The known: Concern is growing that psychotropic medicines are inappropriately prescribed in residential aged care facilities, but the extent to which prescribing changes after people enter residential care in Australia is unknown.
The new: The proportion of older people receiving psychotropic medicines is generally high before they enter residential aged care in Australia, but increases markedly after they enter care.
The implications: Psychotropic medication prescribing in residential aged care should be reduced by adopting evidence‐based non‐pharmacological strategies for behavioural management. The value of interventions that target prescribing of psychotropic medicines before and during the transition to residential aged care should be investigated.
Psychotropic medicines, including antipsychotics, benzodiazepines and antidepressants, are frequently prescribed for people in residential aged care facilities (RACFs) despite the associated high risk of adverse events.1,2 Antipsychotic drugs may be useful for people with severe mental health conditions, and risperidone is indicated for managing severe, persistent psychotic symptoms in people with dementia; benzodiazepines can be used to treat conditions such as sleep disturbance and anxiety. Psychotropic medicines can be appropriate if used in accordance with guidelines, at the lowest therapeutic doses, and with adequate monitoring. However, concerns about their use in RACFs as chemical restraints — that is, for influencing a person's behaviour — have grown in Australia and overseas.3
The authors of a recent national study of 150 Australian RACFs estimated that 22% of residents had received antipsychotics, 22% benzodiazepines, and 41% antidepressants.1 Moving to an RACF can be distressing for new residents because of the unfamiliar surroundings, the reduced contact with family, and the need to adapt to a new lifestyle;4 new residents may experience agitation, depression, and sleep disturbances after moving to the new environment.5 These problems may lead to increased prescribing of psychotropic medicines, but the extent to which Australians entering RACFs are already taking psychotropic medicines and how this changes after entering residential care is unknown. Understanding such changes is important for directing educational resources and quality improvement interventions that aim to limit the prescribing of psychotropic medicines.
Psychotropic medicine use has been reported to be markedly higher among people entering RACFs in Northern Ireland than for older people living in the community.6 Whether psychotropic medicine use changes when people living in the community move to RACFs has not been examined in a national study in Australia. The objective of our investigation was therefore to examine the dispensing of antipsychotic, benzodiazepine, and antidepressant medicines for older people in the year before and the year after they enter residential aged care. We also examined whether dementia status was associated with changes in the dispensing of psychotropic medicines.
Methods
Study design and data sources
For our retrospective cohort study, we analysed data from the Registry of Senior Australians (formerly: Registry of Older South Australians; ROSA).7 In Australia, older people can apply for 24‐hour care and accommodation in government‐subsidised RACFs. The eligibility and care needs of applicants for subsidised aged care are assessed by an Aged Care Assessment Team;8 after they enter an RACF, the core care needs of an individual are further assessed with the Aged Care Funding Instrument (ACFI).9 In ROSA, de‐identified individual data collected during eligibility assessments of applicants for subsidised aged care are linked to information about the aged care services received, medicines dispensed under the Pharmaceutical Benefits Scheme (PBS) and the Repatriation PBS, and mortality information from the National Death Index (Australian Institute of Health and Welfare). Data linkage criteria are detailed in the online Supporting Information.
Study cohort
We included data for all people in Australia who were at least 65 years old, or who identified as Aboriginal or Torres Strait Islander and were at least 50 years old, who entered permanent government‐subsidised residential aged care in Australia between 1 April 2008 (when the current ACFI was introduced) and 30 June 2015 (most recent available data), and had resided in government‐subsidised permanent residential aged care for at least three months (91 days). People without pharmaceutical concession cards were excluded (13 426 people) to ensure that data for all medicines of interest were captured in the pharmaceutical claims data. The date of entry to residential aged care was the first day of permanent residential care, or the first day of residential respite if the person did not return home between their respite stay and the start of permanent care.
Psychotropic medicines
Medicines dispensed to RACF residents during the year before and the year after entering an RACF were identified from World Health Organization Anatomical Therapeutic Classification (ATC) system codes:10 antipsychotics (N05A*; prochlorperazine and lithium were excluded, as they are not typically used in RACFs to treat behavioural and psychological symptoms), benzodiazepines and benzodiazepine derivatives (N05BA*, N05CD*, N05CF*, N03AE*), and antidepressants (N06A*).
