We present a case of acute ethanol toxicity in a preschool child who developed depressed mental status and hypotension and required inotrope support as a result of ingesting an alcohol-based hand sanitiser
Clinical record
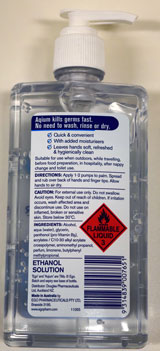
In September 2014, a 3-year-old girl was brought by her parents to the emergency department (ED) with an acutely altered level of consciousness. The history from the parents stated that the young girl had been playing with an alcohol-based hand sanitiser (ABHS; 70% ethanol, 375 mL [Figure]) with her 1-year-old sibling while the parent was in the room. Ingestion of the ABHS had not been witnessed.
On assessment she had a patent airway, a respiratory rate of 18 breaths/min, an oxygen saturation level of 96% on room air, heart rate of 97 beats per minute, blood pressure of 95/54 mmHg and a temperature of 35.5°C. Her Glasgow coma scale (GCS) score was 10/15 (motor response, 5; verbal response, 3; eye response, 2). Her eyes showed alternating disconjugate gaze, with pupils equally constricted at 2 mm. Her pupils dilated in response to noxious stimuli (eg, trapezius squeeze test). The patient's medical history included normal development, no infectious contacts, and she was fully vaccinated and had no surgical history. No odour of ethanol was appreciated on her breath or her clothing. Her 1-year-old sibling was behaving normally.
A blood glucose test at the bedside gave a concentration of 4.6 mmol/L (reference interval [RI], 4.4–6.1 mmol/L), and a venous gas analysis showed a pH of 7.34 (RI, 7.33–7.44), a normal Pco2 of 44 mmHg, a bicarbonate level of 23 mmol/L (RI, 24–28 mmol/L)and a base deficit of − 3 mmol/L (RI, − 2 to 2) with an increased anion gap of 17 mEq/L (RI, 4–12 mEq/L).
Her measured serum osmolality was abnormal at 357 mmol/L (RI, 265–295 mmol/L). She had a normal haemoglobin concentration, platelet count and white cell count with no evidence of left shift. Results of an electrolyte assay included an abnormal serum sodium concentration of 151 mmol/L (RI, 135–145 mmol/L) and a chloride concentration of 111 mmol/L (RI, 98–106 mmol/L), with normal concentrations of potassium, urea, creatinine and C-reactive peptide (7 mg/L; RI, < 8 mg/L). Liver enzymes were not analysed. An electrocardiogram was normal. A computed tomography scan of her brain without contrast showed no acute intracranial injury. Within an hour of ED admission, the patient developed hypotension (70/22 mmHg) which was treated with two fluid boluses of normal saline (20 mL/kg each) and peripheral adrenaline infusion (0.05 µg/kg/h).
Treating physicians deemed that she was not clinically septic, dehydrated or severely injured based on her history and serial examinations paired with investigations. However, they had a high suspicion of intoxication. Subsequently, her serum ethanol concentration just before adrenaline administration was reported as 260 mg/dL (legal blood ethanol level for drivers in the state of Victoria, < 50mg/dL).
She was admitted to the paediatric intensive care unit (PICU) without intubation. No additional blood ethanol concentration tests were performed. A peripheral blood culture was negative, and serial blood gas measurements showed a normal venous lactate level and gradual normalisation of pH and sodium and chloride concentrations over the following 15 hours. The patient's condition improved (at 5 hours after her PICU admission, her GCS score was 15/15, she was normotensive without inotrope support and was mobilising) and she was discharged within 24 hours.
