The known: The proportion of twins born by caesarean delivery has increased in Australia.
The new: The proportion of twins born by caesarean delivery in Victoria increased threefold, from 24% to 71% of all twin births, during 1983–2015. The proportion of twin births with twin pregnancy as the sole indication for caesarean delivery increased from 2% to 21%. The proportion of twin births by caesarean delivery differs between Victorian regions.
The implications: Exploring interventions that safely reduce the reliance on caesarean delivery of twins would be appropriate.
About 2% of all pregnancies in Australia are twin pregnancies, but perinatal mortality and morbidity are disproportionately high for these pregnancies.1,2 The numbers of twin births by caesarean delivery have been increasing worldwide,3,4,5 and there have been calls to reduce the overall number of caesarean deliveries in countries with high rates, including Australia.6,7 While factors that influence its use in singleton pregnancies have been investigated, including maternal age, parity, and obesity,8 caesarean delivery of twins has received less attention. Given high level evidence that routine caesarean delivery of twins does not benefit mothers or babies9,10 and the recent suggestion that vaginal birth may actually be preferable,11 the mode of birth in uncomplicated twin pregnancies should be considered carefully.
In this study, we examined changes in the mode of delivery of twins in Victoria over 33 years, with a view to identifying opportunities for improving care and outcomes for women and their babies.
Methods
For our retrospective population‐based study, we analysed de‐identified data on births in Victoria of at least 20 weeks' gestation from the Consultative Council on Obstetric and Paediatric Mortality and Morbidity (CCOPMM) dataset, the accuracy of which has been validated.12 Data for all twin births during 1 January 1983 – 31 December 2015 were included; we included women only once each by selecting birth records for the first‐born twin. For comparative purposes, we also analysed data for singleton births during 1 January 1992 – 31 December 2015.
For some analyses, we analysed the data in three epochs: 1983–1998, 1999–2008, and 2009–2015. We compared the demographic characteristics of women who gave birth to twins during the first epoch with those of the third epoch in χ2 tests. We assessed changes in the proportions of modes of birth over time (vaginal, planned or unplanned caesarean delivery) in χ2 tests for trend. We also analysed these changes by logistic regression; adjusting for changes in maternal age and parity, we report adjusted odds ratios (aORs) with 95% confidence intervals (CIs) for caesarean delivery during each of the second and third epochs compared with the first epoch.
Indications for caesarean delivery of twins
We examined changes in the indications for caesarean delivery, separately for planned and unplanned deliveries, in eight categories based on International Classification of Diseases, 9th (ICD‐9) (until 1998) or 10th modification (ICD‐10) (after 1998) codes:
- previous caesarean delivery (6542; O342);
- placentation problems (6410–6412, 6418, 6419, 6635; O440, O441, O459, O468, O469, O679, O694);
- malpresentation (6520, 6522–6529, 6600, 6696; O320–O329, O641–O643, O645, O649);
- hypertensive disorders (6420, 6422–6426, 6429; O100, O139, O141, O152, O149, O159);
- non‐reassuring fetal status (typically abnormal cardiotocography; 6563, 6630, 6633; O680–O682, O688–O690, O692);
- failure to progress (6601, 6603, 6606–6612, 6620–6622, 6534, 6591, 6604, 6590; O610, O611, O618, O620, O622, O630, O631, O639, O640, O664, O665, O668, O669);
- other (including polyhydramnios, oligohydramnios, gestational diabetes, pre‐existing diabetes, chorio‐amnionitis) (6584; O409, O410, 6480, O244, O243);
- twin pregnancy (6510; O300).
When more than one coded indication was recorded for a birth, we included the indication positioned highest in this list as the primary indication (ie, the most important indicator for caesarean delivery). We assessed changes in proportions of indications over time in χ2 tests for trend.
We also examined changes in indications for caesarean delivery over time by maternal age group (under 35 years, 35 years or older) and parity (nulliparous, parous). The proportions of each type of caesarean delivery in the first and third epochs for each indication were compared with those for all other indications in χ2 tests. We deemed P < 0.01 statistically significant.
Regional differences
We compared regional levels of recorded indications for caesarean delivery during 2010–2015 (excluding 2014, for which “region” data were not available) by multiple logistic regression adjusted for maternal age group, parity, body mass index group, admission type (public, private), previous caesarean delivery, and use of artificial reproductive technology. The North and West Metropolitan region, which had the highest number of twin births, served as the reference region.
Statistical analyses were undertaken in SPSS Statistics 25 (IBM) and Stata 15 (StataCorp).
Ethics approval
The study was approved by the Monash Health Human Research Ethics Committee (reference, 12126L).