Dementia status
Dementia status was defined according to information in aged care eligibility and ACFI assessments (Supporting Information, table 1), or by a resident being dispensed an acetylcholinesterase inhibitor (ATC codes N06DA02, N06DA03, N06DA04) or memantine (N06DX01) in the six months prior to entering care; these medicines are subsidised by the PBS only for treating the symptoms of dementia.
Statistical analysis
The demographic and other characteristics of residents were summarised as frequencies and percentages (categorical variables) or medians and interquartile ranges (IQRs) (continuous variables). Binary indicators for medicine use (medicine dispensed: yes or no) during each 91‐day time period (0–3 months, 3–6 months, 6–9 months, and 9–12 months before and after entry to care) were assessed in generalised linear mixed models; the prevalence of dispensing of each drug class (all residents and stratified by dementia status) were estimated by post‐estimation of the models. Models were adjusted for age, sex, location (state), and number of comorbid conditions (measured with the Rx‐Risk‐V, a validated comorbidity measure applied to pharmaceutical claims data11). For medicine use after entry to care, we also adjusted for psychotropic drug use during the three months preceding entry. Associations between dementia status at time of entry to residential care and dispensing of psychotropic medicines in the first three months of residential care were examined in Poisson regression models, and prevalence ratios (PRs) adjusted for age, sex, and number of comorbid conditions calculated. Statistical analyses were performed in Stata 15.0.
Ethics approval
Ethics approval for our study was granted by the University of South Australia (reference, ID 200489) and Australian Institute of Health and Welfare (reference, EO2018/1/418) Human Research Ethics Committees.
Results
The median age of the 322 120 included RACF residents was 85.0 years (IQR, 80.0–89.0 years); 205 582 were women (64%), 159 696 had dementia diagnoses (50%), and 10 734 had diagnoses of schizophrenia or other psychoses (3.3%) (Box 1). A total of 195 753 residents (60.8%; 95% confidence interval [CI], 60.6–60.9%) had received at least one psychotropic medicine during their first three months of residential care.
The prevalence of antipsychotic dispensing increased from 6.0% (95% CI, 5.9–6.1%) 9–12 months before entering residential care to 12.3% (95% CI, 12.2–12.4%) 0–3 months before entering residential care. A total of 68 483 residents (21.3%; 95% CI, 21.1–21.4%) received at least one antipsychotic during the first three months of residential care; prevalence was fairly stable during the subsequent nine months (Box 2). The most common atypical antipsychotics dispensed in the first three months of care were risperidone (42 080 residents, or 61.5% of those dispensed an antipsychotic), olanzapine (10 860 residents; 15.9%), and quetiapine (9685 residents; 14.1%); the most frequently dispensed typical antipsychotic was haloperidol (11 245 residents; 16.4%).
The prevalence of benzodiazepine dispensing increased from 17.1% (95% CI, 17.0–17.3%) 9–12 months before entering residential care to 19.7% (95% CI, 19.5–19.8%) 0–3 months before entering residential care. A total of 98 315 residents (30.5%; 95% CI, 30.4–30.7%) received at least one benzodiazepine during their first three months of residential care, and 75 414 residents (25.6%; 95% CI, 25.5–25.7%) 3–6 months after entering residential care; prevalence was fairly stable thereafter (Box 2). The most frequently dispensed benzodiazepines during the first three months in residential care were temazepam (61 098 residents, or 62.2% of those dispensed a benzodiazepine) and oxazepam (28 765; 29.3%).
The prevalence of antidepressant dispensing increased from 27.0% (95% CI, 26.9–27.1%) 9–12 months before entering residential care to 31.4% (95% CI, 31.2–31.5%) 0–3 months before entering residential care. A total of 122 224 residents (37.9%; 95% CI, 37.8–38.1%) received at least one antidepressant during their first three months of residential care (Box 2); 63 283 residents (51.8% of those dispensed an antidepressant) received selective serotonin reuptake inhibitors, 30 556 (25.0%) mirtazapine, and 19 011 (15.6%) tricyclic antidepressants. During the period 9–12 months after entering an RACF, 106 464 residents (41.4%; 95% CI, 41.2–41.5%) received at least one antidepressant (Box 2).
