Bipolar disorder is a common illness that affects 1%–2% of the general population;1 it is therefore often first assessed, and frequently managed, by general practitioners. It usually presents with symptoms of depression, but a diagnosis of bipolar disorder is contingent on the occurrence of an episode of mania or hypomania.2 Consequently, many cases of bipolar disorder remain undetected or are misdiagnosed as major (unipolar) depression. Further, individuals with hypomania rarely seek help, and those with comorbid anxiety or symptoms of depression that do not respond to treatment often resort to self-medication with alcohol or illicit substances. Equally, bipolar disorder is thought to be overdiagnosed in some populations such as adolescents and young adults.3
We synthesised recommendations from recently published guidelines for the treatment of bipolar disorder.4-6 Treatment recommendations are therefore divided into sections on acute bipolar mania, acute bipolar depression and maintenance.
We also conducted a literature search of articles on pharmacological treatment of bipolar disorder that were published up to May 2009 — using electronic databases (MEDLINE, PubMed, PsycINFO), book chapters and articles known to the authors — to identify Cochrane reviews, meta-analyses, review articles and reports from randomised controlled trials. The search terms bipolar disorder, mania, pharmacotherapy, general practice, manic–depressive illness and depression were used. Key recommendations relevant to GPs were synthesised and rated according to National Health and Medical Research Council (NHMRC) levels of evidence.7
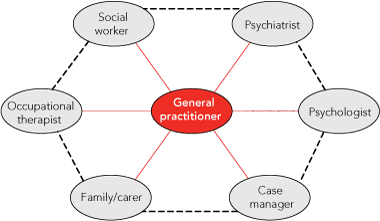
The GP’s role in managing bipolar disorder will vary according to the patient, the severity of the illness and the level of available support. The GP may take on the primary role of treating the patient, with the option of referral to specialist services if and when required. Alternatively, the patient may be primarily managed by an external team, such as a community mental health service, but with links to the GP maintained. Further, multiple professionals are typically involved in working with patients who have a mental illness, including professionals who primarily target clinical interventions and those who target more broad aspects of life affected by the illness, such as social and occupational functioning. While many of the professionals who work with these patients should also communicate with one another, the GP often serves as the focal point around which the other services are provided, including contact with family and carers (Box 1). With respect to pharmacological management, the main priorities for the GP are to assess efficacy, encourage adherence to treatment and monitor for potential side effects. Ideally, treatment plans are developed and initiated following consultation with a psychiatrist, particularly in complex cases, and with referral back to the psychiatrist during periods of increased severity of illness or risk.
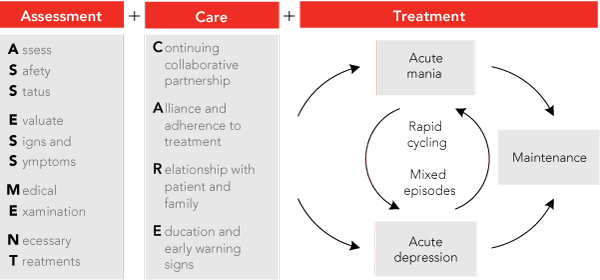
If a diagnosis of bipolar disorder is suspected, the first imperative is to act. Action involves careful assessment so as to provide individualised care and effective treatment. Box 2 provides an overview of the management of bipolar disorder, adapted from previously published recommendations.4 In all cases, management should begin with a detailed clinical assessment that includes diagnostic formulation, assessment of safety and risk, a brief medical examination (including baseline investigations and screening for medical illnesses), and implementation of any necessary action such as facilitating an emergency assessment for hospitalisation. Guidelines for baseline and ongoing monitoring in bipolar disorder have been reviewed in detail recently and are summarised in Box 3. The care principles outlined in Box 2 are applicable throughout all stages of treatment and are essential for effective long-term management. An effective collaborative alliance is important for increasing the likelihood that the patient remains engaged in treatment; this can be fostered by providing emotional support and education to the patient and his or her family. Much of this can be initiated by a GP, but prompt transition to joint involvement of a psychiatrist is recommended, especially when affirming diagnosis and planning future management.