Results
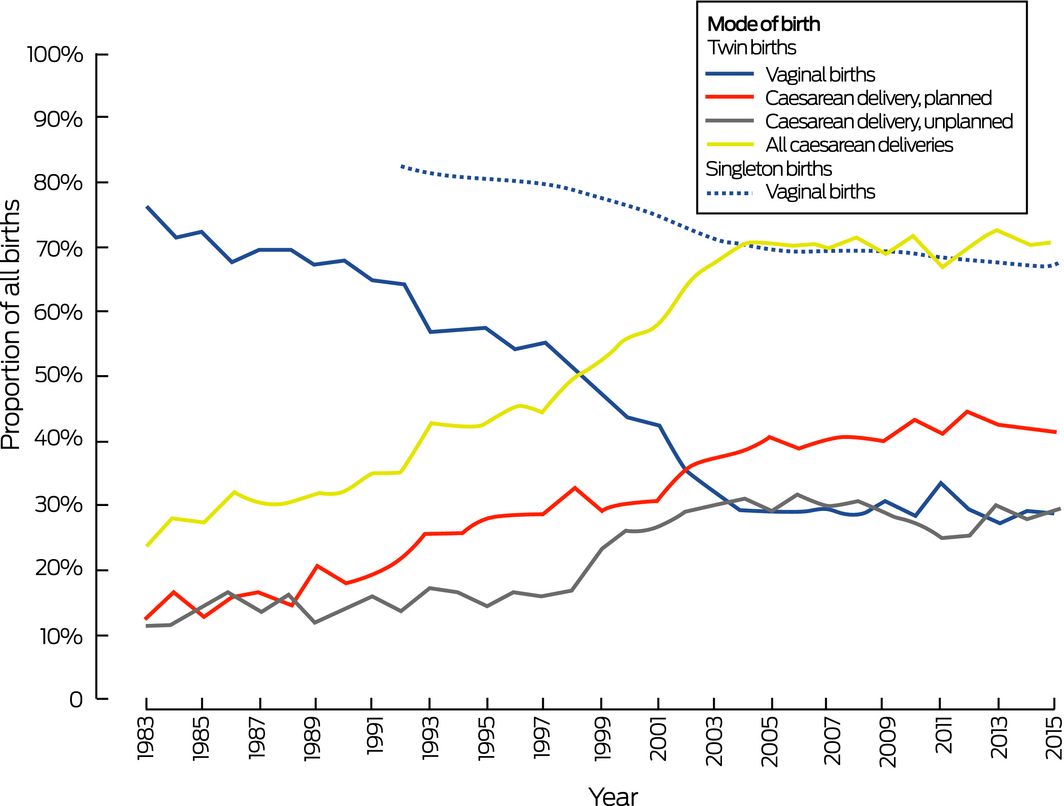
There were 32 187 twin pregnancies (live and stillbirths) in Victoria during 1983–2015. The proportion of twin births by caesarean delivery rose from 24% (156 of 658 twin deliveries) in 1983 to 71% (782 of 1102 deliveries) in 2015; the number of planned caesarean deliveries increased from 84 (13%) to 459 (42%) and that of unplanned caesarean deliveries from 72 (11%) to 323 (29%) (in each case: for trend, P < 0.001). Conversely, the proportion of vaginal twin births declined from 76% (502 of 658 twin deliveries) in 1983 to 29% in 2015 (320 of 1102 deliveries; P < 0.001) (Box 1). After adjusting for maternal age and parity, the odds of caesarean delivery were greater during both 1999–2008 (aOR, 2.9; 95% CI, 2.8–3.4) and 2009–2015 (aOR, 3.6; 95% CI, 3.4–3.8) than during 1983–1998.
The rate of increase in the proportion of twin births by caesarean delivery was steepest during 1983–2003, with no substantial change since 2004. For the 1 647 245 singleton pregnancies during 1992–2015, the proportion of vaginal births declined from 82% (52 682 of 64 521 births) in 1992 to 67% (51 410 of 76 617 births) in 2015; the decline was most marked during 1997–2003 (Box 1).
The proportion of women with twin pregnancies who were aged 35 years or more increased from 15.4% (2007 mothers) during 1983–1998 to 32.6% (2560 mothers) during 2009–2015 (P < 0.001); the proportion of nulliparous women increased from 40.1% (5247 mothers) to 45.5% (3618 mothers) (P < 0.001) (Box 2).
Indications for caesarean delivery of twins
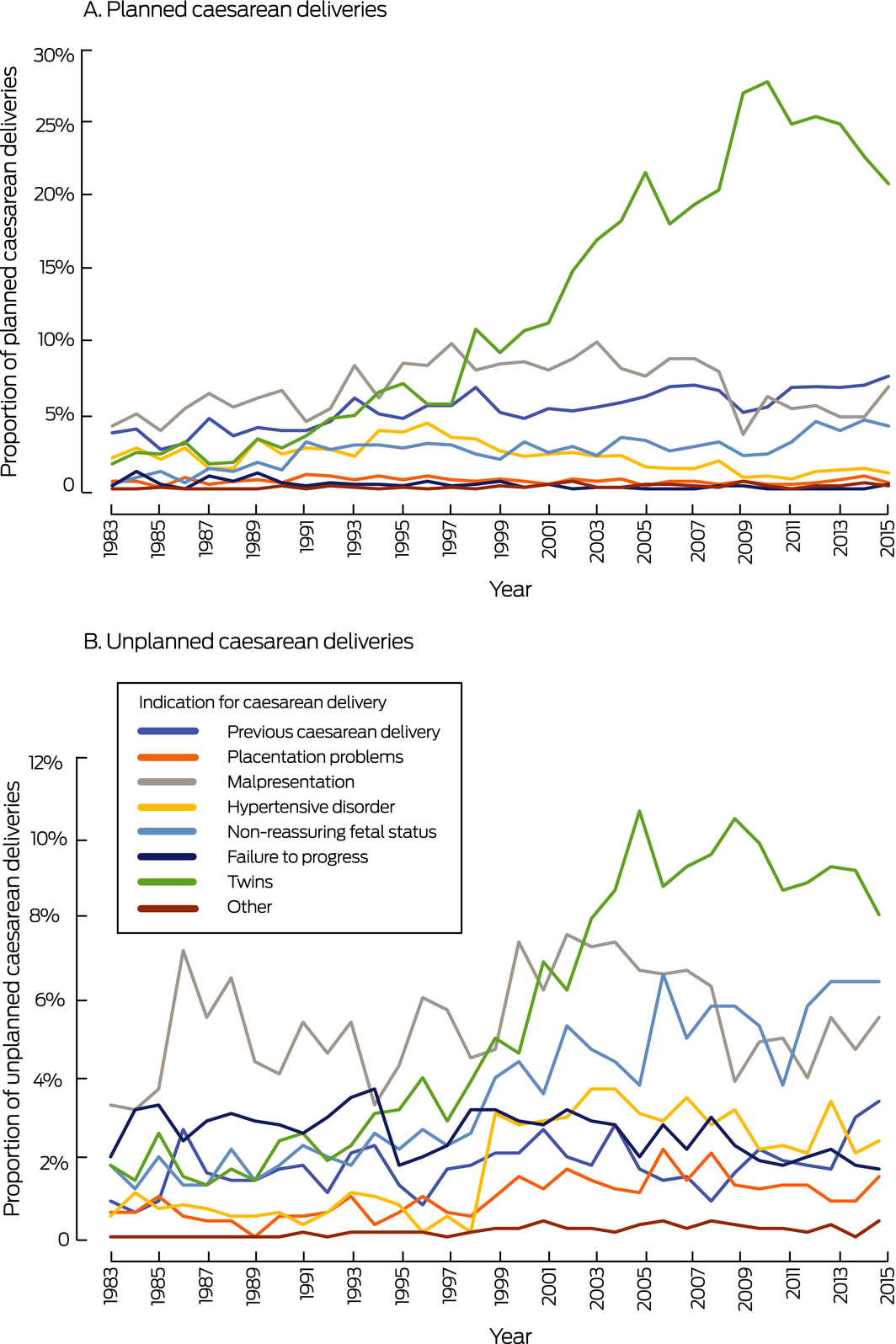
The number of planned caesarean deliveries with twin pregnancy as the indication increased from 12 of 658 (1.8%) in 1983 to 231 of 1102 births (21%) in 2015, and that of unplanned caesarean deliveries from 16 of 658 (2.4%) to 93 of 1102 births (8.4%) (in each case: for trend, P < 0.001). These were the most marked rises for any single indication. The proportion of planned caesarean deliveries with previous caesarean delivery as the principal indication increased from 3.8% (25 of 658 deliveries) in 1983 to 7.7% (85 of 1102 deliveries) in 2015; the proportion of unplanned caesarean deliveries with this indication increased from 0.9% (six of 658 deliveries) to 3.4% (38 of 1102 deliveries; in each case: for trend, P < 0.001). The proportion of planned caesarean deliveries with non‐reassuring fetal status as primary indication increased from 0.3% (two of 658 deliveries) to 4.3% (47 of 1102 deliveries; P < 0.001) and of unplanned caesarean deliveries from 1.8% (12 of 658 deliveries) to 6.4% (70 of 1102 deliveries; for trend, P < 0.001) (Box 3).
For both age groups (under 35 years, 35 years or more; Box 4) and both parity groups (nulliparous, parous; Box 5), the most common indication for caesarean delivery (both planned and unplanned) during 1983–1998 was malpresentation, but twin pregnancy was the most common indication for all groups during 2009–2015. There were no other consistent changes between epochs.
During 2009–2015, two or more indications were recorded for 2401 caesarean twin deliveries (43%) and for 36 678 caesarean singleton deliveries (22%).
Regional differences
In Gippsland, the Victorian health region with the lowest rate of caesarean delivery of twins during 2010–2013 (100 of 187 deliveries, 54%), the proportion of caesarean twin deliveries with twin pregnancy as the sole indication was also relatively low (31 of 100 caesarean deliveries, 31%) (Box 6). After adjusting for potential confounders, the odds of caesarean delivery of twins were lower than those for the reference region (North and West Metro) in the Gippsland, Eastern Metropolitan, Hume, and Southern Metropolitan regions, and non‐significantly higher in the Barwon–South Western region (Box 7).
Discussion
