Patterns of alternative medicine use by cancer patients
Stephen D Begbie, Zoltan L Kerestes and David R Bell
MJA 1996; 165: 540
For editorial comment, see Lowenthal
Readers may print a single copy for personal use. No further reproduction or distribution of the articles in whole or in part should proceed without the permission of the publisher. For copyright permission, contact the Australasian Medical Publishing Company
Journalists are welcome to write news stories based on what they read here, but should acknowledge their source as "an article published on the Internet by The Medical Journal of Australia <http://www.mja.com.au/>".
Abstract - Introduction - Methods - Results - Experiences of conventional treatment - Alternative treatment - Patient characteristics and alternative therapy use - Discussion - Acknowledgements - References - Authors' details
- - ©MJA1996
Abstract Objective: To assess the patterns of alternative medicine use in patients of a public hospital oncology unit, and to compare patients' experience of alternative with conventional medicine.
Design and setting: Self-administered questionnaire survey of cancer patients attending specialist consulting rooms at the Royal North Shore Hospital and the Oncology Outpatient Clinic at Port Macquarie Base Hospital during August 1995.
Participants: 507 patients attended the clinics; 335 (66%) returned questionnaires, of which 319 (62%) were sufficiently complete for analysis.
Main outcome measures: Expectations of and satisfaction with both conventional and alternative treatment, use of alternative treatment, and patient characteristics associated with this use.
Results: Expectations of and satisfaction with both conventional and alternative treatment were very high. Alternative treatments (most commonly dietary and psychological methods) were used by 21.9% of patients. Median annual cost of alternative therapy was $530, with most patients reporting "value for money". Younger age and being married were positively associated, and satisfaction with conventional treatment was negatively associated, with alternative medicine use; 40% of patients did not discuss alternative medicine with their physician.
Conclusions: A significant proportion of cancer patients use one or more forms of alternative therapy. The use of alternative therapy may reflect on deficiencies in the current standard of care.
MJA 1996; 165: 545-548
Introduction
Rapid developments in the conventional management of cancer have been accompanied by an increased consumer-driven move toward choice and individual control. While alternative (or complementary) medicine has always existed, its availability and variety are growing and its use increasing. 1Cancer patients use alternative therapies despite arguments such as lack of scientific validity, proven ineffectiveness of some treatments and reliance on the placebo effect. It may be helpful for Australian doctors to know the range of alternative therapies used by cancer patients, and to have an understanding of the reasons why they use such therapies, as this may cast some light on deficiencies in the current standard of conventional care.
We aimed to investigate the range of alternative therapies used by cancer patients attending outpatient clinics conducted by a teaching hospital clinical oncology unit, and to assess the level of satisfaction with these therapies and with conventional therapy.
Methods Our subjects were all patients who attended the specialist consulting rooms of three medical oncologists at Royal North Shore Hospital (RNSH) in Sydney, and the Oncology Outpatient Clinic at Port Macquarie Base Hospital (PMBH), New South Wales, during August 1995. Reception staff offered each patient a self-administered questionnaire, with a covering letter from the chief investigator encouraging participation, and assuring confidentiality. Response to the questionnaire was voluntary, and patients were not asked to give explanations for not responding.
The questionnaire sought demographic data, and the following information about their conventional treatment: understanding of diagnosis and treatment, expectations before treatment, impressions at the conclusion of treatment, and overall satisfaction. All questions were multiple choice, with the exception of diagnosis.
Those who had used alternative medicine were asked (in multiple-choice questions, but with space for comments) to outline their reasons for doing so, as well as the treatments chosen. The questionnaire did not seek details of the chosen therapies. The same questions that were used to assess their conventional medicine experience were used to assess their alternative medicine experiences. In addition, they were asked about the reaction of family and friends to their use of alternative therapy, whether they had discussed alternative treatment with their medical oncologist, to estimate the financial cost, and whether they felt they had received value for money.
Data were analysed using the Statistical Package for the Social Sciences 2 to determine associations between patient characteristics and alternative medicine use; significance was measured by the odds ratio. Logistic regression analysis was used to analyse all variables which may affect use of alternative therapy.
Approval for this study was received from the Royal North Shore Hospital Ethics Committee, and from Port Macquarie Base Hospital.
