Quitlines are well placed to deliver smoking cessation treatment, given their mass reach, convenience of access, and capacity to tailor to the individual and to offer multiple contacts. A Cochrane review,1 including a randomised controlled trial of the Quitline call-back service2 run by Quit Victoria, demonstrated that call-back cessation services (where the service initiates the subsequent calls to smokers) are effective for the general population. Quitline uses cognitive-behavioural and motivational interviewing principles. It offers up to three pre-quitting and up to five post-quitting calls over a period of about 2 months.
The high incidence of lifetime depression among smokers3 suggests the need to provide collaborative care between call-back services and doctors. While Quitline staff are experts in the cognitive-behavioural treatment of smoking, a number of issues require medical management, including: (i) current depression makes quitting smoking more difficult;4 (ii) smoking cessation may increase the risk of relapse of major depressive disorder which therefore requires monitoring;5 (iii) smoking cessation may require changes in medications affected by nicotine;6 and (iv) this allows for prescription of medications that dually act to aid smoking cessation and alleviate depression.4 Victoria’s Quitline is the first in Australia to have developed and instituted a tailored Quitline–doctor comanagement of smoking cessation call-back and depression. The service draws on existing evidence-based recommendations for comanagement7 and evidence that integrated cognitive-behavioural treatments may help smokers develop better management skills for both smoking cessation and depression.8
Quitline–doctor comanagement has been facilitated by the fact that fax-referral to Quitline is now an integral part of the Australian guidelines for smoking cessation in general practice.9 Indeed, referral to Quitline was reported as one of the most useful aspects.10 A cluster randomised trial of in-practice management of smoking cessation versus doctor fax-referral to Victoria’s Quitline (of any patients) demonstrated an almost threefold increase in sustained smoking cessation rates at 12 months for the referral group, largely because referral increased the amount of cessation assistance received by patients (both groups received equivalent in-practice assistance).11
Quitline–doctor comanagement of smoking cessation is activated by the doctor faxing a signed referral form to Quitline, which includes a section committing the doctor to managing comorbid health issues (eg, depression) and to reviewing and monitoring medications. Quitline then sends automated feedback letters to doctors on their patient’s progress with quitting, designed to mimic feedback from a specialist referral. The letters invite doctors to contact Quitline if they have any queries or comments, and this occurs occasionally, with feedback entered into the client’s record. Quitline advisers ask smokers about their doctor’s advice, which informs the quitting plan. At follow-up, advisers ask about subsequent doctor visits.
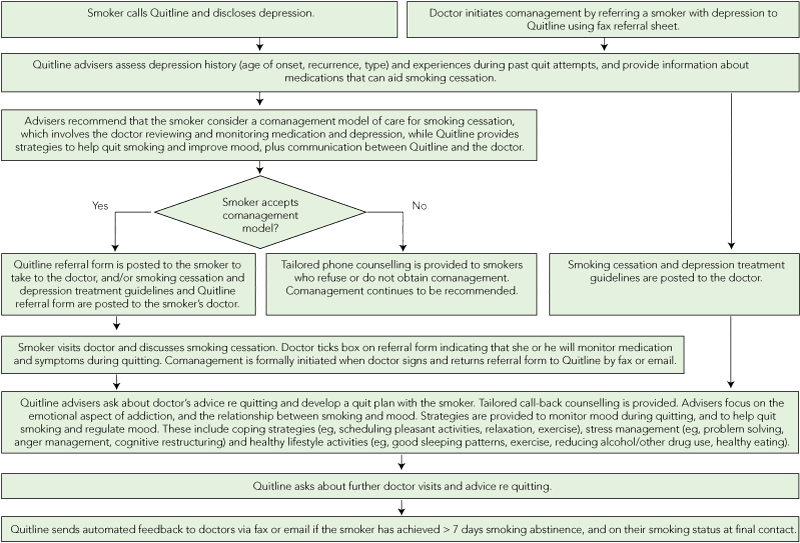
In 2008, a third of clients using Quitline’s call-back service were receiving comanagement. A distinguishing feature of Quitline–doctor comanagement is that it can be initiated either by the doctor referring a patient or by Quitline, whereby a smoker contacting the service is sent a fax-referral form to take to their doctor. The Victorian Quitline’s mental health policy recommends comanagement for all smokers with a mental health condition (defined as use of prescription medications for mental health and/or experience of mental ill-health in the previous 6 months). This is because Quitline staff are working within the limitations of a phone service and are not medically