Abstract |
Objective: To determine the prevalence of the
Wernicke-Korsakoff syndrome (WKS) in Australia and compare this
with previous studies. Design and setting: Prospective autopsy study at the New South Wales Institute of Forensic Medicine, 1996-1997. Methods: Brains of deceased people (aged over 15 years) derived from 2212 sequential autopsies performed between 1 January 1996 and 31 December 1997 were studied macroscopically and microscopically to identify cases of WKS. Main outcome measures: Standard histological criteria for WKS and any available clinical data. Results: Twenty-five cases of WKS were identified (prevalence, 1.1%), mostly among the 5.9% of the 2212 people who had a history suggestive of alcohol abuse. Only four cases (16%) had been diagnosed during life. Conclusions: There has been a significant reduction in the prevalence of WKS in Australia since the introduction of thiamine enrichment of bread flour. While the prevalence is still higher than in most other Western countries, further research is needed before adding thiamine to alcoholic beverages can be recommended. |
Introduction |
Wernicke-Korsakoff syndrome (WKS) is a potentially fatal
neurological disorder caused by thiamine (vitamin B1)
deficiency. It is easily treated by thiamine supplementation, with
most people showing dramatic clinical improvement.
Biochemical studies in the 1980s showed that 10%-20% of Australians had a low thiamine intake, with those who used alcohol excessively being particularly "at risk",1 and previous autopsy studies had shown that Australia had the highest recorded prevalence of WKS in the world, with most cases occurring among those who abused alcohol.2-5 To address these problems, the Australian Health Ministers' Council recommended the mandatory enrichment of bread flour with thiamine. Consequently, since 1991 bread flour in Australia has contained not less than 6.4 mg of thiamine per kilogram.6 Human thiamine requirements have been estimated to be 1.0-1.5 mg daily.7 The major food sources of thiamine are cereal products. Although thiamine is naturally present in the grains used to produce flour, much is removed during some types of processing, and thiamine enrichment of flour has been practised in a number of countries for many years.8,9 It is a mandatory requirement in the United Kingdom, Canada, and Denmark, while in the United States enrichment is not mandatory, but most flour is enriched. Since the introduction of thiamine enrichment of rice and flour, thiamine deficiency is said to have virtually disappeared in countries such as Japan and the US.10,11 Our aim was to establish whether this safe and simple public health measure has reduced the prevalence of WKS in Australia, and hence to determine whether we need to consider alternative public health measures such as adding thiamine to all flours used in food preparation or even to alcoholic beverages.12 |
Methods |
We prospectively studied all sequential autopsies of people aged
over 15 years (as WKS is rare in a younger population in Western
countries) from the NSW Institute of Forensic Medicine in Sydney
during 1996 and 1997.
In line with standard autopsy procedures, brains were fixed in 10% formol saline for at least two weeks. After careful external examination and removal of the brainstem and cerebellum, the brain was cut in the coronal plane, the first cut being made at the level of the anterior (ventral) tip of the mammillary bodies. The hemispheres were then cut at 10 mm intervals. The brainstem and cerebellum were separated by dividing the right and left cerebellar peduncles. The cerebellum was sectioned in the sagittal plane through the vermis and through the lateral hemispheres. The brainstem was sectioned in the horizontal plane at 3 mm intervals. The brain slices were examined, paying particular attention to the mammillary bodies and the regions around the third ventricle and the floor of the fourth ventricle. It has been shown that the mammillary bodies are abnormal on microscopic examination in 99%-100% of cases of WKS.3,13 The mammillary bodies were measured in three dimensions and brain slices were photographed if any macroscopic abnormality was noted. Blocks of tissue were taken for paraffin embedding and the preparation of histological sections. The principal block for this study incorporated both of the mammillary bodies and the walls of the third ventricle. Blocks from other regions of the brain were taken according to routine neuropathological protocols of the Institute of Forensic Medicine and the Neuropathology Department.4 These varied depending on the clinical history, cause of death, and general autopsy findings. Sections were cut at 10 mm and stained with haematoxylin and eosin. Brains were stored until each case was completed, so that, if necessary, additional blocks of tissue could be taken for further examination. This was particularly important if an abnormality was identified in the section of the mammillary bodies. A number of other diseases can affect the mammillary bodies, but these can usually be easily differentiated from WKS.5,14 All cases were examined microscopically by a neuropathologist (C H) without knowledge of the relevant clinical history or the macroscopic findings. In all cases in which WKS was suspected, the mammillary body section was also stained with reticulin, Weil myelin, glial fibrillary acidic protein, Perl's iron stain, Bodian silver impregnation, and Nissl stain for neurones. The purposes of these stains are summarised in Box 1. Clinical histories and general pathological data were correlated with the neuropathological findings. Statistical comparisons were made with data from a previous, similar study3 using chisquared statistics with Yates' correction factor and relative risk with 95% confidence intervals. |
Results |
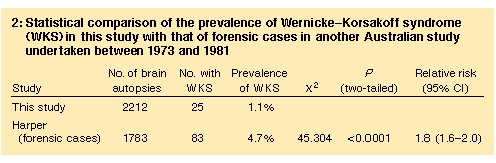
We diagnosed 25 forensic cases of WKS from 2212 brains, giving an
overall prevalence of 1.1%. Box 2 compares the prevalence data with
those of a similar Australian study (including both forensic and
hospital cases of WKS) undertaken by one of the authors (C H) from 1973
to 1981,3 and shows that there
has been a statistically significant reduction in the prevalence of
WKS.
