In March 2009, the Australian Government Department of Health and Ageing issued the terms of reference for an external review of health technology assessment (HTA) agencies in Australia. The review aimed to simplify and achieve better coordination between HTA processes, as well as strengthen transparency and procedural fairness in assessment, decision making and fee negotiation arrangements. Submissions closed in May 2009, with 86 submissions received. Despite the potential of this review to have a major effect on the availability of new procedures and medical technology for use by the medical profession, only about 15% of the submissions came from “medical associations”. The HTA Review’s final report was released in February 2010.1
This article, based on a submission to the HTA Review, focuses on the two HTA agencies responsible for funding medical procedures and medical technology in Australia: the Medical Services Advisory Committee (MSAC) and the Prostheses and Devices Committee (PDC). The role of the National Theatre Banding Committee, not covered by the HTA Review, is also discussed. The overall effectiveness of these agencies in terms of a number of key performance objectives is evaluated, and some of the main concerns with the current process and evidence requirements are highlighted. I argue that the risk of a Type II error2 — recommending against funding for medical procedures or devices that should be funded, based on a finding of “insufficient evidence” from a full-scale HTA — may be reduced by a number of process changes and a move towards more pragmatic evidence requirements.
Medical and pharmaceutical technologies have more differences than similarities (Box 1), and these differences may have important implications for how medical technology is evaluated, both clinically and economically, compared with pharmaceuticals. Campbell points out that there are a number of statistical issues that are unique to evaluations of medical devices compared with pharmaceuticals.3 These issues include: the impossibility of masking or blinding patients and investigators in some instances; the fact that surgeons often differ in their abilities and, for many procedures, the surgeon improves with experience; the clinical end point is often evaluated over many time points, underlining the importance of repeated measures analyses and longitudinal techniques; and changes to the protocol or even to the device may occur while the confirmatory trial is being conducted. The companies that make medical devices also differ from pharmaceutical firms in both size and number.3 While pharmaceutical companies tend to be large, the median size of a medical device company in the United States is less than 50 people. However, in contrast to the relatively few pharmaceutical firms, there are many thousands of US medical device firms. In 2006, worldwide sales of medical devices were estimated to be $220 billion, while sales of prescription medicines were much larger, estimated at $643 billion.
Ramsey and colleagues add to this list of differences.4 There are inherent constraints when designing device trials to prove efficacy — the large-scale, blinded, randomised, placebo-controlled trials common in drug studies are often extremely difficult or unrealistic to perform for medical devices, particularly surgically implantable devices. Most device trials also have limited patient recruitment capacity — unlike drugs, devices typically have small numbers of potential end users and even fewer eligible clinical trial candidates. Another common limiting factor is that many devices require specialised training or skills to install or monitor them. Important device-related outcomes often require years of follow-up observation and even clinically useful intermediate end points are often unavailable. Finally, separating the efficacy of a procedure from the efficacy of the device is an important and often troublesome issue for device evaluations.4
Although Box 1 is based on broad generalisations, it illustrates the key important differences and why medical technology may require a uniquely designed evaluation process rather than a modified pharmaceutical evaluation process.
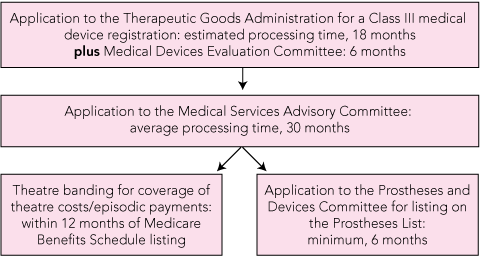
For a new medical procedure to be listed on the Australian Medicare Benefits Schedule (MBS), an application must be made to MSAC for an HTA. Almost without exception, the need for an MSAC HTA is identified by the application sponsor rather than by the horizon scanning process that was introduced in 2004 with the aim of identifying new and emerging technology.5 All medical devices associated with the new procedure require Therapeutic Goods Administration (TGA) registration before the application for the procedure can be lodged with MSAC. In order to list an implantable prosthesis on the Prostheses List (previously known as Schedule 5) for funding, it must be both registered by the TGA (excluding exempt items such as human tissue) and be part of a medical procedure listed on the MBS. “Theatre banding” is the funding process used to cover the associated theatre costs of the new medical procedure, but a theatre band will only be allocated by the National Theatre Banding Committee once the procedure is listed on the MBS. This sequential funding evaluation process for new medical procedures and associated medical devices is illustrated in Box 2.