The proportion of twins born in Victoria by caesarean delivery almost tripled during 1983–2015. This change appears linked with the rises in the proportions of all twin births and of twin caesarean deliveries for which the twin pregnancy was the sole indication for caesarean delivery; these rises applied to both younger (under 35 years) and older mothers and to both nulliparous and parous women.
The increased proportion of twins born by caesarean delivery in Victoria mirrors trends in other parts of Australia13,14 and overseas.4,5,7 The proportion of caesarean delivery twin births in Victoria in 2015 (71%) was similar to that for multiple births in Australia overall (69%)14 and in some high income nations, including the United States (92%),4 Germany (75%) and Scotland (73%),5 but higher than in most European countries, and much higher than in Scandinavia (47–60%), the Netherlands (44%), and England (63%).5 The increasing use of caesarean section for twin births in Victoria is not explained by changes in maternal age or parity. We were unable to explore the significance of increasing rates of assisted reproduction or improved detection of twin–twin transfusion syndrome for caesarean delivery rates because the CCOPMM dataset has captured relevant data only very recently. However, most twin pregnancies are unassisted and the rate of severe twin–twin transfusion syndrome is very low; only 49 twin pregnancies with the syndrome required laser photocoagulation in Victoria during 2006–2011.15 It is therefore improbable that these factors explain the tripling of the twin caesarean delivery proportion.
The increase in the proportion of twins born by caesarean delivery has been accompanied by a marked rise in the proportion of such deliveries with twin pregnancy as the reason for surgery; removing interventions with this factor as the main indication would reduce the twin caesarean delivery proportion in Victoria to 40–50%. Our data cannot provide insights into the reasons for an apparent change in preference regarding twin births. Information is not collected on whether the mother, her obstetrician, or both preferred caesarean delivery to a planned vaginal birth. When the value of caesarean delivery is uncertain for women with a particular indication, such as twin pregnancy, clinical practice may be more influenced by professional and socio‐cultural factors that more generally influence views about caesarean delivery.5 That is, in countries with a generally higher caesarean delivery rate, including Australia, this preference also applies to twin births. It is notable that the region in our study with the lowest adjusted odds of twin caesarean delivery, Gippsland, has one of the lowest overall caesarean delivery rates in Victoria, including a low rate of elective repeat caesarean deliveries.16
If reducing the proportion of children born by caesarean delivery is desirable,7 understanding the cultural influences underlying birth decisions is essential. In a 2004 study, most Canadian women bearing twins preferred vaginal birth,17 but data on the preferences of Australian women have not been reported. Twin pregnancies are more common in older women, in women with a high body mass index, and in women conceiving with assisted reproduction support,2,14 and these women and their obstetricians might prefer caesarean delivery if vaginal birth is regarded as more risky. However, vaginal delivery of twins is not less safe than a planned caesarean delivery, although high level evidence has only recently been reported. Earlier retrospective cohort studies had suggested that caesarean delivery was the safer option,18,19 but a more recent multicentre, randomised controlled trial coordinated in Canada but including several Australian hospitals (published in 2013)9 and a systematic review (2015)10 did not confirm this view. The shifting direction of the evidence may have influenced women's decisions, but we found that the proportion of twins born by caesarean delivery in Victoria has been stable since 2003; that is, well before any of these reports were published, suggesting that the cultural shift may have had other reasons.
