This hiatus of learning incentives may be affecting junior doctors’ engagement in the learning opportunities provided. In 2007, an FEP evaluation conducted by the MEU of Townsville Hospital (a large regional hospital in Queensland) showed that FEP attendance was poor, even with an arbitrary setting of 80% minimum attendance. The mean attendance rate for the 32 interns was 66% (range, 51%–87%), and evaluation of attendance during previous years showed 2007 was not an atypical year (unpublished data) (Box 1). Feedback provided by interns in their 2007 end-of-term evaluations indicated that the biggest barrier to their attendance at the FEP activities was a heavy workload and a corresponding commitment to maintaining patient care. This made attendance difficult, despite these sessions occurring during “protected time” (unpublished data). This is consistent with previous research findings which have shown that junior doctors find it difficult to choose between patient care, work demands and their own professional development (PD).1
Formal ethics approval was obtained from the Townsville Human Research Ethics Committee to undertake and publish a low-risk study to address the issues identified. Design-based research methodologies6 were used, because the study focus was on the development, implementation and evaluation of a new structure for the FEP. Interns’ participation in learning activities was used to evaluate the effectiveness of this new structure.
To meet the design brief, the MEU at Townsville Hospital developed a new FEP for 2008 around a framework of four key PD domains — education sessions, skills workshops, presentations and research. The pre-existing FEP, which consisted of weekly face-to-face education sessions, had been developed by the MEU in 2007 to address components of the Australian Curriculum Framework for Junior Doctors.7 This was expanded to include skills workshops, formal presentations of professional knowledge (eg, at conferences, grand rounds or other teaching sessions) and research (eg, audits, quality assurance activities and peer-reviewed publications). In addition, an online learning portal with the potential to provide more flexible learning options was developed.
providing them with expanded learning opportunities;
allowing them to self-select relevant PD to meet their learning needs at a time that suited them;
creating an impressive resume that could potentially give them a competitive edge for college selections.
The interns’ yearly records of participation in learning activities were converted to CME points before being collated by the MEU. An anonymous attitudinal survey, comprising mainly open-ended questions, was developed by the MEU to evaluate the 2008 FEP at the end of the year. This survey provided feedback that was used to revise the FEP, the associated learning activities and allocation of CME points for 2009, and the process was repeated in 2009 for 2010 (Box 2). Evaluations of the FEP in 2009 and 2010 were carried out using a more detailed survey, consisting of 10 questions requiring a yes or no response and three open-ended questions.
During the trial period, there was an increase in the mean number of points accrued by interns, from 114 points (range 60–168, median 113) in 2008 to 132 points (range 85–298, median 127) in 2010 (Box 3). There was a corresponding decrease in the percentage of interns who failed to accrue the required minimum — 20% in 2008 and 8% in 2010. Each year, points were accrued across all PD domains and the majority were gained through participation in education sessions (Box 3). The development of a research club in 2010 had a positive effect on interns’ use of research as a PD activity.
The FEP evaluation surveys in 2009 and 2010 revealed mixed attitudes towards the CME points system (Box 4). The majority of interns liked the flexible learning options that the system provided, but about half felt pressured to accrue points. In addition, the majority of interns felt that the PD helped them gain better knowledge and skills, helped them to develop as a clinician and contributed to their development as a professional.
Accruing points for participating in learning is not a new concept. It is a well accepted method of providing motivation to participate in professional learning activities.8-12 In medicine, the concept of using CME points has, to date, been restricted to medical graduates who need to accrue points to maintain specialist accreditation.8,9 Yet doctors are students of medicine from the day they enrol in medical school and throughout their entire career.13 It seems reasonable, therefore, to extend the concept of CME into the prevocational period. Many other professions require junior professionals to accumulate evidence of professional activities in the form of points,10-12 and the results of this study suggest that junior medical professionals would respond positively to such a system.
A number of studies have shown that learning contracts are an essential tool for developing learner autonomy.14-16 The FEP that was developed in this trial is a type of learning contract. The final iteration of CME point allocations (Box 2) offered the interns flexible learning options by allowing them to choose learning activities that best suited their preferred learning styles and learning needs. Education sessions provide interns with an opportunity to advance their knowledge base. Clinical skills workshops provide simulated clinical experiences that can mimic situated learning, so that learning becomes clinically relevant. Quality assurance and other research activities require self-regulated learning, whereby interns make their own decisions about what they learn, how they learn and the depth to which they understand their new knowledge.5 The new FEP used in this trial therefore provides a learning environment that adheres to the principles of adult learning.2
2 Allocation of continuing medical education points for interns during 2009 and 2010
Advanced life support for interns and generic essential life support |
|||||||||||||||
4 Results of 2009 and 2010 evaluation surveys on the continuing medical education (CME) points system, completed by interns (yes responses)
Provenance: Not commissioned; externally peer reviewed.
