Incarceration has major health implications. There is increasing evidence that many people in prison are there as a direct consequence of the shortfall in appropriate community-based health and social services, most notably in the areas of housing, mental health and wellbeing, substance use, disability, and family violence.1-3 The most comprehensive study of prisoner health in Australia to date, the New South Wales Inmate Health Survey, identified that two-thirds of inmates had substance use concerns and more than 74% had mental health issues in the preceding 12 months.2,3 Currently, Aboriginal prisoners represent 22% of the total Australian prisoner population, the highest proportion in 10 years.4
One of the key themes of the Royal Commission into Aboriginal Deaths in Custody was that imprisonment should be a sanction of last resort.5 Although this principle is enshrined in legislation in most states, it is highly questionable whether it is followed in practice. Aboriginal people continue to be incarcerated at truly alarming rates. On any one day, 6% of Australia’s young Aboriginal men (aged 25–30 years) are in prison.4 It has been estimated that each year up to a quarter of all young Aboriginal men have direct involvement with correctional services.4,6
Although Australian incarceration rates overall are similar to rates in other industrialised nations, averaging 163 per 100 000 adult population in 2005, national age-standardised rates for Aboriginal prisoners of 1561 per 100 000 are at an unacceptable level and rising (Box 1).4,7,8
Our young people return from gaol to the very same conditions of daily existence that create the patterns of offending in the first place. The whirl of the revolving door is never far away.9
Internationally, there is no evidence that countries with higher rates of incarceration are safer than others.7
Although the above comments focus predominantly on Aboriginal men, the situation for Aboriginal women is also grave. Aboriginal women, who currently comprise around 8% of the Aboriginal population in prison, experience higher rates of substance use and mental health issues than their male peers, many having long histories of childhood and adult sexual or physical abuse.10,11 Their specific needs warrant separate and detailed attention beyond the scope of this article.
The post-release consequences of incarceration are only just beginning to be articulated. Literature in this area is sparse. However, it is becoming evident that the first 6–12 months following release from prison is a high-risk time. Recent studies in Western Australia showed that released Aboriginal prisoners have an almost 10 times greater risk of death than the general WA population and an almost three times greater risk of death compared with their Aboriginal peers in the community. The main causes of death are suicide, drug and alcohol related events, and motor vehicle accidents.12
Attempts to offer continuity of health services from prison to the community, where they exist, are frequently thwarted by former prisoners’ inability to meet their most basic needs, such as housing, transport and Centrelink welfare payments. Nationally, Centrelink has determined that former prisoners are entitled to receive the equivalent of 1 week’s Centrelink payment to carry them through their first 2 weeks after release.13 Policies of this kind place an additional burden on already disadvantaged Aboriginal families to provide financial support for newly released family members. Additionally, former prisoners frequently lack the identification documents required to access Centrelink payments, open bank accounts and complete housing application processes.
Arguably most problematic of all is the lack of access to suitable housing. One of the few studies conducted on housing after release found that former prisoners who are re-incarcerated report that a lack of suitable housing is a key factor in their unsuccessful transition to outside life.14
The finding that 73% of Aboriginal prisoners expected to have no or insecure housing on release corresponded with our clinical experience. On community follow-up, most had left prison without accommodation in place and with few options available to them. Public housing stocks in SA are diminishing and private rental for Aboriginal men without references is rarely achievable.15 Consequently, it becomes almost impossible to provide continuity of health care to these clients, many of whom have major health needs, particularly for mental health and substance use support.
The need for better service integration can be further illustrated by considering hepatitis C treatment. In SA, close to 60% of metropolitan Aboriginal prisoners are positive for hepatitis C virus (HCV) antibodies.16
As part of the National Hepatitis C Strategy, there is an identified priority to increase HCV treatment rates. Custodial settings are seen as one of the key sites to address HCV management.17 However, as treatment programs take 6–12 months to complete and most prison stays are less than 6 months, most prisoners are effectively excluded from access to treatment because of their short prison stays and the inherent difficulties of post-release follow-up.