The rise in the proportion of caesarean twin deliveries may principally reflect clinician preference, a possibility supported by the regional variation in caesarean delivery rates we found. Changes in clinician preference may be partly explained by increasing awareness that earlier delivery of twins improves outcomes for the children,13,20 leading to induced labour or planned caesarean deliveries being preferred. Until fairly recently, inducing labour was thought to increase the risk of an emergency caesarean delivery,21 and, given the extra risk associated with twin pregnancies, a planned caesarean delivery could reasonably be seen as the better option.
The preference for caesarean delivery of twins may also reflect changes in clinician training, skills, and confidence with vaginal twin births;22 clinicians with limited experience are more likely to prefer caesarean to vaginal deliveries.23 If women are to make meaningful choices about how their children are born, a skilled specialist workforce must be maintained. But, as fewer than one‐third of twins are now born by vaginal delivery, the opportunity for obstetric trainees to become proficient in twin vaginal births is much more limited than it once was. This problem is not restricted to Victoria or to twin births; the number of specialist trainees performing operative vaginal deliveries of any sort has declined in Australia over the past few decades.24,25 In 2007, only one in ten Australian obstetric trainees planned to offer vaginal birth for breech presentations after completing training,24 and only one in five intended to undertake rotational forceps deliveries.25
Obstetric trainees want more training in vaginal twin births.22 Increasing the rate of twin vaginal births would require guided mentorship, among other specific measures, an approach that has reversed declining rates of obstetric forceps use.26 That the proportion of planned caesarean deliveries for twins has been stable over the past decade suggests that training in vaginal twin births is still feasible; the recent decline in planned caesarean deliveries with twin pregnancy as the sole indication (Box 3) may reflect changes in clinician preference stimulated by evidence of the safety of vaginal delivery.9 The Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG) curriculum for the training of specialist obstetricians and gynaecologists requires that trainees are able to “safely manage and conduct all obstetric procedures involved in intrapartum care … including a detailed knowledge of … vaginal twin birth”,27 but a trainee is required to attend a total of only 20 complex vaginal births (twin births, breech births, other unspecified complications).
Given calls to reduce caesarean delivery rates in general7 and the safety of vaginal delivery for twin births,9,10 it would be desirable to increase the twin vaginal birth rate in Australia. Increasing caesarean delivery of twins is not explained by the complexity of twin pregnancies nor by rates of maternal comorbid conditions.28 Had all Victorian women who gave birth to twins by caesarean delivery in 2015 with twin pregnancy as the sole indication attempted vaginal birth, and half of these attempts were successful (as generally reported9,11), the vaginal birth rate for twins would have been 15 percentage points higher (rising from 29% to 44%), similar to those of France, Sweden and the Netherlands (46–56%).5 This is feasible; nearly half the twin births in Gippsland during 2010–13 were vaginal births.
The challenge for Victorian and other Australian obstetricians is to re‐examine current practice and, in the light of evidence, decide to change and “bend the cesarean‐delivery curve for twin pregnancies”.29 However, the choice of birth mode ultimately lies with the mother if there are no complicating factors.30
Strengths and limitations
One strength of our study is that we have specifically explored the indications for caesarean delivery of twins, not simply changes in the rate of caesarean twin deliveries.3 Further, as we analysed whole‐of‐population data, our findings can probably be generalised across Australia, to high and low risk pregnancies, private and public care, and to metropolitan and regional services.
There are two key limitations to our study. As caesarean delivery has become increasingly accepted for delivering twins, clinicians may have be more likely to list twin pregnancy as the sole indication rather than specifying another salient reason. This would inflate the number of deliveries with twin pregnancy as the sole indication. However, two or more indications were recorded for 43% of twin caesarean delivery births, twice the rate for singleton caesarean deliveries, suggesting that indications are not under‐reported. Our selecting the records for the first‐born twin means that a small proportion of births in which the first twin was born vaginally and the second by emergency intrapartum caesarean delivery will have been included in the vaginal birth group. This occurs in only 1% of all twin births (data not shown), and would, in any case, have diluted the effect we have described.
Conclusion
We found that the proportion of twins born by caesarean delivery in Victoria almost tripled during 1983–2015. The proportion of twin caesarean deliveries, however, differed considerably between regions. Our findings are probably generalisable, and therefore have implications for women, their babies, and obstetric practice across Australia. We should ensure that we have a skilled and competent workforce to enable women to have a real choice in how their babies are born.