A considerable number of residents who received psychotropic medicines soon after entering care had not received them during the preceding year: 31 326 residents dispensed an antipsychotic (45.7%), 38 529 dispensed a benzodiazepine (39.2%), and 25 259 dispensed an antidepressant (19.8%) during the first three months of residential care had not been dispensed a drug from the corresponding class during the year prior to entering care.
Dementia status and psychotropic medicine dispensing
The prevalence of antipsychotic medicine dispensing during the first three months of residential care was higher for residents with dementia (32.9%; 95% CI, 32.7–33.2%) than for those without dementia (9.8%; 95% CI, 9.7–9.9%; PR, 3.37; 95% CI, 3.31–3.43). The prevalence of benzodiazepine dispensing was similar in both groups (with dementia: 30.3%; 95% CI, 30.1–30.5%; without dementia, 30.1%; 95% CI, 29.9–30.3%; PR, 1.01; 95% CI, 0.99–1.02). The prevalence of antidepressant dispensing was slightly higher among residents with dementia (39.0%; 95% CI, 38.8–39.2%) than among those without dementia (37.2%; 95% CI, 36.9–37.4%; PR, 1.05; 95% CI, 1.04–1.07) (Supporting Information, figures 1–3).
Discussion
In our study, which included all eligible older Australians who entered subsidised permanent residential care during 2008–15, the prevalence of psychotropic medicine dispensing increased markedly after people entered RACFs. Although dispensing had also increased during the year before entering residential care, the rise was greater during the first three months of care and the increased level of dispensing was maintained during the first year of care.
During their first three months in residential care, 21% of residents had received an antipsychotic, similar to the 22% reported by an earlier study1 that included 150 RACFs in seven Australian states and territories; the figures for antidepressant use were also similar (our study, 38%; earlier study, 41%). The same study1 found that 22% of residents had received benzodiazepines, whereas we found that 31% had received them during their first three months in residential care.
Our finding that psychotropic medicine dispensing increased after people entered residential care is consistent with the findings of a study in Northern Ireland6 and of two smaller studies: one in Melbourne including residents of seven RACFs,12 and a single RACF study in the United States.13 Of particular concern is that 20% (antidepressants) to 46% of residents (antipsychotics) in our study first received psychotropic medicines in residential care, probably indicating non‐adherence to psychotropic medicine prescribing guidelines. According to Australian clinical guidelines and PBS criteria, for example, risperidone is indicated only for treating mild to moderate behavioural symptoms in people with Alzheimer disease for up to 12 weeks.14
It has been estimated that only 10% of psychotropic medicine prescribing for treating the behavioural symptoms of people in residential care with dementia is appropriate.15 Psychotropic therapy, however, may be appropriate for some residents, and the possibility of relapse should be considered when contemplating withdrawal of psychotropic medicines. Residents should be carefully monitored when psychotropic therapy is discontinued; in a recent trial, prescribing of regular antipsychotics was subsequently resumed for 22% of people whose antipsychotic medicines had been deprescribed.16 Interdisciplinary, person‐centred interventions, including adequate support, education and training of care staff, improve psychotropic medicine prescribing in RACFs.1,16
People with dementia are often admitted to RACFs because of deteriorating behavioural symptoms, and this factor may contribute to increased psychotropic prescribing during the transition to residential care.17 Psychotropic therapy may help delay the need for residential care, but may also contribute to medicines‐related harm that increases the risk of admission.18 These complex relationships require further investigation.
