The shortage of medical practitioners in rural and remote Australia has reached crisis proportions over the past decade.1,2 This shortage has resulted from government decisions to curb numbers in medical schools during the early 1990s, inadequate long-term medical workforce planning, changing expectations and preferences among recent medical graduates, loss of services in rural and remote communities throughout Australia, and a predominantly negative view of rural practice (and general practice). There is a perception that professional satisfaction is less likely to be achieved as a “rural” doctor. Consequently, recent medical graduates have been deterred from choosing a career in rural practice, and the delivery of medical services in rural areas has become dependent on international medical graduates, who are mandated to work in “areas of workforce shortage” for a period of time.3
Professional satisfaction, the extent to which a workplace matches what a worker aspires to or expects, is associated with individual and organisational outcomes and has important implications for medical workforce planning.4,5 Dissatisfaction results in increased stress and burnout, high turnover, difficulties with recruitment, poor quality of care, and ultimately significant costs to health services.6-8 The decision to take up and stay in a career, and to live in a particular location, reflects the perceived and actual satisfaction it generates.9
To date, there has been a lack of comprehensive evidence to counter the prevailing negative perspective of rural practice, other than a few studies based on small samples that failed to control adequately for the effect of geographical variation.10-12 We therefore investigated whether the level of professional satisfaction of Australian general practitioners varies according to community size and location. Our study used a cohort drawn from the entire GP population of Australia, enabling testing of associations beyond the rural–urban dichotomy.
We used data from the Medicine in Australia: Balancing Employment and Life (MABEL) study, the largest longitudinal survey of the Australian medical workforce. The primary aim of the MABEL study is to investigate labour supply decisions and their determinants among Australian doctors.13 MABEL is currently funded to undertake four annual waves of data collection. The results presented here are based on the first wave conducted between June and November 2008. A brief overview of the MABEL questionnaire is given in Box 1, and further details of survey administration have been reported elsewhere.13
MABEL was approved by the University of Melbourne Faculty of Economics and Commerce Human Ethics Advisory Committee (Ref. 0709559) and the Monash University Standing Committee on Ethics in Research Involving Humans (Ref. CF07/1102 - 2007000291).
The full MABEL Wave 1 cohort (n = 10 498; response rate, 19.36%) was self-selected from the entire Australian medical workforce (N = 54 750). As the number of doctors practising in remote and very remote areas is small, a financial incentive ($100 honorarium) was offered to maximise response rates for this group. A detailed examination of possible non-response bias was made based on sex, age, doctor type, the Australian Standard Geographical Classification (ASGC) Remoteness classification15 and hours worked.16 Compared with the national population of doctors, the Wave 1 cohort slightly under-represented older doctors (aged over 60 years), over-represented women by six percentage points, under-represented GPs by four percentage points, and closely matched the distribution of hours worked.13
Here, we report results for GPs and GP registrars only (referred to collectively as GPs).
Satisfaction was measured using three sets of items. First, professional satisfaction was measured using 10 items from the Warr–Cook–Wall job satisfaction questionnaire on a five-level scale.17 For this report, the two positive responses (“very satisfied” and “moderately satisfied”) were grouped and compared against the two negative responses (“moderately dissatisfied” and “very dissatisfied”).
Because geographical differentiation was a key aspect of this study, initial results were examined using the ASGC Remoteness classification15 and various population size categories, using responding doctors’ self-identified main place of work. Our testing found that the use of community population size was significantly more sensitive for detecting patterns of geographical differences within the data. A major weakness of the ASGC Remoteness classification is the extreme heterogeneity characterising each class, particularly within the “inner regional” and “outer regional” categories.18 To overcome this problem, the data were examined using a 10-level community size scale. These results indicated that a reduced five-level community size scale provided sufficient sensitivity to capture differences between “like” and “unlike” classes: (1) very small rural, < 2500 residents; (2) small rural, 2500–9999 residents; (3) medium–large rural, 10 000–49 999 residents; (4) regional centre, 50 000–999 999 residents; and (5) metropolitan, ≥ 1 million residents. Box 2 provides a breakdown of the number of Wave 1 GP respondents in each category.
Responses were received from 3906 GPs (response rate, 17.65%). Selected characteristics of the cohort in the five community size groups are shown in Box 3.