Box 2 – Characteristics of women giving birth to twins in Victoria, 1983–2015
|
|
1983–1998 |
1999–2008 |
2009–2015 |
||||||||||||
|
|
|||||||||||||||
|
Total number of twin births |
13 073 |
11 162 |
7952 |
||||||||||||
|
Maternal age (years) |
|
|
|
||||||||||||
|
< 20 |
253 (1.9%) |
138 (1.2%) |
96 (1.2%) |
||||||||||||
|
20–24 |
1765 (13.5%) |
828 (7.4%) |
601 (7.6%) |
||||||||||||
|
25–29 |
4565 (34.9%) |
2573 (23.1%) |
1768 (22.5%) |
||||||||||||
|
30–34 |
4481 (34.3%) |
4313 (38.6%) |
2834 (36.1%) |
||||||||||||
|
35–39 |
1768 (13.5%) |
2809 (25.2%) |
2083 (26.5%) |
||||||||||||
|
≥ 40 |
239 (1.8%) |
501 (4.5%) |
477 (6.1%) |
||||||||||||
|
Missing data |
2 (0.2%) |
0 |
93 (1.2%) |
||||||||||||
|
Parity (previous children) |
|
|
|
||||||||||||
|
None |
5247 (40.1%) |
5131 (46.0%) |
3618 (45.5%) |
||||||||||||
|
One |
4331 (33.1%) |
3596 (32.2%) |
2612 (32.8%) |
||||||||||||
|
Two |
2264 (17.3%) |
1509 (13.5%) |
1070 (13.5%) |
||||||||||||
|
Three or more |
1230 (9.4%) |
926 (8.3%) |
648 (8.2%) |
||||||||||||
|
Missing data |
1 (< 0.1%) |
0 |
4 (< 0.1%) |
||||||||||||
|
Residential location* |
|
|
|
||||||||||||
|
Metropolitan |
9386 (71.8%) |
6898 (61.8%) |
4186 (61.6%) |
||||||||||||
|
Rural/regional |
3464 (26.5%) |
4252 (38.1%) |
1483 (21.8%) |
||||||||||||
|
Outside Victoria |
214 (1.6%) |
11 (0.1%) |
1120 (16.5%) |
||||||||||||
|
Missing data |
9 (< 0.1%) |
1 (< 0.1%) |
2 (< 0.1%) |
||||||||||||
|
|
|||||||||||||||
|
* Total number of twin births during 2009–2015 associated with residential location data was 6791 (data not reported for 2014). |
|||||||||||||||
Box 4 – Indications for caesarean delivery of twins in Victoria, by maternal age group
|
Indication for caesarean delivery |
Maternal age group |
||||||||||||||
|
Under 35 years |
35 years or more |
||||||||||||||
|
Epoch 1 |
Epoch 2 |
Epoch 3 |
P (epoch 3 v 1)* |
Epoch 1 |
Epoch 2 |
Epoch 3 |
P (epoch 3 v 1)* |
||||||||
|
|
|||||||||||||||
|
Planned caesarean deliveries |
2320 |
2635 |
2108 |
|
549 |
1463 |
1257 |
|
|||||||
|
Twins |
463 (20.0%) |
1134 (43.0%) |
1247 (59.2%) |
< 0.001 |
134 (24.4%) |
700 (47.8%) |
726 (57.8%) |
< 0.001 |
|||||||
|
Previous caesarean delivery |
481 (20.7%) |
403 (15.3%) |
291 (13.8%) |
< 0.001 |
129 (23.5%) |
268 (18.3%) |
234 (18.6%) |
0.017 |
|||||||
|
Placentation |
61 (2.6%) |
28 (1.1%) |
16 (0.8%) |
< 0.001 |
21 (3.8%) |
26 (1.8%) |
23 (1.8%) |
0.011 |
|||||||
|
Malpresentation |
718 (30.9%) |
676 (25.7%) |
302 (14.3%) |
< 0.001 |
148 (27.0%) |
282 (19.3%) |
129 (10.3%) |
< 0.001 |
|||||||
|
Hypertensive disorders |
319 (13.8%) |
159 (6.0%) |
46 (2.2%) |
< 0.001 |
61 (11.1%) |
66 (4.5%) |
37 (2.9%) |
< 0.001 |
|||||||
|
Non‐reassuring fetal status |
221 (9.5%) |
212 (8.0%) |
192 (9.1%) |
0.63 |
50 (9.1%) |
106 (7.2%) |
98 (7.8%) |
0.35 |
|||||||
|
Failure to progress |
49 (2.1%) |
9 (0.3%) |
5 (0.2%) |
< 0.001 |
6 (1%) |
4 (0.3%) |
0 |
< 0.001 |
|||||||
|
Other |
8 (0.3%) |
14 (0.5%) |
9 (0.4%) |
0.66 |
0 |
11 (0.8%) |
10 (0.8%) |
0.036 |
|||||||
|
Unplanned caesarean deliveries |
1639 |
2325 |
1505 |
|
307 |
912 |
714 |
|
|||||||
|
Twins |
257 (15.7%) |
610 (26.2%) |
462 (30.7%) |
< 0.001 |
63 (20.5%) |
276 (30.3%) |
274 (38.4%) |
< 0.001 |
|||||||
|
Previous caesarean delivery |
156 (9.5%) |
135 (5.8%) |
110 (7.3%) |
0.026 |
44 (14.3%) |
75 (8.2%) |
68 (9.5%) |
0.024 |
|||||||
|
Placentation |
62 (3.8%) |
117 (5.0%) |
65 (4.3%) |
0.45 |
14 (4.6%) |
49 (5.4%) |
30 (4.2%) |
0.80 |
|||||||
|
Malpresentation |
552 (33.7%) |
571 (24.6%) |
288 (19.1%) |
< 0.001 |
82 (26.7%) |
176 (19.3%) |
93 (13.0%) |
< 0.001 |
|||||||
|
Hypertensive disorders |
72 (4.4%) |
249 (10.7%) |
129 (8.6%) |
< 0.001 |
8 (3%) |
104 (11.4%) |
73 (10.2%) |
< 0.001 |
|||||||
|
Non‐reassuring fetal status |
227 (13.8%) |
381 (16.4%) |
322 (21.4%) |
< 0.001 |
37 (12.1%) |
157 (17.2%) |
134 (18.8%) |
0.008 |
|||||||
|
Failure to progress |
308 (18.8%) |