Treatment involves implementing strategies to achieve remission of symptoms of acute manic episodes and/or depressive episodes, as well as longer-term maintenance treatment to optimise social and occupational functioning and prevent relapse. In addition, ensuring safety and specifically reducing the risk of suicide is an ongoing consideration throughout all stages of treatment. Pharmacotherapy remains the primary treatment modality, but ideally it is supplemented with psychological interventions; in some instances, specialist physical measures such as electroconvulsive therapy may also be useful. Box 4 provides a detailed overview of side effects and recommended therapeutic dosing for agents commonly used in bipolar disorder.
During acute mania, an assessment of risk including personal safety, reputation and the safety of others should be undertaken. Steps may need to be taken to manage acute mania — for example, hospitalisation or referral for specialist mental health services is often necessary during this phase of illness. Treatments for acute bipolar mania should aim to treat the acute symptoms of mania and to manage any accompanying behavioural disturbance (Box 5).
With regard to pharmacological treatments, lithium, valproate, atypical antipsychotics, haloperidol and, to a lesser extent, carbamazepine all have indications for acute mania.4-6,9 The choice of agent depends on episode severity, patient preference and likely side effects. While haloperidol is effective in acute mania, it is not a first-line option because of a high risk of extrapyramidal side effects and its inability to prevent depression. If a rapid response is required, valproate or the atypical antipsychotics are preferable to lithium.
If possible, monotherapy should be trialled to reduce the likelihood of adverse effects. However, when there is marked risk or greater severity of illness, or the response to an initial monotherapy trial has not been adequate, combinations such as lithium or valproate combined with an atypical antipsychotic add efficacy.11,12 In general, about 50% of individuals with mania respond to monotherapy with an antimanic agent, and 75% respond to a combination of an atypical antipsychotic and either lithium or valproate.
Depression is the predominant phase of bipolar disorder and, as such, it confers substantive risks in terms of morbidity and suicide.13 In comparison to acute mania, the pharmacotherapy for bipolar depression is more complicated and based on data that are less clear. This is reflected in recommendations that are generally less definitive and vary across guidelines (Box 6).
First-line monotherapy options include lithium, valproate, quetiapine and lamotrigine.9 Lithium is particularly noted for its antisuicidal properties, but is disadvantaged by a delay in effect of 2–3 weeks. First-line medication combinations include olanzapine plus fluoxetine,14 and lithium combined with valproate or lamotrigine.15,16 Each agent, or combination of agents, has unique advantages and disadvantages in relation to clinical effectiveness, speed of antidepressant action, tolerability and prophylactic properties.
Unlike the use of antidepressants in unipolar depression, antidepressant use in bipolar disorder is a controversial issue. The effectiveness of conventional antidepressants in bipolar depression is unclear, and three recent large studies have reported no additional benefit from the adjunctive use of antidepressants in bipolar depression.17-20 Further, in some patients, the use of conventional antidepressants is associated with an increased risk of a switch to mania.17,21,22 Nonetheless, antidepressants may benefit a small cohort of patients with bipolar depression but, if used, should be prescribed in combination with a mood-stabilising agent to minimise the risk of affective instability. In this regard, selective serotonin reuptake inhibitors are preferable because they are less likely to induce a switch to mania than other antidepressant classes and are less dangerous in cases of overdose.23
Maintenance treatment (Box 7) is likely to be necessary in most patients with an established diagnosis of bipolar disorder. Following an acute episode, conservative indications for maintenance treatment include instances where there has been at least one other prior mood episode in the past 5 years or two prior episodes across the lifetime, the acute episode was severe and included suicide risk or psychotic features, or there is ongoing functional disability.
Following an acute episode, it is important to taper and withdraw any agents (such as benzodiazepines or antipsychotics) that were used to manage temporary behavioural or cognitive disturbance. The goal of pharmacotherapy in maintenance is to prevent relapse. In this regard, lithium is still considered the gold-standard treatment, although it appears to be more effective at preventing manic relapse than depression. Lamotrigine and valproate also have prophylactic properties, with lamotrigine being more efficacious at preventing depressive relapse compared with manic relapse.24,25 Other anticonvulsants (eg, carbamazepine) have been less impressive and are not consistently recommended as first-line treatment options.4,9
There is growing interest in the use of atypical antipsychotics for maintenance treatment, and quetiapine, olanzapine and aripiprazole have been shown to have benefits. Quetiapine appears to be equally effective at preventing both manic and depressive episodes, whereas all other atypical antipsychotics are more effective at preventing manic episodes. While some longer-term evidence is beginning to emerge,26-28 the long-term prophylactic properties of atypical antipsychotics are yet to be reliably established and further research is needed before such agents can be confidently recommended for long-term use in bipolar disorder; there is no clear class effect in this regard.
