The Duty to Care study was a comprehensive investigation that used population-based data linkage to examine the burden of physical diseases in users of mental health services (MHS) in Western Australia.1-5 The study showed that users of MHS, representing 8% of the general population (mostly with moderate to severe mental illness), were at excessive risk of developing all major physical diseases and had a high case-fatality rate from those illnesses.1-3 This raises the question as to whether lack of physical health care contributes to the poor physical health outcomes associated with mental illness.
In earlier reports, we postulated that part of the problem in Australia may be that individual and structural barriers might preclude the users of MHS gaining adequate access to primary care provided by general practitioners.1-3 Primary care is thought to be one of the foundations for improving the health outcomes of vulnerable populations6 and, for people with mental illness, could be potentially important in facilitating the interface between MHS and specialist medical services for physical conditions.7 This is particularly the case in Australia, where financial barriers to accessing GP services are largely removed by Medicare.8 The transformation of MHS from an institution-based to a community-based care model in Australia has implied an increasing involvement of GPs in the physical health care of people with mental illness.9
However, the extent to which people with mental illness are engaged by the GP sector in Australia is unknown. Previous studies from the United States suggest that people with serious mental illness, particularly schizophrenia and alcohol or drug disorders, receive a lower intensity of primary care.10-11 Homeless people with mental illness are unlikely to receive any medical care at all.12,13
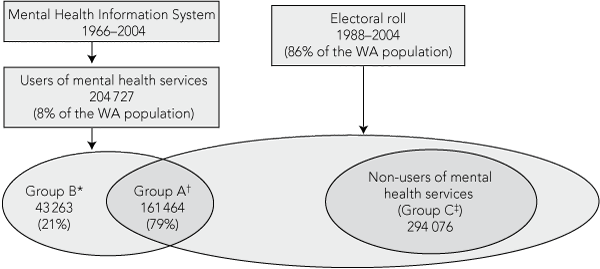
Users of MHS for this study included all people recorded in the MHIS from 1 July 1966 to 31 December 2004 who were still alive on or after 1 January 1990. These people were categorised as Group A or Group B, based on whether or not they had ever been on the Western Australian electoral roll (Box 1). The electoral roll data represented about 86% of the Western Australian general population aged ≥ 18 years. Non-users of MHS were a random sample of people who were on the electoral roll, but never recorded in the MHIS; these people were categorised as Group C. Group C was matched 2:1 with Group A by 5-year age group and sex.
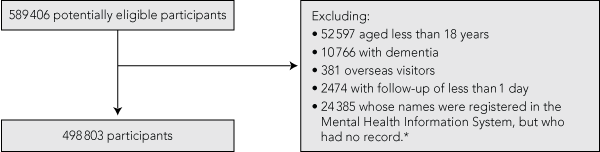
For users of MHS (Groups A and B), the start of follow-up (T0) was 1 January 1990 for people recorded in the MHIS before 1 January 1990, or the first date of registration with the MHIS for those who were first recorded from 1 January 1990 onwards. For non-users (Group C), T0 was the same as that of their matched person in Group A. People aged less than 18 years, those diagnosed with dementia, overseas visitors, those with a follow-up period of less than 1 day and people recorded in the MHIS with only incomplete mental health outpatient records were excluded from the study (Box 2).
Linked records concerning the study participants, dated according to time of services or events, were extracted from Western Australian Government and Australian Government datasets (see Box 3, A for details). Medicare Benefits Scheme (MBS) data included all claims for GP and specialist visits made by the participants within Australia, and not just in WA.
We ascertained the principal mental disorder for each user of MHS using a previously published method.2 Because some patients had extended periods of inpatient and outpatient contact with MHS, during which clinical views on the diagnosis were prone to vary, we used the last diagnosis recorded during the illness episode. However, if an earlier diagnosis was higher in the hierarchy of severity2 (Box 3, B), then the earlier diagnosis was taken as the principal diagnosis. If the last inpatient diagnosis was in the same hierarchical category as the last outpatient diagnosis, then we used the inpatient diagnosis. People with dementia were excluded after ascertaining the principal mental disorder. The remaining records were then grouped into one of 10 mutually exclusive categories of mental disorders (Box 3, C).
