Medicolegal matters are not uniformly distributed across the medical workforce. Previous research has shown that malpractice lawsuits,1-8 complaints,8-11 no-fault compensation claims,12 disciplinary proceedings,8,13-15 and other referrals to oversight bodies8,16 tend to cluster among relatively small groups of doctors, who have identifiable characteristics. However, only three of these studies have centred on complaints: two were reviews of internal complaints within United States medical groups;9,10 the other was a survey of New Zealand doctors.11
Patient complaints can provide useful insights into quality of care and patient dissatisfaction.17,18 This is particularly true in Australia, where complaints to health service commissions — regulatory agencies that operate in all eight states and territories, resolving thousands of complaints each year — have become the primary avenue for medicolegal redress. Unlike lawsuits or disciplinary actions, complaints to commissions are almost entirely patient-driven, legal representation is not required, and matters are usually resolved within months.19
We analysed complaints against doctors in private practice in Victoria. We describe the distribution of these complaints and profile the subgroup of doctors involved in a disproportionately large number of them. Our goal was to inform strategies for identifying and intervening early with complaint-prone doctors.19
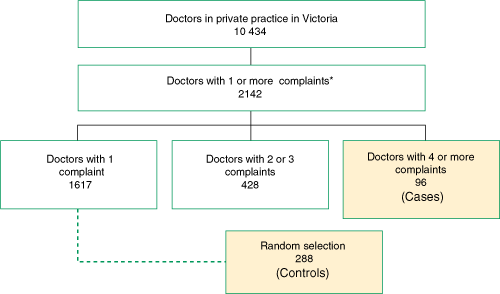
We queried the database of the Health Services Commissioner of Victoria (“the Commissioner”) to identify all doctors in Victoria who were the subject of one or more complaints in the decade 1 January 2000 to 31 December 2009. We focused on doctors in private practice because the Commissioner’s complaint resolution processes for public hospital services do not identify individual doctors. In 2004, the midpoint of our study period, 14 581 doctors were registered to practice in Victoria: 72% (10 434) were in private practice, either fully (7052) or partially (3382), and 28% (4147) were in public practice only.20
Three-quarters (1617/2141) of doctors complained against were the subject of a single complaint during the study period, and 20% (428/2141) were the subject of two or three complaints (Box 1). A total of 96 doctors had four or more complaints (median, 5; interquartile range, 4–6); this is the group we defined as complaint-prone and analysed further.
Box 2 shows the distribution of complaints among doctors. Complaint-prone doctors constituted 4.5% of doctors complained against (95% CI, 3.6%–5.4%) and accounted for 17.6% of all complaints (95% CI, 16.3%–19.0%).
More generally, our findings reinforce the conclusion of previous research that it is incorrect at the population level to construe doctors’ experiences with medicolegal matters as merely the “luck of the draw”.7 Complaints clearly cluster around certain doctors — in Victoria, extrapolations from our findings indicate that less than 100 practitioners, or 1% of the medical workforce in private practice, account for nearly 20% of complaints.
It would be a feasible proposition to mount interventions in a group of this size, and this may help improve patient satisfaction, quality of care, and public confidence in the health care system. Such interventions should be tailored to the concerns identified in complaints and the degree of recidivism. At the low end of the spectrum, they may involve simple guidance (eg, information and feedback), graduating to moderately intrusive measures (eg, specific professional development modules). At the upper end of the spectrum, stronger interventions may be warranted (eg, referral for competence or health assessment), rising to practice restrictions by the appropriate agency where required. In most cases, remediation, re-skilling, or rehabilitation should be enough to help doctors return to safe practice.16
Why surgeons and psychiatrists are disproportionately at risk is not well understood. Previous complaints studies have identified the same phenomenon,9,10,18 as have studies of other medicolegal matters.1,2,5,7-10,12,13,15,16 In surgery, the inherent risks of surgical procedures and the relative visibility of poor outcomes of care are likely to play a role.21 In psychiatry, certain patients may have an increased propensity to initiate medicolegal action, although, despite speculation about this phenomenon, there is little hard evidence of it.22 Additionally, the potential for power imbalances between doctor and patient is high in both specialties.