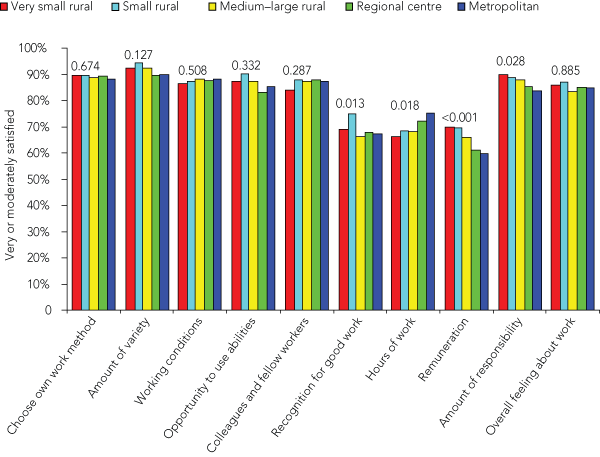
When comparing GPs across the five community size categories, professional satisfaction was not statistically different for most aspects of the job (Box 4). GPs’ overall satisfaction with their work was high (about 85%) and nearly identical for all community sizes (P = 0.885). Professional satisfaction of all GPs was generally high, with seven of the 10 items rating well above 80% satisfaction irrespective of community size. Remuneration was the only aspect with a statistically significant difference, with GPs in smaller communities expressing higher satisfaction (P < 0.001). GPs in smaller communities were also slightly more satisfied with the amount of responsibility they have and recognition they get for good work. Satisfaction with hours of work decreased with decreasing community size, but this association was not statistically significant (P = 0.018).
Multivariate logistic regression analysis confirmed the observed increased satisfaction of GPs working in smaller communities with remuneration, amount of responsibility and, to a lesser degree, opportunities to use their abilities, amount of variety, and freedom to choose their work method (Box 5).
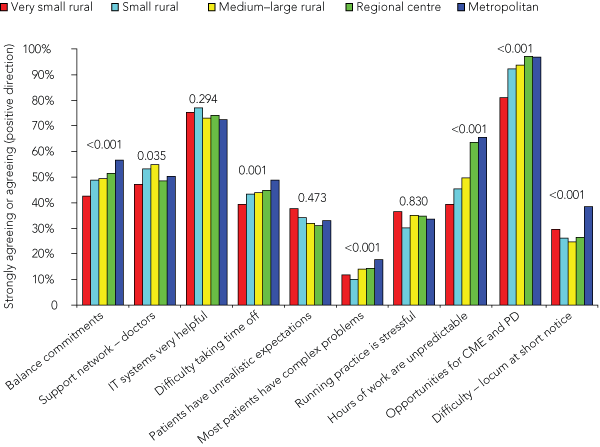
The level of agreement of GPs with statements regarding aspects associated with their job showed more statistically significant variation by community size (Box 6). The strongest negative association with smaller community size was the increased unpredictability of the number of hours worked (P < 0.001); about 65% of metropolitan GPs did not think that their hours were unpredictable, compared with 40% of GPs in very small rural communities. Differences in opportunities for continuing medical education (CME) and difficulty in arranging locums at short notice were both statistically significant (P < 0.001). Just over 80% of GPs from very small rural locations reported that opportunities for CME were good, compared with more than 90% in all other community sizes. Less than 40% of GPs in all community sizes did not have difficulty arranging a locum at short notice, with a small increase only for metropolitan areas. The majority of GPs (> 70%) in all locations found their information technology systems helpful, although around 65% also found running their practice stressful.
Multivariate logistic regression confirmed the association between smaller community size and difficulties with unpredictability of hours, opportunities for CME, and short-notice access to locums (Box 7). A small majority of GPs in rural locations reported difficulty with taking time off and balancing personal and work commitments, with a minor increase in difficulties seen in smaller rural areas (P < 0.001), although no geographic pattern was observed for either of these aspects after adjusting for covariates.
GPs in regional centres had the highest levels of positive response (66%–94%) to statements about non-professional location characteristics, closely followed by GPs in metropolitan areas, with a significant drop of 20–40 percentage points as the community size dropped below 50 000 residents (Box 8). The level of agreement with these items was strongly statistically associated with community size (P < 0.001).
In the absence of any “gold standard” to indicate which job aspects should be considered to capture professional satisfaction outcomes, the choice of measurement instrument and methodology has important implications.14,19 Clearly, it is unlikely that the overall satisfaction and contentment of the rural GP is determined solely by the 20 professional satisfaction aspects considered here, although the literature indicates they are sentinel considerations.4-8,14 A doctor’s decision to stay in or leave rural practice may reflect other non-professional considerations associated with the ability of a location to meet the needs of particular stages of the life cycle. Our study found that satisfaction with six important non-professional aspects dropped significantly as a location’s population dropped below 50 000. However, it is difficult to determine the relative importance of these non-professional factors. It is also unclear to what extent self-selection into rural practice, rather than characteristics of the rural environment or the job, contributes to high professional satisfaction. Additionally, while no serious response bias was demonstrated on observed variables in our study, we acknowledge that differences in unobserved characteristics may bias responses for some survey questions on professional satisfaction.20 Notwithstanding these potential limitations, the fact that our large study cohort relates to a population rather than a sample, and the representativeness of its respondents, provides strong empirical evidence for generalisation of our results.