|
 |
|
| The mean age at death of the people with WKS was 55 years; 23 (95%) were
men. Hospital medical records, located for 18 of the 25 deceased
people with WKS, showed that alcohol appeared to have been a
predisposing factor for WKS in 16 (89%). Of the remaining two, one was a
man with paraplegia who was totally dependent and required
gastrostomy feeding, and the other man had both lung and bowel cancer.
Information available at autopsy indicated that 5.9% of the 2212 brains studied were from people with a history which suggested an alcohol problem, giving a prevalence of WKS in an Australian forensic population with a history suggestive of alcohol problems of 19%. A clinical diagnosis of WKS (Korsakoff's psychosis) during life had been made in only four (16%) of the 25 deceased whose WKS was identified at autopsy. However, two others had a diagnosis of alcohol-related brain damage. The hospital records located for 18 deceased people with WKS showed that four had severe amnesia (Korsakoff's psychosis), two others had memory problems and three had ataxia or unsteady gait. None were reported to have ophthalmoplegia or nystagmus, which are commonly described clinical signs in WKS.15 Three had a history of epilepsy. Eight (44%) had been given thiamine (vitamin B1) supplements during one or more of their hospital admissions. The diagnosis of WKS in this study was based on typical pathological abnormalities, which will not be described in detail as this information is available in current neuropathological texts.6 In brief, lesions are seen in a characteristic distribution -- in the mammillary bodies and around the walls of the third and fourth ventricles. Macroscopic findings vary depending on the stage of the disease (see Box 3). There were two acute cases, six acute-on-chronic cases (evidence of both acute and chronic damage to mammillary bodies), and 17 chronic cases. These data are compared with those of a previous study3 in Box 4. | |
Discussion |
Our findings show a significant reduction in the prevalence of WKS in
Australia compared with the findings of a similar study of forensic
cases between 1973 and 1981 (see Box 2).3 The two forensic populations were
similar, even though these two studies were conducted in different
Australian States (New South Wales and Western Australia) and at
different times. Laws relating to deaths which must be reported to the
Coroner and undergo forensic autopsy are almost identical in these
two States. Moreover, one of the authors (J H) was the Director of the
Forensic Department in Perth, WA, at the time of the first study and is
currently the Director of the NSW Institute of Forensic Medicine,
where the current study was carried out; he commented that the
profiles of cases in the two autopsy studies were very similar.
