The reduction of psychiatric beds in health services has been a matter of much debate since the era of deinstitutionalisation.1-3 Before the National Mental Health Plan of 1992,4 deinstitutionalisation in Australia saw a reduction of beds from 30 000 to 8000 over 30 years.5 This shift of focus from hospital to community-based care was in line with policy direction throughout the Western world.1 The National Mental Health Plan led to mainstreaming of psychiatric services from stand-alone psychiatric institutions to general hospitals and community-based care.5 Between 1993 and 2002, the number of long-stay beds was reduced by 52% and the overall number of acute beds increased by 6%.6 Although the number of psychiatric beds varies internationally, Australia is at the lower end of bed numbers per 100 000 population.7,8
The demand for psychiatric services in Australia has increased. For example, between financial years 1998–99 and 2002–03, overnight admissions to acute psychiatric units increased by 7%.9 One response to this has been to encourage inpatient units to increase efficiency by reducing patients’ length of stay (LOS). While the reduction in LOS raises concerns about increased readmission rates, there is little evidence to associate reduced LOS with poorer health outcomes in hospitalised patients.10
In May 2008, a Team Strategies and Tools to Enhance Performance and Patient Safety (TeamSTEPPS) program was implemented at Cramond Clinic, sponsored by the South Australian Department of Health’s Safety and Quality Unit.11 Following training of a group of key clinicians, roll-out commenced in July 2008, with this group training all Cramond Clinic staff in TeamSTEPPS principles. These included introducing a structured communication tool at all handovers, restructuring multidisciplinary meetings and clearly defining the roles and responsibilities of all clinical staff.
The comparison measures for different time frames are listed in Box 1. Throughout each study period, 10% of the bed days were occupied by patients with LOS > 35 days. The average LOS for patients with LOS > 35 days did not change significantly between the periods.
During the observation period (after bed reduction), there was a 22.5% reduction in bed capacity at the clinic (Box 1). Activity levels, measured by number of discharges per day, dropped by 27.3% (P < 0.001) in the observation period compared with baseline, but there was no significant change in average LOS (P = 0.802). The number of ED presentations with psychiatric diagnoses fell by 13.4% (P < 0.001). For patients requiring admission, there was no significant change in time spent in the ED before being admitted (P = 0.185). Bed occupancy rates were similar in both periods (P = 0.30). The 7-day follow-up rate increased by 9 percentage points (P = 0.008). There was no significant change in readmission rates (P = 0.12). The number of seclusions declined by 47.8% (P = 0.007) (Box 1).
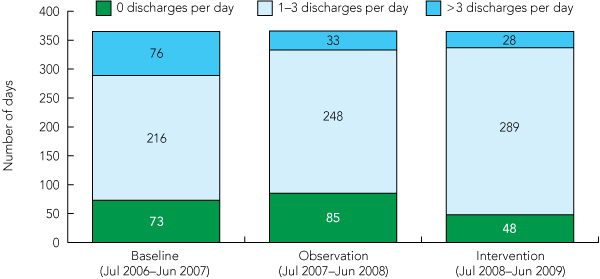
During the intervention period (the second year after bed reduction), activity levels (discharges per day) increased by 12.5% (P = 0.021) compared with those of the observation period (Box 1). There was no significant change in the number of mental health ED presentations (P = 0.427). The waiting time for admissions from the ED to the ward decreased by 14.8% (P = 0.086), influencing occupancy rates, which fell by 2.5% (P = 0.01). Average LOS further decreased by 20.2% (P < 0.001). The number of days without any discharges roughly halved from 85 in the observation period to 48 in the intervention period (Box 2). The 7-day follow-up rate improved a further 11 percentage points (P < 0.001). There was no significant change in readmission rates (P = 0.33). The number of seclusions dropped by 76.3% (P = 0.002) (Box 1).
