The 2002 Bali bombing remains the largest single act of terrorism to have directly affected Australians.1 Such atrocities pose serious challenges to the resilience of survivors, and to the health services charged with their care. Raphael and colleagues highlighted the limited available evidence to guide practice with survivors of the 2002 bombing, including those bereaved by the attack.2 These individuals may experience the interplay of trauma and grief symptoms and have complex, evolving needs over time.2,3
Since the attacks on the World Trade Center and other United States targets on 11 September 2001, there has been an increased research focus on understanding the recovery trajectories and health risk factors of terrorism survivors.4 However, virtually no studies have sought the views of survivors themselves regarding factors that support optimal coping and recovery. Such advice can uniquely inform emergency and health planners about survivor needs.5 Drawing on the experiences of Australians directly affected by terrorism, the aims of this study were (i) to identify factors that would support the coping of similarly impacted groups, and (ii) to determine whether advocated coping supports vary according to demographic, physical and mental health, incident-exposure and bereavement variables.
This cross-sectional convenience sample consisted of individuals who had experienced personal exposure and/or bereavement related to the 2002 bombing and had attended at least one session with a New South Wales Ministry of Health therapeutic program. The Bali Recovery Program offered home-based outreach, psychoeducation sessions, and individual or family-based therapy and maintenance.2 Survey participants completed computer-assisted telephone interviews between 9 July and 22 November 2010. Surveys were completed in 45–55 minutes and were conducted by professional interviewers from the NSW Health Survey Program, who also did the transcriptions. Telephone surveys were used to be consistent with other samples in a wider study of disaster-resilience factors.6 The validity of telephone-based interviews to assess stress and anxiety conditions has been demonstrated.7
Participants responded to closed-ended questions to measure independent variables, and to open-ended items to explore their experiences regarding the 2002 bombing and post-incident experiences. Consistent with Krippendorff,8 we conducted a qualitative content analysis of participant responses to this question: “Based on what you have observed, what do you believe would help other people cope best after an experience like the one you went through?”
Participant-advocated coping supports were examined against several independent variables: demographic; physical and mental health (self-rated physical health, psychological distress, trauma symptoms and mental health diagnosis); incident-exposure and loss (presence in Bali and bereavement type); a validated item measuring self-rated physical health;9 and past-month psychological distress measured using the Kessler Psychological Distress Scale, where scores range from 10 to 50 and high scores (≥ 22) indicate significant risk of a mental health condition.10 The Primary Care Post-Traumatic Stress Disorder (PTSD) Screen measured past-month trauma symptoms specific to Bali bombing-related experiences. Each scale item corresponds to a specific PTSD symptom (re-experiencing, numbing, avoidance or hyperarousal), with two or more symptoms indicating possible PTSD.11 Mental health diagnoses constituted any diagnosis received from a mental health specialist since the bombing.
All transcripts for the responses were reviewed independently by two researchers, to develop a coding frame for the analysis based on thematic content. There was high concordance between these two independently established coding frames. Ten coping support themes were found to accommodate all responses, but could be subsumed under four primary themes: professional help and counselling; social support; government response and policy; and personal coping strategies (Box 1).
Two researchers not previously involved in the analysis independently coded the entire dataset using the agreed coding frame. As with the coding frame, these data were coded manually. The inter-rater reliability of the coded sets was high (κ = 0.88). There were no significant differences between the coding for the four primary themes. When scoring items to determine prevalence, if a respondent made multiple comments in the same primary category, this was only counted once.
All independent variables were dichotomised for analysis: residential location (metropolitan or regional, by postcode); marital status (married or de facto, or non-partnered); presence in Bali (present during or shortly after bombing, or not present); and bereavement type (first-degree relative, or non-relative). Respondent age was bimodally distributed and categorised as younger (20–43 years) or older (51–73 years). We used established clinical cut-offs to categorise psychological distress: Kessler Psychological Distress Scale, low (10–21) or high (22–50); and trauma symptoms: Primary Care PTSD Screen, low (0–1 symptom) or high (2–4 symptoms).10,11 We used χ2 tests to test for significant differences in the prevalence of advocated coping supports by the covariates.
