Primary care is the single most significant contributor to positive health outcomes,1,2 but the number of general practitioners in Australia has been falling, a situation previously described for nations with poorer health outcomes.2 The reasons for the decline are many,3 but this phenomenon has not been described in detail in the peer‐reviewed literature. We have therefore examined the registration categories, as recorded by the Australian Health Practitioner Regulation Agency (AHPRA), of people who graduated from the University of Western Australia (UWA) medical school during 1985–2007. Our study was approved by the UWA Human Research Ethics Committee (reference, RA 4/1/1627).
We included all active medical practitioners who graduated (MBBS) from UWA during 1985–2007 and were registered with AHPRA in December 2019. We included all doctors listed by AHPRA as practising GPs, whether vocationally registered or with college membership, in our GP category; 65 of the 93 1985–1987 graduates registered by AHPRA as GPs did not have postgraduate qualifications, but only five of the 56 2004–2007 graduates.
AHPRA registration as a GP was about half as likely for 2004–2007 graduates as for 1985–1987 graduates (relative risk [RR], 0.46; 95% confidence interval, 0.35–0.60). This decline in entry into general practice was accompanied by an increase in the proportion of graduates with general registration status alone (in 2004–2007 v 1985–1987: RR, 3.01; 95% CI, 1.97–4.61) (Box).
These findings are consistent with the recently reported drop in the proportion of medical graduates who intend to enter general practice,5 which may lead to a further decline in the number of AHPRA GP registrations. We also found an equally concerning increase in the number of doctors practising as generally registered practitioners alone during 2007–2019, presumably waiting for the opportunity to enter their preferred medical specialty. This problem, first discussed without data in the MJA in 2012,6 has not attracted the attention of policymakers.
The reduction in size of the primary care workforce is felt most keenly in rural communities, where dependence on primary health care is more pronounced, but urban practices also struggle to recruit new fellows.2 The causes of this problem include the perceived lower status of general practice, the generally lower income provided by Medicare fees, the burden of practice accreditation, and specialist‐focused teaching in medical schools. Further challenges for rural practice include problems of work–life balance and the focus on fly‐in/fly‐out specialist services instead of developing extended scope primary care models for regional and remote communities.
One limitation of our study is that the AHPRA general registration data need to be compared with college registries for accuracy. Our findings nevertheless suggest that solutions for the general practice problem are urgently needed if Australia is to continue enjoying some of the best health outcomes in the world.
Box – Category of registration for University of Western Australia medical graduates, 1985–2007, as recorded by the Australian Health Practitioner Regulation Agency (AHPRA)*
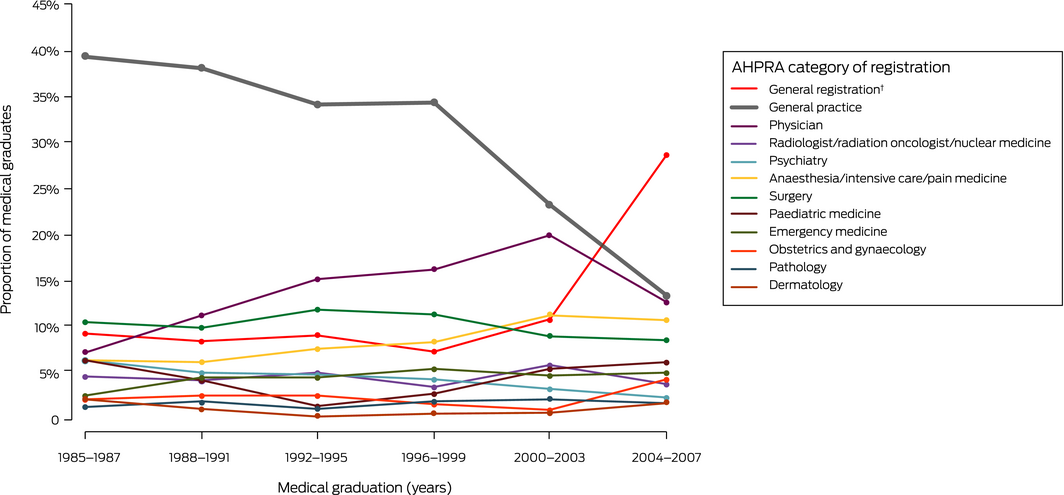
* Data as at 28 November 2019; data shown for categories with at least 25 graduates during 1985–2007. Total number of practising graduates registered with AHPRA, by graduation year: 1985–1987: 237; 1988–1991: 355; 1992–1995: 355; 1996–1999: 370; 2000–2003: 426; 2004–2007: 419. † Includes all medical graduates who have completed an accredited internship in Australia or New Zealand and are not required to complete any additional supervised practice to become eligible for general registration; those who completed a recognised internship elsewhere and have additionally satisfactorily completed 47 weeks of full‐time approved supervised practice in Australia; those who have previously held general registration in Australia; those who have completed the competent authority pathway; and Australian Medical Council certificate holders in the standard pathway who have completed a period of approved supervised practice in Australia.4
Received 9 October 2019, accepted 16 January 2020
- 1. Starfield B, Horder J. Interpersonal continuity: old and new perspectives. Br J Gen Pract 2007; 57: 527–529.
- 2. Basu S, Berkowitz SA, Phillips RL, et al. Association of primary care physician supply with population mortality in the United States, 2005–2015. JAMA Intern Med 2018; 179: 506–514.
- 3. Ianuzzi A. General practice: where the problems lie. MJA Insight [online], 25 June 2018. https://insightplus.mja.com.au/2018/2024/general-practice-where-the-problems-lie (viewed Mar 2020).
- 4. Medical Board of Australia. General registration. Updated Aug 2018. https://www.medicalboard.gov.au/Registration/Types/General-Registration.aspx (viewed Jan 2020).
- 5. Medical Deans Australia and New Zealand. Medical Schools Outcomes Database: national data report 2019. Data from final year students at Australian medical schools. Sept 2019. https://medicaldeans.org.au/md/2019/09/2019-MSOD-National-Data-Report-2014-2018-Full-report.pdf (viewed Jan 2020).
- 6. McNamara S. Does it take too long to become a doctor? Part 1: Medical school and prevocational training. Med J Aust 2012; 196: 528–530. https://www.mja.com.au/journal/2012/196/8/does-it-take-too-long-become-doctor.





No relevant disclosures.