There are concerns about increasing rates of child maltreatment in Australia, with a 50% increase in notifications from the financial years 2002–03 to 2006–07, and a 45% increase in substantiated notifications.1 To prevent child maltreatment, it is important that we provide support for at-risk families, or at least identify children who are being maltreated early in the abuse cycle, to reduce harm.2 Hospitals play an important role in identifying and treating suspected non-accidental injuries and reporting them to child protection agencies.
To date, no studies in Australia have investigated whether children presenting to hospitals with suspected maltreatment are being notified to child protection agencies, and the outcome of such notifications. However, a recent study did find that children subject to abuse substantiated by child protection agencies had a higher prior rate of emergency department use.3 Our aim in this study was to determine the extent to which children with hospital admissions related to assault or maltreatment or a notified sexually transmitted infection (STI) have subsequent contact with child protection agencies. We also investigated specific injuries often associated with child maltreatment.
We obtained child protection data that included notifications, substantiations and out-of-home care for 1990 to 2005, inclusive. Notifications consist of reports made to the DCP about concerns of maltreatment or risk of harm. A substantiation is made when there is reasonable cause to believe the child has been or is at risk of harm.4 In 1995, the DCP introduced a new policy, with child protection referrals being assigned as child concern reports if there was no indication of maltreatment, but concern was expressed over a child’s welfare.5 From 1 January 1990 to 31 December 2005, WA did not have mandatory reporting, but interagency protocols existed between the DCP and the Department of Health.6 For this study, we used the first child concern report, substantiation and notification for any individual child to identify trends.
Data sets were linked by the Western Australian Department of Health Data Linkage Branch by matching identifiers common to the sets of records (eg, name, address, etc).7 Only a unique project identifier and the individual’s clinical information was provided; identifying information was removed.
Children were considered to have had a hospital admission related to maltreatment if they had any of the following ICD-10 diagnostic codes recorded: T74, Y07.1–Y07.3, Y07.8, Y07.9. An assault-related admission was defined by ICD-10 codes: X85–Y09. As most maltreatment admissions also had a code of assault, maltreatment cases were only counted once and removed from assault cases. The distinction between these admissions is explained in detail in our previous work,8 and, based on this, common injuries and conditions associated with child maltreatment were assessed.8 Data on STIs only include children aged 2–13 years, born in WA between 1 January 1990 and 31 December 2005 and notified to the CDC.
Socioeconomic disadvantage was determined by the Index of Relative Social Disadvantage from the Australian Bureau of Statistics (ABS) using the birth registration and Midwives Notifications data.9 We assigned six levels of disadvantage to collection districts, ranging from 1 (least disadvantaged) to 6 (most disadvantaged).
Overall trends were calculated by the number of first child concern reports, notifications and substantiations for any individual child. Annual prevalence rates were calculated based on estimates of the child population using the Rates Calculator, version 9.1.5.10 Linked hospital and child protection data determined the proportion of children with an assault-related or maltreatment-related hospital admission, or a notified STI, with whom child protection agencies had become involved. Temporal relationships between admissions and notifications were examined. Specific injuries and conditions associated with child maltreatment were also assessed for their occurrence in children who had contact with the DCP. SAS, version 9.1 (SAS Institute Inc, Cary, NC, USA) was used for the analyses.
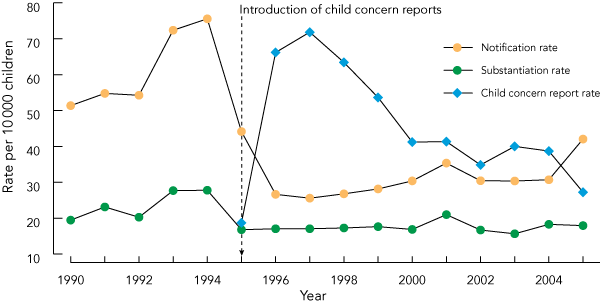
Between 1 January 1990 and 31 December 2005, there were 50 692 notifications with 19 207 of these substantiated. In the early years, there was a sharp increase in the rate of first notifications from 51 per 10 000 children in 1990 to 75 per 10 000 in 1994; this was followed by a decline in 1995 corresponding with the introduction of child concern reports (Box 1). The rate of child concern reports shows an initial increase in child concern reports, peaking in 1997, before falling over the next 5 years, and there was a small but steady increase in the rate of notifications. The substantiation rate followed a similar trend to that of notifications, increasing from 19 to 27 per 10 000 children between 1990 and 1994, and falling to 17 per 10 000 children in 1995; from then onward, the rate remained relatively stable.
