The known: Poor diet, alcohol use, smoking, physical inactivity, poor sleep, and excessive screen time are lifestyle risk factors for chronic disease; they often emerge in adolescence and typically persist into adulthood.
The new: Health4Life, a school‐based multiple health behaviour change intervention, was no more effective than normal school health education for modifying changes in six major risk factors for chronic disease in young adolescents over 24 months.
The implications: School‐based e‐health multiple health behaviour change interventions need effective engagement strategies to maximise their effectiveness.
Physical inactivity, poor diet, poor sleep, excessive recreational screen time, and alcohol and tobacco use are critical risk factors for chronic disease, including type 2 diabetes, cancer, cardiovascular disease, obesity, and mental health disorders.1,2,3 These risk factors, the “big 6”, typically develop and are highly prevalent during adolescence;4 once established, they are likely to persist into adulthood.5,6 Multiple health behaviour change interventions aim to cost‐effectively and efficiently promote healthy lifestyles during adolescence.7
The Health4Life intervention, co‐designed with public health experts, researchers, educators, and young people, aims to prevent development of the six major risk behaviours during adolescence; it is based on models of self‐determination, social cognition, and social influence.8,9 The intervention comprises six internet‐based lessons delivered during health education classes in the first year of secondary school (age, 11–14 years), complemented by a smartphone app.8
We have recently reported our evaluation of the Health4Life trial primary outcomes.9 Although we found that knowledge of the six major risk behaviours increased in the intervention group, the Health4Life program was not more effective than usual health education for modifying these behaviours. Nevertheless, the vast majority of students and teachers regarded the intervention and the app favourably; students enjoyed the learning style, and teachers felt the intervention held student attention.9 Possible reasons for its ineffectiveness include inadequate duration and delivery of the intervention, low use of the app,10 and the fact that we introduced the app and undertook follow‐up assessments during the coronavirus disease 2019 (COVID‐19) pandemic.9
In this article, we report our evaluation of the secondary outcomes of the Health4Life trial: alcohol drinking frequency, binge drinking, alcohol‐related harms, tobacco smoking frequency, discretionary food consumption risk, risk of not meeting fruit and vegetable intake guidelines, light physical activity, time spent watching television and using electronic devices, difficulty in falling asleep, and daytime sleepiness. These twelve secondary outcomes, a broader range of behaviours than the primary outcomes, facilitated more comprehensive evaluation of the effectiveness of the Health4Life intervention.
Methods
The Health4Life trial was a cluster randomised controlled trial in 71 Australian secondary schools during 1 January 2019 – 31 December 2022; the assessments described in this article were undertaken during 19 July 2019 – 31 December 2021. We report our trial, prospectively registered with the Australian New Zealand Clinical Trials Registry (ACTRN12619000431123; 18 March 2019; secondary outcome details updated 11 February 2021), according to the Consolidated Standards of Reporting Trials (CONSORT) guidelines.11
Participants
We invited five hundred and nineteen public, independent, and Catholic diocese schools in New South Wales (Greater Sydney, Newcastle, Wollongong), Queensland (within 100 km of Brisbane), and Western Australia (within 600 km of Perth) to participate. Each school had previously expressed interest in the trial or were identified in the MySchool.com database, had at least 30 enrolled year 7 students, and relevant ethics approvals were available. Eighty‐five schools agreed to participate; 42 were initially randomised to the intervention arm, 43 to the control arm of the study. Five of the intervention arm schools withdrew before baseline assessments, and one after the baseline assessment; 36 schools participated in all assessments and were included in the analysis. Seven of the control arm schools withdrew before baseline assessments, and one after the baseline assessment; 35 schools participated in all assessments and were included in the analysis.
All year 7 students at the participating schools who spoke English fluently were eligible for participation if they provided active consent and their parents provided passive (opt‐out) or active (opt‐in) consent, according to the requirements of their school ethics board. Consent processes and the characteristics of the participants have been reported previously,9,12 as have sample size calculations.8
Procedure
The randomisation and masking procedures have been described previously.8 In short, we applied the Heo–Leon power calculations method for longitudinal cluster randomised controlled trials.13 We assumed that 70% of initial participating students would remain in the trial until the twenty‐four month follow‐up. The participating schools were randomised, stratified by location and school gender composition, by a biostatistician not involved in participant recruitment, using the blockrand function14 in R 4.2.2. As is usual practice for school‐based cluster randomised controlled trials, the schools, participants, and researchers were not blinded to their allocation. Participating year 7 students completed surveys in class at baseline (2019), immediately after the intervention (2019), and twelve months (2020) and 24 months after the intervention (2021). The survey texts are available on justified application to the corresponding author of this article.