Initiating psychotropic therapy in people entering residential care may be curbed by supporting residents with non‐pharmacological approaches to managing the behavioural and psychological symptoms of dementia, stress and insomnia. These approaches should be person‐centred, and a wide range of activities tailored to individual preferences, skills and abilities are available.14 Higher dispensing rates may be linked with a prescribing culture in RACFs that rely on psychotropic medicines as first‐line therapy.19 Sustained behavioural change is more likely when non‐pharmacological approaches to managing behavioural symptoms and staff training are emphasised throughout the entire organisation. The access of Australian RACF residents to psychologists and psychological services is poor, despite evidence for the effectiveness of psychological therapy for reducing depression in RACF residents.14,20 The availability of alternative treatments for people with depression living in RACFs should be improved.
Given the large proportions of people who were receiving psychotropic medicines before entering residential care, informal caregivers should also be better supported with regard to non‐pharmacological techniques. Multicomponent, non‐pharmacological interventions delivered by informal caregivers in the community could alleviate both the behavioural symptoms of dementia and caregiver distress without the risk of adverse events.21
In Australia, residential medication management reviews (RMMRs) are recommended when people enter residential care.22 These reviews are valuable for identifying and resolving medicines‐related problems and can reduce the prescribing of anticholinergic and sedative medicines.23 However, it is unclear whether every new RACF resident undergoes an RMMR, and it is unlikely that many residents undergo more than one during their stay. Adoption of recommendations arising from RMMRs is variable, but may be facilitated by interdisciplinary communication before and after the review.24 The impact of an RMMR is also related to the prescribing culture of the RACF; the resident's general practitioner and the RACF managers and staff must value the review for it to lead to changes in psychotropic medication prescribing.19 The Quality Use of Medicines program, established as a separate service from the RMMR in October 2011, aims to improve medicine use in RACFs, allows tailoring of services to the needs of individual RACFs and can include education and audit and feedback about psychotropic drug prescribing.22 Reducing the use of psychotropic medicines in RACFs will probably be challenging; requiring that antipsychotic prescribing patterns be reported has been suggested, for example, but these alone may not be an adequate measure of the quality of care.25
We found that antipsychotic dispensing during the first three months of residential care was markedly higher for people with than for those without dementia; antidepressant dispensing was slightly higher for residents with dementia, whereas benzodiazepine use was similar in the two groups. These findings highlight the particular need to re‐assess psychotropic medicine prescribing in RACFs for people with dementia.
Strengths and limitations
This is the first study to examine national patterns of psychotropic use before and after people enter RACFs. The ROSA cohort captures all admissions to government‐subsidised RACFs. Linking the ROSA data to the National Death Index and the very small likelihood of the people involved migrating or moving mean that loss to follow‐up was negligible. However, we did not have information on the indications for psychotropic therapy, the dose prescribed, or the frequency of use, and could therefore not assess the appropriateness of prescribing. We did not have information on medicines dispensed on private prescriptions or that were not PBS‐subsidised. We analysed prescription claims data, and therefore had no information about prescriptions issued but not dispensed, nor could we determine whether medicines were dispensed but not used, including those prescribed pro re nata. Further, medicines supplied to hospital inpatients are not PBS‐subsidised and only some Australian hospitals can supply PBS‐subsidised medicines at discharge. Consequently, initiation of the supply of psychotropic medicine may have been dated 0–3 months after entry to care if entry had immediately followed a hospital stay during which psychotropic therapy was commenced. We identified diagnoses of schizophrenia and other psychoses in aged care assessments, but, as these conditions are grouped on the assessment forms, we could not be more specific about the diagnoses. Dementia status was based on aged care assessments and the prescribing of specific medicines, but people with dementia that had not been formally diagnosed or recorded would have been misclassified. Finally, we did not examine changes in prescribing practices over time as it was beyond the scope of this investigation, although we plan to undertake such analyses in future.
Conclusion
Our national study found that dispensing of psychotropic medications increases markedly after people in Australia enter RACFs. Evidence from Australia and overseas suggests that interdisciplinary interventions could significantly reduce the level of prescribing. The underlying reasons for prescribing psychotropic medications should be investigated, and also whether interventions for reducing prescribing should target the periods before and during the transition to residential care. Prescribing cultures in RACFs need to be examined, and all residential aged care staff should be adequately educated and supported in reducing the reliance on psychotropic medicines for behavioural management.