Overall, 4% of children who had been notified to the DCP and 6.4% of those with a substantiated notification had a maltreatment-related hospital admission. A total of 604 children had at least one maltreatment-related admission, while 304 children had at least one assault-related admission (Box 2). Most children with maltreatment-related admissions were aged under 5 years and had been born into communities with higher levels of social disadvantage. Of the children who had an STI notification, over two-thirds were female, and half were born in areas of greater social disadvantage.
Most children with maltreatment-related admissions had contact with the DCP (90%), with 81% having at least one notification (Box 3). Over two-thirds of children had a substantiated notification, while half entered out-of-home care. Of the children who had an assault-related admission, 64% had contact with the DCP, more than half had a notification, 43% had a substantiation and 26% entered out-of-home care.
A total of 98 children aged under 14 years had an STI notification, with almost two-thirds having contact with the DCP (Box 3). Sixty per cent had been notified to the DCP, with over a third having a substantiated notification and 15% entering out-of-home care. When only the 35 cases from 2004 onwards were considered (after the establishment of an interagency protocol), 86% of children had been notified to the DCP, with 54% of those notifications being substantiated.
Of the 490 children admitted to hospital for maltreatment and who had been notified to the DCP (Box 3), 73% were reported directly after admission, usually within the first 4 days. In half of the 73% of cases that were reported after admission, this was the first notification for the children concerned, with hospital health care workers making 42% of the 490 notifications. Of the 413 cases that were substantiated, 68% were first substantiated notifications for the children concerned.
The strength of this study is that we used linked population-level data to facilitate the tracking of child protection outcomes, avoiding the bias introduced by relying on participation and recall by individuals. Researching such a sensitive issue is a challenge, but using de-identified data protects the privacy of research subjects. The study has limitations, as under-ascertainment may arise from the use of the diagnostic codes reported on the morbidity dataset to identify children with maltreatment-related and assault-related hospital admissions.11 Further, child maltreatment is only identified by notification to the DCP, and there may be children who have been maltreated but not reported. Also, it is highly likely that notification rates will be lower in WA than in other Australian states, as WA did not have mandatory reporting during the study period.
This study shows that the hospital system is identifying and reporting real cases of maltreatment, confirmed by the high proportion of substantiations. The widespread collection of morbidity data in many countries, with universal classification codes, creates opportunities to broaden child maltreatment surveillance and make valid comparisons over time and between jurisdictions.12 While cases that reach hospital are the tip of the iceberg, monitoring admissions for maltreatment is an important public health initiative.
1 Rates of child concern reports, child protection notifications and substantiations, 1 January 1990 to 31 December 2005*
 |
2 Characteristics of children born in Western Australia between 1 January 1990 and 31 December 2005 relating to hospital admissions for maltreatment and assault, and to notifications of sexually transmitted infections in the same period
Received 11 August 2009, accepted 13 April 2010
- Melissa O’Donnell1
- Natasha Nassar2,1
- Helen M Leonard1
- Richard P Mathews3
- Yvonne G Patterson4
- Fiona J Stanley1
- 1 Telethon Institute for Child Health Research, Centre for Child Health Research, University of Western Australia, Perth, WA.
- 2 Kolling Institute of Medical Research, University of Sydney, Sydney, NSW.
- 3 Disability Services Commission, Government of Western Australia, Perth, WA.
- 4 Department for Child Protection, Government of Western Australia, Perth, WA.