The Health4Life intervention
Participating students in the intervention group schools received the Health4Life intervention, an e‐health multiple health behaviour change program that provides simultaneous education about the six major lifestyle behaviours and their relationships with each other. It uses a staged prevention model with universal and selective components. The universal components are six 20‐minute online cartoon modules delivered during health education class, ideally over six weeks, supplemented by internet‐based feedback and optional teacher‐facilitated activities, as well as an optional companion smartphone app, provided during the first lesson, for use outside class. The school‐based program was designed to provide evidence‐based information about the six major lifestyle behaviours, develop resistance and self‐regulatory skills, modify perceptions of norms, and increase autonomous motivation. The app was designed to encourage behavioural change through behaviour tracking and goal‐setting activities. Students identified as being at risk of chronic disease (ie, for whom two of the target behaviours were identified at baseline) were offered the selective Health4Life + intervention, which provided additional education about the six behaviours, as well as cognitive behavioural and app‐based motivation enhancement techniques that support behavioural change.8 Four hundred and seven intervention group students (11%) used the Health4Life app during the entire trial period; five students (0.1%) used the supplementary Health4Life + booster content.9,10
Participating students in the control group schools received the usual health education provided by their school. Teachers recorded in logbooks the amount and format of any education related to the six lifestyle behaviours. Thirty‐two control arm schools provided logbooks from a total of 96 teachers, 90 of whom reported one or more lessons touching on at least one of the target behaviours in 2019.9
Outcomes
The twelve outcomes reported in this article were self‐reported measures of the secondary outcome risk factors at baseline, immediately after the intervention, and twelve and 24 months after the intervention: binge drinking, discretionary food consumption risk (consumption of more than one discretionary food item per day on most days), inadequate fruit and vegetable intake,15 difficulty falling asleep, and light physical activity frequency (categorical variables); and tobacco smoking frequency, alcohol drinking frequency, alcohol‐related harms (Abbreviated Rutgers Alcohol Problem Index16), daytime sleepiness (Paediatric Daytime Sleepiness Scale17), and time spent watching television and using electronic devices (continuous variables) (Supporting Information, section 1). Mental health and intention to change behaviour were also examined, but our findings are not reported in this article.
Statistical analysis
For categorical variables, we report frequencies with estimated proportions and 95% confidence intervals (CIs) estimated with the Wilson method; for continuous variables, we report means with 95% CIs or standard deviations (SDs).
We assessed change over the 24‐month follow‐up period in latent growth models (using Mplus 8.4; http://www.statmodel.com). The models had a structural equation framework in which baseline variable values are the reference points and latent intercepts and slopes are respectively interpreted as participant starting points and change over time. To assess the intervention effect, the influence of the intervention group variable on the slope latent factor was deemed to provide an estimate of between‐group differences in change over time. The latent growth model type was selected according to the distribution of values for an outcome (binary, continuous, or ordinal; further details: Supporting Information, section 2). We report odds ratios (ORs) with 95% CIs for binary logistic and ordinal variables, and mean differences with 95% CIs for continuous variables, estimated for each of the four time points using the Mplus model constraint command. School was included as a cluster variable in all models. As randomisation was stratified by gender and site, we controlled for sex at birth and school region in all models. We tested different specifications of time scores (linear, quadratic, freely estimated) on unconditional latent growth models (ie, no covariates) to determine the best fitting time structure and slope estimate interpretation for each outcome. Model fit was assessed with the Akaike, Bayesian, and sample size‐adjusted Bayesian information criteria (Supporting Information, section 3).
To assess the effect of attrition on outcomes, we included a binary completeness variable (ie, students who participated only at baseline or who completed at least one follow‐up survey). The statistical significance of differences in continuous baseline variables between students who did or did not participate in follow‐up surveys was assessed in t tests; binary and multinomial logistic regression were respectively used for dichotomous and categorical variables. The latent growth models used full information maximum likelihood estimation, treating missing data according to intention‐to‐treat principles (ie, including all participants randomised to the study arms). Full information maximum likelihood uses all available information when estimating parameters; it is considered superior to older methods and is widely employed in latent growth model analyses.18
Ethics approval
Our study was approved by the human research ethics committees of the University of Sydney (2018/882), the University of Queensland (2019000037), and Curtin University (HRE2019‐0083), and by ethics committees for each participating school, including the NSW Department of Education (SERAP no. 2019006), the Catholic Education Diocese of Bathurst, the Catholic Schools Office Diocese of Maitland–Newcastle, Edmund Rice Education Australia, the Brisbane Catholic Education Committee (373), and Catholic Education Western Australia (RP2019/07).
Results
Of the 6640 year 7 students in 71 schools with parental permission to participate who completed the baseline survey (intervention: 3610 students; control: 3030 students) (Box 1; Supporting Information, table 1), 6454 (97.2%) completed at least one follow‐up survey (intervention: 3502, 97.0%; control: 2952, 97.4%), and 5698 (85.8%) two or more follow‐up surveys (intervention: 3040, 84.2%; control: 2658, 87.7%).
Secondary outcomes at baseline, by follow‐up survey participation
The proportion of students who completed at least one follow‐up survey who did not meet the fruit guidelines at baseline was smaller than for those who did not (23.8% v 33.5%; OR, 0.62; 95% CI, 0.47–0.82). The reported mean daily television time (2.7 [SD, 2.6] hours v 3.5 [SD, 3.5] hours; P < 0.001) and electronic device use time (3.1 [SD, 3.0] hours v 3.8 [SD, 3.6] hours; P < 0.001) was lower for those who completed at least one follow‐up survey. The mean alcohol‐related harm score was lower for the participants who completed at least one follow‐up survey (5.3 [SD, 6.8] v 6.04 [SD, 6.4]; P = 0.015), as was mean daytime sleepiness score (13.8 [SD, 6.1] v 15.6 [SD, 6.4]; P < 0.001); a larger proportion reported difficulty falling asleep (61.5% v 52.0%; OR, 1.47; 95% CI, 1.11–1.95) (Supporting Information, tables 2, 3).
The likelihood of no follow‐up data was similar for the Health4Life and control groups for all secondary outcomes except discretionary food risk, fruit intake, and vegetable intake (Supporting Information, table 4).