Of the 81 individuals contacted, 55 (68%) participated. Of these, 32 were women, and the mean respondent age was 50 years. Twenty-one respondents were present in Bali during or soon after the bombing, and 54 were bereaved due to the incident. Respondents provided a total of 114 comments. The average interval between the 2002 bombing and the interview was 7 years and 11 months. No significant differences were found between the respondent group (n = 55) and the total Bali Recovery Program population (n = 115) regarding mean age (P = 0.38) or sex (P = 0.39).
Box 1 presents the descriptions and prevalence of the four primary support themes: receipt of professional psychological help (counselling) (29/55); social support (24/55); proactive responses or policies from government agencies (22/55); and personal attitude or coping strategies (18/55). Some quotes from respondents are provided in Box 2.
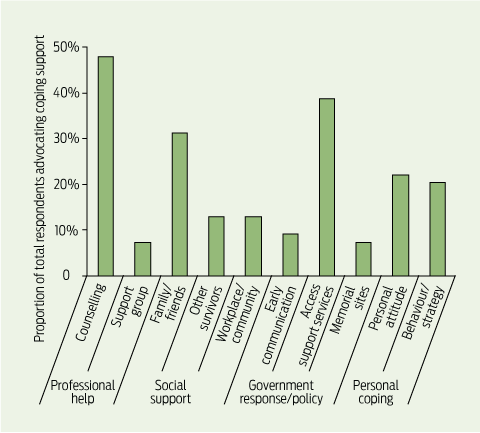
The prevalence of the 10 coping support subthemes is shown in Box 3. The most commonly advocated subtheme of professional help was individual or family-based counselling (as distinct from group interventions), being identified by 26 of the 55 respondents.
Three men recommended having a clear option of a limited number of consultations (or later check-ups) to get information about potential effects in order to prepare for these.
Social support was seen as pivotal in recovery: family and friend support (17/55); sharing thoughts and feelings with other survivors (7/55) and community support (eg, workplace, clubs, general public) (7/55).
Opportunities to share with other survivors appeared to provide a special form of solace: “Some of the people on the outside don’t understand how you feel”.
The largest subtheme regarding government response and policy (21/55) related to service access, primarily counselling. Comments emphasised the value of a service system that was integrated and easy to navigate:
Particular comment was made regarding the reassurance of knowing that established services (eg, counselling) would remain available and not be withdrawn at an arbitrary point. Some people (4/55) reported that memorial services and permanent sites were invaluable, the latter providing a physical place where people could gather, sharing both grief and positive remembrance.
Respondents observed that affected groups would be well served by improved coordination and communication, particularly in the early post-incident phase:
Two elements of personal coping were identified as being likely to assist others: specific behaviour and tasks (11/55) and personal attitudes (12/55). The former included physical exercise, maintaining a simple daily routine, keeping occupied, and expressive outlets such as journal writing. The latter included not giving up, living well to honour those lost, continuing to work on mental health, and being able to accept the losses, including acquired disabilities.
Advocated coping supports were analysed by demographic, health, exposure and bereavement variables (Box 4). Women were significantly more likely to endorse the need for proactive government response (P = 0.03). Men were more likely to advocate personal coping strategies (P < 0.01). Those diagnosed with a mental health condition after the incident were significantly less likely to advocate social support as a support factor for others (P = 0.04).
Our findings highlight several areas that can inform both the type and targeting of support initiatives, and current policy regarding access to health and other services. Receiving professional mental health services was the most frequently advocated coping support process and did not differ significantly based on demographic, health, exposure or bereavement factors. This suggests that when services are proactive and event-specific their tolerance and perceived benefits may be similar across future recipient groups.