240 (10.3%) |
117 (7.8%) |
< 0.001 |
58 (18.9%) |
69 (7.6%) |
39 (5.5%) |
< 0.001 |
|||||||
|
Other |
5 (0.3%) |
22 (0.9%) |
12 (0.8%) |
0.06 |
1 (0.3%) |
6 (0.7%) |
3 (0.4%) |
0.82 |
|||||||
|
|
|||||||||||||||
|
* For comparison of proportions (χ2 tests). |
|||||||||||||||
Box 5 – Indications for caesarean delivery of twins in Victoria, by parity group
|
Indication for caesarean delivery |
Parity |
||||||||||||||
|
Nulliparous |
Parous |
||||||||||||||
|
Epoch 1 |
Epoch 2 |
Epoch 3 |
P (epoch 3 v 1)* |
Epoch 1 |
Epoch 2 |
Epoch 3 |
P (epoch 3 v 1)* |
||||||||
|
|
|||||||||||||||
|
Planned caesarean deliveries |
1223 |
1911 |
1517 |
|
1646 |
2187 |
1840 |
|
|||||||
|
Twins |
300 (24.5%) |
1045 (54.7%) |
1028 (67.8%) |
< 0.001 |
297 (18.0%) |
789 (36.1%) |
942 (51.2%) |
< 0.001 |
|||||||
|
Previous caesarean delivery |
NA |
NA |
NA |
|
604 (36.7%) |
668 (30.5%) |
500 (27.2%) |
< 0.001 |
|||||||
|
Placentation |
37 (3.0%) |
28 (1.5%) |
17 (1.1%) |
< 0.001 |
45 (2.7%) |
26 (1.2%) |
22 (1.2%) |
0.001 |
|||||||
|
Malpresentation |
433 (35.4%) |
478 (25.0%) |
209 (13.8%) |
< 0.001 |
433 (26.3%) |
480 (21.9%) |
221 (12.0%) |
< 0.001 |
|||||||
|
Hypertensive disorders |
270 (22.1%) |
164 (8.6%) |
64 (4.2%) |
< 0.001 |
110 (6.7%) |
61 (2.8%) |
19 (1.0%) |
< 0.001 |
|||||||
|
Non‐reassuring fetal status |
149 (12.2%) |
177 (9.3%) |
164 (10.8%) |
0.26 |
122 (7.4%) |
141 (6.4%) |
125 (6.8%) |
0.48 |
|||||||
|
Failure to progress |
24 (2.0%) |
4 (0.2%) |
4 (0.3%) |
< 0.001 |
31 (1.9%) |
9 (0.4%) |
1 (0.1%) |
< 0.001 |
|||||||
|
Other |
4 (0.3%) |
12 (0.6%) |
9 (0.6%) |
0.31 |
4 (0.2%) |
13 (0.6%) |
10 (0.5%) |
0.16 |
|||||||
|
Unplanned caesarean deliveries |
1639 |
2325 |
1505 |
|
307 |
912 |
714 |
|
|||||||
|
Twins |
190 (18.1%) |
528 (28.3%) |
285 (29.7%) |
< 0.001 |
130 (14.5%) |
358 (26.1%) |
285 (29.7%) |
< 0.001 |
|||||||
|
Previous caesarean delivery |
NA |
NA |
NA |
|
198 (22.1%) |
207 (15.1%) |
170 (17.7%) |
0.018 |
|||||||
|
Placentation |
29 (2.8%) |
76 (4.1%) |
44 (4.6%) |
0.028 |
47 (5.3%) |
90 (6.6%) |
44 (4.6%) |
0.51 |
|||||||
|
Malpresentation |
317 (30.2%) |
387 (20.8%) |
197 (20.6%) |
< 0.001 |
317 (35.4%) |
360 (26.2%) |
197 (20.6%) |
< 0.001 |
|||||||
|
Hypertensive disorders |
63 (6.0%) |
269 (14.4%) |
50 (5.2%) |
0.45 |
17 (1.9%) |
84 (6.1%) |
50 (5.2%) |
< 0.001 |
|||||||
|
Non‐reassuring fetal status |
175 (16.7%) |
342 (18.3%) |
179 (18.7%) |
0.23 |
89 (9.9%) |
196 (14.3%) |
179 (18.7%) |
< 0.001 |
|||||||
|
Failure to progress |
270 (25.7%) |
245 (13.1%) |
28 (2.9%) |
< 0.001 |
96 (10.7%) |
64 (4.7%) |
28 (2.9%) |
< 0.001 |
|||||||
|
Other |
5 (0.5%) |
15 (0.8%) |
5 (0.5%) |
0.88 |
1 (0.1%) |
13 (0.9%) |
5 (0.5%) |
0.12 |
|||||||
|
|
|||||||||||||||
|
NA = not applicable. * For comparison of proportions (χ 2 tests). |
|||||||||||||||
Box 6 – Caesarean deliveries of twins as proportions of all deliveries of twins in Victoria, 2010–2013, by region of residence and indication
|
Indication for caesarean delivery |
Region |
||||||||||||||
|
North and West Metro |
Southern Metro |
Eastern Metro |
Barwon–South Western |
Loddon Mallee |
Hume |
Gippsland |
Grampians |
||||||||
|
|
|||||||||||||||
|
All twin births |
1637 |
1066 |
674 |
267 |
227 |
210 |
187 |
157 |
|||||||
|
Twin births by caesarean delivery |
1198 [73.2%] |
715 [67.1%] |
485 [70.4%] |
206 [77.1%] |
160 [70.5%] |
139 [66.2%] |
100 [53.5%] |
125 [79.6%] |
|||||||
|
Previous caesarean delivery |
140 (12%) |
89 (12%) |
40 (8.4%) |
31 (15%) |
29 (18%) |
25 (18%) |
7 (7%) |
18 (14%) |
|||||||
|
Placentation |
29 (2.4%) |
20 (2.8%) |
7 (2%) |
4 (2%) |
2 (1%) |
1 (0.7%) |
6 (6%) |
2 (2%) |
|||||||
|
Malpresentation |
168 (14%) |
113 (16%) |
50 (1%) |
31 (15%) |
24 (15%) |
30 (22%) |
37 (37%) |
14 (11%) |
|||||||
|
Hypertension |
74 (6.2%) |
28 (3.9%) |
24 (5.1%) |
11 (5.3%) |
6 (4%) |
7 (5%) |
3 (3%) |
6 (5%) |
|||||||
|
Fetal status |
140 (12%) |