Change in secondary outcomes over 24 months, by study arm
All measures of alcohol and tobacco use increased in both groups between the baseline and 24‐month surveys. The proportion of control group participants who reported binge drinking increased from 0.45% (95% CI, 0.27–0.77%) at baseline to 5.9% (95% CI, 5.0–7.0%) at 24 months; in the intervention group it increased from 0.55% (95% CI, 0.35–0.86%) to 6.7% (95% CI, 5.7–7.7%). The mean reported number of days in the past 30 days on which participants used alcohol (24 months: control, 0.39 [95% CI, 0.28–0.50] days; intervention: 0.52 [95% CI, 0.40–0.65] days) or tobacco (24 months: control, 0.33 [95% CI, 0.21–0.45] days; intervention: 0.48 [95% CI, 0.34–0.61] days) also increased between baseline and 24 months, as did the mean reported alcohol‐related harm score (24 months: control, 6.89 [95% CI, 6.18–7.60]; intervention: 7.60 [95% CI, 6.88–8.32]) (Box 2, Box 3).
The proportion of students who did not meet fruit intake guidelines increased over time (24 months: control, 30.6% [95% CI, 28.7–32.6%]; intervention: 33.5% [95% CI, 31.7–35.5%]), but not that of those who did not meet vegetable intake guidelines (24 months: control, 87.7% [95% CI, 86.3–89.0%]; intervention: 89.3% [95% CI, 88.0–90.4%]). The proportions reporting light physical activity five or more times a week declined slightly (24 months: control, 58.8% [95% CI, 56.8–60.8%]; intervention: 59.2% [95% CI, 57.2–61.1%]), as did the proportions reporting discretionary food risk (24 months: control, 37.7% [95% CI, 35.7–39.8%]; intervention: 38.1% [95% CI, 36.1–40.1%]) (Box 2).
The proportions who reported difficulty falling asleep did not change markedly in either group (24 months: control, 36.4% [95% CI, 34.5–38.4%]; intervention: 32.9% [95% CI, 31.1–34.8%]), but mean daytime sleepiness scores increased slightly in each group (24 months: control, 15.5 [95% CI, 15.0–15.5]; intervention: 14.7 [95% CI, 14.4–14.9]) (Box 2, Box 3).
Finally, both mean daily television (24 months: control, 3.0 [95% CI, 2.9–3.1] hours; intervention: 3.1 [95% CI, 3.0–3.2] hours) and mean daily electronic device time (24 months: control, 3.6 [95% CI, 3.5–3.8] hours; intervention: 3.8 [95% CI, 3.7–4.0] hours) increased slightly over 24 months (Box 3).
The best fitting time functions varied by outcome (Supporting Information, table 5). The differences between the Health4Life and control groups in baseline (intercept) and change over 24 months (slope) were statistically non‐significant for all secondary outcomes (Box 4).
Discussion
We report the secondary outcomes of the first study to evaluate the effectiveness of a school‐based e‐health multiple health behaviour change intervention that comprehensively targets the six major risk factors for chronic disease. The twelve secondary outcomes provided a broader picture of the impact of Health4Life than our evaluation of the six primary outcomes.9 For instance, a change in light physical activity (eg, walking more each day) may be easier for adolescents than a change in the related primary outcome, the number of days with at least 60 minutes of moderate to vigorous physical activity. Similarly, binge drinking, frequency of drinking, and alcohol‐related harm capture a greater range of behaviour than the primary outcome, any alcohol consumption during the past six months. Despite the more nuanced approach, however, and consistent with our primary outcome results,9 we identified no major differences in outcomes between the Health4Life and usual health education groups.
Lifestyle disruptions caused by the COVID‐19 pandemic during the study follow‐up period may have reduced students’ motivation, capacity, and opportunities for acting on the knowledge provided by the program. As the impact of the pandemic on mental health was particularly great for adolescents,19 it could have had a strong influence on the effect of the intervention on health behaviour. Knowledge about the chronic disease risk factors increased significantly among Health4Life program participants,9 but knowledge changes might not be sufficient for changing behaviour.20 This is especially true for behaviour entrenched early in adolescence, such as screen use and sedentary behaviour. Given the already high prevalence of these behaviours among our participants,12 earlier or more targeted intervention strategies might be more effective.
Behavioural change interventions aim to modify two dimensions of the target behaviour: value and activation. For value, strategies such as education, persuasion, and modelling aim to change what people think, want, and feel. Activation often involves engagement strategies such as nudges, goal setting, if‐then strategies, and reminders to enhance the accessibility of thoughts, feelings, and goals related to the target behaviour.21 As we did not examine the students’ intention to change their behaviour, we could not assess whether value was affected by the intervention. The Health4Life app was intended to promote engagement by providing motivational interviewing and goal setting to increase behavioural activation.10 By increasing knowledge through education, Health4Life may have changed the value students attached to healthy behaviour, but not the cognitive accessibility needed to convert this knowledge into behavioural change22,23 because the app‐based component that included the activation strategies was not used by most students.
Although the intervention cartoon modules targeted fruit and vegetable intake, internet‐based feedback focused on sugar‐sweetened beverages. Interventions for increasing fruit and vegetable intake should provide feedback regarding all dietary targets, as this is an effective component of electronic health behaviour change interventions for improving fruit and vegetable intake.24
Our findings are consistent with those of other studies that school‐based physical activity interventions typically have limited or no effect.25,26 A 2016 model of expanded, extended and enhanced opportunities provided a set of principles for effective school‐based physical activity interventions based on expanding the number of opportunities for students to be active (eg, providing before and after school activities), increasing the time allocated to existing opportunities (eg, allocating more time to breaks from classes for physical activity), and modifying existing opportunities to increase the amount of physical activity (eg, less waiting time in physical education classes).27 The Health4Life program could be improved by including school‐level engagement and commitment to increasing opportunities for physical activity at school.