Despite a range of government incentives,21 relatively little progress has been made in increasing the number of Australian medical students taking up practice in rural communities. Rural medical practice is often presented negatively, with many reports and research studies highlighting overworked, under-remunerated and undervalued rural doctors struggling to deal with sicker patients in communities characterised by chronic workforce shortages.1,12,22,23 This poor “marketing” of rural medicine as a career choice, combined with students’ and some metropolitan GPs’ apprehensions about their own competence and confidence to work long hours in relative isolation in rural communities and a fear of professionally “missing out” compared with big-city doctors, makes recruitment of the rural medical workforce extremely difficult.24,25 The importance of disseminating positive information to counterbalance negative stereotypes has previously been highlighted.22
To date, there has been limited and often reactive promotion of the benefits of being a rural doctor, a career that, as our study shows, can combine high levels of professional satisfaction with other lifestyle advantages. At the same time, significant resources continue to be invested in rural components of training for Australian doctors, including increased selection of rural-origin students into training programs, increased exposure to rural practice for all medical students, increased training of medical students wholly in rural locations, and increased places for postgraduate training in rural locations,21 where it is hoped that students will discover the fulfilment of living and working in a rural area. With the possible exception of selecting rural-origin students,26 there is little evidence that these programs have made any significant difference to the chronic medical workforce shortage in rural areas.26,27 Our findings indicate there is greater scope to promote rural practice as a highly satisfying professional career path.
1 MABEL study Wave 1 questionnaire
All items were thoroughly pilot tested, and satisfaction items were modelled on previous scales.14
The MABEL questionnaires are available at <https://mabel.org.au/mabelq.html>.
MABEL = Medicine in Australia: Balancing Employment and Life.
2 Wave 1 general practitioner respondents (n = 3906),* by community size and ASGC Remoteness classification categories
ASGC = Australian Standard Geographical Classification. * Location data missing for 31 respondents. |
|||||||||||||||
5 Odds ratios (95% CI) from multivariate logistic regression for general practitioners reporting satisfaction with various aspects of their work*
7 Odds ratios (95% CI) from multivariate logistic regression for positive responses* of general practitioners to statements regarding professional aspects of work†
- Matthew R McGrail1,2
- John S Humphreys2
- Anthony Scott3
- Catherine M Joyce4
- Guyonne Kalb3
- 1 Gippsland Medical School, Monash University, Churchill, VIC.
- 2 School of Rural Health, Monash University, Bendigo, VIC.
- 3 Melbourne Institute of Applied Economic and Social Research, University of Melbourne, Melbourne, VIC.
- 4 Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
This work, part of the MABEL study, was supported by a National Health and Medical Research Council Health Services Research Grant (454799) and by the Australian Government Department of Health and Ageing. The views in this paper are ours alone. Thanks to the other members of the MABEL team for their support and input.
None identified.
- 1. Australian Government Department of Health and Ageing. Report on the audit of health workforce in rural and regional Australia, April 2008. Canberra: Commonwealth of Australia, 2008.
- 2. Productivity Commission. Australia’s health workforce: research report. Canberra: Productivity Commission, 2005.
- 3. Birrell B, Hawthorne L. Medicare Plus and overseas-trained medical doctors. People Place 2004; 12: 83-98.
- 4. Buchbinder SB, Wilson M, Melick CF, Powe NR. Primary care physician job satisfaction and turnover. Am J Manag Care 2001; 7: 701-713.
- 5. Konrad TR, Williams ES, Linzer M, et al. Measuring physician job satisfaction in a changing workplace and a challenging environment. Med Care 1999; 37: 1174-1182.
- 6. Pathman DE, Konrad TR, Williams ES, et al. Physician job satisfaction, job dissatisfaction, and turnover. J Fam Pract 2002; 51: 593.
- 7. Pathman DE, Williams ES, Konrad TR. Rural physician satisfaction: its sources and relationship to retention. J Rural Health 1996; 12: 366-377.
- 8. Williams ES, Konrad TR, Scheckler WE, et al. Understanding physicians’ intentions to withdraw from practice: the role of job satisfaction, job stress, mental and physical health. Health Care Manage Rev 2001; 26: 7-19.