Again, monotherapy is considered ideal and trials of medications may take several months before effectiveness becomes clear. Nonetheless, a significant proportion of patients will not respond adequately and combination regimens are the rule rather than the exception; this may require further consultation with psychiatrists. Treatment options for patients who experience rapid cycling and mixed episodes are summarised in Box 8.
There are a number of novel agents that have shown promise in initial clinical trials in treating bipolar disorder. While further trials are needed before specific recommendations can be made, such agents include N-acetylcysteine,29 omega-3 fatty acids,30 tamoxifen,31,32 asenapine,33 antiglucocorticoids,34 celecoxib,35 modafinil36 and pramipexole.37
3 International Society for Bipolar Disorders guidelines for baseline and ongoing monitoring in bipolar disorder8
4 Side effects and therapeutic dosing for agents commonly used in bipolar disorder*8-10
6 Summary of treatment for bipolar depression
First-line monotherapy options: lithium, valproate, quetiapine and lamotrigine.
First-line combination options: olanzapine plus fluoxetine, and lithium combined with valproate or lamotrigine.
Antidepressants: the efficacy of antidepressants is not established in bipolar depression. If prescribing antidepressants, always do so in combination with an agent that has antimanic properties to limit the risk of affective instability or a switch to mania.
7 Summary of maintenance treatments
Considerations: facilitate engagement in treatment, assess for comorbidities, monitor side effects, provide education about illness, identify and check for early warning signs.
First-line treatments: lithium, lamotrigine, valproate and quetiapine.
Second-line treatments: olanzapine, aripiprazole and carbamazepine.
Inadequate response to treatment: seek consultation with a psychiatrist.
- Gin S Malhi1,2,3
- Danielle Adams1,2
- Michael Berk4,5,6,7
- 1 CADE Clinic, Department of Psychiatry, Royal North Shore Hospital, Sydney, NSW.
- 2 Northern Sydney Central Coast Mental Health Drug and Alcohol Services, Northern Sydney Central Coast Area Health Service, Sydney, NSW.
- 3 Discipline of Psychiatry, University of Sydney, Sydney, NSW.
- 4 Department of Clinical and Biomedical Sciences — Barwon Health, University of Melbourne, Melbourne, VIC.
- 5 The Geelong Clinic, Healthscope, Geelong, VIC.
- 6 Mental Health Research Institute, Melbourne, VIC.
- 7 Orygen Youth Health Research Centre, Melbourne, VIC.
Financial support for this research was provided by the NHMRC (Program Grant 510135).
Gin Malhi has served on international and national pharmaceutical advisory boards, received funding for research and has been in receipt of honoraria for talks at sponsored meetings worldwide involving AstraZeneca, Eli Lilly, Janssen-Cilag, Organon, Pfizer and Wyeth. Danielle Adams has received an honorarium from Eli Lilly for a speaking engagement. Michael Berk has received funding for research from Stanley Medical Research Foundation, MBF, NHMRC, beyondblue, Geelong Medical Research Foundation, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Organon, Novartis, Mayne Pharma and Servier, and honoraria for speaking engagements from AstraZeneca, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Janssen-Cilag, Lundbeck, Pfizer, Sanofi-Synthelabo, Servier, Solvay and Wyeth, and has served as a consultant to AstraZeneca, Bristol-Myers Squibb, Eli Lilly, GlaxoSmithKline, Janssen-Cilag, Lundbeck and Servier.
- 1. Merikangas KR, Akiskal HS, Angst J, et al. Lifetime and 12-month prevalence of bipolar spectrum disorder in the National Comorbidity Survey replication. Arch Gen Psychiatry 2007; 64: 543-552.
- 2. American Psychiatric Association. Diagnostic and statistical manual for mental disorders. 4th ed. Washington, DC: APA, 1994.
- 3. Zimmerman M, Ruggero CJ, Chelminski I, Young D. Is bipolar disorder overdiagnosed? J Clin Psychiatry 2008; 69: 935-940.
- 4. Malhi GS, Adams D, Lampe L, et al. Clinical practice recommendations for bipolar disorder. Acta Psychiatr Scand Suppl 2009; (439): 27-46.
- 5. National Institute for Health and Clinical Excellence. Bipolar disorder: the management of bipolar disorder in adults, children and adolescents, in primary and secondary care. Clinical Guideline 38. London: National Health Service, 2006.