We acknowledge the partnership of the Western Australian Government Departments of Health, Child Protection, Education, Disability Services, Corrective Services and the Attorney General, which provided support as well as data for this project. This article does not necessarily reflect the views of the government departments involved in this research. Melissa O’Donnell was supported by an Australian Postgraduate Award Industry Scholarship, provided through an Australian Research Council Linkage Project Grant (LP0455417). Natasha Nassar is supported by a Public Health Fellowship (404198) from the National Health and Medical Research Council of Australia.
None identified.
- 1. Australian Institute of Health and Welfare. Child protection Australia 2006–07. Child welfare series no. 43. Canberra: AIHW, 2008. (AIHW Cat. No. CWS 31.) http://www.aihw.gov.au/publications/index.cfm/title/10566 (accessed Jun 2010).
- 2. O’Donnell M, Scott D, Stanley FJ. Child abuse and neglect — is it time for a public health approach? Aust N Z J Public Health 2008; 32: 325-330.
- 3. Guenther E, Knight S, Olson LM, et al. Prediction of child abuse risk from emergency department use. J Pediatr 2009; 154: 272-277.
- 4. Australian Institute of Health and Welfare. Child Protection Australia 2007–08. Child welfare series no. 45. Canberra: AIHW, 2008. (AIHW Cat. No. CWS 33.) http://www.aihw.gov.au/publications/index.cfm/title/10687 (accessed Jun 2010).
- 5. Parton N, Mathews R. New directions in child protection and family support in Western Australia: a policy initiative to re-focus child welfare practice. Child Family Soc Work 2001; 6: 97-113.
- 6. Department for Community Development. Reciprocal child protection procedures. Perth: DCD, 2002.
- 7. Kelman CW, Bass AJ, Holman CDJ. Research use of linked health data: a best practice protocol. Aust N Z J Public Health 2002; 26: 251-255.
- 8. O’Donnell M, Nassar N, Leonard H, et al. Monitoring child abuse and neglect at a population level: patterns of hospital admission for maltreatment and assault. Child Abuse Neglect 2010. In press.
- 9. Australian Bureau of Statistics. Socio-economic indexes for areas (SEIFA) — technical paper, 2006. Canberra: ABS, 2008. (ABS Cat. No. 2039.0.55.001.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/DetailsPage/2039.0.55.0012006?OpenDocument (accessed Jun 2010).
- 10. Codde J. Rates calculator, version 9.1.5. Perth: Department of Health, 2007.
- 11. Winn DG, Agran PF, Anderson CL. Sensitivity of hospitals’ e-coded data in identifying causes of children’s violence-related injuries. Public Health Rep 1995; 110: 277-281.
- 12. Zuckerbraun NS, Powell EC, Sheehan KM, et al. Community childhood injury surveillance: an emergency department-based model. Pediatr Emerg Care 2004; 20: 361-366.





Abstract
Objectives: To determine the extent to which children with a hospital admission related to assault or maltreatment or to a notified sexually transmitted infection (STI) have contact with the Western Australian Department for Child Protection (DCP), and to investigate injuries and conditions often associated with child maltreatment and subsequent contact with the DCP.
Design, participants and setting: Retrospective cohort study using de-identified, record-linked child protection and hospital morbidity data to identify all children aged 0–17 years in Western Australia between 1 January 1990 and 31 December 2005, and a subcohort of children born in WA between these dates, admissions of these children to public and private hospitals in WA, and their contact with the Western Australian DCP.
Main outcome measures: Annual trends in notifications and substantiations of child maltreatment; proportion of children with assault-related and maltreatment-related hospital admissions resulting in notifications, substantiations, or out-of-home care.
Results: Most children admitted for maltreatment-related reasons (90%) had contact with the DCP, with 81% of these children being notified, 68% having maltreatment substantiated, and 50% entering out-of-home care. Specific injuries and conditions were associated with children who had greater contact with the DCP, including retinal haemorrhage, rib fractures, multiple injuries, STIs at under 14 years of age, and malnourishment.
Conclusions: The health system effectively identifies and notifies real cases of maltreatment, and a high proportion of these are substantiated. Health data play an important role in improving maltreatment surveillance, providing opportunities to make valid comparisons over time and between jurisdictions, as well as to monitor conditions and injuries associated with child maltreatment.