There is concern that interest in a career in general practice is declining among recent Australian medical graduates, but relatively few data are available on the extent of this trend. Places in the general practice vocational training program have not been filled in 4 of the past 6 years, and future shortages in the general practice workforce have been predicted.1 This trend is not confined to Australia; it has also been observed in the United Kingdom2 and Canada.3
We studied four cohorts of Australian medical graduates (the Monash Medical Graduates Survey) with the aim of investigating workforce participation patterns.4 Data from the survey published previously indicated that, on average, around 10% of each cohort was lost from the Australian medical workforce by 5 years after graduation, rising to 15% by 10 years, then rebounding slightly to 12% by 15 years after graduation.4 Here, we document changes in career choices likely to have an impact on the future general practice workforce.
A total of 386 graduates participated in the survey, representing a response rate of 69%. Response rates by cohort were: 1980, 72%; 1985, 65%; 1990, 73%; and 1995, 66%. The study methods have been reported in more detail in our previous article.4
Characteristics of the final sample of participants are given in Box 1. As previously reported,4 there was some over-representation of women in the study sample for the 1985 cohort, and some over-representation of graduates practising or registered to practise in Australia in the 1980 and 1995 cohorts.
Occupation at the time of the survey is shown for each cohort in Box 2. This indicates higher proportions of graduates currently in general practice in the earlier cohorts (1980 and 1985) compared with the later ones (1990 and 1995). The proportions of graduates in specialist medicine show the opposite trend. Very few graduates were not in the medical labour force — 6% in the 1985 cohort and 2% in the other three.
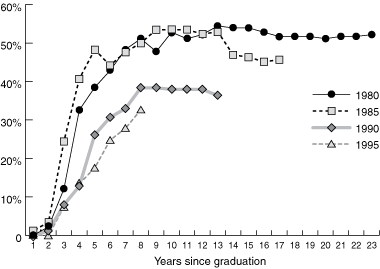
The proportion of graduates in each cohort working in general practice by years since graduation is shown in Box 3. These data take into account differences between cohorts in number of years since graduation by comparing employment at the same time relative to year of graduation. The longest period for which there are data on all cohorts is 8 years after graduation. At this point, 51% of 1980 graduates and 50% of 1985 graduates were working in general practice, compared with 38% of 1990 graduates and 33% of 1995 graduates, indicating a significant drop in pursuit of general practice careers (n = 360; χ23 = 9.25, P < 0.05). Individual comparisons showed that while the proportion in the 1995 cohort was significantly lower than that in the 1980 cohort (odds ratio [OR], 0.46; 95% CI, 0.26–0.84), the difference between the 1980 and the 1990 cohorts was not significant (OR, 0.59; 95% CI, 0.33–1.08).
Box 3 also shows that more recent graduates entered the general practice workforce at a later stage in their careers than earlier cohorts. At 4 years after graduation, for example, the proportion of each cohort working in general practice was: 33% (1980), 41% (1985), 13% (1990) and 13% (1995).
The proportion of males in each cohort working in general practice was around 30%–40%, but there was a notable fall in the number of female graduates making a career in general practice (Box 4). While the interaction between cohort and sex was not significant (OR, 1.05; 95% CI, 0.97–1.13), a significant decrease across the cohorts in the proportion of women working in general practice was observed (OR, 0.92; 95% CI, 0.87–0.97).
The finding that more recent graduates entered the general practice workforce later than previous cohorts is likely to reflect the increasing formalisation of the early postgraduate years occurring from the mid 1990s. The first national guidelines for intern training were produced in 1996, and the Confederation of Postgraduate Medical Education Councils was established in 1998.6,7 This is reflected in our findings that 24% of the 1980 and 1985 cohorts were working in hospital non-specialist medicine 4 years after graduation, compared with 29% of the 1990 and 35% of the 1995 cohorts.