Hand hygiene with alcohol-based hand sanitiser (ABHS) is encouraged in health, education and day-care facilities, workplaces and the home.1,2 The active ingredient of ABHS is ethanol or isopropanol at a concentration of 60% to 95%. The increasing intentional ingestion of these products by teenagers, and consequences, have been well reported.3 The Victorian Poisons Information Centre received a total of 15 729 calls in 2013 relating to children aged under 5 years, and reported that topical antiseptics/hand sanitisers was the fifth most frequent source of poison to which this age group was exposed.4
Our unique case shows the toxic effects of ABHS. The patient had altered Glasgow coma scale scores, associated hypotension, hypernatraemia, hyperchloraemia and one of the highest serum ethanol concentrations yet reported in this age group. A surprising feature was the ingestion of an ABHS that comprised 70% ethanol despite parental supervision of play. The hyperchloraemia and hypernatraemia might be explained by the suppression of antidiuretic hormone by ethanol, resulting in water diuresis, with loss of more water than sodium or chloride and the lack of further fluid intake.5 Strict fluid output was not recorded to confirm this.
A published review of Ovid MEDLINE, EMBASE and CINAHL databases shows that ingestion of household products containing ethanol by children is an increasingly common occurrence, and that there is a paucity of studies from outside North America.6 This review includes two retrospective studies from North American poison centres that report a lack of significant effects from unintended paediatric ingestion of ABHS.6 A previously published case reports mild hypothermia, hypokalaemia and the necessity for mechanical ventilation for airway protection during transport to another facility after ABHS ingestion.7
We used a modified Widmark formula to estimate the minimum weight of ethanol needed to be ingested as follows:
Weight of alcohol ingested in grams = (blood ethanol concentration in mg/dL × total body water in litres)/the percentage of water in blood (which is 80.65%).
The patient's height was 95 cm (50th centile) and her weight was 16 kg, giving an estimated total body water volume of 9.4 L. To achieve a blood ethanol concentration of 260 mg/dL, she would have needed to ingest 30.3 g of ethanol ([260 mg/dL × 9.4 L]/80.65 = 30.3 g).8,9 This equates to a consumption of a minimum 55 mL of an ABHS comprising 70% alcohol (55.3 g ethanol per 100 mL).8
Currently, the only highlighted label on the ABHS indicates that the liquid is flammable (Figure). This may be insufficient to convey the toxic potential of ABHSs to parents, carers and children.
Lessons from practice
- Contrary to perceptions, preschool children are able to ingest enough alcohol-based hand sanitiser to develop severe ethanol toxicity.
- There should be an increased awareness of the hazards associated with alcohol sanitiser ingestion.
- 1. Hand hygiene Australia. http://www.hha.org.au/home.aspx (accessed Oct 2014).
- 2. Zomer T, Erasmus V, Vlaar N, et al. A hand hygiene intervention to decrease infections among children attending day care centers: design of a cluster randomised controlled trial. BMC Infect Dis 2013; 13: 259.
- 3. Forrester MB. Characteristics of hand sanitizer ingestions by adolescents reported to poison centers. Int J Adolesc Med Health 2015; 27: 69-72.
- 4. Victorian Poisons Information Centre, Annual Report 2013. http://www.austin.org.au/Assets/Files/VPIC%20Annual%20Report%202013.pdf (accessed Sept 2014).
- 5. Bouthoorn SH, van der Ploeg T, van Erkel NE, et al. Alcohol intoxication among Dutch adolescents: acute medical complications in the years 2000–2010. Clin Pediatr (Phila) 2011; 50: 244-251.
- 6. Rayar P, Ratnapalan S. Pediatric ingestions of house hold products containing ethanol: a review. Clin Pediatr (Phila) 2013; 52: 203-209.
- 7. Engel JS, Spiller HA. Acute ethanol poisoning in a 4-year-old as a result of ethanol-based hand-sanitizer ingestion. Pediatr Emerg Care 2010; 26: 508-509.
- 8. Brick J. Standardization of alcohol calculations in research. Alcohol Clin Exp Res 2006; 30: 1276-1287.
- 9. Mellits ED, Cheek DB. The assessment of body water and fatness from infancy to adulthood. Monogr Soc Res Child Dev 1970; 35: 12-26.





We thank Jeff Robinson, Manager of the Victorian Poisons Information Centre, Austin Hospital, for his assistance with the toxicology calculations.
No relevant disclosures.