Aboriginal and Torres Strait Islander people are 14 times more likely to be incarcerated than non-Indigenous Australians and represent 26% of the custodial population,1 despite being less than 3% of the Australian population.2 There are complex links between incarceration, social adversity and poor mental health for Indigenous people.3-5 While it is recognised that the prevalence of mental disorder among the general prison population is much higher than in the community,6,7 knowledge about the prevalence of mental illness among Indigenous people in custody is limited.8 This is particularly disconcerting given that the report of the Royal Commission into Aboriginal Deaths in Custody,9 released two decades ago, highlighted the need to better understand the mental health of Indigenous Australians in custody.
A recent report on the general health of Aboriginal inmates5 suggested that the prevalence of mental disorder among Indigenous inmates was high. Similarly, the high rates of death by drug overdose and suicide,10,11 and of hospital admissions for severe mental illness in this group12 in the immediate postrelease period, support this premise. Although previous studies have pointed to a high prevalence of mental illness among Indigenous prisoners,8 many have suffered from ill defined sampling frames that jeopardise generalisability, a lack of systematic screening within these sampling frames, exclusive reliance on screening instruments to identify possible mental illness and, most importantly, a lack of cultural sensitivity in the conceptualisation of mental illness and study design and implementation.
The CIDI is a comprehensive, well validated, fully standardised interview that can be used to assess mental health disorders according to the criteria in the International statistical classification of diseases and related health problems, 10th revision.13 Individuals can meet diagnostic criteria for more than one mental disorder; we anticipated that co-occurring disorders were likely. Although the CIDI has not been validated for an Australian Indigenous population, it was chosen because (i) the Indigenous mental health experts consulted in the design of our research judged that it was appropriate to diagnose depression, anxiety and substance misuse disorders in this population, and (ii) it has been widely used with Indigenous populations in other large prisoner studies14 and in major national mental health epidemiological surveys.15
To prevent culturally congruent experiences being misinterpreted as psychotic experiences,16 the full CIDI interview was not used to identify psychotic disorders; instead, we adopted a three-step process. First, the sample was screened with the CIDI psychosis screener, included in the questionnaire, to identify potential cases. Second, those who screened positive underwent face-to-face interviews with a forensic psychiatrist, who used the interview and all available clinical data to determine the presence or absence of a diagnosis. Third, this information, recorded in a standardised format, was reviewed by a diagnostic panel comprised of two psychiatrists and a cultural adviser (an Indigenous mental health clinician) to reach a consensus diagnosis.
On 30 June 2008, there were 5544 adults in Queensland prisons,18 of whom 1381 men and 116 women identified as Indigenous. In the six centres surveyed, there were 1036 Indigenous men and 88 Indigenous women.
Most participants (79.7%) identified as Aboriginal, about half (51.6%) were not in a relationship and almost two-thirds (61.8%) were unemployed (Box 1). Most did not complete education beyond Year 10; of these, around a quarter of men (23.0%) and a fifth of women (19.4%) did not complete Year 8 schooling. Almost two-thirds (63.7%) were sentenced prisoners; the remainder were individuals who were remanded in custody. Nearly half (46.1%) had been incarcerated four or more times. Over half the men (52.2%) and 37.5% of the women reported having spent time in youth custody, with 23.1% of men and 9.7% of women having spent more than a year in youth custody.
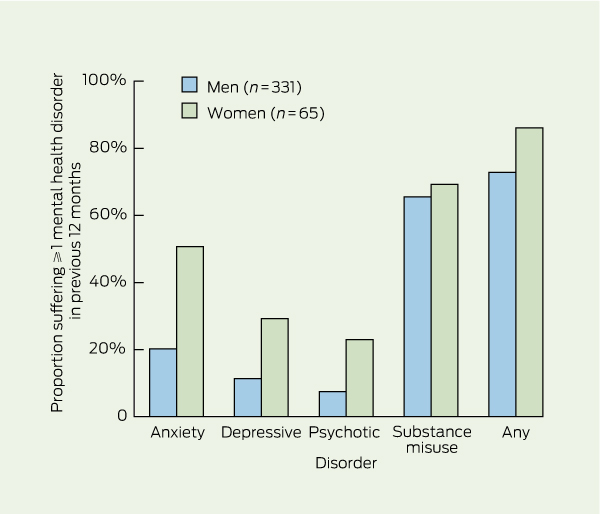
Of the 396 individuals who completed both the questionnaire and the CIDI, most men (72.8%) and women (86.1%) suffered from at least one mental health disorder in the preceding 12 months (Box 2). Two-thirds (66%) suffered from a substance misuse disorder, 25.2% from an anxiety disorder, 14.3% from a depressive disorder, and 10.1% from a psychotic disorder. Mental health disorders were more common among the remanded sample (84.4%) than in the sentenced sample (70.4%) (relative risk [RR], 1.12; 95% CI, 1.08–1.33; P = 0.002).
