Teamwork and communication failures are frequent contributors to adverse events in health care.1,2 Individual execution of clinical tasks is the focus of clinician training, and traditionally little has been done to prepare for the more tightly defined teamwork behaviour typical of other industries.3,4 Similarities between health care and other complex industries such as aviation have been noted, including the need for effective decision making, in spite of incomplete or conflicting information, and the demand for coordination among professionals with varied skills and ranks.5-7
A large body of research has identified a set of core knowledge, skills and attitudes that, according to Salas and colleagues, apply to almost all teams.8,9 The critical aspects of teamwork include team leadership, mutual performance monitoring (situation monitoring), back-up behaviour (mutual support) and communication. A retrospective review of closed indemnity claims in the United States indicated that failure to engage in one or more of these teamwork behaviours always contributed to an adverse event and indemnity payments, with an average of 8.8 teamwork failures per closed case. In 43% of the cases reviewed, application of teamwork behaviours would have prevented or mitigated the adverse event.10 Formal teamwork training improves team performance and outcomes.11,12 In the health care domain, teamwork training has been shown to improve team behaviours and staff attitudes and reduce errors.4 Emergency departments adopting formal teamwork training have experienced a 67% increase in error-averting behaviour and a 58% reduction in observable errors.4,13
TeamSTEPPS (Team Strategies and Tools to Enhance Performance and Patient Safety) is an evidence-based teamwork training system involving four competency areas: leadership, situation monitoring, mutual support, and communication.14 The program, developed by the US Agency for Healthcare Research and Quality and the US Department of Defense, uses principles of aviation crew resource management adapted for the health care sector.15
The TeamSTEPPS program has not previously been formally evaluated in Australia, nor has it been introduced into a mental health care environment. We report here on a case study of the implementation of TeamSTEPPS at an inpatient mental health facility in South Australia. We sought to determine whether the training intervention changed staff attitudes and behaviours and had an impact on patient care. Our aim was to evaluate the effectiveness of the intervention with measures developed to address three outcome constructs: observed team behaviours; attitudes and opinions; and clinical performance and outcomes.5
The implementation of a TeamSTEPPS program in a mental health facility was part of a larger study involving five hospital sites. Nominations received from SA health care sites in November 2007 to participate in the 8-month TeamSTEPPS project were reviewed by a steering committee. Sites were chosen based on a number of criteria, including availability, willingness to commit to the project, clinical and geographical diversity, amenability to cultural change, and availability of key multidisciplinary clinical staff committed to driving the change locally and an executive sponsor willing to dedicate time and personnel to the project. After a successful nomination, each site entered into a site assessment, the first phase of implementation.14
A total of five sites, including the mental health site, then proceeded to training, the second phase. Multidisciplinary staff were selected by the site to receive intensive education in a 2.5-day workshop under a train-the-trainer model, whereby a small group of senior clinical staff would be trained and then pass on their knowledge and skills to other staff. The workshop consisted of education on the evidence base, tools and strategies to support the desired skills and attitudes towards teamwork and communication; coaching; and development of site-specific action plans. Within 1 week after completion of the workshop, the health service trainers from participating sites (health service trainers) commenced delivery on site to their colleagues of a condensed 4-hour course to educate all staff in teamwork competencies, tools and strategies for putting the desired behaviours into practice. The delivery model was based on local factors — for example, staff availability, space and resources. Participants evaluated both forms of training (the 2.5-day workshop and the 4-hour course) using a 12-item questionnaire. After training, the staff who attended the 2.5-day workshop formed a change team to guide the implementation of the program.
Ethics approval for the evaluation was given by the human research ethics committees of the University of South Australia and the Royal Adelaide Hospital.
The 42-item Hospital Survey on Patient Safety Culture16 was administered to assess staff opinions on patient safety, and error and incident reporting. Respondents rated each item on a five-point Likert scale, from 1 (“strongly disagree”) to 5 (“strongly agree”). The proportion of positive responses (agree/strongly agree) were mapped to 12 unit-specific and hospital-wide domains, including those specific to teamwork and communication.
