In England in 2007, a young woman named Kerrie Wooltorton drank ethylene glycol and presented to a hospital with a letter refusing medical treatment (Box 1). Her doctors’ decision to allow her to die generated considerable debate in the profession and the media.1-5
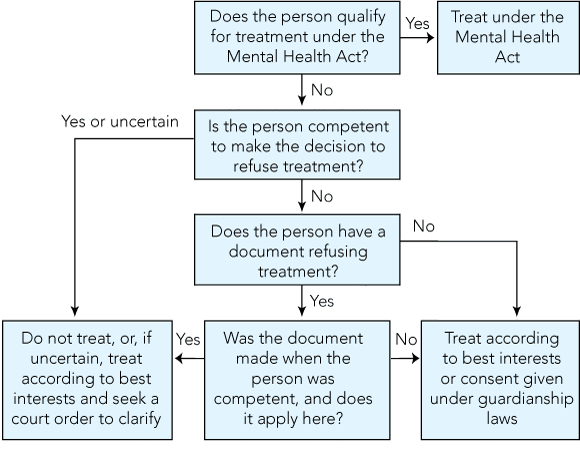
Here, we imagine a patient presenting to an Australian hospital in similar circumstances. We suggest a practical three-stage approach for health care providers to an apparent treatment refusal after an attempted suicide (Box 2) and examine some of the legal and ethical issues that might arise along the way.
If the patient is not subject to the Mental Health Act, or if the treating team feel that the use of the mental health laws would be inappropriate, the next question is whether he or she is competent to refuse treatment.
In most circumstances, the law recognises that a competent person may refuse medical treatment, even if that decision is “not sensible, rational or well considered”6,7 and even if refusal will likely lead to death or serious injury.6-9 Doctors who continue to provide medical treatment to a patient who has competently refused that treatment will be committing a trespass, which may give rise to an action for battery or, potentially, a criminal charge.10,11 So, in most cases when a patient is not subject to the Mental Health Act and is competent, a refusal of treatment should be respected. The fact that a patient has attempted suicide is not, by itself, a basis for concluding that a patient is not competent.
Under the common law, an adult is presumed to be competent to refuse medical treatment, but this presumption may be overturned if there is evidence that the person does not have capacity to make the decision.6 The common law defines “capacity” as a sufficient understanding of the nature, purpose and effects of the proffered treatment,12 and demands that the competent patient be able to do three things: comprehend and retain the treatment information; believe the information; and weigh it among other factors to reach a decision.6,13 The patient must also be able to communicate the decision.14 Some states and territories have defined capacity in their guardianship legislation, but most definitions are based on this common law interpretation. Sufficiency of capacity is seen as a spectrum, and, the more profound the consequences of the decision, the higher the level of capacity that must be demonstrated.6,7,13 A decision that is likely to lead to the patient’s death will require demonstration of a high level of capacity.
An unconscious patient will always be incompetent.14 If the patient is conscious, clinicians must carefully assess his or her mental state and cognition. Patients who arrive at hospital after a toxic ingestion will often be delirious or intoxicated with the substance they have taken. Ethylene glycol, for example, causes a state like alcohol intoxication within an hour or so.15 Even a mildly delirious or intoxicated patient will lack the level of capacity required to comprehend, retain and weigh information about a choice with such profound consequences.
Patients in clear consciousness, not subject to the Mental Health Act, will require detailed assessment of their capacity. They must be provided with information about the risks and benefits of treatment options and information about the consequences of not being treated. Clinicians must decide whether the patient can comprehend and retain the treatment information. An ability to paraphrase the information provided is evidence of comprehension and retention. To be competent, patients must also believe the information. This is not to say they may not disagree with the information given; rather, they must not be affected by a delusion that interferes with their ability to believe it. Of course, if the patient has a delusion, he or she will usually be treatable under the Mental Health Act. Finally, the doctor must decide if the patient can weigh the information and use it to reach a decision. This element is best tested by a series of Socratic questions probing the patient’s motivation for his or her choice and clarifying apparent inconsistencies.