Several factors have been put forward to explain why recent graduates may be less attracted to general practice. Graduates increasingly appear to perceive general practice as less prestigious than other specialties.8 This may be related to the higher profile of technological and scientific advancements in other specialties, or a view of general practice as offering less remuneration and being less challenging. Findings from a study of Australian vocational trainees support this view, noting that “intellectual content of the specialty” was a significantly less important factor in the choice of specialty by general practice trainees compared with other specialist trainees.9 Reports of low morale, high workload, heavy administrative burden, and poor job satisfaction among Australian GPs are also likely to have a negative influence on new graduates’ career choices.10
Imposition of a cap of 400 places in the GP training program (1995), greatly reducing the annual intakes, from over 800 in the early 1990s.11
Introduction of compulsory vocational registration for GPs (1995), thus making postgraduate training required for new graduates to become a GP.
Tightening of training program entry requirements, so that a minimum number of postgraduate years of experience were required before entry.
Introduction of compulsory rural placements during GP training (late 1990s).
These changes meant that the pathway into a general practice career came into much closer alignment with that into other specialist medical careers, and the decision to become a GP required more investment than before. The increased competitiveness and heightened training requirements may have tipped the balance for female graduates, when these were considered alongside perceived positives and negatives of a range of medical specialties. Compulsory rural placements may have been particularly salient for women.12
While general practice fits well with female doctors’ career requirements (such as the opportunity to work flexibly and consideration of their domestic circumstances9), this is also true of other medical specialties. In the two most recent cohorts in our survey, female graduates moved into specialties such as emergency medicine, psychiatry, geriatrics and paediatrics.
Are our findings specific to graduates of Monash University? A study of 1990 graduates from the two South Australian medical schools found that, at 12 years after graduation, 47% were working in general practice, compared with 33% of the Monash cohort graduating in the same year.13 Differences between medical schools in graduates’ career preferences have been observed in the UK, and may relate to differences in selection processes, emphasis on specialties at medical school, and impressions conveyed to students about careers in various specialties.14 Such variations are likely to also exist between medical schools in Australia.
Our findings have implications for the future sustainability of the current Australian health care model, with the central role of the GP. If present trends continue, the shortage of GPs is less and less likely to be resolved with Australian trainees. Efforts must be made to improve the attractiveness of general practice careers. More effective marketing may be part of the solution, highlighting the opportunities to work flexibly, which appeals to more recent graduates.9,15
Another strategy might be that proposed by the recent Productivity Commission report, which would see GPs delegating some of their more routine tasks to assistants, thus allowing them to focus on the more challenging and interesting parts of their work.16
1 Demographic and background characteristics of participants in each cohort
* Citizenship data missing for one case in the 1985 cohort. † Age data missing for one case in each of the 1980, 1990 and 1995 cohorts. |
|||||||||||||||
- Catherine M Joyce1
- John J McNeil2
- Department of Epidemiology and Preventive Medicine, Monash University, Melbourne, VIC.
Our study was supported by an NHMRC Primary Health Care Research Postgraduate Scholarship to Catherine Joyce, and a Project Grant from the Australian Government Department of Health and Ageing. Thanks to the Alumni Office of Monash University Faculty of Medicine, Nursing and Health Sciences for their assistance, and to the participating medical graduates.
None identified.
- 1. Australian Medical Workforce Advisory Committee. The general practice workforce in Australia: supply and requirements to 2013. AMWAC Report 2005.2. Sydney: AMWAC, 2005. Available at: http://www.health.nsw.gov.au/amwac/pdf/gp_summary.pdf (accessed Jun 2006).
- 2. Lambert TW, Evans J, Goldacre M. Recruitment of UK-trained doctors into general practice: findings from national cohort studies. Br J Gen Pract 2002; 52: 364-371.
- 3. Sullivan P. Family medicine loses lustre as students vote with their feet in 2001 residency match. CMAJ 2001; 164: 1194.
- 4. Joyce CM, McNeil JJ. Participation in the workforce by Australian medical graduates. Med Educ 2006; 40: 333-339.