Results Five hundred and seven patients attended, of whom 335 (66%) responded (271 from RNSH, 64 from PMBH). Sixteen questionnaires were excluded from assessment (the alternative medicine question was unanswered in 12, no demographic details were given in 3, and one was returned blank), leaving 319 (62%) to be assessed.
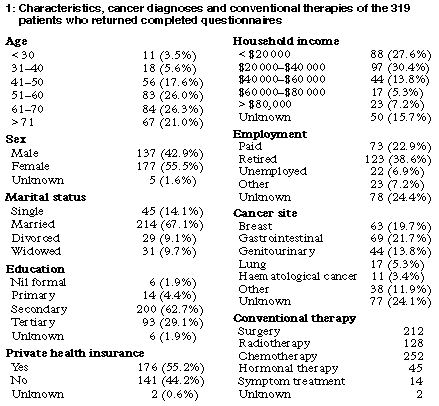
Demographic details for the 319 patients are shown in Box 1. It is noteworthy that in our study women, married people, and those with high levels of education and private health insurance predominate. Only 22.9% of the 319 patients were in paid employment, and median household income was in the $20 000-$40 000 range. A wide variety of diagnoses were represented; breast cancer was the single most common diagnosis.
Experiences of conventional treatment Most respondents had received chemotherapy, and many had undergone other kinds of cancer therapy (Box 1). When asked about their expectations at the beginning of treatment, 85.6% believed that it would cure them or prolong their lives. By contrast, at the end of conventional treatment 63.0% felt that they had been cured or that their life had been prolonged, while 8.2% felt that their treatment had been of no benefit, or had made them worse. Most respondents (75.3%) were either satisfied or very satisfied with their experience of conventional therapy, while only 3.1% were either unsatisfied or very unsatisfied.
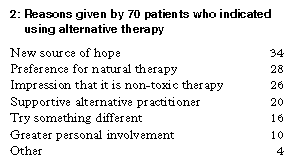
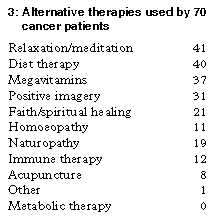
Alternative treatment Seventy patients of the 319 assessed (21.9%) indicated that they were using alternative therapy. The most frequently given reasons were a preference for natural therapy, and seeing the alternative therapy as another source of hope (Box 2). Box 3 shows the alternative therapies chosen; dietary and psychological methods were most prevalent, followed by herbalism. Seventy-five per cent of patients tried more than one therapy (median, 3; range, 1-8).
Most of the patients had learnt of alternative therapies through friend or family recommendation (37; 52.9%), and personal research (32; 45.7%), while doctor's recommendation (11; 15.7%) and media reports (6; 8.6%) were less common (some patients cited more than one source). In addition, family and friends were overwhelmingly supportive, with those of 64 patients (91.4%) being either encouraging or tolerant of the use of alternative therapies.
At the beginning of alternative treatment 51 patients (72.9%) expected it would cure them or prolong their lives, while at the completion 34 (48.6%) felt that they had been cured, or that their lives had been prolonged. Only seven (10%) had the impression that alternative treatment was of no benefit, or had made them worse. Overall, 49 patients (70%) were satisfied or very satisfied with alternative treatment, and only one (1.4%) was unsatisfied.
Forty-five patients gave an estimate of the annual cost of their alternative therapy; the median annual cost was $530 (range, 0-$20 000). Of the 70 patients who had alternative therapy, 45 (64.3%) felt they were getting value for money, five (7.1%) did not, and the remainder did not answer this question. Importantly, 37 (52.9%) felt that they could discuss their alternative treatment with their physician, while 28 (40%) felt they could not.
