To the Editor: Despite the rapid uptake of telemedicine during the coronavirus disease 2019 (COVID‐19) pandemic,1 it is important to identify the barriers that hinder the delivery of alternate modes of care among specific populations. We share our reflections on the challenges of implementing telemedicine in a tertiary addiction medical clinic in Melbourne, providing treatment for about 105 patients each month.
At the start of the COVID‐19 pandemic in February 2020, videoconferencing appointments were encouraged, supported by technical assistance from a clinician. During the Stage 4 lockdown period (August to September 2020 inclusive), appointments were switched to videoconferencing, with face‐to‐face only offered where clinically necessary (eg, for long‐acting injectable opioid agonist treatment). For patients unable to access videoconferencing, telephone appointments were offered.
The uptake of videoconferencing was low, comprising 21% (n = 47) of appointments conducted during lockdown versus 57% (n = 128) via telephone (Box). After the lockdown (November 2020 to February 2021), there was a gradual return to face‐to‐face appointments. Seven per cent (n = 28) of appointments were done via videoconferencing while 40% (n = 155) remained via telephone. Difficulties in connecting to the videoconferencing platform, poor audiovisual quality and time spent troubleshooting contributed to the low uptake of videoconferencing.
While telemedicine has been a convenient mode of health care delivery during the COVID‐19 pandemic,3 not all patients benefit from it. People accessing specialist addiction treatment are often from sociodemographic groups that are digitally excluded, such as the unemployed and people with low income or with disabilities.4 We found several barriers to telemedicine in our patient cohort. Many patients did not own a computer, had poor digital literacy, could not afford internet access or did not have privacy for consultations. Telephone appointments raise clinical gaps, with physical signs, mental state and visual cues unable to be assessed.
Digital inequality further marginalises an already vulnerable population. Access, affordability and digital ability issues need to be managed for telemedicine to be a viable option.4 Examples of how this might be achieved include the establishment of hubs with telemedicine facilities, technical support and private spaces, located at local community health centres for practicality and accessibility, along with providers offering more affordable internet plans for health care card holders.
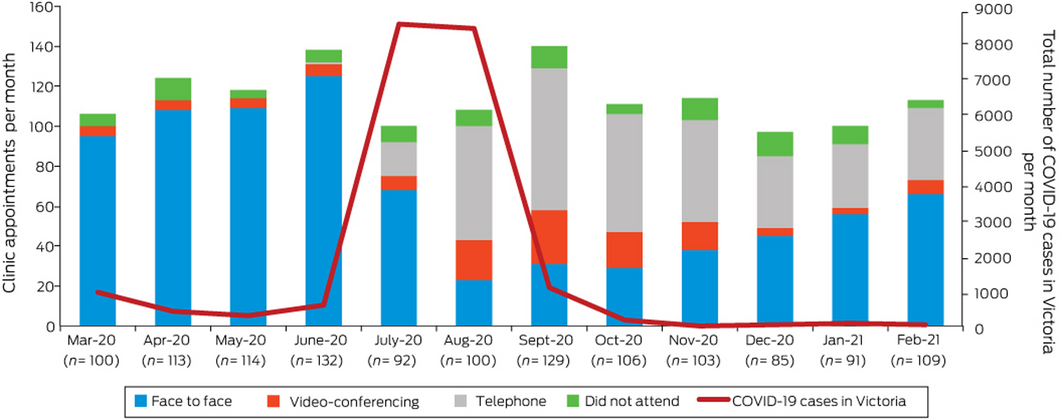
Box – Modality of clinic appointments by month during the coronavirus disease 2019 (COVID‐19)‐related restrictions in Melbourne, Victoria (total monthly COVID‐19 Victorian cases also shown2)
- 1. Snoswell CL, Caffery LJ, Haydon HM, et al. Telehealth uptake in general practice as a result of the coronavirus (COVID‐19) pandemic. Aust Heal Rev 2020; 44: 737–740.
- 2. Department of Health and Human Services, Victoria State Government. Victorian coronavirus (COVID‐19) data [website]. https://www.dhhs.vic.gov.au/victorian-coronavirus-covid-19-data (viewed May 2021).
- 3. Isautier JMJ, Copp T, Ayre J, et al. People’s experiences and satisfaction with telehealth during the COVID‐19 pandemic in Australia: cross‐sectional survey study. J Med Internet Res 2020; 22: e24531.
- 4. Thomas J, Barraket J, Wilson C, et al. Measuring Australia’s digital divide: the Australian digital inclusion index 2020 [website]. Melbourne: RMIT University and Swinburne University of Technology, 2020. https://apo.org.au/node/308474 (viewed May 2021).





Dan Lubman has provided consultancy advice to Lundbeck and Indivior and has received travel support and speaker honoraria from AstraZeneca, Indivior, Janssen, Lundbeck, Servier and Shire. Shalini Arunogiri has received speaker honoraria from Gilead, Janssen and Camurus for work unrelated to this study.