The Health4Life intervention was no more effective than usual health education for reducing substance use. A meta‐analysis similarly found that e‐health multiple health behaviour change interventions did not reduce alcohol or tobacco use by school students,28 but we have previously reported effective prevention of alcohol and drug use with a program for Australian students in high school years 8–10.29 Health4Life was delivered to year 7 students, which may have been too early to influence substance use, suggesting that alcohol and tobacco use might be best targeted separately from other lifestyle risk factors. Other health risks, including physical inactivity and screen use, were already common in year 7, perhaps indicating that prevention should start earlier than year 7. Education about each risk factor, provided sequentially or over several sessions, could provide more opportunities for students to apply the acquired knowledge and skills during their daily lives.
Limitations
The Health4Life study is the largest school‐based multisite cluster randomised controlled trial of an e‐health multiple health behaviour change program. The intervention was co‐designed with public health experts, researchers, educators, and young people, and was well received by both students and teachers.9 Nonetheless, although the Health4Life trial included students from a variety of schools and locations, the sample was not nationally representative, limiting the generalisability of our findings. Further, assessments of all outcomes relied on reports by students. Despite using validated self‐report measures for each outcome, students may have misjudged their health behaviour or been influenced by social desirability or expectancy effects. Corroboration of survey responses by objective health data sources would be desirable in future studies. The choice of functional form of time (ie, linear, quadratic, free) could affect the ability to detect intervention effects, but the decision to use different time scores was based on unconditional model fit, which ensured the use of the most appropriate time function according to the data. Finally, for nine of twelve outcomes the missing data proportion was similar for both trial groups, but this did not apply to fruit or vegetable consumption, or to discretionary food risk.
Conclusions
As with our primary outcomes findings, the Health4Life intervention was no more effective than usual school health education in modifying twelve secondary outcome health behaviours among Australian adolescents over 24 months. The COVID‐19 pandemic may have limited the capacity for students for the behavioural changes promoted by Health4Life, but the program needs to be refined while maintaining its acceptability for students and teachers. Refinements could include changes to the timing, order, and length of the intervention modules, as well as strategies for increasing value and activation at the time of or after knowledge gain.
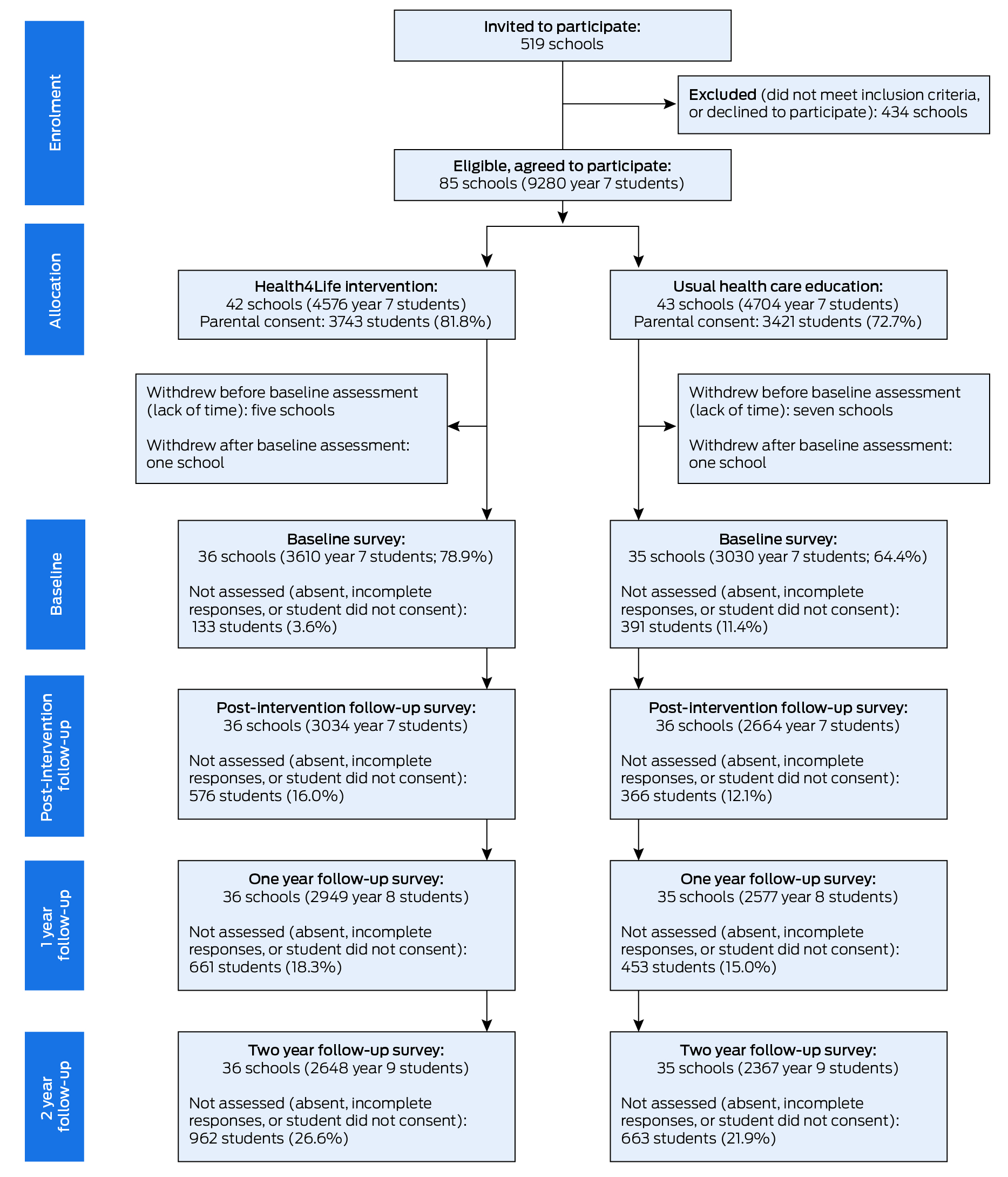
Box 1 – The Health4Life cluster randomised controlled trial: selection of participants and survey completion
Box 2 – Participants who reported behaviour inconsistent with lifestyle guidelines for avoiding chronic disease: categorical outcomes, by Health4Life survey and study arm*
|
|
Participants who did not meet guidelines: number/respondents and estimated proportion (95% CI) |
||||||||||||||
|
Target behaviour |
Baseline survey |
Post‐intervention |
12‐month survey |
24‐month survey |
|||||||||||
|
|
|||||||||||||||
|
Binge drinking† |
|
|
|
|
|||||||||||
|
Control |
13/2868 |
29/2460 |
64/2479 |
134/2256 |
|||||||||||
|
Health4Life |
19/3453 |
20/2825 |
68/2804 |
162/2433 |
|||||||||||
|
