Mastocytosis refers to a group of disorders of mast cell proliferation, in most cases associated with mutations of the c-kit proto-oncogene. The World Health Organization classifies this condition into the categories of cutaneous mastocytosis, systemic mastocytosis, mast cell leukaemia and sarcoma, and extracutaneous mastocytoma.1 Systemic disease is confirmed by demonstrating an abnormal mast cell infiltrate in an extracutaneous site, most often through a bone marrow biopsy.
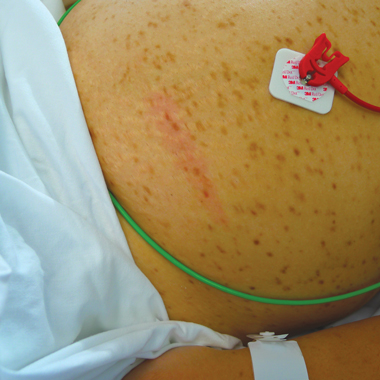
Urticaria pigmentosa is the most common presentation of mastocytosis in the skin. It is characterised by multiple red and brown macules, typically on the trunk, which “urticate” (ie, become swollen, itchy and red) when stroked or rubbed — the so-called Darier’s sign. Most cases of urticaria pigmentosa occur in early childhood, and these have a favourable prognosis, often involving skin alone. Cases that occur in adulthood, typically developing between the ages of 20 and 40 years, are usually associated with systemic disease. Some studies suggest the frequency of occult bone marrow involvement in affected adults to be as high as 92%.2 Neither the frequency nor the severity of systemic events seem to correlate with the category of mastocytosis or the burden of neoplastic cells.3
The manifestations of systemic mastocytosis may be due to the release of mast cell-derived molecules or the direct infiltration of mast cells into tissue, including the bone marrow, liver, spleen, lymph nodes and gastrointestinal tract. Mast cells are known to release a large array of molecules, including histamine, heparin, tryptase, leukotrienes and prostaglandins. Mastocytosis may be associated with symptoms of pruritus, flushing, headache, palpitations, light-headedness, dyspnoea, wheezing, abdominal pain, nausea, vomiting, diarrhoea and musculoskeletal pain. Anaphylaxis is an uncommon presentation that is generally associated with systemic involvement, although patients with mastocytosis apparently confined to the skin may still be at risk of anaphylaxis.4
A biopsy of the distinctive pigmented macules of urticaria pigmentosa will usually demonstrate an elevated number of mast cells in the dermis, although the diagnosis may be missed by pathologists in the absence of clinical guidance. Systemic mastocytosis is suggested by an increased level of mast cell mediators. A serum tryptase level greater than 20 μg/L strongly suggests systemic mastocytosis,5 although transient elevations may occur after acute mast cell degranulation, and testing should be repeated if levels are initially elevated. Changes in the coagulation profile during acute episodes may be due to the release of heparin from mast cells. Bone marrow biopsy should be considered in all patients with suspected systemic mastocytosis, even in the absence of a raised serum tryptase level.6
Treatment of mastocytosis is primarily symptomatic, although cytoreductive therapy is sometimes indicated in aggressive cases or for treatment of an associated clonal haematological non-mast cell lineage disease. Antihistamines (H1 blockers) are often sufficient to control the pruritus and flushing, and phototherapy can also be helpful for the cutaneous manifestations.7 Combined H1 and H2 blockers, proton pump inhibitors, and mast cell stabilisers such as sodium cromoglycate may help alleviate gastrointestinal symptoms. Short courses of prednisolone may be needed for severe symptoms. Other agents used include leukotriene antagonists and, more recently, omalizumab.8
Adrenaline remains the drug of choice for treating acute anaphylaxis, and an adrenaline auto-injector prescription and anaphylaxis management plan should be considered for all patients with systemic mastocytosis, irrespective of the severity of prior reactions. The wearing of emergency identification, such as a MedicAlert bracelet, should be encouraged. Severe systemic allergic reactions are well recognised in response to Hymenoptera (eg, bee and wasp) stings,9 and care should be taken to avoid stings when engaging in outdoor activities. In cases of known allergy, venom immunotherapy should be strongly considered. Agents that may precipitate mast cell degranulation, such as aspirin, other non-steroidal anti-inflammatory drugs, radiocontrast media and opiates, should be avoided. Rarely, procedures such as endoscopy and general anaesthesia have been reported to trigger cardiovascular collapse in patients with mastocytosis,10 and prophylactic corticosteroids and antihistamines have been advocated, although they may not necessarily be protective.
Systemic mastocytosis is a rare cause of severe or fatal anaphylaxis, which may be triggered by an insect sting or drug. Most patients with mastocytosis will have a history of pigmented macules on the skin that urticate when rubbed, or display symptoms related to mast cell mediator release. An awareness of this condition, its potential triggers, and both prophylactic and self-administered emergency treatment may help to avoid a life-threatening situation.
- 1. Tefferi A, Vardiman JW. Classification and diagnosis of myeloproliferative neoplasms: the 2008 World Health Organization criteria and point-of-care diagnostic algorithms. Leukemia 2008; 22: 14-22.
- 2. Fearfield LA, Francis N, Henry K, et al. Bone marrow involvement in cutaneous mastocytosis. Br J Dermatol 2001; 144: 561-566.
- 3. Wimazal F, Geissler P, Shnawa P, et al. Severe life-threatening or disabling anaphylaxis in patients with systemic mastocytosis: a single-center experience. Int Arch Allergy Immunol 2012; 157: 399-405.
- 4. Brockow K, Jofer C, Behrendt H, Ring J. Anaphylaxis in patients with mastocytosis: a study on history, clinical features and risk factors in 120 patients. Allergy 2008; 63: 226-232.
- 5. Schwartz LB, Irani AM. Serum tryptase and the laboratory diagnosis of systemic mastocytosis. Hematol Oncol Clin North Am 2000; 14: 641-657.
- 6. Lee JK, Vadas P. An elusive case of systemic mastocytosis. Allergy Asthma Clin Immunol 2010; 6 Suppl 1: P24.
- 7. Prignano F, Troiano M, Lotti T. Cutaneous mastocytosis: successful treatment with narrowband ultraviolet B phototherapy. Clin Exp Dermatol 2010; 35: 914-915.
- 8. Douglass JA, Carroll K, Voskamp A, et al. Omalizumab is effective in treating systemic mastocytosis in a nonatopic patient. Allergy 2010; 65: 926-927.
- 9. Fricker M, Helbling A, Schwartz L, Muller U. Hymenoptera sting anaphylaxis and urticaria pigmentosa: clinical findings and results of venom immunotherapy in ten patients. J Allergy Clin Immunol 1997; 100: 11-15.
- 10. Vaughan ST, Jones GN. Systemic mastocytosis presenting as profound cardiovascular collapse during anaesthesia. Anaesthesia 1998; 53: 804-807.





We acknowledge the contribution of Dr Desmond Gan in determining the initial diagnosis and assisting in the preparation of this article. We are grateful to the patient’s family for allowing us to report the details of this case.
No relevant disclosures.