It was notable that women were significantly more likely to advocate proactive government responses, while men generally saw personal attitudes and responses as pivotal to effective coping. These outcomes may reflect broader findings regarding sex-related stress coping, with men and women tending to employ problem-focused and emotion-focused (affiliative) coping strategies, respectively.12 Such findings may have implications for target interventions. For example, while no differences by sex were evident regarding the advocacy of counselling per se, a small number of men expressed preferences for counselling or group work focused on symptom education (what to expect) or flexibly delivered contact (eg, a periodic check-up). As men are also more reluctant to attend mental health services in general,13 future survivors may benefit from comprehensive stepped-care services that include brief intervention and education options.14
The strong advocacy of social support processes is consistent with other findings of an association between perceived support and lower mental health morbidity among survivors.15 Disaster losses and specific trauma effects (eg, withdrawal, depression) often degrade interpersonal relationships over time. The ability to actively maintain social support in such contexts may be highly protective.16 The finding that survivors with a mental health diagnosis were significantly less likely to advocate social supports may indicate that they perceive their available supports to be insufficient or that their capacity to access them is compromised due to mental health related issues. Support maintenance may therefore constitute an important early intervention. A recently developed program, Skills for Psychological Recovery, teaches disaster survivors key recovery skills (eg, managing reactions, problem solving, rebuilding social supports) and could be adapted for terrorism survivors.17
This study has several limitations. Its findings are cross-sectional, and coping support perceptions may change over time. The response rate could potentially introduce responder bias, although no significant differences by age or sex were observed between the study and total program samples. Participants had varying contact with a therapeutic program, which may have inflated their advocacy of counselling. Importantly, such advocacy reflects direct experience of this process and its perceived value in this context. While qualitative data are often context-dependent, these findings are likely to be relevant to other Australians directly affected by terrorism and the policy and practice frameworks intended to support them.
1 Coding categories for responses to the key question: “What would help other people cope best after an experience like the one you went through?”(n = 55)
Primary theme |
Expanded description (subtheme) |
No. of respondents* |
|||||||||||||
Professional help |
Counselling/mental health consultation: receipt of professional counselling; mental health consultation(s); group information sessions |
29 |
|||||||||||||
|
Support group: formal groups led by professional mental health workers |
||||||||||||||
Social support |
Family and friends: able to talk with and confide in family and friends; maintaining support relationships |
24 |
|||||||||||||
|
Other survivors: share thoughts and feelings with others directly affected/bereaved |
||||||||||||||
|
Workplace/community: support from workplaces, clubs, wider community |
||||||||||||||
Government response and policy |
Early communication/coordination: proactive response by government agencies; early post-incident coordination and communication; better regulations (ie, protections) regarding media |
22 |
|||||||||||||
|
Access support services: accessible, integrated information detailing health/welfare services available (eg, counselling, financial assistance) |
||||||||||||||
|
Memorial services/sites: services; creation of permanent sites |
||||||||||||||
Personal coping |
Personal attitude: positive/adaptive attitudes; willingness to get personal or professional help |
18 |
|||||||||||||
|
Coping strategies: adaptive behaviours (eg, keeping busy, maintaining a simple daily routine, returning to work, engaging in tasks supporting reflection and restoration) |
||||||||||||||
* Respondents could report in more than one primary category. |
|||||||||||||||
2 Selected responses, by theme
Professional help
“Being able to see someone that has knowledge about the mental health side and the after affects, an idea of what mental health effects are likely to take place.”
Social support
“People being there for you, being where you are that day, and refraining from telling you what to do, how to feel.”
Government response
“These memorials are important. My children, nephews and nieces visit them regularly.”
“For me, it was being able to know the circumstances of their death.”
“Putting some restrictions on the media, on how they deal with things and allowing people their privacy if that’s what they want.”
Personal coping
“I believe that you should try and accept it, which is very hard, and if you don’t it is very difficult to get over it.”