Scores for social and locational disadvantages were derived from the Index of Relative Socio-Economic Disadvantage (IRSD),14 and the Accessibility/Remoteness Index of Australia (ARIA).15 The IRSD and ARIA indices were available at the collector’s district level of the Australian Census, obtained for each record by geocoding the address field. IRSD scores were grouped into five levels of social disadvantage: most disadvantaged (the lowest 10% of IRSD scores of the Western Australian general population), more disadvantaged (10% to < 25%), little disadvantaged (25% to < 50%), less disadvantaged (50% to < 75%) and least disadvantaged (75%+).
Age, social and locational disadvantages, and calendar year were measured at T0. Physical comorbidities were measured by means of the Charlson Index, based on hospital inpatient data with a 5-year look-back period from T0.16
Characteristics and crude outcomes of study cohorts were compared usingχ2 tests (for categorical variables) or Mann–Whitney tests (for continuous variables). As there was overdispersion in our data, negative binomial regression models were used to compare the rates of visits to GPs between users and non-users of MHS as well as between the two subgroups of MHS users, after adjustment for 5-year age group, sex, Indigenous status, social disadvantage, locational disadvantage, calendar year, physical co-morbidities and visits to specialists. We also assessed locational disadvantage as a potential effect modifier in the relationship between mental disorders and visits to GPs. Missing values were treated as a separate exposure group so that all subjects were included in the analyses (Box 4). The analyses were performed using Stata version 10.0 for Windows (StataCorp, College Station, Tex, USA).
There were 498 803 eligible participants selected: 204 727 users of MHS and 294 076 non-users (Box 1). Characteristics of the study cohorts at T0 are shown in Box 4. Relative to non-users, users of MHS were more socially disadvantaged, more likely to be Indigenous and more likely to live in remote WA. Among users of MHS, Group B was younger, had a higher ratio of males to females (Box 4), and higher proportions of alcohol/drug disorders, schizophrenia and personality disorders compared with Group A (Box 5).
The 498 803 participants visited GPs a total of 32 575 719 times during a mean follow-up period of 10.9 years. The crude rate of visits to GPs was higher in Group A (8.22 visits per person-year; Box 6), and lower in Group B (4.31) compared with Group C (5.00). There were no visits to GPs observed in 2.1% of people in Group A, 44.4% in Group B (mainly because 98.3% of people in Group B who never had an address recorded in the WADLS had no visits to GPs recorded at all) and 3.9% in Group C (Box 6).
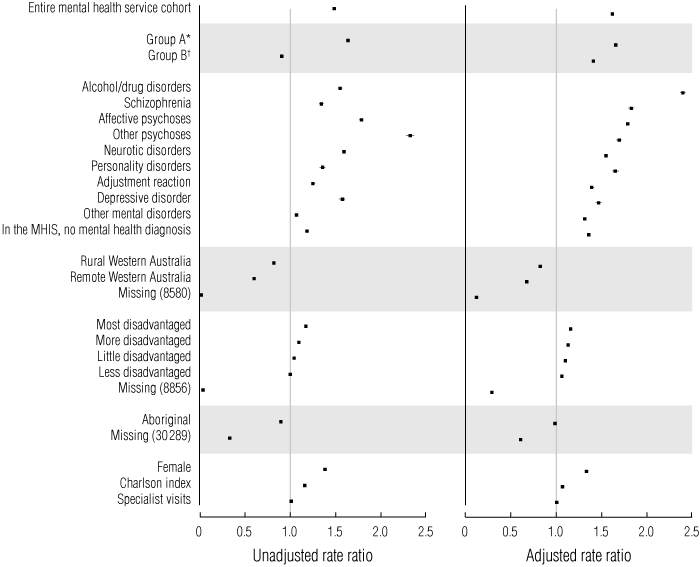
The large number of visits to GPs produced effect measures with very narrow confidence intervals (and all P values < 0.0001), so rate ratios were reported to three decimal places. Univariate regression analysis showed that users of MHS visited GPs significantly more often than non-users; and Group A participants visited GPs significantly more often, but Group B participants significantly less often, than Group C participants (Box 7). Multivariate regression analysis (Box 7) showed that, compared with non-users of MHS, the overall adjusted rate ratio (ARR) for visits to GPs among users of MHS was 1.622 (95% CI, 1.613–1.631). The ARR was highest in Group A (ARR, 1.663; 95% CI, 1.653–1.672), and higher in Group B (ARR, 1.416; 95% CI, 1.401–1.431), compared with Group C (ARR = 1).