trained; thus they are not in a position to competently manage issues such as interactions between chemicals in cigarettes and psychotropic medications, and their potential effects in exacerbating or precipitating mental health symptoms. Smokers seeking assistance from Quitline are encouraged to disclose health problems, including mental health problems; about a quarter disclose a mental health problem, most commonly depression and often at a subclinical level. The comanagement model for smokers with depression is shown in Box 1 and includes sending treatment guidelines for smoking cessation and depression to doctors, and tailoring the Quitline call-back counselling for depression.12
The objectives of our study were: (i) to report smokers’ uptake and evaluations of Quitline–doctor comanagement of smoking cessation and depression; (ii) to explore the relationship between comanagement and quitting success; and (iii) to investigate whether quitting was associated with exacerbation of depression.
Key baseline measures are listed in Box 2. Baseline depressive symptoms were assessed using the Patient Health Questionnaire (PHQ-9),13 a nine-item scale (each rated 0 for “not at all” to 3 for “nearly every day”) with a summed score range of 0–27. To relieve response burden, if participants scored zero for the first two items — “little interest or pleasure in doing things” and “feeling down, depressed and hopeless” — their PHQ-9 score was set at zero. Opinions and reports of doctor, Quitline and pharmacological cessation assistance were asked of participants at the 2-month follow-up interview (Box 2). The primary smoking cessation outcomes were: making a quit attempt (quit for at least 24 hours) between the baseline and 2-month follow-up, and period prevalence (quit for 4 months) at 6-month follow-up. Exacerbation of depression between baseline and 6 months was defined as a within-subject increase of more than 5 points on the PHQ-9, which put (or kept) the participant’s score in the major/severe depression categories.
Baseline patient characteristics are shown in Box 2. About two-thirds were women, almost all were planning to quit, and the mean level of baseline depression was 10.9 (SD, 7.5), which is in the moderate range. There were no significant differences in sociodemographic variables, cigarette consumption or quitting history between those with current and past depression, nor did they differ on the main outcomes of uptake of comanagement and quit rates. Participants with current depression were more likely than those with past depression to report major/severe levels of depressive symptoms (38% v 18%; χ22,220 = 6.33; P = 0.04), current psychotropic medication usage (77% v 14%; χ21,221 = 41.83; P < 0.001) and concurrent anxiety disorder(s) (34% v 14%; χ21,223 = 4.93; P = 0.03).
Strong participant support and corresponding action to involve the doctor with their quitting are shown in Box 3. Participants’ main reasons for not discussing quitting with their doctor were: “didn’t think the doctor would be able to assist” (33%), “needed to discuss other issues” (29%) and “didn’t think the doctor’s help was necessary” (16%). Participants who did not discuss quitting with their doctor (compared with those who did) were less likely to be taking prescribed psychotropic medication (50% v 71%; χ21,172 = 6.78; P = 0.009), to have experienced depression following a previous quit attempt (3% v 17%; χ21,122 = 4.81; P = 0.03) and were less addicted (smoking mean 20 v 24 cigarettes per day; t = 1.90, df = 169; P = 0.06) and smoking their first cigarette of the day later after waking (mean 43 v 18 minutes; t = − 2.60; df = 41.4; P < 0.05).
There were high levels of quitting activity (Box 4). Overall, 20% (14% if missing cases are imputed as failures) managed to maintain cessation for at least 4 months.