- Allyson J Agnew1
- Carl J O’Kane2
- Postgraduate Medical Education Unit, Townsville Hospital, Townsville, QLD.
We thank the medical administration staff for their support and the interns for participating in the surveys. We also thank Vincent Ho, Maree Mayer, Roslyn Geaney, Jenine Lawlor and Debbie Paltridge for providing editorial assistance.
None identified.
- 1. Neate SL, Dent AW, Weiland TJ, et al. Barriers to continuing medical education in Australian prevocational doctors. Aust Health Rev 2008; 32: 292-300.
- 2. Knowles MS. The modern practice of adult education: from pedagogy to andragogy. Englewood Cliffs, NJ: Prentice Hall/Cambridge, 1980: 40-62.
- 3. Lave J, Wenger E. Situated learning. New York: Cambridge, 1991.
- 4. Knowles M. Self-directed learning: a guide for learners and teachers. New York: Association Press, 1975.
- 5. Zimmerman BJ. Theories of self-regulated learning and academic achievement: an overview and analysis. In: Zimmerman BJ, Schunk DH, editors. Self-regulated learning and academic achievement: theoretical perspectives. 2nd ed. London: Lawrence Erlbaum, 2001: 1-37.
- 6. Sandoval WA, Bell P. Design-based research methods for studying learning in context: introduction. Educ Psychol 2004; 39: 199-201.
- 7. Confederation of Postgraduate Medical Education Councils. Australian Curriculum Framework for Junior Doctors. 2008. http://curriculum.cpmec.org.au (accessed Mar 2009).
- 8. Australian Council on Healthcare Standards. Healthcare quality and safety workshop series: CPD point details. http://www.achs.org.au/CPDpoints (accessed Jun 2010).
- 9. Royal Australian College of General Practitioners. QA&CPD Program. http://www.racgp. org.au/membership/qacpd (accessed Jun 2010).
- 10. Australian Association of Social Workers. Continuing professional education. http://www. aasw.asn.au/whatwedo/continuing-professional-education (accessed Jun 2010).
- 11. Australian Physiotherapy Association. APA Continuing Professional Development scheme. http://www.physiotherapy.asn.au/index.php/prof-dev/about-cdp-scheme (accessed Jun 2010).
- 12. Exercise and Sports Science Australia. CE registration. http://www.essa.org.au/index. php?q=node/157 (accessed Jun 2010).
- 13. Miller SH. American Board of Medical Specialties and repositioning for excellence in lifelong learning: maintenance of certification. J Contin Educ Health Prof 2005; 25: 151-156.
- 14. Lane D. Using learning contracts – pitfalls and benefits for adult learners. Training Dev Aust 1988; 15 (1): 7-9.
- 15. Knowles MS. Using Learning Contracts. San Francisco, Calif: Jossey-Bass, 1986.
- 16. Tompkins C, McGraw MJ. The negotiated learning contract. In: Boud D, editor. Developing student autonomy in learning. London: Kogan Page, 1988: 172-191.





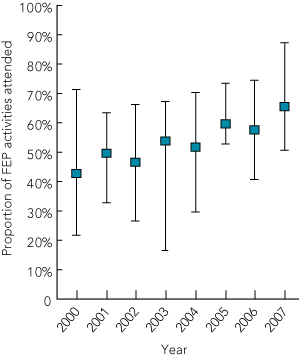
Abstract
Objectives: To describe the development and uptake of a new self-directed learning program for interns, and to evaluate interns’ attitudes towards the program.
Design, setting and participants: Using design-based research methodologies, a facility education program was developed to provide flexible learning options, complement the situated learning that occurs at the bedside and foster the development of self-directed and self-regulated learning behaviour. From 2008 to 2010, interns at a large regional Australian hospital (Townsville Hospital) were required to accrue a minimum 100 continuing medical education (CME) points.
Main outcome measures: Mean number of CME points accrued per intern and attitudes of interns towards the CME points system.
Results: A total of 30, 39 and 59 interns participated in the program during 2008, 2009 and 2010, respectively. The mean number of points accrued by interns increased from 114 points (range, 60–168; median, 113) in 2008 to 132 points (range, 85–298; median, 127) in 2010. There was a corresponding decrease in failure to accrue 100 points, from 20% of interns (6/30) in 2008 to 8% of interns (5/59) in 2010. Evaluations showed that the majority of interns (surveyed at the end of 2009 [n = 22] and 2010 [n = 46]) liked the flexible learning options of the CME points system, and also felt that the professional development helped them gain better knowledge and skills and develop as a clinician. However, about half of them felt pressured to accrue points.
Conclusions: A CME points system is acceptable to and used by interns. This system has the flexibility to be expanded to other junior doctor years and implemented in all Australian facilities to ensure that self-directed and self-regulated learning occurs across the entire prevocational continuum.