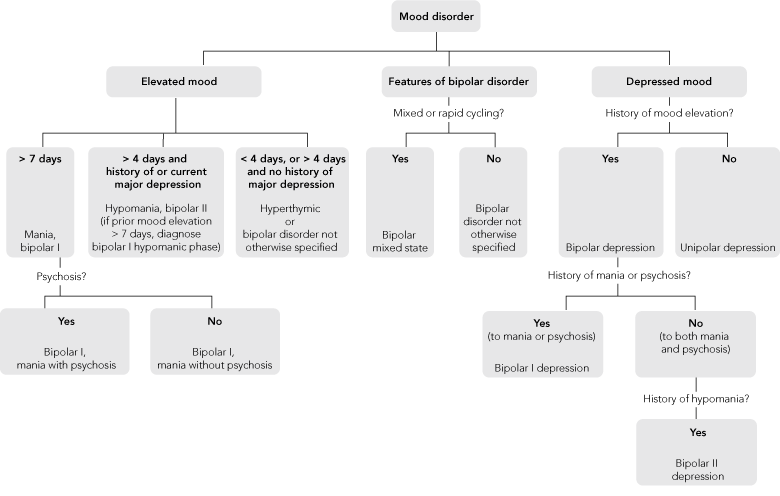
Bipolar disorders are classified in a number of ways. One diagnostic system is described in the Diagnostic and statistical manual of mental disorders, fourth edition, text revision (DSM-IV-TR),1 which is United States based; another is described in the International statistical classification of diseases and related health problems, 10th revision (ICD-10),2 which is World Health Organization and predominantly European based. Although these diagnostic classifications have similarities, there are several differences in their detail. Here we refer to the DSM-IV-TR1 criteria, unless otherwise specified. Box 1 provides a summarised approach to classifying bipolar disorder.
The most florid presentation of bipolar disorder is type I, in which mood elevations are marked and include clinical features of mania (see Box 2 for a guide derived from DSM-IV-TR criteria for a manic episode1). This illness has a distinct period of abnormality with persistently elevated, expansive, or irritable mood lasting at least a week, or requiring hospitalisation.
Although bipolar disorder is defined by mood elevation, the greatest disability and risk occurs during depression, which is typically the dominant phase of the illness, especially for those who are untreated. Depression typically takes up 30%–50% of the patient’s life and mania takes up about 5%–10%, with a semblance of normality making up the remainder of the patient’s life.3-5
Features of depression associated with bipolar disorder (referred to as bipolar depression) are essentially the same as those of major depression (see Box 3 for a guide derived from DSM-IV-TR criteria for a major depressive episode1) but occur in patients with a history of mania or hypomania. Depressive features themselves cannot distinguish bipolar disorder from unipolar depression, although some features appear more commonly in bipolar disorder.6 These include the tendency to have atypical features of depression, with symptoms such as hypersomnia (rather than insomnia) and hyperphagia (rather than anorexia). These features are indicative, rather than diagnostic, of bipolar depression. The presence of psychotic symptoms in the depressive phase also suggests an increased likelihood of bipolar disorder (see Mitchell et al).7
During bipolar depression, patients can feel desperate about the depth and severity of and disability from their low mood. They may not recall or be able to think of the prospect of returning to normal mood and normal life — they may not even recall antecedent mood elevations. They can also feel suicidal; 10%–19% of patients diagnosed with bipolar disorder commit suicide.8 Suicide usually occurs during a depressive episode (79%)9 when the risk of suicide is 15 times that of the general population.10 Patients with bipolar disorder who have attempted suicide are over four times more likely than those who have not attempted suicide to subsequently attempt or complete suicide.11
As bipolar depression requires different treatments than those used for unipolar depression, treatment resistance (ie, the loss of effectiveness of antidepressants that initially appeared effective) may be a hint of bipolar disorder. Although this may seem paradoxical, antidepressants may be ineffective, only briefly effective or more destabilising than helpful for many patients with bipolar disorder. Antidepressant use is more likely to increase the rate of mood cycling, induce mood elevation or result in a mixed state than mood-stabilising agents (see Malhi et al).12
Bipolar II disorder is characterised by cyclical mood and defined by mood elevation in a patient who has had at least one or more major depressive episodes. The persistently elevated, expansive or irritable mood (referred to as hypomania) only needs to last at least 4 days (see Box 4 for a guide derived from DSM-IV-TR criteria for a hypomanic episode1), rather than a week as in mania; however, if the patient is hospitalised during hypomania, the diagnosis becomes bipolar I disorder. The ICD-102 criteria differentiate hypomania on the basis of a persistent mild elevation of mood with less disorganisation than in mania, rather than the more marked mood elevation and disorganisation of mania.