Among participants who spoke with their doctor about quitting, those receiving comanagement were more likely to make a quit attempt compared with participants who did not receive comanagement (78% v 63%; χ21,128 = 3.78; P = 0.05). Talking with the doctor about quitting did not increase the likelihood of making a quit attempt, perhaps because those who spoke with the doctor were more likely to have characteristics that make it harder to quit. Also, participants whose doctor discouraged quitting were less likely to make a quit attempt — 55% of those told that it was “not a good time to quit” made a quit attempt compared with 63% of those told to “proceed with caution” and 77% of those told to “go straight ahead” (χ21,117 = 3.53; P = 0.06).
Participants making quit attempts reported fewer baseline depressive symptoms (mean PHQ-9 score 9.76 v 12.40 among non-attempters; t = 2.06; df = 167; P = 0.04), and were more likely to use cessation pharmacotherapy (79% v 60% non-users; χ21,163 = 6.38; P = 0.01), be employed (80% v 67% unemployed; χ21,173 = 3.61; P = 0.06) and be men (81% v 68% women; χ21,174 = 3.39; P = 0.07).
Among participants making a quit attempt, those who achieved sustained cessation were more likely to be men (29% v 15% women; χ21,144 = 4.33; P = 0.04), received more Quitline calls (mean 4.2 v 3.2; t = − 1.93; df = 141; P = 0.06) and were more likely to use cessation pharmacotherapy (25% v 13% non-users; χ21,136 = 3.16; P = 0.08).
This project found that a well structured Quitline–doctor comanagement of smoking cessation for people with a depression history is workable, beneficial and acceptable to participants. These participants are likely to be highly motivated, as evidenced by their calling Quitline, but the high level of cessation activity (even by general population standards) among smokers reporting doctor-diagnosed depression is very encouraging. It was also reassuring that attempts at or success with smoking cessation did not increase the risk of exacerbation of depression. Further data analysis is underway to explore reductions in depressive symptoms following quitting.
The study’s main limitation is the use of an uncontrolled design. While a randomised controlled trial would have been ideal, Quitline’s mental health policy recommends comanagement for all smokers with current depression and this precluded random allocation of smokers. If the comanagement option had been taken away and problems arose, there would have been issues of liability.
As the participants were Quitline clients disclosing doctor-diagnosed depression, this sample included participants with subclinical levels of depression and as well as those independently assessed as having major depressive disorder. This is in line with the practical realities of the service, where it is not possible to routinely implement a formalised assessment and such an assessment could prove counterproductive if it excluded those who were below caseness threshold.
The key benefits of formalised doctor referral of participants to Quitline (comanagement) were increased likelihood of quit attempts and of receiving more Quitline calls, a predictor of sustained cessation. The finding that comanagement was more likely when Quitline sent the fax form directly to the participant’s doctor (as well as to the patient) supports the ongoing implementation of this strategy by Quitline. Around a quarter of participants did not speak with their doctor about quitting. This highlights the need for doctors to continue to be proactive in encouraging patients to quit and in offering assistance to do so. A Cochrane review shows that even brief simple advice increases patient success with quitting.14 Further, comanagement with Quitline is not only effective,11 but takes pressure off doctors who may be underresourced or not confident in managing smoking cessation.
Consistent with other research, higher levels of baseline depression inhibited cessation attempts. Treatment guidelines recommend that depression be treated first in preparation for smoking cessation.4 This finding reinforces the need for comanagement and justifies Quitline’s focus on strategies that target both smoking cessation and mood.
Forging routine links with Quitline provides an easy and efficient means to deliver smoking cessation treatment. The Victorian Quitline’s tailored counselling protocol for smokers with a history of depression is being shared with Quitline services nationally to help ensure that effective smoking cessation treatment which competently manages comorbid issues is available to the many smokers in the community with a history of depression. Further, this tailored treatment model has the potential to be adapted for smokers with other comorbid issues.