It is important to note that a competent decision to refuse treatment need not be rational per se, and need not be based on beliefs that everybody shares — Jehovah’s Witnesses may competently refuse a blood transfusion based on their religious beliefs. However, it is important that the patient’s reasoning be internally consistent and follow logically from any starting premises.14 The law also recognises that confusion, shock, fatigue, pain or fear may all erode capacity.7,13
If the patient is definitely competent and not subject to the Mental Health Act, then his or her decision to refuse treatment should probably be honoured (see “Other considerations”). If the patient is not competent but is carrying a document requesting no treatment, the next step is to examine that document. If the patient is incompetent and carries no such document, he or she should be treated according to an assessment of his or her best interests, notwithstanding a stated refusal of that treatment.6,16 Guardianship laws in all Australian states and territories provide for consent to be given by a substitute decisionmaker in the same circumstances.
If a patient is not competent, any document refusing medical treatment will require further consideration as to whether it may be a valid advance care directive under state or territory laws.
As a general rule, if an advance care directive is made by a capable adult, is clear and unambiguous, and extends to the situation at hand, it must be respected.6 All jurisdictions require that the patient was competent at the time it was completed.
Most people who present in a manner similar to Ms Wooltorton will not have made a considered decision to die.17 For most, the attempt will be impulsive, and a suicide note, even one refusing treatment, will be unwitnessed, written in the context of that impulsive decision, and will contain insufficient information to make a confident judgement about the person’s capacity.18 Even Ms Wooltorton’s note, which was unusually direct and specific, contained little information on which to judge her capacity at the time of writing. It provided no justification for her decision, told nothing of how she came to it, and, in requesting that no questions be asked of her, made an unreasonable and unrealistic demand. It was certainly not detailed enough to allow the in-depth analysis of capacity required to be reasonably sure that she was competent when she wrote it.
Ms Wooltorton had taken similar overdoses in the past, for which she had received life-saving medical treatment. After her previous overdoses, she seemed to have decided, at least for a time, to get on with life. Were things different this time? Why? How long had things been different? Why had she called the ambulance, knowing there was a good chance she would be treated against her will? Why was it so important that she not die alone, that she would risk almost certainly not dying at all? Is it possible that her calling the ambulance revealed an ongoing ambivalence about dying that was not apparent in the letter’s text?
Leaving the law to one side momentarily, it is generally suggested that competent decisions, at least those with profound and irreversible consequences, must be well considered and consistent with a person’s usual or sustained life views.19 This is not to imply that people cannot change their minds, but rather that such choices should be consistent with a person’s agency, or what they generally want from life. This notion recognises that we may all be impulsive and make decisions that we might normally (and will later) regret. It holds that, when it comes to important irreversible decisions, our normal selves have a sort of moral primacy and deserve a chance to reconsider the actions of our impulsive selves. Recognition of this concept partly underlies the provisions for a cooling-off period after making certain significant financial commitments — like buying a home or even entering into a mobile phone contract. This need for consistency with a person’s “normal self” raises significant problems when assessing a refusal of treatment in a situation like Ms Wooltorton’s. Although she presented with a letter declining treatment, she refused or, more likely, was unable15 to justify her decision in terms of her normal wishes and desires.
In any case, whether or not a person’s agency has been fully engaged in a decision to refuse treatment is not a direct consideration in the common law test for competence — unless it indicates that the patient has not understood the nature, purpose and effects of the proposed treatment. It is not clear to what extent Ms Wooltorton did, or could, participate in a discussion to allow a proper assessment of her capacity, and her doctors may have largely had to guess. They guessed she was competent according to the law, and the coroner, who clearly sympathised with the difficulties the treating clinicians faced, agreed (Inquest into the death of Kerrie Wooltorton, 29 September 2009, unpublished extracts, Norfolk Coroner Service, Norwich, UK). In the end though, without the ability to check with her directly, their judgement was only a guess made with limited information.
A suicide note like Ms Wooltorton’s should be distinguished from other more conventional advance directives, like those refusing blood transfusion for Jehovah’s Witnesses, or those refusing specific treatments for people with terminal illness. These documents are typically carefully constructed, witnessed, appear to reflect more considered opinion, and may offer much less room for doubt on validity and applicability.