4 Prevalence of advocated coping supports by demographic, health and incident-related factors (n = 55)
|
No. of respondents |
||||||||||||||
Covariates |
Total |
Professional help |
Social support |
Government response |
Personal coping |
||||||||||
Sex |
|
|
|
|
|
||||||||||
Male |
23 |
13 |
10 |
5 |
13 |
||||||||||
Female |
32 |
16 |
14 |
17* |
5* |
||||||||||
Age |
|
|
|
|
|
||||||||||
Younger (20–43 yrs) |
22 |
13 |
8 |
11 |
8 |
||||||||||
Older (51–73 yrs) |
33 |
16 |
16 |
11 |
10 |
||||||||||
Location |
|
|
|
|
|
||||||||||
Metropolitan |
35 |
17 |
16 |
14 |
13 |
||||||||||
Regional |
20 |
12 |
8 |
8 |
5 |
||||||||||
Married/de facto |
|
|
|
|
|
||||||||||
No |
15 |
9 |
4 |
8 |
5 |
||||||||||
Yes |
40 |
20 |
20 |
14 |
13 |
||||||||||
Good self-rated health |
|
|
|
|
|
||||||||||
No |
10 |
7 |
2 |
2 |
2 |
||||||||||
Yes |
45 |
22 |
22 |
20 |
16 |
||||||||||
Present in Bali† |
|
|
|
|
|
||||||||||
No |
34 |
19 |
16 |
16 |
9 |
||||||||||
Yes |
21 |
10 |
8 |
6 |
9 |
||||||||||
Bereavement type‡ |
|
|
|
|
|
||||||||||
Non-family |
17 |
10 |
7 |
5 |
5 |
||||||||||
Family |
37 |
19 |
17 |
17 |
13 |
||||||||||
Psychological distress§ |
|
|
|
|
|
||||||||||
Low |
43 |
25 |
20 |
17 |
20 |
||||||||||
High |
12 |
4 |
4 |
5 |
3 |
||||||||||
Trauma symptoms¶ |
|
|
|
|
|
||||||||||
Low |
28 |
18 |
13 |
11 |
11 |
||||||||||
High |
27 |
11 |
11 |
11 |
7 |
||||||||||
Mental health diagnosis |
|
|
|
|
|
||||||||||
No |
34 |
18 |
19 |
13 |
11 |
||||||||||
Yes |
21 |
11 |
5* |
9 |
7 |
||||||||||
Total respondent group |
55 |
29 |
24 |
22 |
18 |
||||||||||
* P < 0.05. † At time of or within 48 hours of bombing. ‡ n = 54; family bereavement defined as loss of first-degree relative. § Kessler Psychological Distress Scale: low (range, 10–21); high (range, 22–50). ¶ Primary Care Post-Traumatic Stress Disorder Screen: low (0–1 symptoms); high (2–4 symptoms). |
|||||||||||||||
Received 26 April 2013, accepted 28 September 2013
- Garry J Stevens1
- Julie C Dunsmore2,3
- Kingsley E Agho1
- Melanie R Taylor1
- Alison L Jones4
- Beverley Raphael1
- 1 School of Medicine, University of Western Sydney, Sydney, NSW.
- 2 Northern Sydney Local Health District, NSW Health, Sydney, NSW.
- 3 National Association for Loss and Grief (NSW) Inc, Sydney, NSW.
- 4 Graduate School of Medicine, University of Wollongong, Wollongong, NSW.
This study was funded by the Australian Research Council (DP0881463) and is part of Garry Stevens’s PhD thesis for the School of Medicine at the University of Western Sydney. We thank the Health Survey Program Interviewers, Centre for Epidemiology and Evidence, NSW Ministry of Health.
No relevant disclosures.
- 1. Rosenfeld JV, Fitzgerald M, Kossmann T, et al. Is the Australian hospital system adequately prepared for terrorism? Med J Aust 2005; 183: 567-570. <MJA full text>
- 2. Raphael B, Dunsmore J, Wooding S. Terror and trauma in Bali: Australia’s mental health disaster response. J Aggress Maltreat Trauma 2004; 9: 245-256.
- 3. Stevens GJ, Dunsmore JC, Agho KE, et al. Long-term health and wellbeing of people affected by the 2002 Bali bombing. Med J Aust 2013; 198: 273-277. <MJA full text>
- 4. Neria Y, DiGrande L, Adams BG. Posttraumatic stress disorder following the September 11, 2001, terrorist attacks: a review of the literature among highly exposed populations. Am Psychol 2011; 66: 429-446.
- 5. Sample PL, Greene D, Johns NR. Life-bombing-injury-life: a qualitative follow-up study of Oklahoma City bombing survivors with TBI. Brain Inj 2012; 26: 13-14.