2 Participant baseline characteristics
Characteristic |
Mean (SD) |
||||||||||||||
Age (n = 223) |
45.2 (13.6) |
||||||||||||||
Cigarettes per day (n = 223) |
23.0 (11.3) |
||||||||||||||
Minutes to first cigarette (n = 178) |
24.5 (45.4) |
||||||||||||||
|
No. |
||||||||||||||
Sex (n = 227) |
|
||||||||||||||
Male |
79 (34.8%) |
||||||||||||||
Female |
148 (65.2%) |
||||||||||||||
Employed (n = 223) |
|
||||||||||||||
Yes |
85 (38.1%) |
||||||||||||||
No |
138 (61.9%) |
||||||||||||||
Highest education level (n = 217) |
|
||||||||||||||
Up to Year 10 |
106 (48.8%) |
||||||||||||||
Years 11 or 12 or equivalent |
54 (24.9%) |
||||||||||||||
Tertiary |
57 (26.3%) |
||||||||||||||
PHQ-9 (n = 220) |
|
||||||||||||||
None |
53 (24.1%) |
||||||||||||||
Mild/moderate |
89 (40.5%) |
||||||||||||||
Major/severe |
78 (35.5%) |
||||||||||||||
Concurrent anxiety disorder (n = 223) |
|
||||||||||||||
Yes |
70 (31.4%) |
||||||||||||||
No |
153 (68.6%) |
||||||||||||||
Taking prescription medication for mental wellbeing (n = 221) |
|||||||||||||||
Yes |
152 (68.8%) |
||||||||||||||
No |
69 (31.2%) |
||||||||||||||
Ever hospitalised for depression (n = 212) |
|
||||||||||||||
Yes |
68 (32.1%) |
||||||||||||||
No |
144 (67.9%) |
||||||||||||||
Stage of change (n = 227) |
|
||||||||||||||
Planning |
223 (98.2%) |
||||||||||||||
Ambivalent |
4 (1.8%) |
||||||||||||||
Ever made past quit attempt (n = 227) |
|
||||||||||||||
Yes |
201 (88.5%) |
||||||||||||||
Never |
26 (11.5%) |
||||||||||||||
Quit attempt in last year (n = 147) |
|
||||||||||||||
Yes |
64 (43.5%) |
||||||||||||||
No |
83 (56.5%) |
||||||||||||||
Experienced depression after quitting (n = 157) |
|||||||||||||||
Yes |
22 (14.0%) |
||||||||||||||
No |
135 (86.0%) |
||||||||||||||
Contact with Quitline (n = 227) |
|
||||||||||||||
Self-initiated |
198 (87.2%) |
||||||||||||||
Initiated after doctor referral |
29 (12.8%) |
||||||||||||||
PHQ-9 = Patient Health Questionnaire. |
|
||||||||||||||
3 Participant opinions and use of doctor, Quitline and pharmacological cessation assistance
Measure |
No. |
||||||||||||||
Good idea to involve doctor with quitting (n = 169) |
|
||||||||||||||
Agree |
141 (83.4%) |
||||||||||||||
Disagree |
28 (16.6%) |
||||||||||||||
Spoke with doctor about quitting (n = 173) |
|
||||||||||||||
Yes |
128 (74.0%) |
||||||||||||||
No |
45 (26.0%) |
||||||||||||||
Received comanagement* (n = 174) |
|
||||||||||||||
Yes |
74 (42.5%) |
||||||||||||||
No |
100 (57.5%) |
||||||||||||||
Of those discussing quitting with doctor: |
|
||||||||||||||
Mean no. of appointments about quitting (n = 120) |
2.6 (SD, 2.6) |
||||||||||||||
Who raised issue of quitting (n = 123) |
|
||||||||||||||
Patient |
82 (66.7%) |
||||||||||||||
Doctor |
41 (33.3%) |
||||||||||||||
Doctor advice re quitting (n = 117) |
|
||||||||||||||
Go straight ahead |
57 (48.7%) |
||||||||||||||
Proceed with caution |
49 (41.9%) |
||||||||||||||
Not a good time to quit |
11 (9.4%) |
||||||||||||||
Doctor recommended new medication or changes to medication (n = 120) |
|||||||||||||||
Yes |
58 (48.3%) |
||||||||||||||
No |
62 (51.7%) |
||||||||||||||
Involving doctor increased confidence to manage mood (n = 118) |