Patient characteristics and alternative therapy use Being young and being married were significantly associated with use of alternative medicine, with marital status significant at P = 0.02. Logistic regression analysis showed that age and satisfaction with conventional therapy are the key predictors for a decision to use alternative therapy. Overall, younger patients used more alternative therapy (odds ratio, 1.67; P < 0.0001; 95% CI, 1.32-2.13), and those who were very satisfied with their conventional treatment used less alternative therapy (odds ratio, 0.55; P < 0.0001; 95% CI, 0.38-0.79). Sex, level of education, employment status, income, private health insurance, diagnosis, expectations at beginning of treatment or impressions at the end of treatment were not significantly associated with use of alternative therapy. Discussion Any discussion of alternative medicine is complicated by arguments about terminology. The most commonly used terms in the literature are "alternative", "complementary" or "unproven". Some have suggested that the term "alternative" is spurious, because it suggests equally valid options, 3 but we have chosen to use it because it is in common use in describing treatments outside conventional medicine. "Complementary" may seem an appropriate term for a study of patients attending a hospital, but it suggests therapies that are valuable when combined with conventional medicine. "Unproven" is the American Cancer Society's preferred term and relates to methods that are "on the basis of careful review by scientists and/or clinicians, not deemed proven, nor recommended for current use". 4 It has also been suggested that "There are no unproven treatments for universally curable diseases" 5 -- the very fact that this issue is so controversial in cancer medicine suggests that conventional treatment has a long way to go in optimising management of malignant disease.
Previous studies have shown that between 9% and 54% of adult cancer patients use some form of alternative medicine, 6-10 while a recent Australian study reported a 46% rate of alternative therapy use in a paediatric oncology population. 11 The rate of alternative medicine use in our study (21.9%) is within this range. It may not be an accurate reflection of alternative therapy use in cancer patients as our patients' response to the questionnaire was voluntary, creating a potential selection bias. Nevertheless it does indicate that a significant proportion of cancer patients use some form of alternative therapy, and gives some idea of the current range of therapies.
Several features of our study population should be considered when relating our results to other populations. Royal North Shore Hospital services the northern Sydney area, where the population is characterised by being relatively wealthy, and having high levels of education and private health insurance. Port Macquarie Base Hospital serves a community with a large retired population and relative wealth (by rural standards). The high prevalence of breast cancer managed by this unit explains the predominance of women in the group studied.
There was a high level of optimism at the outset of both conventional treatment and alternative therapy (85.6% v. 63.0% belief in cure/life-prolongation), which fell modestly by completion of treatment (72.9% v. 48.6%). As most patients were receiving palliative chemotherapy, it seems that many patients had an unrealistic expectation about the goals of treatment. This reinforces the need for clear communication with patients. However, most patients were highly satisfied with both conventional and alternative treatments (75.3% v. 70.0%), and dissatisfaction was almost non-existent (3.1% v. 1.4%). This high level of satisfaction, often in the absence of objective benefit, has been described in studies of conventional 12 and alternative 6,11 medicine, and may be related to a hope engendered by the intervention of a clinician. 13,14
As in other studies which report that patients will frequently try multiple alternative therapies, 6,11 we found that over 75% of patients used two or more therapies. Alternative therapies available in Australia appear to be a mixture of the British and United States experience. Psychological methods such as relaxation, imagery and healing, which are prevalent in the United Kingdom, 6 and interventional methods, such as diet and megavitamins, more common in the US, 7 are used with similar frequency.
The predominance of friend and family recommendation (52.9%) as the source of information on alternative medicine may partially explain the significantly increased use by married patients. The contribution of recommendation by doctors is comparatively low, but it must be remembered that these patients were attending an oncology service. Of course, some cancer patients may not seek conventional care, and consultations with alternative practitioners, or with medical practitioners who combine conventional and alternative therapies, are becoming more common. 15,16 In the US there are currently more referrals to alternative practitioners than to primary care physicians. 17
Many studies report the significant financial costs of alternative medicine. 5,9,18-20 There is a wide variation in the cost of various therapies, with psychological methods usually far less expensive than interventions such as metabolic therapy, Laetrile and high-dose vitamin C. In one US study, the median annual outlay was US$262, and the mean was US$3492, suggesting enormous expense in some cases. 7 Our findings are similar, with expenditure ranging from nothing to $20 000 per year. However, nearly all of those using alternative medicine felt they were getting value for money.
Previous studies have reported that users of alternative therapy tend to be young, female, of higher social class and more highly educated, while income, increased time since cancer diagnosis, increased number of people in a household, and tumour site may be associated with alternative therapy use. 6,7,9 We found that being young and being married were significantly associated with increased use, and that those who were very satisfied with conventional therapy used less alternative therapy. The finding that being married is associated with increased use of alternative therapy may be related to having increased numbers in a household, 9 and perhaps greater access to ideas and support for trying new things.