The duration of processing MSAC applications from the month of lodgement until the month of listing on the MBS (positive recommendations only) is shown in Box 3. In an attempt to capture the most current average processing time, this table only includes applications lodged in the second half of the decade covered by MSAC (2004–2009). The average duration from lodgement to listing through the MSAC process is just over 30 months (range, 19–48 months). Although it is difficult to discern a pattern, new MBS item numbers that will potentially have a low annual number of claims appear to be processed faster. Such applications include: SIR-Spheres for the treatment of non-resectable liver tumours (280 claims in 2008–09); double balloon enteroscopy (367 claims in 2008–09); capsule endoscopy for Peutz–Jeghers syndrome (only three claims in 2008–09); endoscopic ultrasound and fine needle aspiration for lung cancer (39 claims for half the financial year 2008–09); and sacral nerve stimulation for faecal incontinence (16 claims in 2008–09).6 These calculations of processing durations appear to contradict the average reported time frame of 18 months from lodgement to listing through the MSAC process.7
Based on the average MSAC processing time of 30 months and the 24 months needed by the TGA to process a Class III (high-risk) medical device, the sequential funding evaluation process, with no overlap or parallel processing, can result in total processing times approaching 5 years (Box 2). Often these medical devices have already been approved by the US Food and Drug Administration (FDA) and received European conformity (CE) marking. The processing time for new medical procedures with already FDA-approved and CE-marked Class III medical devices could be halved if the MSAC application was processed in parallel with the application to the TGA, and the evaluation of implantable prostheses was incorporated into the MSAC HTA.
At pre-lodgement meetings with sponsors of MSAC applications, the Health Technology and Medical Services Group of the Medical Benefits Division (Department of Health and Ageing) does not provide guidance on the evidence requirements for the new procedure’s HTA. The probability of MBS listing of medical procedures is indicated in Box 4, which gives a summary of all known outcomes of applications to MSAC as of June 2009. This shows that less than one in four applications resulted in permanent funding for the full indication applied for by the application’s sponsor. The most common reason for not recommending funding was “insufficient” clinical evidence, although more recently lack of proven cost-effectiveness has also been cited. These results indicate that a preliminary outline of the minimal requirements for evidence demonstrating safety, efficacy and effectiveness of the proposed medical procedure needs to be provided at these pre-lodgement meetings.
The most recent minutes of a meeting held by MSAC that are publicly available on the Committee’s website are those of the 41st meeting, held on 7 March 2008.8 Updates on the progress of applications can also be slow. For instance, the MSAC website lists Application 1139, lodged in April 2009, but in October 2009, 6 months after lodgement, it still gave no details of the Advisory Panel for this application.
The PDC does not provide minutes of its meetings but issues bulletins on an irregular basis. Bulletin Number 27 was issued in October 2008, Bulletin Number 28 in April 2009 and Bulletin Number 29 in July 2009.9 This is in contrast to the total of eight PDC meetings held between January and July 2009.
Up until 2005, listing of a prosthesis on the Prostheses List meant full funding by private health insurers, with no gap fee paid by the patient. However, data derived from PDC Bulletins show that between 2005 and February 2009, the proportion of technologies listed with “gap” benefits rose to 18.5%.10 In many cases, this was the result of the applicant’s inability to satisfy the PDC’s clinical evidence requirements. The validity of these evidence requirements needs to be investigated.
Single-use consumables and disposables are perhaps the best example of the funding perverse incentive when compared with prostheses. In November 2006, a new MBS item (number 38241) was listed for the use of a coronary pressure wire during selective coronary angiography.11 Despite the evidence showing a clear advantage in the use of this equipment, use of the MBS item number shows that uptake of this procedure has been slow, because of a lack of coverage for the equipment. There is no “equipment list” operating in a similar way to the Prostheses List, and the current theatre banding is not designed to cover “high-cost” equipment.