Box 1 – Characteristics and mortality of residential aged care residents, April 2008 – June 2015, by psychotropic medicine dispensed during first three months of residential care
|
|
All residents |
Residents dispensed psychotropic medicines during first three months of residential care |
|||||||||||||
|
Antipsychotics |
Benzodiazepines |
Antidepressants |
None |
||||||||||||
|
|
|||||||||||||||
|
Total number of residents |
322 120 |
68 483 (21.3%) |
98 315 (30.5%) |
122 224 (37.9%) |
126 367 (39.2%) |
||||||||||
|
Age (years), median (IQR) |
85.0 (80.0–89.0) |
83.0 (77.0–87.0) |
84.0 (79.0–89.0) |
83.0 (78.0–88.0) |
86.0 (81.0–90.0) |
||||||||||
|
Sex (women) |
205 582 (63.8%) |
38 911 (56.8%) |
63 348 (64.4%) |
80 835 (66.1%) |
80 571 (63.8%) |
||||||||||
|
State/territory |
|
|
|
|
|
||||||||||
|
New South Wales |
108 518 (33.7%) |
22 307 (32.6%) |
26 257 (26.7%) |
37 778 (30.9%) |
47 488 (37.6%) |
||||||||||
|
Victoria |
84 141 (26.1%) |
18 720 (27.3%) |
29 167 (29.7%) |
32 394 (26.5%) |
31 059 (24.6%) |
||||||||||
|
Queensland |
58 419 (18.1%) |
12 721 (18.6%) |
19 703 (20.0%) |
23 793 (19.5%) |
21 121 (16.7%) |
||||||||||
|
South Australia |
30 934 (9.6%) |
6485 (9.5%) |
11 545 (11.7%) |
12 099 (9.9%) |
11 170 (8.8%) |
||||||||||
|
Western Australia |
26 979 (8.4%) |
5774 (8.4%) |
7961 (8.1%) |
11 250 (9.2%) |
10 097 (8.0%) |
||||||||||
|
Tasmania |
9162 (2.8%) |
1801 (2.6%) |
3131 (3.2%) |
3572 (2.9%) |
3437 (2.7%) |
||||||||||
|
Australian Capital Territory |
3230 (1.0%) |
567 (0.8%) |
451 (0.5%) |
1149 (0.9%) |
1558 (1.2%) |
||||||||||
|
Northern Territory |
737 (0.2%) |
108 (0.2%) |
100 (0.1%) |
189 (0.2%) |
437 (0.4%) |
||||||||||
|
Comorbidity score (Rx‐Risk‐V), median (IQR) |
5 (3–7) |
5 (3–7) |
6 (4–8) |
6 (4–8) |
4 (2–6) |
||||||||||
|
Dementia diagnosis |
159 696 (49.6%) |
52 423 (76.6%) |
47 012 (47.8%) |
59 058 (48.3%) |
57 194 (45.3%) |
||||||||||
|
Schizophrenia/other psychosis diagnosis |
10 734 (3.3%) |
7877 (11.5%) |
3579 (3.6%) |
4327 (3.5%) |
1433 (1.1%) |
||||||||||
|
Deaths after entering care |
|
|
|
|
|