Although it might seem that bipolar II disorder is a less severe illness than bipolar I disorder, it can be associated with increased disability. Although elevated mood is less severe, patients spend more time in the depressive phase of their illness,3 and may be severely ill and suicidal. As with bipolar I disorder, the dominant phase of this illness is depression.
Mixed episodes occur when patients have features of mood elevation and depression simultaneously. DSM-IV-TR1 criteria for a mixed episode require that the patient has full features of both mania and depression. Using this approach, mixed episodes do not include mixed states where only some criteria are met, or states in which there are simultaneous features of both elevation and depression but not the severity of either mania or major depression. Many experts in psychiatry view the DSM-IV-TR1 criteria as being too strict and limiting. In contrast, ICD-102 criteria allow for the diagnosis of a mixed episode in the presence of either of a mixture of manic and depressive symptoms or a rapid alteration between manic and depressive symptoms.
Bipolar illnesses are often complicated by use of alcohol or illicit drugs. Substance misuse is more common in bipolar I disorder (50%) than bipolar II disorder (39%); alcohol is the most commonly misused substance (42% and 34% for bipolar I and II, respectively),3 and illicit drug use is also common. Sometimes the mood disorder will be undiagnosed in the context of florid substance misuse. Diagnosis can be problematic in such patients because alcohol and many drugs can cause substantive mood alterations that remit without treatment once substance use ceases.
Most patients with bipolar disorder will have two or fewer episodes of mood disorder per year. Some may have many years between episodes. In this latter case, when there is an episode of bipolar mood elevation or depression after many years of euthymia, the clinician should always check for possible organic precipitants. Patients who have four or more episodes in one year are referred to as having a rapid cycling disorder. These patients are typically difficult to treat and often unresponsive to conventional mood stabiliser regimens (see Malhi et al, The pharmacological treatment of bipolar disorder in primary care).12 Occasionally, patients may experience mood changes more than once per day, typically being depressed in the morning, with mood elevation in the evening or at night. This has been referred to as ultradian cycling, and can raise diagnostic confusion with borderline personality disorder.
Consistent with a prevailing view that bipolar disorder has a primary biological basis, structural neuroimaging studies have revealed a reduction in central nervous system volume in patients with bipolar I disorder and increased rates of deep white matter hyperintensities.13 There may be a loss of hippocampal volume, consistent with that seen in untreated depression.14,15 There are also significant cognitive deficits in bipolar disorder, even during euthymia, which can impede functioning.16 These impairments can result in patients who seem to have achieved symptomatic recovery not regaining full social and occupational rehabilitation. Thus, a goal of treatment should be a full remission of all symptoms and rehabilitation, rather than only alleviation of mood symptoms.16
Antecedent depression may predate the first episode of mood elevation by many years. Mood elevation may seem to be the element which defines bipolar disorder, but depression is the more enduring element of the illness and results in the greatest disability over time.17
There is controversy over the long-term outcome of bipolar depression. Clinically, some experts believe that depressive episodes tend to become more severe over time, while mood elevation tends to decline over time. However, some data suggest that the proportions of mania and depression remain stable into old age.18 Depression is not always full syndromic major depression. Even less severe depressive states can cause considerable disability, demoralisation, and increase the likelihood of a more complete relapse that may result in hospitalisation.
2 Guide for diagnosing a manic episode*
(1) inflated self-esteem or grandiosity
(4) flight of ideas or feeling that thoughts are racing
(6) increase in goal-directed activity, or agitation
C. The symptoms do not meet criteria for a mixed episode.
4 Guide for diagnosing a hypomanic episode*
(1) inflated self-esteem or grandiosity
(4) flight of ideas or feeling that thoughts are racing
(6) increase in goal-directed activity, or agitation
D. The disturbance in mood and the change in functioning are observable by others.
* Derived from the Diagnostic and statistical manual of mental disorders, fourth edition, text revision.1
3 Guide for diagnosing a major depressive episode*
(1) depressed mood most of the day, nearly every day
(2) marked loss of interest or pleasure in all, or almost all, activities
(3) significant weight loss when not dieting, or weight gain, or altered appetite
(4) insomnia or hypersomnia nearly every day
(5) psychomotor agitation or retardation nearly every day
(7) feelings of worthlessness or excessive or inappropriate guilt
(8) loss of ability to think or concentrate, or indecisiveness
B. The symptoms do not meet criteria for a mixed episode.
C. The symptoms cause clinically significant distress or impairment.
E. The symptoms are not better accounted for by bereavement.
* Derived from the Diagnostic and statistical manual of mental disorders, fourth edition, text revision.1
- John W G Tiller1
- Isaac Schweitzer2
- 1 Department of Psychiatry, Albert Road Clinic, University of Melbourne, Melbourne, VIC.
- 2 Department of Psychiatry, The Melbourne Clinic, University of Melbourne, Melbourne, VIC.