Previous studies have found that overseas training is not a risk factor for complaints;8,11 our findings go a step further and find a “protective effect” associated with training outside of Australia. The extent to which this effect can be generalised is questionable. For example, a recent report from the United Kingdom indicated a higher rate of referral to the National Clinical Assessment Service for non-white doctors and doctors who qualified outside Europe.23
Our study has some limitations. First, we used head counts of practitioners in each descriptive category, rather than more sophisticated measures of doctors’ exposure to complaint risk, such as full-time equivalents, or volumes of patients seen and procedures conducted. Second, we selected our control group from among doctors who had experienced one isolated complaint over a decade, rather than doctors who had experienced none. A comparison of the doctors in our control group to summary statistics for all doctors in Victoria suggests that our controls closely resemble the wider pool in terms of specialty and location,20 but slightly larger proportions were male and had been in practice for more than 21 years. These differences, although minor, open up the possibility of biases toward the null in our analyses of sex and years in practice. Third, the characteristics we examined were doctor-focused. Patient characteristics,24,25 treatment outcomes,24 and the nature of the patient–doctor relationship26-29 are also likely to be important predictors. Finally, our findings are from an analysis of complaints against doctors in private practice in Victoria; the extent to which they can be generalised to practitioners in public hospital settings and in other states is unknown.
The insight that large numbers of complaints are concentrated among a small group of doctors, and that those doctors exhibit distinctive characteristics, has important policy implications. Case-by-case complaint resolution processes overlook the importance of past complaints as a predictor of future complaints, and spread regulators’ scarce resources thinly across a wide group of practitioners, most of whom are at minimal risk of future complaints. Aiming interventions at high-risk doctors has the potential to steer outliers back towards safer practice, thereby reducing risks of future harm and patient dissatisfaction. Realising that potential requires two advances: better tools for flagging complaint-prone doctors early in their complaints trajectory; and effective interventions to address problems in a timely fashion.30 Future research should address both challenges.
2 Distribution among doctors in private practice in Victoria of complaints about them to the Victorian Health Services Commissioner, 2000–2009
Provenance: Not commissioned; externally peer reviewed.
Received 24 January 2011, accepted 18 May 2011
- Marie M Bismark1
- Matthew J Spittal2
- David M Studdert3
- School of Population Health, University of Melbourne, Melbourne, VIC.
This study was funded through an Australian Research Council Federation Fellowship (to David Studdert). We thank Beth Wilson, Health Services Commissioner of Victoria, and Grant Davies, Deputy Commissioner. Without their support and the assistance of their team in preparing the data, this study would not have been possible.
None identified.
- 1. Sloan FA, Mergenhagen PM, Burfield WB, et al. Medical malpractice experience of physicians: predictable or haphazard? JAMA 1989; 262: 3291-3297.
- 2. Taragin MI, Wilczek AP, Karns ME, et al. Physician demographics and the risk of medical malpractice. Am J Med 1992; 93: 537-542.
- 3. Bovbjerg RR, Petronis KR. The relationship between physicians’ malpractice claims history and later claims: does the past predict the future? JAMA 1994; 272: 1421-1426.
- 4. Abbott RL, Ou RJ, Bird M. Medical malpractice predictors and risk factors for ophthalmologists performing LASIK and photorefractive keratectomy surgery. Ophthalmology 2003; 110: 2137-2146.
- 5. Gibbons RD, Hedeker DR, Charles SC, Frisch P. A random-effects probit model for predicting medical malpractice claims. J Am Stat Assoc 1994; 89: 760-767.
- 6. Adamson TE, Baldwin DC, Sheehan TJ, Oppenberg AA. Characteristics of surgeons with high and low malpractice claims rates. West J Med 1997; 166: 37-44.
- 7. Rolph JE, Adams JL, McGuigan KA. Identifying malpractice-prone physicians. J Empir Leg Stud 2007; 4: 125-153.
- 8. Nash LM, Kelly PJ, Daly MG, et al. Australian doctors’ involvement in medicolegal matters: a cross-sectional self-report study. Med J Aust 2009; 191: 436-440. <MJA full text>
- 9. Hickson GB, Federspiel CF, Blackford J, et al. Patient complaints and malpractice risk in a regional healthcare center. South Med J 2007; 100: 791-796.
- 10. Hickson GB, Federspiel CF, Pichert JW, et al. Patient complaints and malpractice risk. JAMA 2002; 287: 2951-2957.
- 11. Cunningham W, Crump R, Tomlin A. The characteristics of doctors receiving medical complaints: a cross-sectional survey of doctors in New Zealand. N Z Med J 2003; 116: U625.
- 12. Pukk-Harenstam K, Ask J, Brommels M, et al. Analysis of 23,364 patient-generated, physician-reviewed malpractice claims from a non-tort, blame-free, national patient insurance system: lessons learned from Sweden. Postgrad Med J 2009; 85: 69-73.