The high prevalence of WKS at autopsy in Australia2-5 has been reflected in clinical studies, with, for example, 170 cases of WKS being identified among 1100 total inpatients at Queensland's largest hospital for the mentally ill.12 However, a retrospective study of records from 17 major Sydney hospitals from 1978 to 1993 showed that the number of acute cases of WKS was lower in 1992 and 1993 than in any of the other years.16 This suggests that dietary enrichment of bread flour with thiamine may have had an impact on the occurrence of acute cases of WKS. Our finding of fewer cases of acute WKS compared with the earlier WA study also supports this (see Box 4, above). As patients with acute WKS who are treated appropriately with parenteral thiamine respond within days, and signs and symptoms usually resolve completely, not all cases will progress to chronic disease. The development of chronic disease is not fully understood, but many chronic cases of WKS are likely to be the result of recurrent episodes of either clinical or subclinical thiamine deficiency.17 WKS is said in the medical textbooks to have a characteristic clinical picture of mental changes (confusion, obtundation), ataxia, and eye signs (nystagmus, ophthalmoplegia). However, as shown in this study and previously, analysis of clinical signs and symptoms of patients diagnosed with WKS post mortem reveals that a minority of cases have the full clinical picture and about a third exhibit only mental changes.15 Thus, the diagnosis can be easily overlooked. Many authors agree that WKS can develop as a result of repeated "subclinical" episodes of thiamine deficiency,18 so that studies of the prevalence of this disorder based on clinical findings are unsatisfactory and may underestimate the true incidence.15 Given that most of the cases of WKS we identified were chronic, some explanation must be sought for the significant reduction in the prevalence of this disease within six years of the introduction of thiamine enrichment of bread flour. There are four possible explanations: 1. A true reduction in the number of new (acute) cases of WKS as a result of the increase in dietary thiamine, and reduced numbers of "at risk" cases. 2. An improvement in the clinical status of patients who already have WKS and a reduced occurrence of further clinical or "subclinical" episodes of thiamine deficiency.17 This could result in an increase in the longevity of patients with existing WKS -- for example, through a reduction in the sudden unexpected deaths seen among chronic alcoholics. 3. A general improvement in the health status of the Australian population, independent of the introduction of thiamine supplementation. 4. Publication of the high prevalence of WKS in Australia may have led to an increased awareness, particularly among health professionals, of the necessity for thiamine treatment in "at risk" patients. Almost half of the 25 people whose WKS was identified at autopsy had been treated with thiamine in hospital. This increased awareness and therapeutic intervention may have played a role in the reduced prevalence. It is likely that each of these explanations played a part in reducing the prevalence of WKS. However, the relative importance of each will only be clarified with time and further study as the enrichment of bread flour with thiamine, has only been in place for six years. It should be noted that the results of this study may in fact underestimate the beneficial effect of the enrichment of bread flour with thiamine as many of the cases of chronic WKS will have developed before the enrichment program commenced. Further prevalence studies should be carried out in, say, another five years, and this information, together with biochemical studies of the thiamine status of the Australian population, will enable rational decisions to be made with regard to other public health programs, such as fortification of alcoholic beverages with thiamine. Our findings neither support nor confirm the prediction of Price and Theodorous that many people who abused alcohol would not be protected by a flour enrichment program because alcoholic beverages are, "for a hazardously long period of their lives, their only form of caloric intake".12 However, they had suggested, on the basis of this prediction, that thiamine supplementation of alcoholic beverages might be a more effective preventive measure, and in reviewing this proposal Connelly and Price noted that fortification of beverages, rather than bread flour, would be more cost-effective by a factor of 20-40-fold.19 Although there has been a significant decrease in the prevalence of WKS in Australia since the introduction of thiamine enrichment of bread flour in 1991, the rate is still higher than in most other Western countries5 and there is a need to maintain vigilance in the management of patients, particularly those with known or suspected alcohol problems. |
Acknowledgements | This research was supported by the Australian Brewers' Foundation and by the National Health and Medical Research Council (Grant number 943302). We are grateful to all the staff at the NSW Institute of Forensic Medicine for their assistance and cooperation. |
References |
(Received 7 Aug1997, accepted 16 Feb 1998) |
Authors' details
Department of Pathology, University of Sydney, and Royal Prince Alfred Hospital, Sydney, NSW.Clive G Harper, MD, FRCPA, Professor;
Donna L Sheedy, BA, Research Assistant;
Ana I Lara, Technical Assistant.
Network for Brain Research into Mental Disorders, Prince of Wales
Hospital, Sydney, NSW.
Therese M Garrick, RN, BNurs, Research Assistant.
New South Wales Institute of Forensic Medicine, Sydney, NSW.
John M Hilton, MB ChB, FRCPA, Director;
Jack
Raisanen, MD, Forensic Neuropathologist.
Reprints: Professor C G Harper, Department of Pathology,
University of Sydney, NSW 2006.
E-mail:
clivehATpathology.su.oz.au
Readers may print a single copy for personal use. No further reproduction or distribution of the articles should proceed without the permission of the publisher. For permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia ".
Received 25 May 2026, accepted 25 May 2026
- Clive G Harper
- Donna L Sheedy
- Ana I Lara
- Therese M Garrick
- John M Hilton
- Jack Raisanen