A second questionnaire was developed and administered to measure staff knowledge, skills and attitudes in relation to teamwork and communication. The 23-item knowledge, skills and attitudes questionnaire was based on an existing Total Team Assessment questionnaire,17 the learning objectives of the TeamSTEPPS training, and a literature review.18 Each item was scored on a five-point Likert scale. Using a scoring system for each question of 1 (strongly disagree) to 5 (strongly agree), the total score ranged from a minimum of 23 to a maximum of 115.
The results reported here relate to the mental health facility site.
A structured communication tool known as SBAR (situation, background, assessment, request/recommendation)14 was introduced to support changes to clinical handover. After 1 month, multidisciplinary use of SBAR was demonstrated in virtually all patient presentations at handover. The SBAR framework was also used in written communication in patient clinical notes.
Most respondents to the patient safety culture survey were nursing and medical staff (56% registered nurses, 5% enrolled nurses, 11% residents and 4% consultants). Before implementation of the TeamSTEPPS program, the patient safety culture for nearly all domains tended to be lower at the mental health site than at all sites included in the study (Box 1). This was particularly true for domains 2 (feedback and communication about error), 3 (frequency of event reporting), 7 (organisational learning) and 12 (teamwork within hospital units). After implementation, two of these domains (3 and 7) showed significant improvement at the mental health site (Z test comparison of proportions, P < 0.05), and patient safety culture for only two of the domains was lower for the mental health site than for all sites combined (Box 1).
There was an increase in total knowledge, skills and attitudes score for the mental health site of 6.8% following TeamSTEPPS implementation (Box 2). Although the increase was not statistically significant, the implementation at the mental health site suggested a greater effect size than was apparent for all sites combined (1.9%). Scores for three individual items in the mental health site data increased by more than 15% after implementation: “My manager focuses on building the skills that I need to perform my role”; “My manager coaches and supports me”; and “Staff work together to monitor and progress patient care plans”.
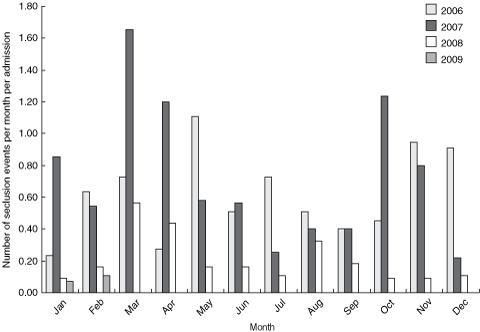
Before the introduction of TeamSTEPPS, the initiation of seclusion in patients was determined by individual clinicians, and seclusion rates were variable (Box 3). The introduction of “huddles” (ad hoc gatherings of clinical staff to re-establish a clear and accurate understanding of the patient’s current status and plan of care)14 and a structured team approach has established a team commitment to resolve aggression, with seclusion used as a last resort. Seclusion rates before implementation (ie, before February 2008) were significantly higher than after implementation (from May 2008) (Mann–Whitney U test, Z = –4.1; P < 0.001).
The advantage of observation as a research tool is that health care practitioners’ activities and behaviour can be captured in their own environment without having to rely on their willingness or ability to respond to questions.19,20 The observational evaluation identified several key factors that contributed to the implementation of TeamSTEPPS at the mental health site. Firstly, the change team that was formed to support TeamSTEPPS implementation recognised the need for change. This also cultivated a “bottom-up” approach, which ensured that ownership of change was taken up and driven by the local change team. The recognition of barriers enabled the change team to address them early in the implementation. The implementation was supported by strong leadership, both locally, by the medical staff, and throughout the hierarchy, ensuring transparency and confidence in the change-management process. The local actions to review, display and strive for improved results in their measurement-driven improvement cycle (as demonstrated through the display of seclusion data) also assisted in staff engagement. Coaching of staff in the desired teamwork behaviour was also a feature. These are the principles that contribute to a successful implementation of TeamSTEPPS.21
Reducing the rate of seclusion is a national priority area in mental health.22 The reduction in seclusion rates associated with the implementation of team activities (huddles) in our study is a significant finding.
Considering the complexity of behavioural change, the implementation was assessed in a relatively brief post-training intervention period of up to 5 months, with the change in culture demonstrated through the results of the patient safety culture survey — notably by the frequency of event reporting and the extent to which errors led to positive changes and organisational learning. Moreover, the changes to patient safety culture and knowledge, skills and attitudes to teamwork and communication tended to exceed those shown by overall data from all sites.
