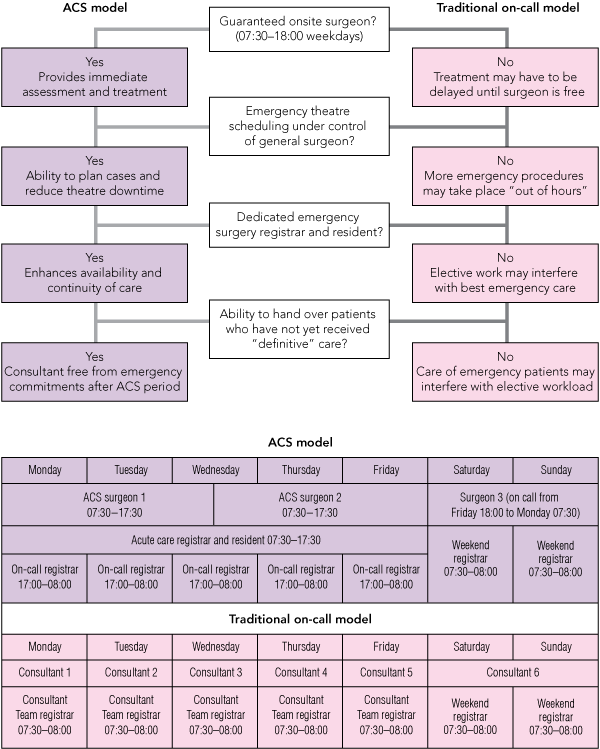
An acute care surgery (ACS) service1 was introduced at Prince of Wales Public Hospital (POWH), Sydney, in September 2005 (Box 1). The primary aim of introducing an ACS was to provide a consultant-led service to improve the efficiency and the predictability of the emergency surgery service. This was achieved by separating the elective and emergency workloads and placing control of the emergency theatre under the acute care general surgeon. Control of the emergency operating theatre allowed for planning of the semi-urgent caseload. The duty acute care surgeon remained on site during the working day, with no other commitments other than the ACS service. Patients whose surgical care had not been completed by the end of the duty period were handed on to the next acute care duty surgeon for definitive care. The introduction of the ACS service at our institution coincided with the formalised referral of surgical patients from a second emergency department within the area network. There were no changes in the clinical guidelines for patient care.
Of 402 patients who underwent appendicectomy for suspected acute appendicitis during the study period, 176 had the operation during the Trad period and 226 during the ACS period. There were no statistically significant differences in the demographics or insurance status of the two groups (Box 2), and there were no deaths in either group. Patients in the ACS group were more likely to have a documented preoperative review by a consultant surgeon and to undergo ultrasound and computed tomography. There was no significant difference between groups in the histological perforation rate or negative appendicectomy rate, but there was weak evidence that the ACS model reduced the latter.
A significantly higher proportion of operations took place during the day in the ACS period (47.8% v 34.1%; P = 0.006), and a significantly lower proportion of operations were performed at night in the ACS period (15.0% v 26.1%; P = 0.006). The proportion of operations performed in the evening did not differ significantly between the Trad and ACS groups (Box 3).
The overall complication rate was significantly lower in the ACS period than the Trad period (9.3% v 17.0%; P = 0.02) (Box 4), and the complication rate during daytime hours (08:00–17:00) was also significantly lower in the ACS group than the Trad group (9.3% v 21.7%; P = 0.02) (Box 3). The complication rate for non-perforated appendicitis was significantly lower in the ACS group (4.6% v 12.5%; P = 0.009).
The negative appendicectomy rate was significantly lower in the ACS group than the Trad group at night (P < 0.05) but not at other times (Box 3). There was no overall change in the appendiceal perforation rate. There was also no significant difference between groups in the perforation rates when analysed according to time of day (P [day] = 0.10; P [evening] = 0.33; P [night] = 0.31).