We thank Ms Iveta Krivonos, Research Assistant, for assisting in the preparation of this article.
John Tiller is on the Board of Directors of Therapeutic Guidelines Limited (unpaid position) and has received speaker fees and travel assistance from AstraZeneca, Eli Lilly, Lundbeck, Pfizer, Schering-Plough and Wyeth. Isaac Schweitzer has received payment for board membership and honoraria from AstraZeneca, Eli Lilly, Lundbeck, Pfizer, Schering-Plough and Wyeth.
- 1. American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 4th ed. Text revision. Washington, DC: APA, 2000.
- 2. World Health Organization. International statistical classification of diseases and related health problems, 10th revision. Geneva: WHO, 1992.
- 3. Judd LL, Akiskal HS, Schettler PJ, et al. The comparative clinical phenotype and long term longitudinal episode course of bipolar I and II: a clinical spectrum or distinct disorders? J Affect Disord 2003; 73: 19-32.
- 4. Judd LL, Akiskal HS, Schettler PJ, et al. The long-term natural history of the weekly symptomatic status of bipolar I disorder. Arch Gen Psychiatry 2002; 59: 530-537.
- 5. Judd LL, Akiskal HS, Schettler PJ, et al. A prospective investigation of the natural history of the long-term weekly symptomatic status of bipolar II disorder. Arch Gen Psychiatry 2003; 60: 261-269.
- 6. Mitchell PB, Goodwin GM, Johnson GF, et al. Diagnostic guidelines for bipolar depression: a probabilistic approach. Bipolar Disord 2008; 10: 144-152.
- 7. Mitchell PB, Loo CK, Gould BM. Diagnosis and monitoring of bipolar disorder in general practice. Med J Aust 2010; 193 (4 Suppl): S10-S13. <MJA full text>
- 8. Goodwin FK, Jamison KR. Manic-depressive illness. New York: Oxford University Press, 1990.
- 9. Isometsa E, Henriksson M, Aro H, et al. Suicide in psychotic major depression. J Affect Disord 1994; 31: 187-191.
- 10. Harris EC, Barraclough B. Review: risk for suicide is increased for most mental disorders where patients require treatment in a hospital setting. Br J Psychiatry 1997; 170: 205-228.
- 11. Marangell LB, Bauer MS, Dennehy EB, et al. Prospective predictors of suicide and suicide attempts in 1,556 patients with bipolar disorders followed for up to 2 years. Bipolar Disord 2006; 8: 566-575.
- 12. Malhi GS, Adams D, Berk M. The pharmacological treatment of bipolar disorder in primary care. Med J Aust 2010; 193 (4 Suppl): S24-S30. <MJA full text>
- 13. Kempton MJ, Geddes JR, Ettinger U, et al. Meta-analysis, database, and meta-regression of 98 structural imaging studies in bipolar disorder. Arch Gen Psychiatry 2008; 65: 1017-1032.
- 14. Sheline YI, Gado MH, Kraemer HC. Untreated depression and hippocampal volume loss. Am J Psychiatry 2003; 160: 1516-1518.
- 15. Frodl T, Meisenzahl EM, Zetzsche T, et al. Hippocampal and amygdala changes in patients with major depressive disorder and healthy controls during a 1-year follow-up. J Clin Psychiatry 2004; 65: 492-499.
- 16. Goldberg F, Burdick KE, editors. Cognitive dysfunction in bipolar disorder: a guide for clinicians. Arlington, Va: American Psychiatric Publishing, 2008.
- 17. Judd LL, Akiskal HS, Schettler PJ, et al. Psychosocial disability in the course of bipolar I and II disorders. A prospective, comparative, longitudinal study. Arch Gen Psychiatry 2005; 62: 1322-1330.
- 18. Angst J, Sellaro R. Historical perspective and natural history of bipolar disorder. Biol Psychiatry 2000; 48: 445-457.





Abstract
Bipolar disorders are cyclical mood disorders with clinical features including distinct sustained periods of mood elevation.
Briefer (4 days or more), mild episodes of mood elevation define bipolar II disorder; lengthier (7 days or more), more severe episodes (or those requiring hospitalisation), with or without psychotic features, define bipolar I disorder.
Depressive periods are more common and lengthier than manic or hypomanic states, and are the main cause of disability.
Bipolar depression may respond poorly to antidepressants and these medications may destabilise the illness. The diagnosis of bipolar disorder should be considered when a patient with depression is treatment resistant.
Irritability is a common symptom in bipolar disorder, particularly during mixed states (during which patients have features of mood elevation and depression concurrently) or when there is rapid cycling of mood (more than four episodes of mood disorder per year).
Alcohol misuse and use of illicit drugs may simulate mood changes in bipolar disorder.
Accurate diagnosis and assessment of bipolar disorder is essential for clinical decision making and determining prognosis and treatments.