There were no significant negative findings, and while positive changes are evident, it is premature to assess whether they will result in lasting cultural change. However, given the change in behaviour from baseline, a multifaceted intervention, a clear description of the problem to solve, and an action plan with ongoing measurement, there is increased probability that the changes gained at the site will be sustained.23
1 Proportion of positive responses for 12 domains of patient safety culture before and after implementation of the TeamSTEPPS program: mental health (MH) site versus all sites combined
Proportion of positive responses |
|||||||||||||||
Before–after comparison (MH site) |
|||||||||||||||
10 Supervisor/manager expectations and actions promoting safety |
|||||||||||||||
- Karen Stead1
- Saravana Kumar2
- Timothy J Schultz3
- Sue Tiver4
- Christy J Pirone1
- Robert J Adams5
- Conrad A Wareham6
- 1 South Australian Department of Health, Adelaide, SA.
- 2 Centre for Allied Health Evidence, University of South Australia, Adelaide, SA.
- 3 Australian Patient Safety Foundation, Adelaide, SA.
- 4 Cramond Clinic, Queen Elizabeth Hospital, Adelaide, SA.
- 5 Health Observatory, University of Adelaide and Queen Elizabeth Hospital, Adelaide, SA.
- 6 Intensive Care Unit, Lyell McEwin Hospital, Adelaide, SA.
We acknowledge the contribution of the following organisations and committees: Australian Commission on Safety and Quality in Healthcare, SA Department of Health, SA Council for Safety and Quality in Health Care, SA Safety and Quality in Health Care Consumer and Community Advisory Committee, Australian Patient Safety Foundation, University of South Australia, Women’s and Children’s Hospital, Queen Elizabeth Hospital, Port Augusta Hospital, and Repatriation General Hospital. We acknowledge the generosity of the US Department of Defense and the Agency for Healthcare Research and Quality in permitting the use of their TeamSTEPPS materials and in their guidance during program implementation. We also thank Ms Mary Salisbury for her support.
None identified.
- 1. Wong MC, Yee KC, Turner P. A structured evidence-based literature review regarding the effectiveness of improvement interventions in clinical handover. eHealth Services Research Group, University of Tasmania, 2008. http://www.safetyandquality.gov.au/internet/safety/publishing.nsf/Content/PriorityProgram-05 (accessed Sep 2008).
- 2. Australian Council for Safety and Quality in Health Care. Clinical handover and patient safety: literature review report. Canberra: ACSQHC, 2005. http://www.safetyandquality.gov.au/internet/safety/publishing.nsf/Content/F3D3F3274D393DFCCA257483000D8461/$File/clinhovrlitrev.pdf (accessed Sep 2008).
- 3. Mann S, Marcus R, Sachs B. Lessons from the cockpit: how team training can reduce errors on L&D. Contemp Ob Gyn 2006; 51: 34-45.
- 4. Morey J, Simon R, Jay G, et al. Error reduction and performance improvement in the emergency department through formal teamwork training: evaluation of results of the MedTeams project. Health Serv Res 2002; 37: 1553-1581.
- 5. Morey JC, Simon R, Jay GD, Rice MM. A transition from aviation crew resource management to hospital emergency departments: the MedTeams story. In: Jensen R, editor. Proceedings of the 12th International Symposium on Aviation Psychology. 2003 Apr 14–17; Dayton, Ohio, USA. Dayton, Ohio: Wright State University Press, 2003: 826-832.
- 6. Simon R, Langford V, Locke A, et al. A successful transfer of lessons learned in aviation psychology and flight safety to health care: the MedTeams system. Proceedings of Patient Safety Initiative 2000: spotlighting strategies, sharing solutions; 2000 Oct 4–6; Chicago, USA. Chicago: National Patient Safety Foundation, 2000: 45-49.
- 7. Simon R, Morey JC, Rice MM, et al. Reducing errors in emergency medicine through team performance: the MedTeams project. In: Scheffler AL, Zipperer L, editors. Enhancing patient safety and reducing errors in health care. Chicago: National Patient Safety Foundation, 1998: 142-146.
- 8. Salas E, Sims DE, Burke CS. Is there “big five” in teamwork? Small Group Res 2005; 36: 555-599.