A culturally responsive health perspective allows us to hear what Aboriginal people have been telling us for a long time — that patterns of criminal behaviour are often an expression of the deep wells of pain, anger and grief experienced by Aboriginal people on a daily basis as a consequence of their long history of dispossession in this country.18,19 Forced separation through incarceration intensifies this, creating a further marginalised and destabilised young Aboriginal population and placing added burdens, both financial and social, on the individuals and on Aboriginal women and children.
A recent study in NSW showed that nearly half of all the young people in juvenile justice custody, 42% of whom are Aboriginal, have a history of a parent in prison. Eleven per cent have a parent currently in custody.20 For the sake of this and future generations, we must break the cycle.
1 Indigenous and non-Indigenous prisoners, rate per 100 000 adults, 1992–2004
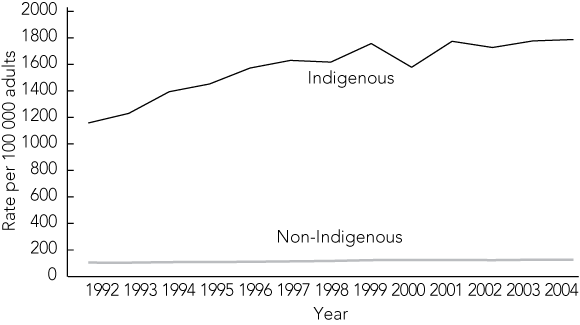
Reproduced with permission from Australian crime facts and figures 2005, Figure 91.6
2 Findings from a survey of 41 male Aboriginal prisoners at Adelaide Remand Centre, November 2005
30 (73%) expected to have insecure or no accommodation on release
15 (36%) reported being homeless before admission
37 (90%) were on Centrelink payments before admission, 2 (5%) had some casual employment, and 2 (5%) had no income at all
35 (85%) did not have a driver’s licence (ie, no photo ID)
More than half had no birth certificate or Medicare card
- Anthea Susan Krieg1
- Nunkuwarrin Yunti of South Australia Inc, Adelaide, SA.
None identified.
- 1. Mental Health Council of Australia. Not for service: experiences of injustice and despair in mental health care in Australia. Canberra: Mental Health Council of Australia, 2005. Available at: http://www.mhca.org.au/notforservice (accessed Apr 2006).
- 2. Butler T, Milner L. The 2001 New South Wales inmate health survey. Sydney: NSW Corrections Health Service, 2003. Available at: http://www.justicehealth.nsw.gov.au/2nd_level/pubs.html (accessed Apr 2006).
- 3. Butler T, Allnut S. Mental illness among New South Wales’ prisoners. Sydney: NSW Corrections Health Service, 2003. Available at: http://www.justicehealth.nsw.gov.au/2nd_level/pubs.html (accessed Apr 2006).
- 4. Australian Bureau of Statistics. Prisoners in Australia, 2004. Canberra: ABS, 2004. (ABS Catalogue No. 4517.0.)
- 5. Johnston E (Commissioner). Royal Commission into Aboriginal Deaths in Custody, National report. Volumes 1 to 5. Canberra: AGPS, 1991. Available at: http://www.austlii.edu.au/au/special/rsjproject/rsjlibrary/rciadic (accessed Apr 2006).
- 6. Australian Institute of Criminology. Australian crime facts and figures 2005. Canberra: Australian Institute of Criminology, 2006. Available at: http://www.aic.gov.au/publications/facts (accessed Apr 2006).
- 7. Stern V. A sin against the future: imprisonment in the world. Lebanon, NH: University Press of New England, 1998.
- 8. International Centre for Prison Studies. Entire world — prison population rates per 100,000 of the national population. Available at: http://www.prisonstudies.org (accessed Apr 2006).