- 6. Stevens G, Agho K, Taylor M, et al. Perceived coping and concern predict terrorism preparedness in Australia. BMC Public Health 2012; 12: 1117.
- 7. Rohde P, Lewinsohn PM, Seeley JR. Comparability of telephone and face-to-face interviews in assessing axis I and axis II disorders. Am J Psychiatry 1997; 154: 1593-1598.
- 8. Krippendorff K. Content analysis. An introduction to its methodology. Beverly Hills: Sage, 1980.
- 9. Centre for Epidemiology and Research. New South Wales Population Health Survey: 2010 report on adult health. Sydney: NSW Department of Health, 2011.
- 10. Slade T, Grove R, Burgess P. Kessler Psychological Distress Scale: normative data from the 2007 Australian National Survey of Mental Health and Wellbeing. Aust N Z J Psychiatry 2011; 45: 308-316.
- 11. Prins A, Ouimette P, Kimerling R, et al. The primary care PTSD screen (PC-PTSD): development and operating characteristics. Prim Care Psychiatr 2003; 9: 9-14. http://www. ptsd.va.gov/professional/articles/article-pdf/id26676.pdf (accessed Aug 2013).
- 12. Lazarus RS, Folkman S. Stress, appraisal, and coping. New York: Springer, 1984.
- 13. Wang PS, Aguilar-Gaxiola S, Alonso J, et al. Use of mental health services for anxiety, mood, and substance disorders in 17 countries in the WHO world mental health surveys. Lancet 2007; 370: 841-850.
- 14. Bower P, Gilbody S. Stepped care in psychological therapies: access, effectiveness and efficiency. Narrative literature review. Br J Psychiatry 2005; 186: 11-17.
- 15. Bleich A, Gelkopf M, Solomon Z. Exposure to terrorism, stress-related mental health symptoms, and coping behaviors among a nationally representative sample in Israel. JAMA 2003; 290: 612-620.
- 16. Benight CC, Freyaldenhoven RW, Hughes J, et al. Coping self-efficacy and psychological distress following the Oklahoma City bombing. J Appl Soc Psychol 2000; 30: 1131-1344.
- 17. Forbes D, Fletcher S, Wolfgang BJW, et al. Practitioner perceptions of Skills for Psychological Recovery: a training programme for health practitioners in the aftermath of the Victorian bushfires. Aust N Z J Psychiatry 2010; 44: 1105-1111.





Abstract
Objectives: To examine terrorism survivors’ perceptions of factors likely to promote coping and recovery, and to determine whether coping supports vary according to demographic, physical and mental health, incident-exposure and bereavement variables.
Design, setting and participants: Individuals directly exposed to and/or bereaved by the 2002 Bali bombings and who had participated in a New South Wales Health therapeutic support program completed cross-sectional telephone interviews during July–November 2010. Spoken passages were categorised into coping support themes. Advocated supports were then examined by demographic, physical and mental health, incident-exposure and bereavement variables.
Main outcome measures: Based on their experiences, respondents identified personal, social and service-related factors that they believed would optimally support future survivors of terrorism.
Results: Of the 81 people contacted, 55 (68%) participated, providing a total of 114 comments. Thirty-two respondents were women, and 54 had lost relatives or friends in the bombing. Mean age was 50 years (range, 20–73 years). Four meaningful coping support themes emerged, with excellent inter-rater reliability: professional help and counselling; social support; proactive government response and policy; and personal coping strategies. Women were significantly more likely to advocate the need for proactive government response (P = 0.03). Men were more likely to endorse the use of personal coping strategies (P < 0.01). Respondents diagnosed with a mental health condition since the bombings were significantly less likely to advocate social support processes (P = 0.04).
Conclusions: Our findings highlight the perceived value of counselling-related services for terrorism-affected groups. Male survivors may benefit more from mental health interventions that initially build on problem-focused forms of coping, including brief education about reactions and periodic check-ups. Proactive government health and support services that allow simplified and longer-term access were consistently identified as priority areas.