- 9. Salas E, Burke CS, Stagl KC. Developing teams and team leaders: strategies and principles. In: Day DV, Zaccaro SJ, Halpin SM, editors. Leader development for transforming organizations: growing leaders for tomorrow. Mahwah, NJ: Lawrence Erlbaum Associates, 2004: 325-355.
- 10. Risser DT, Rice MM, Salisbury ML, et al. The potential for improved teamwork to reduce medical errors in the emergency department. The MedTeams Research Consortium. Ann Emerg Med 1999; 34: 373-383.
- 11. Salas E, Nichols DR, Driskell JE. Testing three team training strategies in intact teams: a meta-analysis. Small Group Res 2007; 38: 471-488.
- 12. Salas E, Diaz Granados D, Weaver SJ, King H. Does team training work? Principles for health care. Acad Emerg Med 2008; 15: 1002-1009.
- 13. Leedom D, Simon R. Improving team coordination: a case for behavior-based training. Mil Psychol 1995; 7: 109-122.
- 14. Agency for Healthcare Research and Quality. TeamSTEPPS instructor guide. Rockville, Md: AHRQ, 2006. (AHRQ Publication No. 06-0020-0.)
- 15. Alonso A, Baker DP, Holtzman A, et al. Reducing medical error in the military health system: how can team training help? Hum Resour Manage Rev 2006; 16: 396-415.
- 16. Sorra JS, Nieva VF. Hospital survey on patient safety culture. Rockville, Md: Agency for Healthcare Research and Quality, 2004. (AHRQ Publication No. 04-0041.)
- 17. QV Research. Total team assessment. http://www.qvresearch.com/organizational_assessments/total_team_assessment.htm (accessed Apr 2009).
- 18. Singla A, Kitch BT, Weissman JS, Campbell EG. Assessing patient safety culture: a review and synthesis. J Patient Saf 2006; 2: 105-116.
- 19. Taylor-Powell E, Steele S. Collecting evaluation data: direct observation. University of Wisconsin, 1996. http://learningstore.uwex.edu/pdf/G3658-5.PDF (accessed Apr 2009).
- 20. Leonard KL, Masatu MC. The use of direct clinical observation and vignettes for health service quality evaluation in developing countries. Soc Sci Med 2005; 61: 1944-1951.
- 21. Clancy C, Tornberg D. TeamSTEPPS: assuring optimal teamwork in clinical settings. Am J Med Qual 2007; 22: 214-217.
- 22. Australian Government National Mental Health Seclusion and Restraint Project. NMHSRP background. http://www.nmhsrp.gov.au/c/mh?a=da&did=1006037&pid=1197368795 (accessed Mar 2009).
- 23. Cockburn J. Adoption of evidence into practice: can change be sustainable? Med J Aust 2004; 180 (6 Suppl): S66-S67. <MJA full text>





Abstract
Objective: To evaluate the effectiveness of the implementation of a TeamSTEPPS (Team Strategies and Tools to Enhance Performance and Patient Safety) program at an Australian mental health facility.
Design, setting and participants: TeamSTEPPS is an evidence-based teamwork training system developed in the United States. Five health care sites in South Australia implemented TeamSTEPPS using a train-the-trainer model over an 8-month intervention period commencing January 2008 and concluding September 2008. A team of senior clinical staff was formed at each site to drive the improvement process. Independent researchers used direct observation and questionnaire surveys to evaluate the effectiveness of the implementation in three outcome areas: observed team behaviours; staff attitudes and opinions; and clinical performance and outcome. The results reported here focus on one site, an inpatient mental health facility.
Main outcome measures: Team knowledge, skills and attitudes; patient safety culture; incident reporting rates; seclusion rates; observation for the frequency of use of TeamSTEPPS tools.
Results: Outcomes included restructuring of multidisciplinary meetings and the introduction of structured communication tools. The evaluation of patient safety culture and of staff knowledge, skills and attitudes (KSA) to teamwork and communication indicated a significant improvement in two dimensions of patient safety culture (frequency of event reporting, and organisational learning) and a 6.8% increase in the total KSA score. Clinical outcomes included reduced rates of seclusion.
Conclusion: TeamSTEPPS implementation had a substantial impact on patient safety culture, teamwork and communication at an Australian mental health facility. It encouraged a culture of learning from patient safety incidents and making continuous improvements.