Many patients in our study did not discuss their use of alternative therapy with their physicians, possibly because they were afraid of getting a negative response. This may reflect a need to improve doctor-patient communication. If a proportion of patients are going to use alternative therapies, it is important that their doctors are informed: firstly, so that possible interactions and complications can be avoided, and, secondly, to enable doctors to provide informed opinion on the alternative choices available.
Acknowledgements
We thank Professor John A Levi and Dr Helen R Wheeler for contributing
their patients to the study.
References
- MacLennan AH, Wilson DH, Taylor AW. Prevalence and cost of
alternative medicine in Australia. Lancet 1996; 347:
569-573.
-
SPSS: Statistical package for the social sciences [computer
program], version 5. Chicago, Ill: SPSS inc, 1990.
-
McGinnis LS. Alternative therapies, 1990. An overview. Cancer
1991; 67: 1788-1792.
-
Pamphlet number 3028-REV. Atlanta, Ga.: American Cancer Society,
1990.
-
Cassileth BR. The social implications of questionable cancer
therapies. CA Cancer J Clin 1989; 39: 311-316.
-
Downer SM, Cody MM, McCluskey P, et al. Pursuit and practice of
complementary therapies by cancer patients receiving conventional
treatment. BMJ 1994; 309: 86-89.
-
Cassileth BR, Lusk EJ, Strouse TB, Bodenheimer BA. Contemporary
unorthodox treatments in cancer medicine. A study of patients,
treatments and practitioners. Ann Intern Med 1984; 101:
105-112.
-
Harris L and associates. Health information and the use of
questionable treatments: a study of the American Public, 1987.
Washington DC: Department of Health and Human Services, 1987.
-
Lerner IJ, Kennedy BJ. The prevalence of questionable methods of
cancer treatments in the United States. CA Cancer J Clin 1992;
42: 181-191.
-
Miller MJ, Boyer MJ, Dunn SM, et al. Why do Australian cancer
patients use unproven therapies? Proc Clin Oncol Soc Aust
1995; 22: 78.
-
Sawyer MG, Gannom AF, Toogood IR, et al. The use of alternative
therapies by children with cancer. Med J Aust 1994; 160:
320-322.
-
Coates A, Gebski V, Bishop JF, et al. Improving the quality of life
during chemotherapy for advanced breast cancer. N Engl J Med
1987; 317: 1490-1495.
-
Stoll BA. Can unorthodox cancer therapy improve quality of life?
Ann Oncol 1993; 4: 121-123.
-
Kodish E, Post SG. Oncology and hope. J Clin Oncol 1995; 13:
1817-1822.
-
Borkan J, Neher JO, Anson O, Smoker B. Referrals for Alternative
therapies. J Fam Prac 1994; 39: 545-550.
-
Paterson C, Peacock W. Complementary practitioners as part of the
primary health care team: evaluation of one model. Br J Gen Pract
1995; 45: 255-258.
-
Burke C, Sikora K. Complementary and conventional cancer care:
the integration of two cultures. Clin Oncol 1993; 5: 220-227.
-
Guzley GJ. Alternative cancer treatments: impact of unorthodox
therapy on the patient with cancer. South Med J 1992; 85:
519-523.
-
Cassileth BR, Lusk EJ, Guerry D, et al. Survival and quality of life
among patients receiving unproven as compared with conventional
cancer therapy. N Eng J Med 1991; 324: 1180-1185.
-
Ernst E. Complementary medicine: common misconceptions. J R
Soc Med 1995; 88: 244-247.
(Received 24 Jan, accepted 5 Aug 1996)
Authors' details
Department of Clinical Oncology, Royal North Shore
Hospital, Sydney, NSW.
Stephen D Begbie, MB BS, Oncology Registrar;
Zoltan L
Kerestes, PhD, Computer Scientist;
David R Bell, MB BS,
FRACP, Medical Oncologist.
Reprints: Dr D R Bell, Department of Medical Oncology, Royal
North Shore Hospital, St Leonards, NSW 2065.
- To top of article - ©MJA 1996
<URL: http://www.mja.com.au/> © 1996 Medical Journal of Australia.
Received 26 May 2026, accepted 26 May 2026
- Stephen D Begbie
- Zoltan L Kerestes
- David R Bell