- 5. Australian Institute of Health and Welfare. Medical labour force 2001. Canberra: AIHW, 2003. (AIHW Catalogue No. HWL 28; ABS Catalogue No. 8908.0.) Available at: http://www.aihw.gov.au/publications/index.cfm/title/9529 (accessed Jun 2006).
- 6. Australian Government Department of Health and Ageing. National training and assessment guidelines for junior medical doctors PGY 1 & 2. Revised national guidelines for the training and assessment of junior medical doctors. Canberra: The Department, 2003. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-workforce-new-jmonatgui.htm (accessed May 2006).
- 7. Australian Government Department of Health and Ageing. Medical Training Review Panel — ninth report. Canberra: The Department, 2005. Available at: http://www.health.gov.au/internet/wcms/publishing.nsf/Content/health-workforce-education-mtrp9thr.htm (accessed Jun 2006).
- 8. Lambert T, Evans J, Goldacre M. Attitudes towards general practice are changing. BMJ 2002; 324: 1456.
- 9. Harris MG, Gavel PH, Young JR. Factors influencing the choice of specialty of Australian medical graduates. Med J Aust 2005; 183: 295-300. <MJA full text>
- 10. Chew M, Williams A. Australian general practitioners: desperately seeking satisfaction. Med J Aust 2001; 175: 85-86. <MJA full text>
- 11. Birrell B. Implications of controls on access to Medicare billing for GPs. People Place 1997; 5: 67-77.
- 12. Commonwealth Department of Health and Family Services. Trainee selection in Australian medical colleges. Canberra: AGPS, 1998.
- 13. Laven G, Newbury J, White M, et al. A longitudinal cohort study of South Australian final year medical students 1990-2002. Proceedings of the General Practice and Primary Care Research Conference; 2002 May 30–31; Melbourne, VIC. Available at: http://www.phcris.org.au/conference/2002/index.php (accessed Jun 2006).
- 14. Goldacre MJ, Turner G, Lambert TW. Variation by medical school in career choices of UK graduates of 1999 and 2000. Med Educ 2004; 38: 249-258.
- 15. Dorsey ER, Jarjoura D, Rutecki GW. Influence of controllable lifestyle on recent trends in specialty choice by US medical students. JAMA 2003; 290: 1173-1178.
- 16. Australian Government Productivity Commission. Australia’s health workforce. Research report. Canberra: Productivity Commission, 2005. Available at: http://www.pc.gov.au/study/healthworkforce/finalreport/healthworkforce.pdf (accessed Jun 2006).





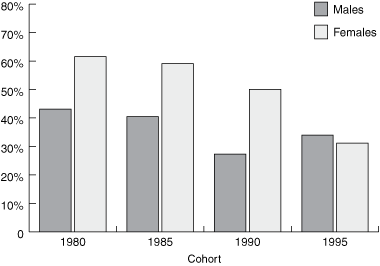
Abstract
Objective: To compare general practice career choices of four cohorts of medical graduates.
Design and setting: Retrospective longitudinal study of medical graduates. Data on employment since graduation, nature of current employment, and postgraduate qualifications were collected by postal survey in 2003.
Participants: Four cohorts of Monash University Medical School graduates who completed their degrees in 1980, 1985, 1990 and 1995 (n = 386).
Main outcome measure: Proportion of each cohort pursuing a general practice career.
Results: At 8 years after graduation, half of the graduates in the 1980 and 1985 cohorts were working in general practice, compared with 38% of 1990 graduates and 33% of 1995 graduates. Differences were mainly attributable to fewer female graduates working as GPs: female GPs comprised 62% of the 1980 cohort compared with 31% of the 1995 cohort. Graduates in more recent cohorts also entered the general practice workforce at a later stage than those in earlier cohorts.
Conclusion: A rapidly declining proportion of new graduates from Monash University Medical School, particularly female graduates, are choosing general practice as a career. This will exacerbate future shortages in the general practice workforce.