The causes of these evisceration injuries are well described in the literature. Vortex-style drains can create a powerful vacuum when occluded.1 In addition to the transanal route, direct evisceration through the perineum has been described.2 Other non-suction-related causes of transanal evisceration have also been described — in adults, it is usually associated with increased abdominal pressure or blunt trauma. This is a rare occurrence in adults, with only 53 reported cases.3 Non-suction-related transanal evisceration in children has only recently been described in relation to accidental and self-inflicted rectal trauma.4,5 The potential for penetrating trauma to cause evisceration should be considered by the astute clinician if the history or physical findings are not consistent. Associated perineal oedema and petechiae are well described with suction injuries. Entrapment in deeper water has also resulted in drowning.6
There can be a spectrum of injury associated with this mechanism, and treatment should be tailored accordingly. At the mild end of the spectrum, prolapse of the rectum can occur, which can be treated with simple reduction.7 True transanal evisceration always requires operative repair and often multiple procedures.1 In the patients described here, the bowel was difficult to reduce and required gentle pressure from below with guidance via laparotomy from above. The injury to the bowel in all cases was due to the traction on the mesentery and subsequent damage to the mesenteric vessels. This is in contrast to reported cases of evisceration from penetrating injury, where the eviscerated bowel was viable and otherwise intact.4,5 Patients 2 and 3 illustrate the importance of second-look laparotomy in the evaluation of bowel of questionable viability, as has been highlighted in the literature.1,6 Bowel that is initially of dubious viability can later be found to have survived, thus preserving length and avoiding complications of short bowel. The use of pulse oximetry to aid in determination of bowel viability has previously been described8 and was helpful in avoiding massive resection in our third patient. Prostacyclin analogues have been shown to have a beneficial effect on splanchnic perfusion in animal models and in human studies.9
There is considerable morbidity associated with this condition. The most minor form of injury can be a transient rectal mucosal prolapse with no perforation, but, even at this end of the spectrum, there is considerable psychological impact.7 At the most serious end of the injury spectrum, short bowel syndrome can occur, with an ongoing requirement for parenteral nutrition, and potentially even death following small bowel transplant.1,2,6 A 2007 review of published cases found that nine of 13 patients were dependent on parenteral nutrition.10 The lengths of bowel lost through these injuries are graphically represented in Box 1. By comparison, our patients had good outcomes, with no ongoing requirement for parenteral nutrition.
There is growing literature suggesting that suction drains are not necessary for pool cleaning, and that more effective, safer alternatives are available.11,12 If a suction drain is newly installed or is already in place, protective, or antivortex, covers have been advocated to minimise the suction risk.1 Although these covers will prevent direct suction injuries, hair or digits could still be trapped, and the covers only offer protection when fitted correctly and not removed. Two of our patients’ injuries occurred because the covers had been temporarily removed. In addition to the inherent danger of the pool suction drain, the arrangement of the drain in two of our cases made it even more inviting for a young child to sit on when uncovered (Box 2). Changing the shape, size and configuration of the aperture may therefore also prevent injury. Other potential remedies are adding an automatic cut-off switch so that the filter cannot function if the cover is off, or an override system that cuts off the filter if the intake appears to be occluded, thus limiting the peak negative pressure that can be generated.
The role of legislation with regard to education also needs to be considered. There has been a voluntary standard for swimming pool drains in Australia since 1980, and this was updated in 2003. This document mandates that any access hole greater than 150 mm in diameter be separated from the pool edge by a solid permanent beam of at least 100 mm width and be covered by a vented lid.13 The ongoing incidence of these injuries shows that this approach alone has failed to protect children. The “four Es” of injury prevention — education, engineering, enforcement and economics — have previously been described.14 Rather than a voluntary standard, legislation is needed to mandate the safety of swimming pool fittings, as has been the case with pool fencing.15 Enforcement of such legislation is also required to effect change.16 Finally, public education has been shown to be effective in injury prevention in other areas.17 These suction injuries are rare but potentially catastrophic. It is important to publicly highlight the danger of these injuries and effect change before more children are maimed.