||||||||||
|
3–6 months |
27 428 (8.5%) |
7159 (10.5%) |
10 167 (10.3%) |
10 739 (8.8%) |
9137 (7.2%) |
||||||||||
|
6–9 months |
20 218 (6.3%) |
4799 (7.0%) |
6876 (7.0%) |
7512 (6.2%) |
7480 (5.9%) |
||||||||||
|
9–12 months |
17 239 (5.4%) |
4118 (6.0%) |
5639 (5.7%) |
6522 (5.3%) |
6395 (5.1%) |
||||||||||
|
|
|||||||||||||||
|
IQR = interquartile range. |
|||||||||||||||
Box 2 – Dispensing of psychotropic medicines before and after entering residential aged care (with 95% confidence intervals), by class and 91‐day quarter*
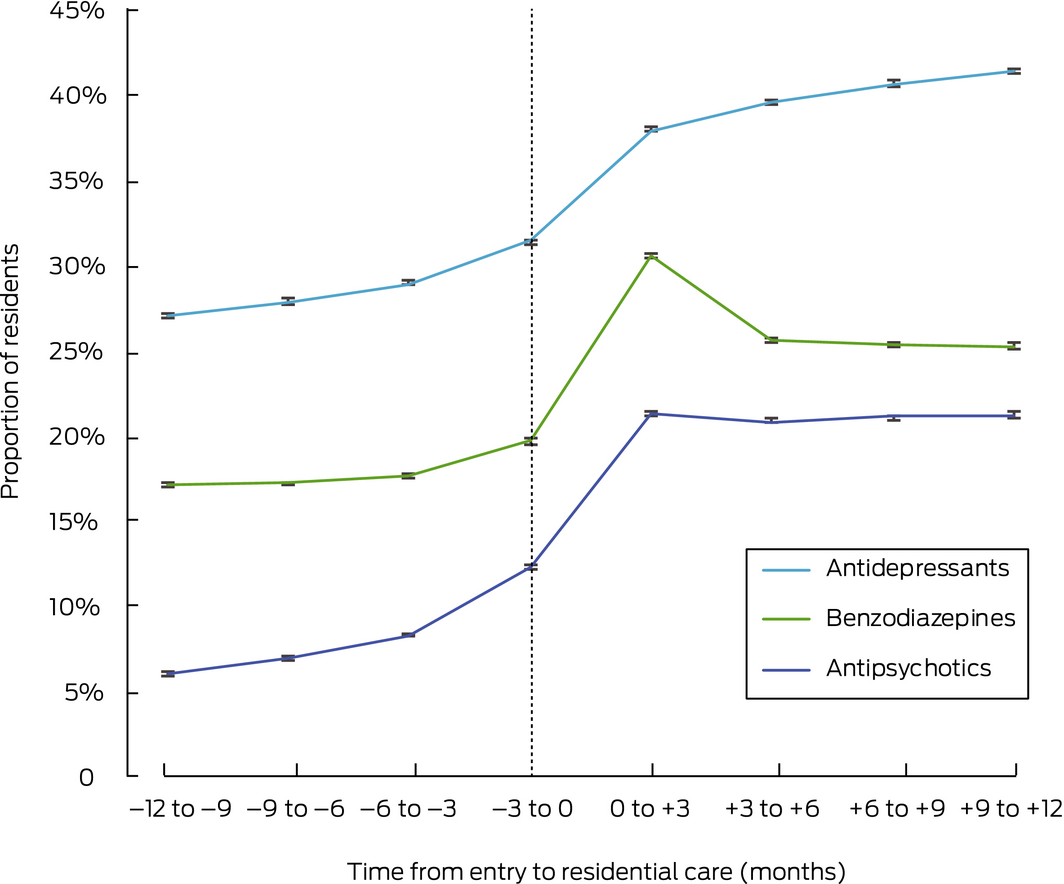
* Adjusted for age, sex, number of comorbid conditions, and location (state); prevalence after entering care also adjusted for use of antipsychotic, benzodiazepine, or antidepressant in the three months preceding care. Number of people: prior to residential care and first three months of residential care: 322 120; 3–6 months after entering care, 294 692; 6–9 months, 274 474; 9–12 months, 257 235.
Received 3 August 2019, accepted 22 November 2019
- Stephanie L Harrison1,2
- Janet K Sluggett1,3
- Catherine Lang1
- Craig Whitehead4
- Maria Crotty5
- Megan Corlis6
- Steven L Wesselingh7
- Maria C Inacio1,8
- 1 Registry of Senior Australians, South Australian Health and Medical Research Institute, Adelaide, SA
- 2 Liverpool Centre for Cardiovascular Science, University of Liverpool and Liverpool Heart and Chest Hospital, Liverpool, United Kingdom
- 3 Centre for Medicine Use and Safety, Monash University, Melbourne, VIC
- 4 Southern Adelaide Local Health Network, SA Health, Adelaide, SA
- 5 Flinders University, Adelaide, SA
- 6 Helping Hand Aged Care, Adelaide, SA
- 7 South Australian Health and Medical Research Institute, Adelaide, SA
- 8 Sansom Institute for Health Research, University of South Australia, Adelaide, SA
The South Australian Department of Innovation and Skills funded this study with a grant from the Premier's Research and Industry Fund. The funders had no role in study design, methods, data collection and analysis, decision to publish, or preparation of this manuscript.