Women were significantly more likely than men to report suffering from an anxiety disorder (RR = 2.5; 95% CI, 1.8–3.5), a depressive disorder (RR = 2.6; 95% CI, 1.6–4.1) or a psychotic disorder (RR = 3.1; 95% CI, 1.8–5.3). The most common anxiety disorder among both men and women was post-traumatic stress disorder and the most prevalent depressive disorder was major depression (Box 3).
Of the 419 individuals administered the CIDI psychosis screener, 71 (16.9%) screened positive. Of these, eight men and one woman were unable to be assessed by a psychiatrist as they were either released or transferred before the assessment. Of the remaining 62 individuals, 28 men and 18 women were found to have a psychotic disorder (Box 4).
The majority of both men and women had a substance misuse disorder (Box 5), most commonly alcohol dependence (48.2%) or cannabis dependence (21.0%). Most individuals who had a substance misuse disorder had the more severe form — dependence.
Among the Indigenous inmates sampled, most men and women were diagnosed with at least one mental disorder, whereas the 12-month prevalence of mental disorder among adults in the Australian community is estimated at 20%.15 Given the vast overrepresentation of Indigenous people in prison, their frequent transition between prison and the community, and the high prevalence estimates of mental disorder in this group, the consequences of inadequate health care in prison7,19 must inevitably affect Indigenous communities. The prevalence of depression and anxiety disorders, especially post-traumatic stress disorder, was high in this sample, and is similar to prevalence estimates of general prison populations,14 highlighting the critical need for adequate mental health services in prison settings.7 The high prevalence of diagnosed psychotic disorder, particularly among women, is of concern and is consistent with other Australian studies.14,20 Psychotic disorder is associated with significant morbidity21 and increased risk of reincarceration.22 These findings highlight a critical mental health need for these individuals, both in custody and during the transition back to their communities.
This study, like others before it,8 identified a high rate of substance use problems among Indigenous prisoners. However, most previous studies have relied exclusively on screening instruments to do this, whereas our study has, for the first time, robustly estimated the diagnostic prevalence of harmful levels of substance misuse and dependence among Indigenous prisoners. The National Indigenous Drug and Alcohol Committee recently highlighted the lack of opportunities that exist for Indigenous people to access appropriate treatment for these problems in custody.23 It suggested that, if available, culturally appropriate interventions are likely to be successful, and it provided clear recommendations about how to implement these services. Evaluation of such services, in a way that is both culturally sensitive and scientifically rigorous, is an essential next step.
The information obtained from our research is crucial to the planning and implementation of adequate mental health services for Indigenous people in contact with and leaving the criminal justice system. For mental health services to be effective, they must be culturally capable, and accessible both in custody and in the community, with a focus on enabling continuity of care between the two. Such services can only be achieved through appropriate resourcing and stewardship. Their development is not only supported from a public health perspective, but also from human rights and ethical perspectives.24,25
While the marked over-representation of Indigenous people in Australian prisons remains a significant concern, prisons provide an opportunity for health care for a population who underaccess health care in the community.26 Although reducing the Indigenous incarceration rate remains a priority, improving the mental health of Indigenous Australians, including those who come into contact with the criminal justice system, is also important. Access to appropriate treatment may help prevent the “revolving door” of incarceration.
1 Demographic characteristics of participants among Indigenous people in Queensland prisons, May–June 2008 (n = 419)
2 Twelve-month prevalence of mental health disorder among Indigenous people in Queensland prisons, May–June 2008 (n = 396)*
3 Twelve-month prevalence of anxiety and depressive disorder among Indigenous people in Queensland prisons, May–June 2008 (n = 396)*
4 Twelve-month prevalence of psychotic disorder among Indigenous people in Queensland prisons, May–June 2008 (n = 419)
Received 21 October 2011, accepted 5 March 2012
- Edward B Heffernan1
- Kimina C Andersen1
- Abhilash Dev1
- Stuart Kinner2,3
- 1 Queensland Health, Brisbane, QLD.
