. The type and scope of patient education in
general practice and hospitals should be thoroughly evaluated to
identify areas in which GPs and specialists could be trained and
supported more effectively. Continued dissemination and
implementation of the Australian AMP is required to improve the
self-management skills of patients in general practice.
|
Acknowledgements | |
We acknowledge a public health postgraduate research scholarship
from the National Health and Medical Research Council. Dr Andrew
Forbes, Jan Driver and Michael Bailey provided statistical support.
We are grateful to the general practitioners who participated in the
study. Drs Guy Marks, Rae Allen and Bonnie Sibbald gave permission to
use their questionnaires. Dr John Kolbe gave permission to use his
scoring system for the asthma attack scenarios.
|
| |
References |
- Bridges-Webb C, Britt H, Miles DA, et al. Morbidity and treatment in
general practices in Australia 1990-1991. Med J Aust 1992;
157 Suppl: 1-56.
-
Tse M, Cooper C, Bridges-Webb C, Bauman A. Asthma in general
practice. Opportunities for recognition and management. Aust
Fam Phys 1993; 22: 736-741.
-
Robertson CF, Rubinfeld AR, Bowes G. Deaths from asthma in
Victoria: a 12 month survey. Med J Aust 1990; 152: 511-517.
-
Antic R. Asthma in Australia: the current understanding. Overview
of a national series of interactive meetings for general
practitioners. Sydney: Excerpta Medica, 1993.
-
Woolcock A, Rubinfeld AR, Seale JP, et al. Asthma management plan,
1989. Med J Aust 1989; 151: 650-653.
-
Byrne DM, Drury J, Mackay RC, et al. Evaluation of the efficacy of an
instructional program in the self-management of patients with
asthma. J Adv Nursing 1993; 18: 637-646.
-
Tse M, Bauman A, Bridges-Webb C. Asthma management in general
practice. Aust Fam Phys 1991; 20: 1085-1092.
-
Abdulwadud O, Abramson M, Forbes A, et al. Evaluation of a
randomized controlled trial of adult asthma education in a hospital
setting. Thorax 1999; 54: 493-500.
-
American Thoracic Society. Standards for the diagnosis and care of
patients with chronic obstructive pulmonary disease (COPD) and
asthma. Am Rev Respir Dis 1987; 136: 225-244.
-
Gibson J, Gallagher H, Johansen A, Webster I. Lung function in an
Australian population: spirometric standards for non-smoking
adults. Med J Aust 1979; 1: 292-295.
-
Allen RM, Jones MP. The validity and reliability of an asthma
knowledge questionnaire used in the evaluation of a group asthma
education self-management program for adults with asthma. J
Asthma 1998; 35: 537-545.
-
Marks GB, Dunn SM, Woolcock AJ. A scale for the measurement of
quality of life in adults with asthma. J Clin Epidemiol 1992;
45: 461-472.
-
Sibbald B. Patient self care in acute asthma. Thorax 1989;
44: 97-101.
-
Sibbald B, Collier J, D'Souza M. Questionnaire assessment of
patients' attitudes and beliefs about asthma. Fam Pract
1986; 3: 37-40.
-
National Asthma Campaign (NAC) National Asthma Strategy. Goals
and targets. Melbourne: National Asthma Campaign, 1994.
-
SAS Institute Inc. SAS language guide for personal computers, the
SAS system for Microsoft Windows. Release 6.10. Cary, NC: SAS
Institute Inc, 1994.
-
Abramson MJ, Kutin JJ, Rosier MJ, Bowes G. Morbidity, medication
and trigger factors in a community sample of adults with asthma.
Med J Aust 1995; 162: 78-81.
-
Comino EJ, Mitchell CA, Bauman A, et al. Asthma management in
eastern Australia, 1990 and 1993. Med J Aust 1996; 164:
403-406.
(Received 28 Sep 1998, accepted 7 Jun 1999)
|
| | Authors' details |
Department of Epidemiology and Preventive Medicine, Monash Medical
School, The Alfred Hospital, Melbourne, VIC.
Omar A Abdulwadud, PhD, Postdoctoral Fellow;
Michael J
Abramson, PhD, FRACP, Associate Professor.
Department of Allergy and Clinical Immunology, Monash Medical
School, The Alfred Hospital, Melbourne, VIC.
Larry Light, MB BS, Clinical Assistant;
Francis C K Thien,
MD, FRACP, Staff Physician.
Department of Respiratory Medicine, Monash Medical School, The
Alfred Hospital, Melbourne, VIC.
E Haydn Walters, DM, FRACP, Professor, and Director of
Respiratory Medicine.
Reprints: Associate Professor M J Abramson, Department of
Epidemiology and Preventive Medicine, Monash Medical School, The
Alfred Hospital, Prahran, VIC 3181.
Email: Michael.AbramsonATmed.monash.edu.au
|
| |  | | Back to text | |  | | Back to text | | 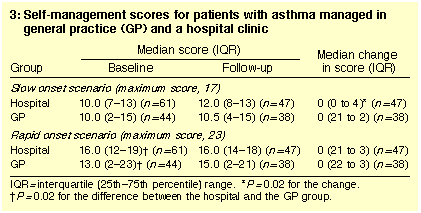 | | Back to text | | 
| | Back to text |
|