If a patient’s decision to refuse treatment is clearly and unambiguously competent, or their advance directive is clearly and unambiguously valid and applicable, then health professionals should probably honour the patient’s decision. We use the qualifier “probably” here because, even in these situations, which we believe will be very rare, there are still ethical and legal arguments against giving effect to a decision to refuse treatment that need further consideration. For example, while the right to autonomy is strong, in some circumstances there may be competing rights and interests that are sufficient to override a competent decision to refuse treatment. These may include the state’s interests in preventing suicide and the need to protect innocent third parties, such as dependent children and even fetuses.20
While the strength of these other rights and interests are not certain, they may, in theory at least, be sufficient to invalidate a competent patient’s decision to refuse medical treatment — particularly in an attempted suicide. If this were the case, and the patient were not treated, it might be possible for the patient’s family to bring an action in negligence with a hefty damages claim. Kerrie Wooltorton’s parents have reportedly begun such proceedings.21 There is also the possibility that refusal to treat in these circumstances might be construed as aiding and abetting a suicide attempt, which is illegal in all Australian states and territories. Some jurisdictions provide a defence to people who use force to prevent a suicide (Crimes Act 1900 [NSW] s. 574B; Crimes Act 1900 [ACT] s. 18; Crimes Act 1958 [Vic] s. 463B; Criminal Law Consolidation Act 1935 [SA] s. 13A). This defence protects against criminal prosecution and may also prevent a civil claim; however, the applicability of this defence to the case of an otherwise valid refusal of medical treatment is not established.
If the treating doctors remain uncertain about the patient’s capacity or about the validity of an advance directive, or if they are uncertain as to whether an apparently competent request to refuse treatment should be followed (eg, because of concerns about aiding a suicide), there is a further option. They may provide life-saving treatment under the doctrine of necessity and simultaneously seek an urgent court order to clarify these questions.
Admittedly, this course of action is not risk-free, as a court may ultimately disagree with the clinicians’ interim assessment of the patient’s capacity, and there is a risk of civil and criminal liability for assault if the doctrine of necessity were held by a court not to apply in these circumstances. However, the law recognises that where there is genuine doubt about the legality of a decision to refuse treatment, that doubt falls to be resolved in favour of the preservation of life, at least until the legality of the refusal is confirmed.6,7
A presentation like Ms Wooltorton’s places an enormous burden on the treating team. In addition to the clinical demands associated with treating a patient with a life-threatening condition, clinicians must do their best to ascertain the patient’s capacity for his or her apparent decision, consider the correct ethical course, and navigate through uncharted legal waters.
While ultimately each case will need to be examined on its individual merits, we believe that, in most cases, clinicians will be acting ethically and within the law if they provide treatment to such patients, unless the patient cannot be treated under mental health legislation and there is no doubt that the patient’s refusal of treatment is competent.
1 The Wooltorton case
Kerrie Wooltorton was 26 years old when she presented to Norfolk and Norwich University Hospital, having consumed 350 mL of ethylene glycol. She carried a letter dated 3 days earlier that began:
To whom this may concern If I come into hospital regarding an overdose or any attempt of my life, I would like for NO life saving treatment to be given. I would appreciate it if you could continue to give medicines to help relieve my discomfort, painkillers, oxygen etc. I would hope these wishes would be carried out without loads of questioning.
Over three further paragraphs, the letter went on to assure the reader that the author knew the consequences of her refusal, including the likelihood of renal failure should she survive. It also stated specifically that she did not want dialysis and insisted that she had called the ambulance only because she did not wish to die alone at home, not because she had wanted treatment.
When questioned, Ms Wooltorton said simply, “It’s in the letter, it says what I want”.
The treating team consulted widely and sought legal advice. They took the view that Ms Wooltorton was competent to refuse treatment and, on this basis, believed they were obliged to act in accordance with her wishes. She was not given life-saving treatment and died in hospital 2 days later. The Norfolk Coroner recently endorsed the doctors’ decisions (Inquest into the death of Kerrie Wooltorton, 29 September 2009, unpublished extracts, Norfolk Coroner Service, Norwich, UK).