Our study specifically investigated the treatment of patients with appendicitis, rather than those with right iliac fossa pain. However, the presence of an on-site acute care surgeon can have a major impact in all areas. A previous study conducted at POWH showed that 40% of all general surgical presentations are saved from admission by the presence of an on-site acute care surgeon.1
We did not observe any significant improvement in patient flow in terms of time to theatre or length of stay. A previous study of patients undergoing appendicectomy showed that the introduction of acute care surgery was associated with a reduced time to theatre and reduced length of stay.2 However, this was achieved against a background of an increased proportion of appendicectomies being carried out after midnight. Control of the emergency operating theatre gave the acute care surgeon the ability to intentionally delay non-urgent appendicectomy during the night until the following day. With this conservative approach, there was no increase in perforation rate, the complication rate was reduced and there was no increase in length of stay.
The increasing use of preoperative imaging and laparoscopic techniques are two confounders. The greater use of preoperative imaging during the ACS period compared with the Trad period could potentially have reduced the negative appendicectomy rate, but our results did not show this. Meta-analyses have also failed to consistently show a decrease in the overall rate of complications when comparing conventional with laparoscopic appendicectomy.3-7 Laparoscopic appendicectomy has been shown to reduce the rate of wound infection, but is associated with a higher incidence of intra-abdominal collection. Reduced postoperative pain scores in patients undergoing laparoscopic appendicectomy may also reduce the incidence of cardiorespiratory complications, but this was not demonstrated in our study.4-7
An increase in the number of patients treated conservatively overnight did not lead to an overall increase in perforation rate. Other surgical studies and the findings of the National Confidential Enquiry into Peri-Operative Deaths in the United Kingdom suggest that it is safe to delay surgery for non-perforated appendicitis and that surgery after midnight may be associated with increased morbidity and mortality.8-12 Prospective studies have reported that delay in presentation, rather than in-hospital delay, account for most of the perforations in patients with appendicitis.13-16
We have demonstrated that delaying operations for uncomplicated appendicitis reduced the complication rate and did not alter length of stay. Other studies have confirmed that a 12–24-hour delay before surgery is acceptable.14,17,18 The potential to perform appropriately timed appendicectomy is achieved by providing the duty surgeon with control of access to the emergency theatre during the day. Greater input and supervision from senior clinicians with respect to diagnosis, management and timeliness of intervention enhance the safety of a surgical service.
1 Essential differences between the traditional on-call model for emergency appendicectomy and the acute care surgery (ACS) model
2 Patient demographics, investigations and outcomes*
* Data are number of patients (%) unless otherwise specified. |
|||||||||||||||
3 Outcomes, by time of day of operation
ACS = acute care surgery model. Trad = traditional on-call model. * P < 0.01. † P < 0.05. |
|||||||||||||||
- Robert C Gandy1
- Phillip G Truskett2
- Shing W Wong3
- Sanchia Smith4
- Michael H Bennett5
- Andrew D Parasyn6
- Department of General Surgery, Prince of Wales Hospital, University of New South Wales, Sydney, NSW.
None identified.
- 1. Parasyn AD, Truskett PG, Bennett M, et al. An acute care surgical service — a change in culture. ANZ J Surg 2009; 79: 12-18.
- 2. Earley AS, Pryor JP, Kim PK, et al. An acute care surgery model improves outcomes in patients with appendicitis. Ann Surg 2006; 244: 498-504.
- 3. Meynaud-Kraemer L, Colin C, Vergnon P, et al. Wound infection in open versus laparoscopic appendectomy. A meta-analysis. Int J Technol Assess Health Care 1999; 15: 380-391.
- 4. Chung RS, Rowland DY, Li P, et al. A meta-analysis of randomized controlled trials of laparoscopic versus conventional appendectomy. Am J Surg 1999; 177: 250-256.
- 5. Golub R, Siddiqui F, Pohl D. Laparoscopic versus open appendectomy: a metaanalysis. J Am Coll Surg 1998; 186: 545-553.