- 9. Dodson M. Aboriginal and Torres Strait Islander Social Justice Commissioner, Fourth report 1996. Sydney: Human Rights and Equal Opportunity Commission, 1996. Available at: http://www.hreoc.gov.au/Social_Justice/sj_reports.html#96 (accessed Apr 2006).
- 10. Johnson H. Risk factors for drug use and offending. In: Drugs and crime: a study of incarcerated female offenders. Chapter 6. Canberra: Australian Institute of Criminology, 2004. Available at: http://www.aic.gov.au/publications/rpp/63 (accessed Apr 2006).
- 11. Lawrie R. Speak out speak strong. Researching the needs of Aboriginal women in custody. Sydney: Aboriginal Justice Advisory Council, 2003. Available at: http://www.lawlink.nsw.gov.au/ajac.nsf/pages/reports (accessed Apr 2006).
- 12. Stewart LM, Henderson CJ, Hobbs MS, et al. Risk of death after release from jail. Aust N Z J Public Health 2004; 28: 32-36.
- 13. Australian Government Department of Family and Community Services. Guide to social security law. Section 3.1.4 Imprisonment, psychiatric confinement and prison release. Available at: http://www.facs.gov.au/guide/ssguide/314.htm (accessed Apr 2006).
- 14. Baldry E, McDonnell D, Maplestone P, Peeters M. Ex-prisoners and accommodation: what bearing do different forms of housing have on social reintegration of ex-prisoners? Presented at Housing, crime and stronger communities conference. Australian Institute of Criminology. Melbourne, 6–7 May 2002. Available at: http://www.aic.gov.au/conferences/housing (accessed Apr 2006).
- 15. Haggerty R. Ending homelessness in South Australia. Adelaide: Department of the Premier and Cabinet, 2005. Available at: http://thinkers.sa.gov.au/reports.html (accessed Apr 2006).
- 16. Miller ER, Bi P, Ryan P. The prevalence of HCV antibody in South Australian prisoners. J Infect 2006. In press.
- 17. Australian Government Department of Health and Ageing. National hepatitis C strategy 2005–2008. Canberra: Department of Health and Ageing, 2005. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/Hepatitis+C-1 (accessed Apr 2006).
- 18. Blair EM, Zubrick RS, Cox AH; WAACHS Steering Committee. The Western Australian Aboriginal Child Health Survey: findings to date on adolescents. Med J Aust 2005; 183: 433-435. <MJA full text>
- 19. Atkinson J. The transgenerational effects of trauma within Indigenous Australia. PhD thesis. Brisbane: Queensland University of Technology, 2002. (QUT 368/9.)
- 20. New South Wales Department of Juvenile Justice. 2003 NSW young people in custody health survey. Key findings report. Sydney: Department of Juvenile Justice, 2003. Available at: http://www.djj.nsw.gov.au/publications.htm (accessed Apr 2006).





Abstract
Each year up to a quarter of all young Aboriginal men have direct involvement with correctional services, and Aboriginal prisoners currently represent 22% of the total Australian prisoner population.
The high rates of repeated short-term incarceration experienced by Aboriginal people in Australia have a multitude of negative health effects for Aboriginal communities and the wider society, while achieving little in terms of increased community safety.
Well identified health and social priorities for Aboriginal people affected by incarceration include housing and tenancy support; mental health and wellbeing, including family violence, grief and loss support; substance misuse support; general health services, including hepatitis C management; and social inclusion, including the need for family and community integration, skills development and employment.
The post-release period is a crucial time for the provision of integrated health and social services to address these priorities and to break the cycle of incarceration.
To achieve significant health gains for Aboriginal people, there is a need to develop a broader collaborative approach to primary health care, incorporating social health and justice perspectives as fundamental components of health care planning.
Health and human services have a critical role to play in developing community-based solutions to reduce excessive incarceration rates for Aboriginal people.