|
||||||||||||||
Yes, a lot |
46 (39.0%) |
||||||||||||||
Yes, somewhat |
30 (25.4%) |
||||||||||||||
No |
42 (35.6%) |
||||||||||||||
Helpful to have both doctor and Quitline (n = 112) |
|
||||||||||||||
Yes |
93 (83.0%) |
||||||||||||||
Prefer just doctor |
8 (7.2%) |
||||||||||||||
Prefer just Quitline |
11 (9.8%) |
||||||||||||||
Cessation management: |
|
||||||||||||||
Quitline calls received (n = 173) |
|
||||||||||||||
Initial call only (did not receive call-back service) |
30 (17.3%) |
||||||||||||||
2–3 calls |
81 (46.8%) |
||||||||||||||
≥ 4 calls |
62 (35.9%) |
||||||||||||||
Quitline call-back service helpful (n = 174) |
|
||||||||||||||
Very |
127 (73.0%) |
||||||||||||||
Somewhat |
32 (18.4%) |
||||||||||||||
Not at all |
15 (8.6%) |
||||||||||||||
Used cessation medication (n = 163) |
|
||||||||||||||
Yes |
105 (64.4%) |
||||||||||||||
No |
58 (35.6%) |
||||||||||||||
Type of cessation medication used (n = 174) |
|
||||||||||||||
Varenicline |
56 (32.2%) |
||||||||||||||
Nicotine replacement |
54 (31.0%) |
||||||||||||||
Bupropion |
21 (12.1%) |
||||||||||||||
* Doctor completes the Quitline fax-referral, which activates Quitline feedback on participant’s progress with quitting. |
|||||||||||||||
4 Quit rates
Measure |
No. of respondents |
All cases |
|||||||||||||
2-month follow-up |
174 |
227 |
|||||||||||||
Made quit attempt |
|
|
|||||||||||||
Yes |
126 (72.4%) |
126 (55.5%) |
|||||||||||||
No |
48 (27.6%) |
101 (44.5%) |
|||||||||||||
Point-prevalence abstinence |
|
|
|||||||||||||
Yes |
65 (37.4%) |
65 (28.6%) |
|||||||||||||
No |
109 (62.6%) |
162 (71.4%) |
|||||||||||||
6-month follow-up |
159 |
227 |
|||||||||||||
Point-prevalence abstinence |
|
|
|||||||||||||
Yes |
52 (32.7%) |
52 (22.9%) |
|||||||||||||
No |
107 (67.3%) |
175 (77.1%) |
|||||||||||||
Quit for ≥ 4 months (sustained abstinence) |
|||||||||||||||
Yes |
32 (20.1%) |
32 (14.1%) |
|||||||||||||
No |
127 (79.9%) |
195 (85.9%) |
|||||||||||||
- Catherine J Segan1
- Ron Borland2
- Kay A Wilhelm3
- Sunil S Bhar4
- Ainslie T Hannan2
- David R Dunt1
- Ian T Ferretter2
- 1 School of Population Health, University of Melbourne, Melbourne, VIC.
- 2 The Cancer Council Victoria, Melbourne, VIC.
- 3 St Vincent's Hospital, Sydney, NSW.
- 4 Faculty of Life and Social Sciences, Swinburne University of Technology, Melbourne, VIC.
We thank participating Quitline clients, Quitline advisers for recruitment, and the research interviewers Diane Abbott, Anthony Talbot, and Jessica Ross. The project was primarily funded by the Victorian Centre of Excellence in Depression and Related Disorders, an initiative between beyondblue and the State Government of Victoria, with contribution from Quit Victoria.
Ainslie Hannan and Ian Ferretter are employed by Quit Victoria. Together with Catherine Segan, Kay Wilhelm and Sunil Bhar, they developed and implemented Quit Victoria’s tailored service for depression-history smokers evaluated in this study. Ron Borland is employed by The Cancer Council Victoria, which houses Victoria’s Quitline. He has conducted research on the Quitline and has an ongoing interest in helping them improve the quality of their services.