Discretionary food risk‡ |
|
|
|
|
|||||||||||
|
Control |
1002/2475 |
908/2349 |
873/2272 |
815/2159 |
|||||||||||
|
Health4Life |
1355/3252 |
994/2702 |
930/2495 |
859/2257 |
|||||||||||
|
Fruit intake inadequate |
|
|
|
|
|||||||||||
|
Control |
585/2828 |
527/2452 |
597/2441 |
682/2227 |
|||||||||||
|
Health4Life |
907/3338 |
647/2788 |
786/2768 |
803/2394 |
|||||||||||
|
Vegetable intake inadequate |
|
|
|
|
|||||||||||
|
Control |
2425/2841 |
2069/2458 |
2111/2440 |
1951/2225 |
|||||||||||
|
Health4Life |
2937/3374 |
2349/2800 |
2392/2768 |
2129/2385 |
|||||||||||
|
Light physical activity (per week) |
|
|
|
|
|||||||||||
|
Control: none |
112/2852 |
101/2468 |
118/2454 |
135/2244 |
|||||||||||
|
Control: once or twice |
359/2852 |
334/2468 |
331/2454 |
341/2244 |
|||||||||||
|
Control: three or four times |
536/2852 |
471/2468 |
459/2454 |
448/2244 |
|||||||||||
|
Control: five times or more |
1845/2852 |
1562/2468 |
1546/2454 |
1320/2244 |
|||||||||||
|
Health4Life: none |
169/3404 |
100/2803 |
142/2785 |
156/2412 |
|||||||||||
|
Health4Life: once or twice |
411/3404 |
358/2803 |
391/2785 |
383/2412 |
|||||||||||
|
Health4Life: three or four times |
634/3404 |
514/2803 |
509/2785 |
445/2412 |
|||||||||||
|
Health4Life: five times or more |
2190/3404 |
1831/2803 |
1743/2785 |
1428/2412 |
|||||||||||
|
Difficulty falling asleep |
|
|
|
|
|||||||||||
|
Control |
1148/2985 |
930/2608 |
900/2541 |
847/2325 |
|||||||||||
|
Health4Life |
1392/3556 |
933/2977 |
988/2888 |
847/2572 |
|||||||||||
|
|
|||||||||||||||
|
CI = confidence interval. * Outcomes and their assessment are described in the Supporting Information, part 1. † Five or more standard alcoholic drinks on one occasion in the past six months. ‡ Consumption of more than one discretionary food item per day on most days. |
|||||||||||||||
Box 3 – Participants who reported behaviour inconsistent with lifestyle guidelines for avoiding chronic disease: continuous outcomes, by Health4Life survey and study arm*
|
|
Mean (95% confidence interval) |
||||||||||||||
|
Behaviour |
Baseline survey |
Post‐intervention |
12‐month survey |
24‐month survey |
|||||||||||
|
|
|||||||||||||||
|
Tobacco use (days in past 30 days) |
|
|
|
|
|||||||||||
|
Control |
0.06 (0.02–0.11) |
0.20 (0.11–0.29) |
0.23 (0.13–0.32) |
0.33 (0.21–0.45) |
|||||||||||
|
Health4Life |
0.06 (0.02–0.10) |
0.15 (0.08–0.23) |
0.25 (0.16–0.34) |
0.48 (0.34–0.61) |
|||||||||||
|
Alcohol use (days in past 30 days) |
|
|
|
|
|||||||||||
|
Control |
0.03 (0.01–0.05) |
0.22 (0.13–0.32) |
0.27 (0.18–0.37) |
0.39 (0.28–0.50) |
|||||||||||
|
Health4Life |
0.07 (0.03–0.10) |
0.12 (0.06–0.18) |
0.26 (0.17–0.34) |
0.52 (0.40–0.65) |
|||||||||||
|
Alcohol‐related harm† |
|
|
|
|
|||||||||||
|
Control |
5.31 (4.91–5.70) |
— |
8.19 (7.20–9.17) |
6.89 (6.18–7.60) |
|||||||||||
|
Health4Life |
5.85 (5.44–6.25) |
— |
7.89 (7.04–8.75) |
7.60 (6.88–8.32) |
|||||||||||
|
Daytime sleepiness‡ |
|
|
|
|
|||||||||||
|
Control |
13.9 (13.7–14.1) |
13.6 (13.3–13.8) |
14.3 (14.0–14.5) |
15.5 (15.0–15.5) |
|||||||||||
|
Health4Life |
13.9 (13.7–14.1) |
12.3 (12.0–12.5) |
13.8 (13.5–14.0) |
14.7 (14.4–14.9) |
|||||||||||
|
Television time (hours per day) |
|
|
|
|
|||||||||||
|
Control |
2.61 (2.52–2.70) |
2.64 (2.53–2.74) |
2.90 (2.78–3.02) |
3.00 (2.89–3.12) |
|||||||||||
|
Health4Life |
2.85 (2.76–2.94) |
2.80 (2.69–2.90) |
2.99 (2.88–3.11) |
3.07 (2.95–3.19) |
|||||||||||
|
Device use time (hours per day) |
|
|
|
|
|||||||||||
|
Control |
2.96 (2.86–3.05) |
3.03 (2.92–3.15) |
3.62 (3.50–3.76) |
3.64 (3.52–3.77) |
|||||||||||
|
Health4Life |
3.33 (3.22–3.44) |
3.07 (2.96–3.18) |
3.62 (3.50–3.74) |
3.85 (3.72–3.98) |
|||||||||||
|
|
|||||||||||||||
|