98 (14%) |
70 (15%) |
25 (12%) |
23 (14%) |
13 (9.4%) |
9 (9%) |
15 (12%) |
|||||||
|
Failure to progress |
33 (2.8%) |
18 (2.5%) |
12 (2.5%) |
3 (2%) |
1 (0.6%) |
7 (5%) |
6 (6%) |
6 (5%) |
|||||||
|
Other |
6 (0.5%) |
2 (0.3%) |
2 (0.4%) |
1 (0.5%) |
1 (0.6%) |
0 |
1 (1%) |
1 (0.8%) |
|||||||
|
Twin pregnancy |
608 (50.8%) |
347 (48.5%) |
270 (56.8%) |
100 (48.5%) |
74 (46%) |
56 (40%) |
31 (31%) |
63 (50%) |
|||||||
|
|
|||||||||||||||
|
|
|||||||||||||||
Box 7 – Caesarean twin deiveries in Victoria, 2010–2013 and 2015, by region of residence
|
Region |
Adjusted odds ratio* |
P |
|||||||||||||
|
|
|||||||||||||||
|
Barwon–South Western |
1.37 (1.04–1.82) |
0.26 |
|||||||||||||
|
Grampians |
1.01 (0.71–1.43) |
0.96 |
|||||||||||||
|
North and West Metro |
1 |
— |
|||||||||||||
|
Loddon Mallee |
0.94 (0.71–1.26) |
0.69 |
|||||||||||||
|
Southern Metro |
0.71 (0.60–0.83) |
< 0.001 |
|||||||||||||
|
Hume |
0.70 (0.53–0.92) |
0.012 |
|||||||||||||
|
Eastern Metro |
0.69 (0.58–0.82) |
< 0.001 |
|||||||||||||
|
Gippsland |
0.46 (0.35–0.61) |
< 0.001 |
|||||||||||||
|
|
|||||||||||||||
|
* Adjusted for maternal age, body mass index, parity, admission type (public, private), use of artificial reproductive technology, and previous caesarean delivery. |
|||||||||||||||
Received 3 February 2019, accepted 22 July 2019
- Yizhen (Amy) Liu1
- Mary‐Ann Davey1
- Rilka Lee2
- Kirsten R Palmer1,3
- Euan M Wallace1,4
- 1 Monash University, Melbourne, VIC
- 2 Mercy Hospital for Women, Melbourne, VIC
- 3 Monash Health, Melbourne, VIC
- 4 Safer Care Victoria, Victoria Department of Health and Human Services, Melbourne, VIC
This investigation was supported by a National Health and Medical Research Council program grant (1113902). We are grateful to the Consultative Council on Obstetric and Paediatric Mortality and Morbidity (CCOPMM) for providing access to the de‐identified data we analysed and for the assistance of staff at the Consultative Councils Unit, Safer Care Victoria. The conclusions, findings, opinions and views or recommendations expressed in this article are strictly ours, and do not necessarily reflect those of CCOPMM.
No relevant disclosures.
- 1. Australian Institute of Health and Welfare. Perinatal deaths in Australia: 2013–14 (Cat. No. PER 94). Canberra: AIHW, 2018.
- 2. Consultative Council on Obstetric and Paediatric Mortality and Morbidity. Victoria's mothers, babies and children report 2016. Melbourne: Department of Health and Human Services, 2017. https://bettersafercare.vic.gov.au/reports-and-publications/victorias-mothers-babies-and-children-report-2016 (viewed May 2019).
- 3. Lee HC, Gould JB, Boscardin WJ, et al. Trends in cesarean delivery for twin births in the United States: 1995–2008. Obstet Gynecol 2011; 118: 1095–1101.
- 4. Antsaklis A, Malamis FM, Sindos M. Trends in twin pregnancies and mode of delivery during the last 30 years: inconsistency between guidelines and clinical practice. J Perin Med 2013; 41: 355–364.
- 5. Macfarlane AJ, Blondel B, Mohangoo AD, et al; Euro‐Peristat Scientific Committee. Wide differences in mode of delivery within Europe: risk‐stratified analyses of aggregated routine data from the Euro‐Peristat study. BJOG 2016; 123: 559–568.
- 6. Vogel JP, Betran AP, Vindevoghel N, et al. Use of the Robson classification to assess caesarean section trends in 21 countries: a secondary analysis of two WHO multicountry surveys. Lancet Glob Health 2015; 3: e260–e270.
- 7. The Lancet. Stemming the global caesarean section epidemic. Lancet 2018; 392: 1279.
- 8. Althabe F, Sosa C, Belizán J, et al. Cesarean section rates and maternal and neonatal mortality in low‐, medium‐, and high‐income countries: an ecological study. Birth 2006; 33: 270–277.
- 9. Barrett JFR, Hannah ME, Hutton EK, et al. A randomized trial of planned cesarean or vaginal delivery for twin pregnancy. New Engl J Med 2013; 369: 1295–1305.