LOS and waiting times in the ED decreased during the intervention period. There was a more even flow of discharges, shifting towards one to three discharges per day, during the observation period compared with the baseline period, but there was no reduction in the number of days without discharges (Box 2).
Our study demonstrated that reducing beds and introducing new care pathway interventions in inpatient and community settings are associated with better ward practices and improvements in patient flow between the ED, the inpatient ward and community teams. Most notably, we observed a marked reduction in seclusion rates. The literature on seclusion rates in psychiatric settings suggests that a multimodal team-based approach is necessary to reduce rates of seclusion.12 Certainly, in our study, the reduction was associated with improved staff training in handling aggression, improved team communication, better data feedback on seclusion rates, and strengthened clinical leadership. The introduction of a TeamSTEPPS program, with its emphasis and training in the four competency areas of leadership, situation monitoring, mutual support and communication, may have led to improved teamwork and clinical outcomes in the unit. The effect of formal teamwork training has been previously documented in health care settings and has been shown to improve team behaviours and staff attitudes and to reduce errors.11 While a reduction in rehospitalisation rates would have been ideal, there was at least no evidence of an increase in 28-day rehospitalisation rates during the period of our study. We developed a protocol for discharge planning that encompassed structured communication processes. Discharge-planning interventions are also effective in reducing rehospitalisation rates and LOS.13 A formal transfer clinic, in which patients were seen by the treating inpatient team within 1 week of discharge, was facilitated by the appointment of a transfer-of-care coordinator.
The reduced rate of presentation to the ED over the study period may indicate that community services to psychiatric patients improved. Awareness of the bed reduction may have led community services to raise the severity-of-illness threshold for referral to the ED. This is in line with the finding that demand is to some extent generated by ready availability of psychiatric beds.14 Reducing demand is beneficial from a health economics point of view, but may also indicate that care is being more appropriately provided in the community. There have been concerns that reducing psychiatric beds without providing appropriate community services may contribute to increased homelessness. However, retrospective review that we conducted of the number of referrals to the Homeless Support Service in metropolitan Adelaide did not substantiate these concerns. Referrals to this service decreased from 103 to 59 during the study period, and hospital-at-home activity rose from 25 to 66 patient episodes.
Mathematical modelling of contributions to access block in inpatient units suggests that variable discharge patterns are more influential than variable admission rates.15 Therefore, the policy aimed at consistent rather than fluctuating discharge rates may have been a significant contributor to the efficiencies noted in our study. After bed reduction, the ward’s capacity to care for local patients increased, but the change only became apparent after a year. It could be argued that localised treatment is better for patients, as it provides better coordination of care, reduced referral pathways and improved access to local resources. It may therefore be important to set incentives that promote localisation, such as allowing units to run wards at 85% occupancy rates.16 Evidence indicates that allowing vacant beds prevents future crises and bed access block.17,18
Received 26 November 2009, accepted 10 May 2010
- Tarun J Bastiampillai1
- Niranjan P Bidargaddi2
- Rohan S Dhillon3
- Geoffrey D Schrader4
- Jörg E Strobel3
- Philip J Galley2
- 1 Southern Adelaide Health Service, Adelaide, SA.
- 2 Mental Health, Country Health SA, Adelaide, SA.
- 3 Queen Elizabeth Hospital and Health Services, Central Northern Adelaide Health Service, Adelaide, SA.
- 4 Discipline of Psychiatry, University of Adelaide, Adelaide, SA.
None identified.
- 1. Fakhoury W, Priebe S. The process of deinstitutionalization: an international overview. Curr Opin Psychiatry 2002; 15: 187-192.
- 2. Lamb HR, Bachrach LL. Some perspectives on deinstitutionalization. Psychiatr Serv 2001; 52: 1039-1045.
- 3. Kalucy R, Thomas L, King D. Changing demand for mental health services in the emergency department of a public hospital. Aust N Z J Psychiatry 2005; 39: 74-80.