* Outcomes and their assessment are described in the Supporting Information, part 1. † Students who reported drinking alcohol in the past six months only: Abbreviated Rutgers Alcohol Problem Index.16 ‡ Paediatric Daytime Sleepiness Scale.17 |
|||||||||||||||
Box 4 – Effects of the Health4Life intervention (v control) on baseline differences (intercept) and change over time (slope) in secondary outcomes: latent growth models
|
Behaviour |
Intercept (95% CI) |
Slope (95% CI) |
Quadratic slope (95% CI) |
||||||||||||
|
|
|||||||||||||||
|
Categorical outcomes |
|
|
|
||||||||||||
|
Binge drinking* |
0.55 (0.16 to 1.85) |
1.64 (0.34 to 7.01) |
— |
||||||||||||
|
Discretionary food risk* |
0.93 (0.64 to 1.33) |
0.99 (0.71 to 1.39) |
— |
||||||||||||
|
Fruit intake inadequate* |
0.69 (0.32 to 1.50) |
1.08 (0.57 to 2.05) |
— |
||||||||||||
|
Vegetable intake inadequate* |
1.01 (0.46 to 2.19) |
0.97 (0.64 to 1.47) |
— |
||||||||||||
|
Light physical activity† |
0.93 (0.78 to 1.12) |
1.00 (0.72 to 1.38) |
— |
||||||||||||
|
Difficulty falling asleep* |
1.14 (0.79 to 1.65) |
0.72 (0.51 to 1.01) |
— |
||||||||||||
|
Continuous outcomes‡ |
|
|
|
||||||||||||
|
Tobacco use frequency |
–0.02 (–0.11 to 0.07) |
0.03 (–0.58 to 0.64) |
0.09 (–0.53 to 0.71) |
||||||||||||
|
Alcohol use frequency |
0.03 (–0.03 to 0.10) |
–0.34 (–1.16 to 0.49) |
0.36 (–0.50 to 1.23) |
||||||||||||
|
Alcohol‐related harm |
0.51 (–0.29 to 1.31) |
–2.86 (–8.59 to 2.87) |
2.71 (–3.32 to 8.73) |
||||||||||||
|
Daytime sleepiness |
–0.33 (–0.83 to 0.17) |
–0.84 (–2.16 to 0.48) |
0.88 (–0.52 to 2.28) |
||||||||||||
|
Television time |
0.17 (–0.12 to 0.47) |
–0.07 (–0.35 to 0.06) |
— |
||||||||||||
|
Device use time |
0.19 (–0.17 to 0.55) |
–0.07 (–0.29 to 0.16) |
— |
||||||||||||
|
|
|||||||||||||||
|
CI = confidence interval. * Logistic latent growth models; slope estimates are odds ratios, intervention v control group, at 24 months (not statistically significant if 95% CI includes 1). † Ordinal logistic latent growth model; slope estimate is odds ratio for being in a higher activity category, intervention v control group, at 24 months (not statistically significant if 95% CI includes 0). ‡ Linear regression models; slope estimates are relative differences in the mean change in outcome over 24 months, intervention v control group. All models are adjusted for sex at birth and school location; outcomes and their assessment are described in the Supporting Information, part 1. |
|||||||||||||||
Received 18 March 2023, accepted 17 October 2023
- Siobhan O'Dean1
- Matthew Sunderland1
- Nicola Newton1
- Lauren Gardner1
- Maree Teesson1
- Cath Chapman1
- Louise Thornton1
- Tim Slade1
- Leanne Hides2,3
- Nyanda McBride4
- Frances J Kay‐Lambkin5
- Steve J Allsop6
- David Lubans7
- Belinda Parmenter8
- Katherine Mills1
- Bonnie Spring9
- Bridie Osman1
- Rhiannon Ellem3
- Scarlett Smout1
- Karrah McCann1
- Emily Hunter1
- Amra Catakovic3
- Katrina Champion1
- 1 Matilda Centre for Research in Mental Health and Substance Use, University of Sydney, Sydney, NSW
- 2 Centre of Youth Substance Abuse, University of Queensland, Brisbane, QLD
- 3 University of Queensland, Brisbane, QLD
- 4 National Drug Research Institute, Curtin University, Perth, WA
- 5 Priority Research Centre for Brain and Mental Health, University of Newcastle, Newcastle, NSW
- 6 National Drug Research Institute, Curtin University of Technology, Perth, WA
- 7 University of Newcastle, Newcastle, NSW
- 8 University of New South Wales, Sydney, NSW
- 9 Northwestern University, Evanston, United States of America
Open access:
Open access publishing facilitated by The University of Sydney, as part of the Wiley ‐ The University of Sydney agreement via the Council of Australian University Librarians.
