To the Editor: Wu and colleagues1 describe a case of congenital syphilis where the mother had no apparent risk factors and a single negative syphilis serology collected in early pregnancy. The father had an identifiable risk factor.
In metropolitan Perth, Western Australia, infectious syphilis among women of reproductive age is rising, with an over 18‐fold increase from 2015 to 2021 (Box). During this period, most cases (229, 74.1%) were non‐Indigenous women. This growth has been accompanied by cases in pregnancy and, concerningly, neonates with congenital syphilis.
The authors1 observed that identifying risk factors during pregnancy is challenging. They may be absent, difficult to ascertain, subject to change during the pregnancy, and are dependent on the pregnant woman and her sexual partners, whose risks she may not know. Identification relies on health care providers checking the risk throughout pregnancy and on whether the woman recognises, discloses or feels safe to discuss a risk factor. In Perth, syphilis diagnoses among pregnant women are occurring across cultural backgrounds. While some women have additional risks such as insecure housing or illicit drug use, this is not the norm.
Consequently, and because we have likewise observed neonates with congenital syphilis born to women who screened negative early in pregnancy, routine syphilis serology at initial visit and at 28 and 36 weeks (or delivery, if earlier) is now recommended for all pregnant women in metropolitan Perth as per the WA sexual health guidelines2 and local obstetric guidelines.3 This was achieved through the collaboration of clinical and public health staff under the Antenatal and Postnatal Working Group of the WA Syphilis Outbreak Response Group, where a decision was made that monitoring risk factors throughout pregnancy has limitations.
Three‐test syphilis screening for all pregnant women minimises the risk of congenital syphilis occurring because of an unrecognised risk factor, ensures emerging risk factors are not missed, helps normalise testing and reduce stigma, and recognises that women remain sexually active while pregnant. Notably, screening is not a replacement for good history taking and clinical examination, but syphilis can present in subtle and unusual ways that can be overlooked.
Routine syphilis testing at the first antenatal visit is advised by the Australian sexually transmissible infections guidelines.4 A test early in the third trimester is recommended depending on local guidelines.4 As syphilis rates grow in many parts of Australia,5 other jurisdictions should consider adopting additional routine syphilis screening for all pregnant women.
Box – Infectious syphilis cases among women of reproductive age, 2015–2021
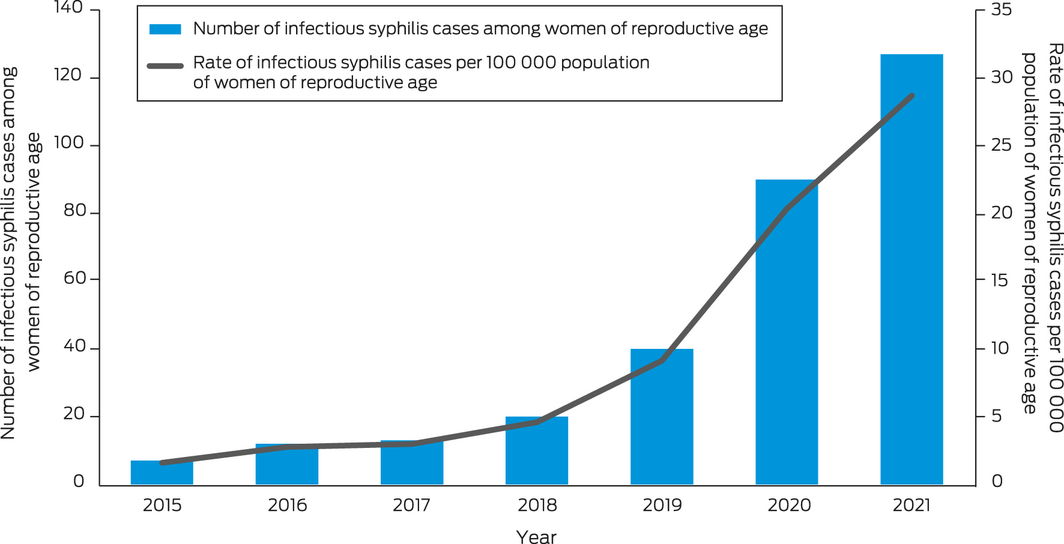
Data sources: The number of cases were obtained from the Western Australian Notifiable Infectious Diseases Database, Department of Health Western Australia (Jan 2022); and the rate of cases were obtained from the Australian Bureau of Statistics census‐derived population data from the Epidemiology Branch, Public and Aboriginal Health Division, Western Australia Department of Health (Dec 2021).
- 1. Wu MX, Moore A, Seel M, et al. Congenital syphilis on the rise: the importance of testing and recognition. Med J Aust 2021; 215: 345–347. https://www.mja.com.au/journal/2021/215/8/congenital‐syphilis‐rise‐importance‐testing‐and‐recognition
- 2. Government of Western Australia, Department of Health. Silver book — STI/BBV management guidelines, 2020 [website]. https://ww2.health.wa.gov.au/Silver‐book (viewed Oct 2021).
- 3. Government of Western Australia, North Metropolitan Health Service, Women and Newborn Health Service. Statewide maternity shared care guidelines, 2021. https://www.kemh.health.wa.gov.au/~/media/HSPs/NMHS/Hospitals/WNHS/Documents/Clinical‐guidelines/Statewide‐Maternity‐Shared‐Care‐Guidelines.pdf (viewed Oct 2021).
- 4. Australasian Society for HIV, Viral Hepatitis and Sexual Health Medicine. Australian STI management guidelines for use in primary care: pregnant people. ASHM, 2021. https://sti.guidelines.org.au/populations‐and‐situations/pregnant‐people/ (viewed Dec 2021).
- 5. Kelly P. Increasing notifications of infectious syphilis in women of reproductive age. Australian Government Department of Health, 2021. https://www.acrrm.org.au/docs/default‐source/all‐files/cmo‐letter‐to‐providers‐congenital‐syphilis.pdf?Status=Temp&sfvrsn=deb07958_4 (viewed Oct 2021).





No relevant disclosures.