- 2 Centre for Population Health, Burnet Institute, Melbourne, VIC.
- 3 School of Population Health, University of Queensland, Brisbane, QLD.
We acknowledge the significant contributions of Aboriginal and Torres Strait Islander communities in Queensland and the Queensland Health Indigenous mental health workforce. We thank Queensland Corrective Services for supporting our research. This research was funded by the Mental Health Alcohol and Other Drugs Directorate, Queensland Health. Stuart Kinner is supported by National Health and Medical Research Council Career Development Fellowship No. 1004765.
No relevant disclosures.
- 1. Australian Bureau of Statistics. Prisoners in Australia, 2010. Canberra: ABS, 2010. (ABS Cat. No. 4157.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4517.0Main+Features12010? OpenDocument (accessed Mar 2012).
- 2. Australian Bureau of Statistics. Population distribution, Aboriginal and Torres Strait Islander Australians, 2006. Canberra: ABS, 2007. (ABS Cat. No. 4705.0.) http://www.abs.gov.au/ausstats/abs@.nsf/mf/4705.0 (accessed Mar 2012).
- 3. Krieg AS. Aboriginal incarceration: health and social impacts. Med J Aust 2006; 184: 534-536. <MJA full text>
- 4. Weatherburn D, Snowball L, Hunter B. The economic and social factors underpinning Indigenous contact with the justice system: results from the 2002 NATSISS. Crime and Justice Bulletin 2006; 104: 1-16. http://www.bocsar.nsw. gov.au/lawlink/bocsar/ll_bocsar.nsf/vwFiles/cjb104.pdf/$file/cjb104.pdf (accessed Mar 2012).
- 5. Indig D, McEntyre E, Page J, Ross B. 2009 NSW inmate health survey: Aboriginal health report. Sydney: Justice Health, 2010. http://www. justicehealth.nsw.gov.au/publications/Inmate_Health_Survey_Aboriginal_Health_Report.pdf (accessed Mar 2012).
- 6. Butler T, Andrews G, Allnutt S, et al. Mental disorders in Australian prisoners: a comparison with a community sample. Aust N Z J Psychiatry 2006; 40: 272-276.
- 7. White P, Whiteford H. Prisons: mental health institutions of the 21st century? Med J Aust 2006; 185: 302-303. <MJA full text>
- 8. Heffernan E, Andersen K, Kinner S. The insidious problem inside: mental health problems of Aboriginal and Torres Strait Islander people in custody. Australas Psychiatry 2009; 17 Suppl 1: S41-S46.
- 9. Johnston EC. Royal Commission into Aboriginal Deaths in Custody. National reports. Canberra: AGPS, 1991. http://www.austlii.edu.au/au/other/IndigLRes/rciadic/ (accessed Mar 2012).
- 10. Stewart LM, Henderson CJ, Hobbs MS, et al. Risk of death in prisoners after release from jail. Aust N Z J Public Health 2004; 28: 32-36.
- 11. Kinner SA, Preen DB, Kariminia A, et al. Counting the cost: estimating the number of deaths among recently released prisoners in Australia. Med J Aust 2011; 195: 64-68. <MJA full text>
- 12. Alan J, Burmis M, Preen D, Pfaff J. Inpatient hospital use in the first year after release from prison: a Western Australian population-based record linkage study. Aust N Z J Public Health 2011; 35: 264-269.
- 13. Andrews G., Peters L. The Cidi-Auto: a computerised diagnostic interview for psychiatry. Discussion paper. Sydney: CRUfAD, St Vincent’s Hospital, 2010. http://www.crufad.org/index. php/cidi/discussion-paper (accessed Oct 2011).
- 14. Butler T, Allnut S, Cain D, et al. Mental disorder in the New South Wales prisoner population. Aust N Z J Psychiatry 2005; 39: 407-413.
- 15. Slade T, Johnston A, Teeson M, et al. The mental health of Australians 2. Report on the 2007 National Survey of Mental Health and Wellbeing. Canberra: Department of Health and Ageing, 2009. http://www.health.gov.au/internet/main/publishing.nsf/content/mental-pubs-m-mhaust2 (accessed Mar 2012).