- Christopher J Ryan1,2
- Sascha Callaghan1
- 1 Centre for Values, Ethics and the Law in Medicine, University of Sydney, Sydney, NSW.
- 2 Discipline of Psychiatry, University of Sydney, Sydney, NSW.
None identified.
- 1. Appleby L. The verdict on Wooltorton — clarifying the law [letter]. RCPsych News 2010; January. http://www.rcpsych.ac.uk/members/rcpsychnews/january2010/applebyletter.aspx (accessed May 2010).
- 2. McLean SAM. Live and let die. BMJ 2009; 339: b4112.
- 3. Bashir FA, Crawford M. Autonomy or life saving treatment for the mentally vulnerable [letter]? BMJ 2009; 339: b4400.
- 4. Dyer C. Coroner rules that treating 26 year old woman who wanted to die would have been unlawful. BMJ 2009; 339: b4070.
- 5. Smith R, Laing A, Devlin K. Doctors feared saving suicidal young woman. Sydney Morning Herald 2009; 2 Oct: 6.
- 6. Hunter and New England Area Health Service v A [2009] NSWSC 761.
- 7. Re T (Adult: Refusal of Treatment) [1992] EWCA Civ 18.
- 8. Airedale Hospital Trustees v Bland [1992] UKHL 5.
- 9. Re PVM [2000] QGAAT 1.
- 10. Brightwater Care Group (Inc) v Rossiter [2009] WASC 229.
- 11. Secretary, Department of Health and Community Services v JWB and SMB (“Marion’s Case”) [1992] HCA 15.
- 12. Re C (Adult: Refusal of Medical Treatment) [1994] 1 All ER 819.
- 13. Re MB (Medical Treatment) [1997] EWCA Civ 1361.
- 14. Stewart C, Biegler P. A primer on the law of competence to refuse medical treatment. Aust Law J 2004; 78: 325-342.
- 15. Leth PM, Gregersen M. Ethylene glycol poisoning. Forensic Sci Int 2005; 155: 179-184.
- 16. F v West Berkshire Health Authority [1990] UKHL 1.
- 17. Hall RCW, Platt DE, Hall RCW. Suicide risk assessment: a review of risk factors for suicide in 100 patients who made severe suicide attempts. Psychosomatics 1999; 40: 18-27.
- 18. Barr W, Leitner M, Thomas J. Self-harm or attempted suicide? Do suicide notes help us decide the level of intent in those who survive? Accid Emerg Nurs 2007; 15: 122-127.
- 19. Richardson G. Autonomy, guardianship and mental disorder: one problem, two solutions. Mod Law Rev 2002; 65 (5): 702-723.
- 20. Stewart C. Public interests and the right to die: compelling reasons for overriding the right to self-determination. Issues Paper 14. Sydney: Australian Institute of Health, Law & Ethics, 2001.
- 21. Bingham J, Cockcroft L, Prince R. Family of ‘living-will’ girl to sue hospital. Telegraph (London) 2009; 2 Oct: 7.





Abstract
When a patient presents to hospital after a suicide attempt and appears to refuse treatment, clinicians should first assess if he or she should be treated under mental health legislation, regardless of competence to refuse treatment.
When it is not possible or is inappropriate to treat under mental health legislation, the person’s competence to refuse treatment should be assessed. If the patient is definitely competent, his or her decision to refuse treatment should probably be honoured.
If an incompetent patient carries a document refusing treatment, clinicians must determine the validity of that document as an advance care directive — including whether or not the patient was competent at the time it was written.
The law around the right to refuse treatment after a suicide attempt remains unclear and, if uncertain of what to do, clinicians should provide urgently required life-saving treatment and simultaneously seek an urgent court order to clarify how they should proceed.
In all but extraordinary circumstances, a patient who refuses treatment after a suicide attempt can and should be given life-saving treatment, under either mental health legislation or the common law concept of necessity.