- 10. Hofmeyr GJ, Barrett JF, Crowther CA. Planned caesarean section for women with a twin pregnancy. Cochrane Database Syst Rev 2015; CD006553.
- 11. Schmitz T, Prunet C, Azria E, et al. Association between planned cesarean delivery and neonatal mortality and morbidity in twin pregnancies. Obstet Gynecol 2017; 129: 986–995.
- 12. Flood MM, McDonald SJ, Pollock WE, Davey MA. Data accuracy in the Victorian perinatal data collection: results of a validation study of 2011 data. Health Infor Man J 2017; 46: 113–126.
- 13. Roberts CL, Algert CS, Morris JM, Henderson‐Smart DJ. Trends in twin birth in New South Wales, Australia, 1990–1999. Int J Gynecol Obstet 2002; 78: 213–219.
- 14. Australian Institute of Health and Welfare. Australia's mothers and babies 2016 (Cat. No. PER 97; Perinatal statistics series no. 34). Canberra: AIHW, 2018.
- 15. Teoh M, Walker S, Cole S, Edwards A. A problem shared is a problem halved: success of a statewide collaborative approach to fetal therapy. Outcomes of fetoscopic laser photocoagulation for twin‐twin transfusion syndrome in Victoria. Aus NZ J Obstet Gynaecol 2013; 53: 108–113.
- 16. Hunt RW, Davey MA, Ryan‐Atwood TE, et al; Maternal and Newborn Clinical Network INSIGHT committee. Victorian perinatal services performance indicators 2017–18. Melbourne: Safer Care Victoria, Victorian Government, 2018. https://bettersafercare.vic.gov.au/sites/default/files/2019-02/Vic%20perinatal%20services%20performance%20indicators%202017-18.pdf (viewed May 2019).
- 17. McLeod L, Barrett J, Hewson S, Hannah ME. Women's views regarding participation in a proposed randomised controlled trial of twin delivery. J Obstet Gynaecol Can 2004; 26: 575–579.
- 18. Smith GC, Shah I, White IR, et al. Mode of delivery and the risk of delivery‐related perinatal death among twins at term: a retrospective cohort study of 8073 births. BJOG 2005; 112: 1139–1144.
- 19. Armson BA, O'Connell C, Persad V, et al. Determinants of perinatal mortality and serious neonatal morbidity in the second twin. Obstet Gynecol 2006; 108: 556–564.
- 20. Dodd JM, Deussen AR, Grivell RM, Crowther CA. Elective birth at 37 weeks' gestation for women with an uncomplicated twin pregnancy. Cochrane Database Syst Rev 2014; CD003582.
- 21. Wood S, Cooper S, Ross S. Does induction of labour increase the risk of caesarean section? A systematic review and meta‐analysis of trials in women with intact membranes. BJOG 2014; 121: 674–685.
- 22. Easter SR, Taouk L, Schulkin J, et al. Twin vaginal delivery: innovate or abdicate. Am J Obstet Gynecol 2017; 216: 484–488.
- 23. Chevreau J, Foulon A, Abou Arab O, et al. Management of breech and twin labor during registrarship: a two‐year prospective, observational study. J Gynecol Obstet Hum Reprod 2018; 47: 191–196.
- 24. Chinnock M, Robson S. Obstetric trainees' experience in vaginal breech delivery: implications for future practice. Obstet Gynecol 2007; 110: 900–903.
- 25. Chinnock M, Robson S. An anonymous survey of registrar training in the uses of Kjelland's forceps in Australia. Aust NZ J Obstet Gynaecol 2009; 49: 515–516.
- 26. Skinner S, Davies‐Tuck M, Wallace E, Hodges R. Perinatal and maternal outcomes after training residents in forceps before vacuum instrumental birth. Obstet Gynecol 2017; 130: 151–158.
- 27. Royal Australian and New Zealand College of Obstetricians and Gynaecologists. RANZCOG curriculum: a framework to guide the training and practice of Specialist Obstetricians and Gynaecologists. Updated Nov 2017. https://www.ranzcog.edu.au/RANZCOG_SITE/media/RANZCOG-MEDIA/Training%20and%20Assessment/Specialist%20Training/Curriculum%20and%20Handbook/RANZCOG-Curriculum.pdf (viewed May 2019).
- 28. Rouse DJ. Twins are not a per se indication for cesarean delivery. Obstet Gynecol 2017; 129: 974–975.
- 29. Greene MF. Delivering twins. New Engl J Med 2013; 369: 1365–1366.
- 30. Little MO, Lyerly AD, Mitchell LM, et al. Mode of delivery: toward responsible inclusion of patient preferences. Obstet Gynecol 2008; 112: 913–918.





Abstract
Objectives: To examine changes in the modes of delivery of twins in Victoria over 33 years.
Design: Retrospective population‐based study.
Setting, participants: All twin births in Victoria, 1 January 1983 – 31 December 2015.
Major outcomes: Mode of birth (vaginal, planned or unplanned caesarean delivery); indications for caesarean delivery.
Results: During 1983–2015, 32 187 twin pregnancies ended in live or stillbirths in Victoria. The proportion of twins born by caesarean delivery increased from 24% (156 twin deliveries) in 1983 to 71% (782 deliveries) in 2015. The proportion of twin births by planned caesarean delivery with twin pregnancy as the sole indication for caesarean delivery increased across this period from 1.8% (12 twin deliveries) to 21% (231 deliveries). The proportion of twin births by caesarean delivery and the proportion of caesarean twin deliveries with twin pregnancy as the principal indication each differed between Victorian regions.
Conclusion: During 1983–2015, the proportion of twins born in Victoria by caesarean delivery increased almost threefold, mostly because caesarean delivery has become the preferred mode of birth for twin pregnancies. Regional differences in the delivery of twins suggest that the number of caesarean deliveries can be reduced with appropriate system and training support.