- 6. Yatham LN, Kennedy SH, Schaffer A, et al. Canadian Network for Mood and Anxiety Treatments (CANMAT) and International Society for Bipolar Disorders (ISBD) collaborative update of CANMAT guidelines for the management of patients with bipolar disorder: update 2009. Bipolar Disord 2009; 11: 225-255.
- 7. National Health and Medical Research Council. A guide to the development, implementation and evaluation of clinical practice guidelines. Canberra: Commonwealth of Australia, 1999.
- 8. Ng F, Mammen OK, Wilting I, et al. The International Society for Bipolar Disorders (ISBD) consensus guidelines for the safety monitoring of bipolar disorder treatments. Bipolar Disord 2009; 11: 559-595.
- 9. Malhi GS, Adams D, Cahill CM, et al. The management of individuals with bipolar disorder: a review of the evidence and its integration into clinical practice. Drugs 2009; 69: 2063-2101.
- 10. Malhi GS, Berk M. How to treat bipolar disorder. Aust Doctor 2008; 13 Jun: 25-32. http://www.australiandoctor.com.au/HTT/PDF/ad_025_032__jun13_08.pdf (accessed Jul 2010).
- 11. Scherk H, Pajonk FG, Leucht S. Second-generation antipsychotic agents in the treatment of acute mania: a systematic review and meta-analysis of randomized controlled trials. Arch Gen Psychiatry 2007; 64: 442-455.
- 12. Smith LA, Cornelius V, Warnock A, et al. Acute bipolar mania: a systematic review and meta-analysis of co-therapy vs. monotherapy. Acta Psychiatr Scand 2007; 115: 12-20.
- 13. Mitchell PB, Malhi GS. Bipolar depression: phenomenological overview and clinical characteristics. Bipolar Disord 2004; 6: 530-539.
- 14. Tohen M, Vieta E, Calabrese J. Efficacy of olanzapine and olanzapine/fluoxetine combination in the treatment of bipolar I depression. Arch Gen Psychiatry 2003; 60: 1079-1088.
- 15. van der Loos ML, Mulder PG, Hartong EG, et al. Efficacy and safety of lamotrigine as add-on treatment to lithium in bipolar depression: a multicenter, double-blind, placebo-controlled trial. J Clin Psychiatry 2009; 70: 223-231.
- 16. Young LT, Joffe RT, Robb JC, et al. Double-blind comparison of addition of a second mood stabilizer versus an antidepressant to an initial mood stabilizer for treatment of patients with bipolar depression. Am J Psychiatry 2000; 157: 124-126.
- 17. Gijsman HJ, Geddes JR, Rendell JM, et al. Antidepressants for bipolar depression: a systematic review of randomized, controlled trials. Am J Psychiatry 2004; 161: 1537-1547.
- 18. Sachs GS, Nierenberg AA, Calabrese JR, et al. Effectiveness of adjunctive antidepressant treatment for bipolar depression. N Engl J Med 2007; 356: 1711-1722.
- 19. Ghaemi SN. Why antidepressants are not antidepressants: STEP-BD, STAR*D, and the return of neurotic depression. Bipolar Disord 2008; 10: 957-968.
- 20. Malhi GS. Seeking definition. Bipolar Disord 2008; 10: 853-855.
- 21. Leverich GS, Altshuler LL, Frye MA, et al. Risk of switch in mood polarity to hypomania or mania in patients with bipolar depression during acute and continuation trials of venlafaxine, sertraline, and bupropion as adjuncts to mood stabilizers. Am J Psychiatry 2006; 163: 232-239.
- 22. Post RM, Altshuler LL, Leverich GS, et al. Mood switch in bipolar depression: comparison of adjunctive venlafaxine, bupropion and sertraline. Br J Psychiatry 2006; 189: 124-131.
- 23. Peet M. Induction of mania with selective serotonin re-uptake inhibitors and tricyclic antidepressants. Br J Psychiatry 1994; 164: 549-550.
- 24. Bowden CL, Calabrese JR, Sachs G, et al. A placebo-controlled 18-month trial of lamotrigine and lithium maintenance treatment in recently manic or hypomanic patients with bipolar I disorder. Arch Gen Psychiatry 2003; 60: 392-400.