- 9. General Practice Education and Training. If the job fits ... the complexity of medical career decision making: a review. Canberra: GPET, 2007.
- 10. Lepnurm R, Dobson R, Backman A, Keegan D. Factors associated with career satisfaction among general practitioners in Canada. Can J Rural Med 2007; 12: 217-230.
- 11. Luman K, Zweifler J, Grumbach K. Physician perceptions of practice environment and professional satisfaction in California: from urban to rural. J Rural Health 2007; 23: 222-228.
- 12. Ulmer B, Harris M. Australian GPs are satisfied with their job: even more so in rural areas. Fam Pract 2002; 19: 300-303.
- 13. Joyce CM, Scott A, Jeon SH, et al. The “Medicine in Australia: Balancing Employment and Life (MABEL)” longitudinal survey — protocol and baseline data for a prospective cohort study of Australian doctors’ workforce participation. BMC Health Serv Res 2010; 10: 50.
- 14. Lichtenstein R. Measuring the job satisfaction of physicians in organized settings. Med Care 1984; 22: 56-68.
- 15. Australian Bureau of Statistics: ASGC remoteness classification: purpose and use. Census Paper No. 03/01. Canberra: ABS, 2003.
- 16. Groves RM, Peytcheva E. The impact of nonresponse rates on nonresponse bias: a meta-analysis. Public Opin Q 2008; 72: 167-189.
- 17. Warr P, Cook J, Wall T. Scales for the measurement of some work attitudes and aspects of psychological well-being. J Occup Psychol 1979; 52: 129-148.
- 18. McGrail MR, Humphreys JS. Geographical classifications to guide rural health policy in Australia. Aust New Zealand Health Policy 2009; 6: 28.
- 19. van Saane N, Sluiter JK, Verbeek JHAM, Frings-Dresen MHW. Reliability and validity of instruments measuring job satisfaction — a systematic review. Occup Med (Lond) 2003; 53: 191-200.
- 20. Gravelle H, Hole AR, Hossain MI. Response bias in job satisfaction surveys: English general practitioners. Discussion papers in economics no. 2008/24. York: University of York, 2008.
- 21. Australian National Audit Office. Rural and remote health workforce capacity — the contribution made by programs administered by the Department of Health and Ageing. Canberra: ANAO, 2009.
- 22. Peach HG. Badmouthing between disciplines. Aust Fam Physician 1999; 28: 581.
- 23. Australian Institute of Health and Welfare. Rural, regional and remote health: indicators of health. Rural health series no. 5. Canberra: AIHW, 2005. (AIHW Cat. No. PHE 59.)
- 24. Joyce CM, McNeil JJ. Fewer medical graduates are choosing general practice: a comparison of four cohorts, 1980–1995. Med J Aust 2006; 185: 102-104. <MJA full text>
- 25. Thistlethwaite JE, Leeder SR, Kidd MR, Shaw T. Addressing general practice workforce shortages: policy options. Med J Aust 2008; 189: 118-121. <MJA full text>
- 26. Wilson NW, Couper ID, De Vries E, et al. A critical review of interventions to redress the inequitable distribution of healthcare professionals to rural and remote areas. Rural Remote Health 2009; 9: 1060.
- 27. Ranmuthugala G, Humphreys J, Solarsh B, et al. Where is the evidence that rural exposure increases uptake of rural medical practice? Aust J Rural Health 2007; 15: 285-288.





Abstract
Objective: To investigate whether the level of professional satisfaction of Australian general practitioners varies according to community size and location.
Design, setting and participants: Cross-sectional, population-level national survey using results for a cohort of 3906 GPs (36% were “rural” participants) from the first wave of a longitudinal study of the Australian medical workforce, conducted between June and November 2008. Geographical differences in levels of professional satisfaction were examined using five community size categories: metropolitan, ≥ 1 million residents; regional centre, 50 000–999 999; medium–large rural, 10 000–49 999; small rural, 2500–9999; and very small rural, < 2500.
Main outcome measures: Level of professional satisfaction expressed by GPs working in different sized communities with respect to various job aspects.
Results: Professional satisfaction of GPs did not differ by community size for most aspects of the job. Overall satisfaction was high, at about 85% across all community sizes. Satisfaction with remuneration was slightly higher in smaller rural towns, even though the hours worked there were less predictable. Professional satisfaction with freedom of choosing work method, variety of work, working conditions, opportunities to use abilities, amount of responsibility, and colleagues was very high across all community sizes, while difficulties with arranging locums and the stress of running the practice were commonly reported by GPs in all community sizes.
Conclusions: GPs working in different sized communities in Australia express similar levels of satisfaction with most professional aspects of their work.