- 6. Sauerland S, Lefering R, Holthausen U, et al. Laparoscopic vs conventional appendectomy — a meta-analysis of randomised controlled trials. Langenbecks Arch Surg 1998; 383: 289-295.
- 7. Styrud J, Eriksson S, Nilsson I, et al. Appendicectomy versus antibiotic treatment in acute appendicitis: a prospective multicenter randomized controlled trial. World J Surg 2006; 30: 1033-1037.
- 8. Yardeni D, Hirschl RB, Drongowski RA, et al. Delayed versus immediate surgery in acute appendicitis: do we need to operate during the night? J Pediatr Surg 2004; 39: 464-469.
- 9. Eldar S, Nash E, Sabo E, et al. Delay of surgery in acute appendicitis. Am J Surg 1997; 173: 194-198.
- 10. Paterson HM, Qadan M, de Luca SM, et al. Changing trends in surgery for acute appendicitis. Br J Surg 2008; 95: 363-368.
- 11. Cullinane M, Gray AJ, Hargraves CM, et al. Who operates when? II. The 2003 report of the National Confidential Enquiry into Perioperative Deaths. Section 8. London: NCEPOD, 2003: 69-76.
- 12. Temple CL, Huchcroft SA, Temple WJ. The natural history of appendicitis in adults: a prospective study. Ann Surg 1995; 221: 278-281.
- 13. Maroju NK, Robinson Smile S, Sistla SC, et al. Delay in surgery for acute appendicitis. ANZ J Surg 2004; 74: 773-776.
- 14. Stahlfeld K, Hower J, Homitsky S, et al. Is acute appendicitis a surgical emergency? Am Surg 2007; 73: 626-629.
- 15. Kearney D, Cahill RA, O’Brien E, et al. Influence of delays on perforation risk in adults with acute appendicitis. Dis Colon Rectum 2008; 51: 1823-1827.
- 16. Wong SW, Haxhimolla H, Grieve DA, et al. Insurance and the risk of ruptured appendix in the adult. Aust N Z J Surg 1999; 69: 31-33.
- 17. Abou-Nukta F, Bakhos C, Arroyo K, et al. Effects of delaying appendectomy for acute appendicitis for 12–24 h. Arch Surg 2006; 141: 504-507.
- 18. Clyde C, Bax T, Merg A, et al. Timing of intervention does not affect outcome in acute appendicitis in a large community practice. Am J Surg 2008; 195: 590-592.





Abstract
Objective: To assess the outcomes of appendicectomy in an acute care surgery (ACS) model compared with a traditional on-call (Trad) model.
Design: Retrospective historical control study comparing appendicectomy outcomes in the Trad period (April 2004 to March 2005) with outcomes in the ACS period (April 2006 to March 2007).
Setting: The Prince of Wales Public Hospital, a metropolitan tertiary referral centre in Sydney.
Patients: All adult patients undergoing appendicectomy during 1-year periods before and after the introduction of the ACS model.
Intervention: The introduction of an ACS model for managing all emergency general surgical presentations.
Main outcome measure: Complication rate.
Results: A total of 402 appendicectomies were performed, 176 during the Trad period and 226 during the ACS period. There was no perioperative mortality. The complication rate was lower in the ACS period than the Trad period (9.3% v 17.0%; P = 0.02). After the intervention, there was no significant change in the time from presentation to arrival in theatre or in length of stay, but the proportion of operations performed at night (24:00–08:00) was reduced from 26.1% to 15.0% (P = 0.006). The proportion of negative appendicectomies was reduced from 22.7% to 17.3%, but the change was not statistically significant (P = 0.08). There was no difference in perforation rate before and after the intervention (13.6% v 13.3%; P = 0.86).
Conclusion: The ACS model provides a safe surgical environment for patients and is associated with a reduced complication rate. Under the ACS model, there was an increase in the number of patients treated conservatively overnight, but this did not lead to an overall increase in perforation rate or length of stay.