No relevant disclosures.
- 1. Westbury JL, Gee P, Ling T, et al. RedUSe: reducing antipsychotic and benzodiazepine prescribing in residential aged care facilities. Med J Aust 2018; 208: 398–403. https://www.mja.com.au/journal/2018/208/9/reduse-reducing-antipsychotic-and-benzodiazepine-prescribing-residential-aged
- 2. Westbury J, Gee P, Ling T, et al. More action needed: psychotropic prescribing in Australian residential aged care. Aust N Z J Psychiatry 2018; 53: 136–147.
- 3. Royal Commission into Aged Care Quality and Safety. Restrictive practices in residential aged care in Australia (Background paper 4). May 2019. https://agedcare.royalcommission.gov.au/publications/Documents/background-paper-4.pdf (viewed Aug 2019).
- 4. Bradshaw SA, Playford ED, Riazi A. Living well in care homes: a systematic review of qualitative studies. Age Ageing 2012; 41: 429–440.
- 5. NHS England. Optimising treatment and care for people with behavioural and psychological symptoms of dementia: a best practice guide for health and social care professionals. 2017. http://medicine.exeter.ac.uk/media/universityofexeter/medicalschool/pdfs/nhs-dementia-best-practice-guide.pdf (viewed Aug 2019).
- 6. Maguire A, Hughes C, Cardwell C, et al. Psychotropic medications and the transition into care: a national data linkage study. J Am Geriatr Soc 2013; 61: 215–221.
- 7. Inacio MC, Bray SCE, Whitehead C, et al. Registry of Older South Australians (ROSA): framework and plan. BMJ Open 2019; 9: e026319.
- 8. Australian Institute of Health and Welfare. Aged care assessment program: data dictionary, version 1.0 (Cat. no. AGE 26). Canberra: AIHW, 2002. https://www.aihw.gov.au/reports/aged-care/aged-care-assessment-program-data-dictionary-versi/contents/table-of-contents (viewed July 2019).
- 9. Australian Department of Health. Aged Care Funding Instrument (ACFI) user guide. Updated Feb 2018. https://agedcare.health.gov.au/funding/aged-care-subsidies-and-supplements/residential-care-subsidy/basic-subsidy-amount-aged-care-funding-instrument/aged-care-funding-instrument-acfi-user-guide (viewed June 2019).
- 10. World Health Organization. ATC/DDD Index, 2019. Updated Dec 2018. https://www.whocc.no/atc_ddd_index (viewed July 2019).
- 11. Pratt NL, Kerr M, Barratt JD, et al. The validity of the Rx‐Risk Comorbidity Index using medicines mapped to the Anatomical Therapeutic Chemical (ATC) classification system. BMJ Open 2018; 8: e021122.
- 12. O'Connor DW, Griffith J, McSweeney K. Changes to psychotropic medications in the six months after admission to nursing homes in Melbourne, Australia. Int Psychogeriatr 2010; 22: 1149–1153.
- 13. Cohen‐Mansfield J, Lipson S, Gruber‐Baldini AL, et al. Longitudinal prescribing patterns of psychotropic drugs in nursing home residents. Exp Clinical Psychopharm 1996; 4: 224–233.
- 14. Laver K, Cumming RG, Dyer SM, et al. Clinical practice guidelines for dementia in Australia. Med J Aust 2016; 204: 191–193. https://www.mja.com.au/journal/2016/204/5/clinical-practice-guidelines-dementia-australia
- 15. van der Spek K, Gerritsen DL, Smalbrugge M, et al. Only 10% of the psychotropic drug use for neuropsychiatric symptoms in patients with dementia is fully appropriate. The PROPER I‐study. International Psychogeriatr 2016; 28: 1589–1595.
