To the Editor: Trachoma control guidelines from the World Health Organization1 and Communicable Diseases Network Australia (CDNA)2 recommend the “SAFE” strategy that includes surgery for trichiasis, antibiotic treatment, facial cleanliness and environmental improvement. Lack of access to antibiotics in isolated areas should not be a major contributor to the persistence of trachoma in Australia because special Pharmaceutical Benefits Scheme arrangements (SPBSA) under section 100 of the National Health Act 1953 for the supply of medicines to remote-area Indigenous health services should enable a ready availability of azithromycin. The 1999–00 to 2001–02 evaluation of the SPBSA suggested that the program had led to major increases in the supply of medicines in remote areas, but that the supply of azithromycin did not change as a result of the introduction of the program.3
We assessed the relationship between reported azithromycin treatment of people with trachoma, their household contacts, and community members; levels of treatment recommended by WHO and CDNA guidelines; and the total number of courses of azithromycin available through the SPBSA. The National Trachoma Surveillance and Reporting Unit (NTSRU) provided 2008 data on treatment with azithromycin and trachoma prevalence in the Northern Territory, South Australia and Western Australia (refer to the report for limitations of the data).4 Data for 2007–08 on the supply of azithromycin to health services under SPBSA were obtained from Medicare Australia.
The WHO guidelines recommend treatment of an entire community if the prevalence of active trachoma among children is above 10%.1,5 The CDNA guidelines2 recommend that contacts (> 6 months of age) of infected children within a household be treated. Our estimate of trachoma treatment according to CDNA guidelines is based on multiplying the number of infected children (from the NTSRU data) by the average number of members in remote Indigenous households.5 The impact of shared and multiple residence on estimates of household contacts could not be taken into account.
The Box shows the numbers of azithromycin courses available through the SPBSA to remote-area Aboriginal and Torres Strait Islander health services in the three states. In the NT, the reported number of courses given (3069) fell well below the level recommended by both WHO (by 34%) and CDNA (by 41%) guidelines. In SA, reported courses of azithromycin given (7) fell well below the 45 suggested by the CDNA guidelines. The prevalence of trachoma did not exceed 10% in any SA community, so no treatment was required under WHO guidelines. In WA, the reported number of courses given (2917) also fell below recommended levels, although the deficit (WHO, 35%; CDNA, 81%) varied substantially depending on which guidelines were used.
Reported treatment with azithromycin was below levels recommended by the CDNA and the WHO despite health services having sufficient courses available to them to mostly meet these targets. All aspects of the SAFE strategy are important in the eradication of trachoma. However, improving the supply and distribution of azithromycin should be relatively easy to implement, fund and monitor.
Azithromycin courses* available, 2007–08;† courses given, 2008;‡ and WHO- and CDNA-recommended courses,§ in three Australian states with remote-area Indigenous health services
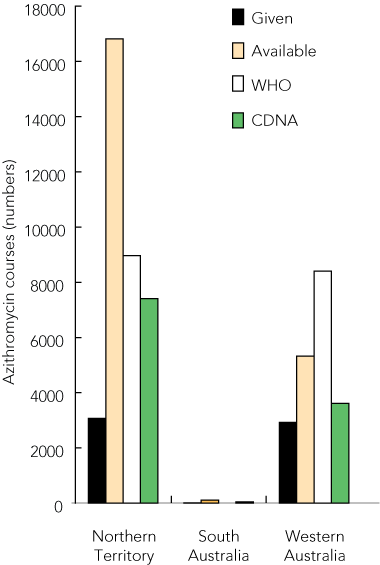 WHO = World Health Organization. CDNA = Communicable Diseases Network Australia. * Azithromycin courses are given to those with active trachoma, their household contacts, and community members. † Under special Pharmaceutical Benefits Scheme arrangements and reported by Medicare Australia. ‡ Reported by the National Trachoma Surveillance and Reporting Unit (NTSRU). § Based on NTSRU data and using community population estimates. |
- 1. Trachoma control: a guide for programme managers. Geneva: World Health Organization, London School of Hygiene and Tropical Medicine, International Trachoma Initiative, 2006.
- 2. Australian Government Department of Health and Ageing. Guidelines for the public health management of trachoma in Australia. Canberra: Communicable Diseases Network Australia, 2006.
- 3. Kelaher M, Dunt D, Taylor-Thomson D, et al. Improving access to medicines among clients of remote area Aboriginal and Torres Strait Islander Health Services. Aust N Z J Public Health 2006; 30: 177-183.
- 4. Tellis B, Fotis K, Dunn R, et al. National Trachoma Surveillance and Reporting Unit. Trachoma surveillance report 2008. Melbourne: Centre for Eye Research Australia, University of Melbourne, 2009.
- 5. Australian Bureau of Statistics. Household and family composition. 2010. http://www.ausstats.abs.gov.au/Ausstats/subscriber.nsf/0/526FE126443EBCC6CA257718001D547F/$File/47130_2006_reissue.pdf (accessed Dec 2010.)





This research was funded by the Ian Potter Foundation and the Harold Mitchell Foundation. Margaret Kelaher holds an Australian Research Council Future Fellowship.