The risk of a Type II error (not recommending funding for a procedure or medical device that should be funded due to a conclusion from a full-scale HTA of “insufficient evidence”) could be reduced by a number of changes to processes and evidence requirements of Australian HTA agencies, especially those relating to MSAC and the PDC. The recommendations of the HTA Review1 and the resulting changes to the way our HTA agencies process applications and assess evidence for the funding of medical technology need to be closely monitored by the medical profession, as well as by the medical devices industry.
3 Durations from lodgement to listing of Medical Services Advisory Committee (MSAC) applications, March 2004 – March 2009*
- Susanne P O’Malley1
- Medical Intelligence, Sydney, NSW.
Medical Intelligence is an independent consultancy specialising in reimbursement strategies and submissions for medical technology. Data for this article were compiled as part of a Doctorate of Business Administration by publication at Macquarie Graduate School of Management. No financial support was provided from any source for the writing of this article.
- 1. Australian Government Department of Health and Ageing. Review of health technology assessment in Australia December 2009. Canberra: DoHA, 2009. http://www.health.gov.au/internet/main/publishing.nsf/Content/hta-review (accessed May 2010).
- 2. O’Malley SP. The Australian experiment: the use of evidence based medicine for the reimbursement of surgical and diagnostic procedures (1998–2004). Aust New Zealand Health Policy 2006; 3: 3.
- 3. Campbell G. Statistics in the world of medical devices: the contrast with pharmaceuticals. J Biopharm Stat 2008; 18: 4-19.
- 4. Ramsey SD, Luce BR, Deyo R, Franklin G. The limited state of technology assessment for medical devices: facing the issues. Am J Manag Care 1998; 4: SP188-SP199.
- 5. O’Malley SP, Jordan E. Horizon scanning of new and emerging medical technology in Australia: its relevance to Medical Services Advisory Committee health technology assessments and public funding. Int J Technol Assess Health Care 2009; 25: 374-382.
- 6. Medicare Australia. MBS Item statistics reports. https://www.medicareaustralia.gov.au/statistics/mbs_item.shtml (accessed Jan 2010).
- 7. Australian Government Department of Health and Ageing. Review of health technology assessment in Australia — a discussion paper. Appendix C — Current HTA process in Australia. Canberra: DoHA, 2009. http://www.health.gov.au/internet/main/publishing.nsf/Content/htadiscussionpaper.htm#appendixc (accessed Jun 2009).
- 8. Medical Services Advisory Committee. Minutes of previous meetings. http://www.health.gov.au/internet/msac/publishing.nsf/Content/minutes-1 (accessed May 2010).
- 9. Australian Government Department of Health and Ageing. Prostheses and Devices Committee (PDC). http://www.health.gov.au/internet/main/ publishing.nsf/Content/health-privatehealth-providers-prosths.htm (accessed Jun 2009).
- 10. Australian Government Department of Health and Ageing. Prostheses and Devices Committee (PDC) Bulletins. http://www.health.gov.au/internet/main/publishing.nsf/Content/privatehealth-pdc-bulletin.htm (accessed Jun 2009).
- 11. Australian Government Department of Health and Ageing. MBS Online. Item 38241. http://www9.health.gov.au/mbs/search.cfm?q=38241&sopt=I (accessed Jun 2009).





Abstract
The Australian Health Technology Assessment Review has the potential to have a major effect on the availability of new medical technology and the listing of associated medical procedures on the Medicare Benefits Schedule. Despite this, only about 15% of submissions to the Review came from “medical associations”.
Pharmaceutical and medical technologies are inherently different, and there are a number of difficulties associated with evaluating medical technology using the same process and evidence levels as those used for pharmaceuticals.
The current sequential and lengthy processing of new medical technology and procedures is delaying access to beneficial medical technology and could be substantially reduced.
There is currently no effective funding process for medical technology classified as capital equipment or consumables and disposables. This has created a perverse incentive in favour of using funded implantable prostheses based on access to funding rather than superior clinical effectiveness.
The existing horizon scanning process could be better used to not only identify all potentially cost-effective new and emerging medical technology and procedures as early as possible, but also to identify gaps in the evidence.