- 4. National Mental Health Plan. Canberra: Commonwealth and state/territory health ministers, 1992. http://www6.health.gov.au/internet/main/publishing.nsf/Content/8E185E7F3B5 74CCFCA2572220005FF0D/$File/plan92.pdf (accessed Aug 2010).
- 5. Whiteford HA, Buckingham WJ. Ten years of mental health service reform in Australia: are we getting it right? Med J Aust 2005; 182: 396-400. <MJA full text>
- 6. Arean PA, Gum AM, Tang L, Unutzer J. Service use and outcomes among elderly persons with low incomes being treated for depression. Psychiatr Serv 2007; 58: 1057-1064.
- 7. Priebe S, Frottier P, Gaddini A, et al. Mental health care institutions in nine European countries, 2002 to 2006. Psychiatr Serv 2008; 59: 570-573.
- 8. Rosenman S. Acute psychiatric beds: distribution and staffing in NSW and ACT. Aust N Z J Psychiatry 1995; 29: 238-247.
- 9. Australian Institute of Health and Welfare. Mental health services in Australia 2002–03. Canberra: AIHW, 2004. (AIHW Cat. No. HSE 35; Mental Health Series No. 6.)
- 10. Clarke A, Rosen R. Length of stay. How short should hospital care be? Eur J Public Health 2001; 11: 166-170.
- 11. Stead K, Kumar S, Schultz TJ, et al. Teams communicating through STEPPS. Med J Aust 2009; 190 (11 Suppl): S128-S132. <MJA full text>
- 12. Bowers L, Allan T, Simpson A, et al. Identifying key factors associated with aggression on acute inpatient psychiatric wards. Issues Ment Health Nurs 2009; 30: 260-271.
- 13. Steffen S, Kösters M, Becker T, Puschner B. Discharge planning in mental health care: a systematic review of the recent literature. Acta Psychiatr Scand 2009; 120: 1-9.
- 14. Lee R, Bradley D. Mental health. Wrong side of beds. Health Serv J 2000; 110: 30-31.
- 15. Harrison GW, Shafer A, Mackay M. Modelling variability in hospital bed occupancy. Health Care Manag Sci 2005; 8: 325-334.
- 16. Bagust A, Place M, Posnett JW. Dynamics of bed use in accommodating emergency admissions: stochastic simulation model. BMJ 1999; 319: 155-158.
- 17. Dunn R. Reduced access block causes shorter emergency department waiting times: an historical control observational study. Emerg Med (Fremantle) 2003; 15: 232-238.
- 18. Thornton V, Hazell W. Junior doctor strike model of care: reduced access block and predominant Fellow of the Australasian College for Emergency Medicine staffing improve emergency department performance. Emerg Med Australas 2008; 20: 425-430.





Abstract
Objective: To evaluate the impact of psychiatric inpatient bed closures, accompanied by a training program aimed at enhancing team effectiveness and incorporating data-driven practices, in a mental health service.
Design and setting: Retrospective comparison of the changes in services within three consecutive financial years: baseline period — before bed reduction (2006–07); observation period — after bed reduction (2007–08); and intervention period — second year after bed reduction (2008–09). The study was conducted at Cramond Clinic, Queen Elizabeth Hospital, Adelaide.
Main outcome measures: Length of stay, 28-day readmission rates, discharges, bed occupancy rates, emergency department (ED) presentations, ED waiting time, seclusions, locality of treatment, and follow-up in the community within 7 days.
Results: Reduced bed numbers were associated with reduced length of stay, fewer referrals from the community and subsequently shorter waiting times in the ED, without significant change in readmission rates. A higher proportion of patients was treated in the local catchment area, with improved community follow-up and a significant reduction in inpatient seclusions.
Conclusion: Our findings should reassure clinicians concerned about psychiatric bed numbers that service redesign with planned bed reductions will not necessarily affect clinical care, provided data literacy and team training programs are in place to ensure smooth transition of patients across ED, inpatient and community services.