- 1. Stead L, Perera R, Lancaster T. Telephone counselling for smoking cessation. Cochrane Database Syst Rev 2006; (3): CD002850.
- 2. Borland R, Segan C, Livingston P, Owen N. The effectiveness of callback counselling for smoking cessation: a randomised trial. Addiction 2001; 96: 881-889.
- 3. Degenhardt L, Hall W. The relationship between tobacco use, substance-use disorders and mental health: results from the National Survey of Mental Health and Wellbeing. Nicotine Tob Res 2001; 3: 225-234.
- 4. Wilhelm K, Richmond R, Wodak A. Clinical aspects of nicotine dependence and depression. Med Today 2004; 5: 40-46.
- 5. Hughes JR. Depression during tobacco abstinence. Nicotine Tob Res 2007: 9: 443-446.
- 6. Zevin S, Benowitz NL. Drug interactions with tobacco smoking. An update. Clin Pharmacokinet 1999; 36: 425-438.
- 7. Wilhelm K, Arnold K, Niven H, Richmond R. Grey lungs and blue moods: smoking cessation in the context of lifetime depression history. Aust N Z J Psychiatry 2004; 38: 896-905.
- 8. Brown RA, Kahler CW, Niaura R, et al. Cognitive-behavioral treatment for depression in smoking cessation. J Consult Clin Psychol 2001; 69: 471-480.
- 9. Zwar N, Richmond R, Borland R, et al. Smoking cessation guidelines for Australian general practice. Canberra: Australian Government Department of Health and Ageing, 2004.
- 10. Richmond R, Zwar N, Borland R, et al. Smoking cessation for Australian general practice: evaluation of best practice guidelines. Aust Fam Physician 2005; 34: 505-507.
- 11. Borland R, Balmford J, Bishop N, et al. In-practice management v quitline referral for enhancing smoking cessation in general practice: a cluster randomised trial. Fam Pract 2008; 25: 382-389.
- 12. Quit Victoria. Smoking cessation guidelines for working with callers with current, past or suspected depression. Melbourne: Tobacco Control Unit, The Cancer Council Victoria, 2010.
- 13. Kroenke K, Spitzer RL, Williams JB. The PHQ-9: validity of a brief depression severity measure. J Gen Intern Med 2001; 16: 606-613.
- 14. Stead L, Bergson G, Lancaster T. Physician advice for smoking cessation. Cochrane Database Syst Rev 2008; (2): CD000165.





Abstract
Objectives: To report smokers’ evaluations and uptake of Quitline–doctor comanagement of smoking cessation and depression, a key component of the Victorian Quitline’s tailored call-back service for smokers with a history of depression and to explore its relationship to quitting success.
Design, participants and setting: Prospective study followed Quitline clients disclosing doctor-diagnosed depression (n = 227). Measures were taken at baseline (following initial Quitline call), posttreatment (2 months) and 6 months from recruitment (77% and 70% response rates, respectively).
Main outcome measures: Uptake of comanagement (initiated by fax-referral to Quitline), making a quit attempt (quit for 24 hours), sustained cessation (> 4 months at 6-month follow-up).
Results: At 2-month follow-up, 83% thought it was a good idea to involve their doctor in their quit attempt, 74% had discussed quitting with their doctor, and 43% had received comanagement. In all, 72% made a quit attempt, 37% and 33% were abstinent posttreatment and at 6 months, respectively, and 20% achieved sustained cessation. Among participants who discussed quitting with their doctor, those receiving comanagement were more likely to make a quit attempt than those who did not receive comanagement (78% v 63%). Participants with comanagement also received more Quitline calls (mean 4.6 v 3.1) — a predictor of sustained cessation. Exacerbation of depression between baseline and 6 months was reported by 18% of participants but was not related to cessation outcome.
Conclusion: Quitline–doctor comanagement of smoking cessation and depression is workable, is valued by smokers, and increases the probability of quit attempts. Smoking cessation did not increase the risk of exacerbation of depression.