Data sharings:
We will allow data sharing with researchers from not‐for‐profit organisations or commercial organisations, based in any location, of de‐identified individual participant survey data from all Health4Life assessments from eighteen months to twenty years after each assessment. The statistical analysis code (syntax) and data collected for the study, including de‐identified participant data, will be made available to researchers on request to the corresponding author, accompanied by a study protocol, analysis plan, and signed data access agreement.
This study was funded by the Paul Ramsay Foundation, the National Health and Medical Research Council (fellowships: Katrina Champion, APP1120641; Maree Teesson, APP1078407; Nicola Newton, APP1166377; David Lubans, APP1154507; Centre of Research Excellence in the Prevention and Early Intervention in Mental Illness and Substance Use [PREMISE], APP11349009), the Australian Department of Health and Aged Care and the National Institutes of Health (US) (R01 DK125414, Spring/Hedeker). We acknowledge the schools, students and teachers who participated in this study.
No relevant disclosures.
- 1. Cappuccio FP, Taggart FM, Kandala NB, et al. Meta‐analysis of short sleep duration and obesity in children and adults. Sleep 2008; 31: 619‐626.
- 2. Loewen OK, Maximova K, Ekwaru JP, et al. Lifestyle behaviour and mental health in early adolescence. Pediatrics 2019; 143: e20183307.
- 3. Ding D, Rogers K, van der Ploeg H, et al. Traditional and emerging lifestyle risk behaviours and all‐cause mortality in middle‐aged and older adults: evidence from a large population‐based Australian cohort. PLoS Med 2015; 12: e1001917.
- 4. Guthold R, Stevens GA, Riley LM, Bull FC. Global trends in insufficient physical activity among adolescents: a pooled analysis of 298 population‐based surveys with 1.6 million participants. Lancet Child Adolesc Health 2020; 4: 23‐35.
- 5. Uddin R, Lee EY, Khan SR, et al. Clustering of lifestyle risk factors for non‐communicable diseases in 304 779 adolescents from 89 countries: a global perspective. Prev Med 2020; 131: 105955.
- 6. Kaikkonen JE, Mikkilä V, Magnussen CG, et al. Does childhood nutrition influence adult cardiovascular disease risk? Insights from the Young Finns Study. Ann Med 2013; 45: 120‐128.
- 7. Prochaska JJ, Spring B, Nigg CR. Multiple health behaviour change research: an introduction and overview. Prev Med 2008; 46: 181‐188.
- 8. Teesson M, Champion KE, Newton NC, et al; Health4Life Team. Study protocol of the Health4Life initiative: a cluster randomised controlled trial of an eHealth school‐based program targeting multiple lifestyle risk behaviours among young Australians. BMJ Open 2020; 10: e035662.
- 9. Champion KE, Newton NC, Gardner LA, et al; Health4Life Team. Health4Life eHealth intervention to modify multiple lifestyle risk behaviours among adolescent students in Australia: a cluster‐randomised controlled trial. Lancet Digit Health 2023; 5: e276‐e287.
- 10. Thornton L, Brown HM, Osman B, et al. Factors associated with adolescents’ engagement with a healthy lifestyles app. Procedia Comput Sci 2022; 206: 56‐67.
- 11. Moher D, Hopewell S, Schulz KF, et al. CONSORT 2010 explanation and elaboration: updated guidelines for reporting parallel group randomised trials. BMJ 2010; 340: c869.
- 12. Champion KE, Chapman C, Gardner LA, et al. Lifestyle risks for chronic disease among Australian adolescents: a cross‐sectional survey. Med J Aust 2021; 216: 156‐157. https://www.mja.com.au/journal/2022/216/3/lifestyle‐risks‐chronic‐disease‐among‐australian‐adolescents‐cross‐sectional
- 13. Heo M, Leon AC. Sample size requirements to detect an intervention by time interaction in longitudinal cluster randomized clinical trials. Stat Med 2009; 28: 1017‐1027.
- 14. Snow G. blockrand: Randomization for block random clinical trials. 6 Apr 2020. https://CRAN.R‐project.org/package=blockrand (viewed Mar 2024).
- 15. National Health and Medical Research Council. Australian dietary guidelines. Feb 2013. https://www.health.gov.au/sites/default/files/australian‐dietary‐guidelines.pdf (viewed Mar 2024).