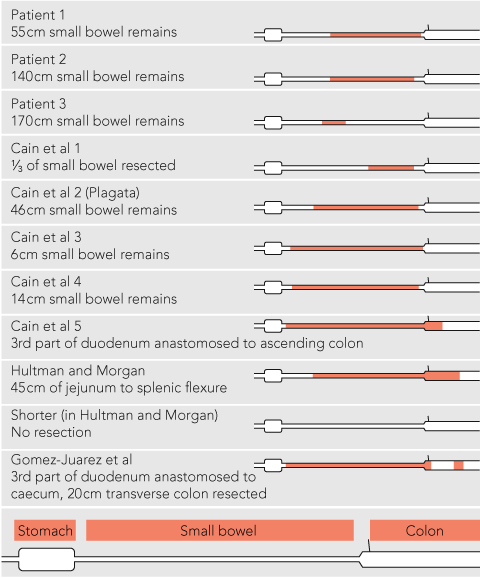
1 Length of bowel resected* in our three patients and eight other cases1,2,6 of transrectal evisceration
 |
Lessons from practice
Evisceration injuries caused by the suction of swimming pool drains are rare but potentially catastrophic events.
Delayed resection can minimise the chance of short bowel syndrome in evisceration injuries.
Although current engineering standards are adequate to prevent these kinds of injuries, education of pool owners and ultimately enforcement of legislation are required to ensure that standards are enacted.
- 1. Hultman CS, Morgan R. Transanal intestinal evisceration following suction from an uncovered swimming pool drain: case report. J Trauma 1994; 37: 843-847.
- 2. Gomez-Juarez M, Cascales P, Garcia-Olmo D, et al. Complete evisceration of the small intestine through a perianal wound as a result of suction at a wading pool. J Trauma 2001; 51: 398-399.
- 3. Morris AM, Setty SP, Standage BA, Hansen PD. Acute transanal evisceration of the small bowel: report of a case and review of the literature. Dis Colon Rectum 2003; 46: 1280-1283.
- 4. Bronkhorst MW, Wilde JC, Hamming JF, Heij HA. Anorectal impalement in a pediatric patient with transanal evisceration of small bowel. J Pediatr Surg 2007; 42: e23-e25.
- 5. Ravikumar R, Robb A, Jawaheer G. Small bowel evisceration through the rectum in childhood. J Pediatr Surg 2008; 43: 562-563.
- 6. Cain WS, Howell CG, Ziegler MM, et al. Rectosigmoid perforation and intestinal evisceration from transanal suction. J Pediatr Surg 1983; 18: 10-13.
- 7. Davison A, Puntis JWL. Awareness of swimming pool suction injury among tour operators. Arch Dis Child 2003; 88: 584-586.
- 8. La Hei ER, Shun A. Intra-operative pulse oximetry can help determine intestinal viability. Pediatr Surg Int 2001; 17: 120-121.
- 9. Lehmann C, König JP, Dettmann J, et al. Effects of iloprost a stable prostacyclin analog on intestinal leukocyte adherence and microvascular blood flow in rat experimental endotoxemia. Crit Care Med 2001; 29: 1412-1416.
- 10. Valletta E, Zampieri N, Fornaro M, et al. Transanal intestinal evisceration from swimming pool skimmer suction: a spur to prevention. Acta Paediatr 2007; 96: 1376-1377.
- 11. Association of Pool and Spa Professionals Technical Committee report on suction outlet safety and the effectiveness of ANSI/APSP-7. Alexandria, Va: APSP, 2007. http://www.apsp.org/utility/showDocumentFile/?objectID=13 (accessed Mar 2010, link updated Apr 2010).
- 12. Cronise R, Schowalter D. Eliminating the risk of swimming pool drains. Fluent News 2006; Summer: 32-34. http://www.fluent.com/about/news/newsletters/06v15i2/a10.pdf (accessed Mar 2010).
- 13. Australian Standard AS 1926.3—2003. Swimming pool safety. Part 3: water recirculation systems. Sydney: Standards Australia International, 2003.
- 14. Mello MJ, Getz MA, Lapidus G, et al. Innovations in injury prevention education. J Trauma 2007; 63 (3 Suppl): S7-S9.
- 15. Pearn JH, Nixon JW, Franklin RC, Wallis B. Safety legislation, public health policy and drowning prevention. Int J Inj Contr Saf Promot 2008; 15: 122-123.
- 16. van Weerdenburg K, Mitchell R, Wallner F. Backyard swimming pool safety inspections: a comparison of management approaches and compliance levels in three local government areas in NSW. Health Promot J Austr 2006; 17: 37-42.
- 17. Peat BG, Muller MJ, Skinner AM. Burns treatment for children: a comparative study of initial burns first aid, hospital care and changes following an education campaign [abstract PS027]. ANZ J Surg 2006; 76 Suppl 1: A51.






None identified.