- 16. Parker R, Milroy H. Schizophrenia and related psychoses in the Aboriginal population of Australia. Aboriginal and Islander Health Worker Journal 2003; 27: 17-19.
- 17. National Health and Medical Research Council. Values and ethics: guidelines for ethical conduct in Aboriginal and Torres Strait Islander health research. Canberra: Commonwealth of Australia, 2003. http://www.nhmrc.gov.au/guidelines/publications/e52 (accessed Mar 2012).
- 18. Australian Bureau of Statistics. Prisoners in Australia, 2008. Canberra: ABS, 2008. (ABS Cat. No. 4157.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/Lookup/4517.0Main+Features12008? OpenDocument (accessed Mar 2012).
- 19. Grace J, Krom I, Maling C, et al. Review of Indigenous offender health. Australian Indigenous Health Bulletin [internet] 2011; 11: 1-20. http://healthbulletin.org.au/articles/review-of-indigenous-offender-health/ (accessed Mar 2012).
- 20. Tye CS, Mullen PE. Mental disorders in female prisoners. Aust N Z J Psychiatry 2006; 40: 266-271.
- 21. Jablensky A, McGrath, J, Herrman, H, et al. People living with psychotic illness: an Australian study 1997–98. Canberra: Commonwealth of Australia, 1999. http://www.health.gov.au/internet/main/publishing.nsf/Content/mental-pubs-p-psych (accessed Mar 2012).
- 22. Fazel S, Yu R. Psychotic disorders and repeat offending: systematic review and meta-analysis. Schizophr Bull 2011; 37: 800-810.
- 23. National Indigenous Drug and Alcohol Committee. Bridges and barriers: addressing Indigenous incarceration and health. Canberra: Australian National Council on Drugs, 2009. http://www.nidac.org.au/images/PDFs/nidac_bridges_and_barriers.pdf (accessed Mar 2012).
- 24. Office of the United Nations High Commissioner for Human Rights. Standard Minimum Rules for the Treatment of Prisoners. 1977. http://www2. ohchr.org/english/law/treatmentprisoners.htm (accessed Oct 2011).
- 25. Mental Health Consumer Outcomes Task Force. Mental health: statement of rights and responsibilities. Canberra: Commonwealth of Australia, 1991. http://www.health.gov.au/internet/main/publishing.nsf/content/mental-pubs-m-rights (accessed Mar 2012).
- 26. Australian Institute of Health and Welfare. The health of Australia’s prisoners 2009. Canberra: AIHW, 2010. (AIHW Cat. No. PHE 123.) http://www.aihw.gov.au/publication-detail/?id=6442468371 (accessed Mar 2012).





Abstract
Objective: To estimate the prevalence of mental disorder in a representative sample of Aboriginal and Torres Strait Islander people in Queensland prisons.
Design, setting and participants: Cross-sectional assessment of mental health using the Composite International Diagnostic Interview (CIDI) and clinical interviews, conducted by Indigenous mental health clinicians who undertook specific training for this purpose, with support from forensic psychiatrists when indicated. We assessed adults who self-identified as Indigenous and were incarcerated in six of the nine major correctional centres across Queensland (housing 75% of all Indigenous men and 90% of all Indigenous women in Queensland prisons) between May and June 2008.
Main outcome measures: Diagnoses of anxiety, depressive and substance misuse disorders using the CIDI; diagnosis of psychotic illness determined through psychiatrist interviews supplemented by a diagnostic panel.
Results: We interviewed 25% of all Indigenous men (347/1381; mean age, 31.5 years) and 62% of all Indigenous women (72/116; mean age, 29.2 years) incarcerated at the time of our study. The recruitment fraction was 71% for men and 81% for women. Among the 396 individuals who completed both the interview and the CIDI, the 12-month prevalence of mental disorder was 73% among men and 86% among women. This comprised anxiety disorders (men, 20%; women, 51%); depressive disorders (men, 11%; women, 29%); psychotic disorders (men, 8%; women, 23%) and substance misuse disorders (men, 66%; women, 69%).
Conclusions: The prevalence of mental disorder among Indigenous adults in Queensland custody is very high compared with community estimates. There remains an urgent need to develop and resource culturally capable mental health services for Indigenous Australians in custody.