- 16. White HR, Labouvie EW. Towards the assessment of adolescent problem drinking. J Stud Alcohol 1989; 50: 30‐37.
- 17. Drake C, Nickel C, Burduvali E, et al. The Pediatric Daytime Sleepiness Scale (PDSS): sleep habits and school outcomes in middle‐school children. Sleep 2003; 26: 455‐458.
- 18. Schafer JL, Graham JW. Missing data: our view of the state of the art. Psychol Methods 2002; 7: 147‐177.
- 19. Bower M, Smout S, Donohoe‐Bales A, et al. A hidden pandemic? An umbrella review of global evidence on mental health in the time of COVID‐19. Front Psychiatry 2023; 14: 1107560.
- 20. Arlinghaus KR, Johnston CA. Advocating for behaviour change with education. Am J Lifestyle Med 2018; 12: 113‐116.
- 21. Sheeran P, Suls J, Bryan A, et al. Activation versus change as a principle underlying intervention strategies to promote health behaviors. Ann Behav Med 2023; 57: 205‐215.
- 22. Prochaska JO, DiClemente CC. Toward a comprehensive model of change. In Miller W, Heather N, editors. Treating addictive behaviors: processes of change. Boston: Springer US, 1986; pp. 3‐27.
- 23. Ajzen I, Kuhl J, Beckmann J. From intentions to actions: a theory of planned behavior. In Kuhl J, Beckmann J, editors. Action control: from cognition to behavior. Berlin: Springer, 1985; pp. 11‐39.
- 24. Rodriguez Rocha NP, Kim H. eHealth interventions for fruit and vegetable intake: a meta‐analysis of effectiveness. Health Educ Behav 2019; 46: 947‐959.
- 25. Borde R, Smith JJ, Sutherland R, et al. Methodological considerations and impact of school‐based interventions on objectively measured physical activity in adolescents: a systematic review and meta‐analysis. Obes Rev 2017; 18: 476‐490.
- 26. Wolfenden L, McCrabb S, Barnes C, et al. Strategies for enhancing the implementation of school‐based policies or practices targeting diet, physical activity, obesity, tobacco or alcohol use. Cochrane Database Syst Rev 2022; 8: CD011677.
- 27. Beets MW, Okely A, Weaver RG, et al. The theory of expanded, extended, and enhanced opportunities for youth physical activity promotion. Int J Behav Nutr Phys Act 2016; 13: 120.
- 28. Champion KE, Parmenter B, McGowan C, et al; Health4Life team. Effectiveness of school‐based eHealth interventions to prevent multiple lifestyle risk behaviours among adolescents: a systematic review and meta‐analysis. Lancet Digit Health 2019; 1: e206‐e221.
- 29. Newton NC, Stapinski LA, Slade T, et al. The 7‐year effectiveness of school‐based alcohol use prevention from adolescence to early adulthood: a randomized controlled trial of universal, selective, and combined interventions. J Am Acad Child Adolesc Psychiatry 2022; 61: 520‐532.






Abstract
Objectives: To investigate the effectiveness of a school‐based multiple health behaviour change e‐health intervention for modifying risk factors for chronic disease (secondary outcomes).
Study design: Cluster randomised controlled trial.
Setting, participants: Students (at baseline [2019]: year 7, 11–14 years old) at 71 Australian public, independent, and Catholic schools.
Intervention: Health4Life: an e‐health school‐based multiple health behaviour change intervention for reducing increases in the six major behavioural risk factors for chronic disease: physical inactivity, poor diet, excessive recreational screen time, poor sleep, and use of alcohol and tobacco. It comprises six online video modules during health education class and a smartphone app.
Main outcome measures: Comparison of Health4Life and usual health education with respect to their impact on changes in twelve secondary outcomes related to the six behavioural risk factors, assessed in surveys at baseline, immediately after the intervention, and 12 and 24 months after the intervention: binge drinking, discretionary food consumption risk, inadequate fruit and vegetable intake, difficulty falling asleep, and light physical activity frequency (categorical); tobacco smoking frequency, alcohol drinking frequency, alcohol‐related harm, daytime sleepiness, and time spent watching television and using electronic devices (continuous).
Results: A total of 6640 year 7 students completed the baseline survey (Health4Life: 3610; control: 3030); 6454 (97.2%) completed at least one follow‐up survey, 5698 (85.8%) two or more follow‐up surveys. Health4Life was not statistically more effective than usual school health education for influencing changes in any of the twelve outcomes over 24 months; for example: fruit intake inadequate: odds ratio [OR], 1.08 (95% confidence interval [CI], 0.57–2.05); vegetable intake inadequate: OR, 0.97 (95% CI, 0.64–1.47); increased light physical activity: OR, 1.00 (95% CI, 0.72–1.38); tobacco use frequency: relative difference, 0.03 (95% CI, –0.58 to 0.64) days per 30 days; alcohol use frequency: relative difference, –0.34 (95% CI, –1.16 to 0.49) days per 30 days; device use time: relative difference, –0.07 (95% CI, –0.29 to 0.16) hours per day.
Conclusions: Health4Life was not more effective than usual school year 7 health education for modifying adolescent risk factors for chronic disease. Future e‐health multiple health behaviour change intervention research should examine the timing and length of the intervention, as well as increasing the number of engagement strategies (eg, goal setting) during the intervention.
Trial registration: Australian New Zealand Clinical Trials Registry: ACTRN12619000431123 (prospective).