- 13. Morrison J, Wickersham P. Physicians disciplined by a State Medical Board. JAMA 1998; 279: 1889-1893.
- 14. Clay SW, Conatser RR. Characteristics of physicians disciplined by the State Medical Board of Ohio. J Am Osteopath Assoc 2003; 103: 81-88.
- 15. Kohatsu ND, Gould D, Ross LK, Fox PJ. Characteristics associated with physician discipline: a case-control study. Arch Intern Med 2004; 164: 653-658.
- 16. Scotland A, Old P. NCAS Casework: the first eight years. London: National Clinical Assessment Service, 2009.
- 17. Bismark MM, Studdert DM. Realising the research power of complaints data. N Z Med J 2010; 123: 12-17.
- 18. Anderson K, Allan D, Finucane P. A 30-month study of patient complaints at a major Australian hospital. J Qual Clin Pract 2001; 21: 109-111.
- 19. Paterson R. The patients’ complaints system in New Zealand. Health Aff (Millwood) 2002; 21: 70-79.
- 20. Victorian Department of Human Services. The Victorian medical workforce 2000–2006. Melbourne: DHS, 2009.
- 21. Gawande AA, Thomas EJ, Zinner MJ, Brennan TA. The incidence and nature of surgical adverse events in Colorado and Utah in 1992. Surgery 1999; 126: 66-75.
- 22. Lester G, Wilson B, Griffin L, Mullen PE. Unusually persistent complainants. Br J Psychiatry 2004; 184: 352-356.
- 23. National Clinical Assessment Service. Concerns about professional practice and associations with age, gender, place of qualification and ethnicity – 2009/10 data. London: NCAS, 2010.
- 24. Bismark MM, Brennan TA, Paterson RJ, Studdert DM. Relationship between adverse events and quality of care complaints in New Zealand: a descriptive analysis of complainants and non-complainants. Qual Saf Healthcare 2006; 15: 17-22.
- 25. Chun-Ying WU, Huei-Jen LI, Rong-Chi C. Patient characteristics predict cccurrence and outcome of complaints against physicians: a study from a medical center in central Taiwan. J Formosan Med Assoc 2009; 108: 126-134.
- 26. Levinson W, Roter DL, Mullooly JP, et al. Physician-patient communication: the relationship with malpractice claims among primary care physicians and surgeons. JAMA 1997; 277: 553-559.
- 27. Hsieh SY. The use of patient complaints to drive quality improvement: an exploratory study in Taiwan. Health Serv Manage Res 2010; 23: 5-11.
- 28. Tamblyn R, Abrahamowicz M, Dauphinee D, et al. Physician scores on a national clinical skills examination as predictors of complaints to medical regulatory authorities. JAMA 2007; 298: 993-1001.
- 29. Bazrafkan LS, Shokrpour N, Tabeie SZ. A survey of patients’ complaints against physicians in a five year period in Fars province: implication for medical education. J Med Educ 2008; 12: 23-28.
- 30. Leape LL, Fromson JA. Problem doctors: Is there a system-level solution? Ann Intern Med 2006; 144: 107-115.





Abstract
Objective: To identify characteristics of doctors who are repeated subjects of complaints by patients.
Design and setting: Case–control study of doctors about whom patients had complained to the Victorian Health Services Commissioner between 1 January 2000 and 31 December 2009.
Participants: 384 doctors in private practice; cases comprised 96 doctors who were the subject of four or more separate complaints; and the control group comprised 288 doctors who were the subject of a single complaint over the study period.
Results: Among doctors in private practice in Victoria, 20.5% (95% CI, 19.7%–21.3%) experienced at least one complaint over the decade. Among doctors who were the subject of a complaint, 4.5% (95% CI, 3.6%–5.4%) had four or more complaints, and this group accounted for 17.6% (95% CI, 16.3%–19.0%) of all complaints to the Victorian Health Services Commissioner. Multivariate analyses showed that surgeons (odds ratio [OR], 8.90; 95% CI, 3.69–21.50) and psychiatrists (OR, 4.59; 95% CI, 1.46–14.43) had higher odds of being in the complaint-prone group than general practitioners. Doctors trained overseas had lower odds of being complaint-prone than those trained in Australia (OR, 0.31; 95% CI, 0.13–0.72).
Conclusions: A small group of doctors in private practice in Victoria account for nearly 18% of complaints. Interventions to improve patient satisfaction and public confidence in health services should target complaint-prone subgroups of practitioners.