- 25. Calabrese JR, Bowden CL, Sachs G, et al. A placebo-controlled 18-month trial of lamotrigine and lithium maintenance treatment in recently depressed patients with bipolar I disorder. J Clin Psychiatry 2003; 64: 1013-1024.
- 26. Vieta E, Eggens I, Persson I, et al. Efficacy and safety of quetiapine in combination with lithium/divalproex as maintenance treatment for bipolar I disorder (international trial D1447C00126). Eur Psychiatry 2008; 23 Suppl 2: S237-S238.
- 27. Suppes T, Liu S, Brecher M, et al. Maintenance treatment in bipolar I disorder with quetiapine concomitant with lithium or divalproex: a placebo-controlled, randomized multicenter trial: Abstracts from the 3rd Biennial Conference of the International Society for Bipolar Disorders 2008. Bipolar Disord 2008; 10 Suppl 1: 40.
- 28. Brecher M, Anderssen H, Paulsson B. Quetiapine in the maintenance treatment of bipolar I disorder: combined data from two long-term phase III studies. Eur Psychiatry 2008; 23 Suppl 2: S225-S226.
- 29. Berk M, Copolov DL, Dean O, et al. N-acetyl cysteine for depressive symptoms in bipolar disorder — a double-blind randomized placebo-controlled trial. Biol Psychiatry 2008; 64: 468-475.
- 30. Montgomery P, Richardson AJ. Omega-3 fatty acids for bipolar disorder. Cochrane Database Syst Rev 2008; (2): CD005169. doi: 10.1002/14651858.
- 31. Palmer JT, Payne JL. Stabilization of hypomania following initiation of tamoxifen. Am J Psychiatry 2008; 165: 650-651.
- 32. Mathew SJ, Manji HK, Charney DS. Novel drugs and therapeutic targets for severe mood disorders. Neuropsychopharmacology 2008; 33: 2080-2092.
- 33. Calabrese J, Cohen M, Zhao J, Panagides J. Efficacy and safety of asenapine as adjunctive treatment for acute mania associated with bipolar disorder [Abstract NR3-061]. New Research Abstracts, Annual Meeting of the American Psychiatric Association. Washington, DC: American Psychiatric Association, 2008
- 34. Gallagher P, Malik N, Newham J, et al. Antiglucocorticoid treatments for mood disorders. Cochrane Database Syst Rev 2008; (1): CD005168.
- 35. Nery FG, Monkul ES, Hatch JP, et al. Celecoxib as an adjunct in the treatment of depressive or mixed episodes of bipolar disorder: a double-blind, randomized, placebo-controlled study. Hum Psychopharmacol 2008; 23: 87-94.
- 36. Frye MA, Grunze H, Suppes T, et al. A placebo-controlled evaluation of adjunctive modafinil in the treatment of bipolar depression. Am J Psychiatry 2007; 164: 1242-1249.
- 37. Goldberg JF, Burdick KE, Endick CJ. Preliminary randomized, double-blind, placebo-controlled trial of pramipexole added to mood stabilizers for treatment-resistant bipolar depression. Am J Psychiatry 2004; 161: 564-566.





Abstract
Objective: To provide a practical overview of the pharmacological management of adults with bipolar disorder in primary care and the role of general practitioners in the pharmacotherapy of this complex disorder.
Data sources: Published guidelines for the treatment of bipolar disorder, plus Cochrane reviews, meta-analyses, review articles and reports from randomised controlled trials that were published up to May 2009.
Study selection: Over 500 articles on the treatment of bipolar disorder were reviewed, with an emphasis on meta-analyses and systematic reviews of randomised controlled trials. Where evidence was more limited, open trials and non-controlled data were also reviewed.
Data extraction: Key recommendations relevant to GPs were synthesised and rated according to National Health and Medical Research Council levels of evidence.
Data synthesis: Lithium, valproate and atypical antipsychotics are first-line treatment options for acute mania, and monotherapy is ideal if it produces an adequate response. For depressive episodes, recommendations are less definitive and the use of antidepressants is controversial. Most patients require maintenance treatment, during which pharmacotherapy should be used to prevent relapse, and psychological and social interventions should be considered.
Conclusions: Bipolar disorder is a lifelong episodic illness that affects 1%–2% of the population, many of whom are principally managed by their GPs. Pharmacological treatment with mood-stabilising agents is the primary form of management, although this is ideally provided in conjunction with psychosocial interventions.