- 16. Brodaty H, Aerts L, Harrison F, et al. Antipsychotic deprescription for older adults in long‐term care: the HALT study. J Am Med Dir Assoc 2018; 19: 592–600.e7.
- 17. Toot S, Swinson T, Devine M, et al. Causes of nursing home placement for older people with dementia: a systematic review and meta‐analysis. International Psychogeriatr 2017; 29: 195–208.
- 18. Nerius M, Johnell K, Garcia‐Ptacek S, et al. The impact of antipsychotic drugs on long‐term care, nursing home admission, and death in dementia patients. J Gerontol A Biol Sci Med Sci 2018; 73: 1396–1402.
- 19. Sawan MJ, Jeon YH, Fois RJ, Chen TF. A qualitative study exploring visible components of organizational culture: what influences the use of psychotropic medicines in nursing homes? Int Psychogeriatr 2016; 28: 1725–1735.
- 20. Stargatt J, Bhar SS, Davison TE, et al. The availability of psychological services for aged care residents in Australia: a survey of facility staff. Aust Psychol 2017; 52: 406–413.
- 21. Brodaty H, Arasaratnam C. Meta‐analysis of nonpharmacological interventions for neuropsychiatric symptoms of dementia. Am J Psychiatry 2012; 169: 946–953.
- 22. Pharmaceutical Society of Australia. Guidelines for pharmacists providing Residential Medication Management Review and Quality Use of Medicines services. Oct 2011. https://my.psa.org.au/servlet/fileField?entityId=ka17F000000cmjcQAA&field=PDF_File_Member_Content__Body__s (viewed Aug 2019).
- 23. Nishtala PS, Hilmer SN, McLachlan AJ, et al. Impact of residential medication management reviews on drug burden index in aged‐care homes. Drugs Aging 2009; 26: 677–686.
- 24. Chen EYH, Wang KN, Sluggett JK, et al. Process, impact and outcomes of medication review in Australian residential aged care facilities: a systematic review. Australas J Ageing 2019; Suppl 2: 9–25.
- 25. Maust DT, Kim HM, Chiang C, Kales HCl. Association of the Centers for Medicare & Medicaid Services’ National Partnership to Improve Dementia Care with the use of antipsychotics and other psychotropics in long‐term care in the United States from 2009 to 2014. JAMA Intern Med 2018; 178: 640–647.





Abstract
Objective: To examine the prevalence of psychotropic medicine dispensing before and after older people enter residential care.
Design: Retrospective national cohort study; analysis of Registry of Senior Australians (ROSA) data.
Setting, participants: All concession card‐holding residents of government‐subsidised residential aged care facilities in Australia who entered residential care for at least three months between 1 April 2008 and 30 June 2015.
Main outcome measures: Proportions of residents dispensed antipsychotic, benzodiazepine, or antidepressant medicines during the year preceding and the year after commencing residential care, by quarter.
Results: Of 322 120 included aged care residents, 68 483 received at least one antipsychotic (21.3%; 95% CI, 21.1–21.4%), 98 315 at least one benzodiazepine (30.5%; 95% CI, 30.4–30.7%), and 122 224 residents at least one antidepressant (37.9%; 95% CI, 37.8–38.1%) during their first three months of residential care; 31 326 of those dispensed antipsychotics (45.7%), 38 529 of those dispensed benzodiazepines (39.2%), and 25 259 residents dispensed antidepressants (19.8%) had not received them in the year preceding their entry into care. During the first three months of residential care, the prevalence of antipsychotic (prevalence ratio [PR], 3.37; 95% CI, 3.31–3.43) and antidepressant dispensing (PR, 1.05; 95% CI, 1.04–1.07) were each higher for residents with than for those without dementia; benzodiazepine dispensing was similar for both groups (PR, 1.01; 95% CI, 0.99–1.02).
Conclusions: Dispensing of psychotropic medicines to older Australians is high before they enter residential care but increases markedly soon after entry into care. Non‐pharmacological behavioural management strategies are important for limiting the prescribing of psychotropic medicines for older people in the community or in residential care.