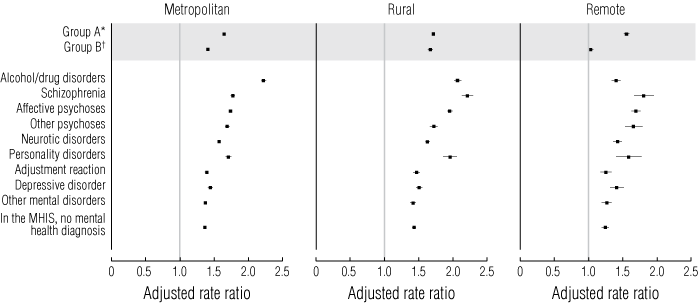
Among users of MHS, ARRs were most elevated in people with alcohol/drug disorders, schizophrenia and affective psychoses (ARRs, 2.404, 1.834 and 1.798, respectively); moderately raised in people with other psychoses, neurotic disorders, personality disorder (ARRs, 1.658, 1.552 and 1.700, respectively); and least elevated, but still higher than for non-users in those with adjustment disorder, simple depression and other mental disorders (ARRs, 1.399, 1.472 and 1.321, respectively). Patients from all categories of mental disorders visited GPs more often than non-users of MHS in metropolitan, rural and remote parts of WA (all ARRs > 1; Box 8).
Our findings differ from those of two large US studies that showed poor access to ambulatory general medical services among people with severe mental illness.10,11 One reason may be the differences between the Australian and US health care systems. The Australian health care system provides universal access to GP services financed by Medicare, while the US system does not. Another reason is that because MBS record data for visits to GPs have information on the length but not the purpose of consultations, we could not distinguish whether a GP visit was for physical or mental health reasons. A proportion of visits to GPs in this study may have been solely for mental health reasons, whereas physical and other preventive and health promotion issues may not have been dealt with during the same consultation. Our finding that the 4% of users of MHS who never had an address recorded in the WADLS (presumably homeless people) were unlikely to visit GPs at all is consistent with other studies.12,13
One limitation of our study was that the MBS data for visits to GPs did not have information on the purpose of the visit. Another limitation was the lack of data for private psychiatrists and GPs treating mental disorders. This would limit the extrapolation of our findings to all people with mental illness in Australia. Nevertheless, our study included about 40% of people with mental illness (generally with moderate to severe illness) whose physical health disparities were probably greater than the remainder of people with mental illness. Moreover, we used the same definition for our mental health cohort as did the Duty to Care study,2 which ensures the continuity and integrity of our investigations and findings.
The previously reported Duty to Care study highlighted the poorer physical health outcomes in users of MHS.1-3 With the opportunity provided by the recent development of the crossjurisdictional data linkage facility of the WADLS, we were able to determine whether the poorer physical health outcomes were partly the result of poorer engagement with the GP sector. The results show that, for the vast majority of users of MHS, this is not the case, at least in terms of the frequency of visits to GPs.
3 Summary of study methods
4 Characteristics of study participants at the start of follow up (T0)
Users of mental health services |
|||||||||||||||
5 Distribution of mental disorders in 204 727 users of mental health services
Users of mental health services |
|||||||||||||||
6 Numbers and crude rates of visits to general practitioners and specialists by users and non-users of mental health services, 1 January 1990 to 30 June 2006
Users of mental health services |
|||||||||||||||
7 Unadjusted (univariate analysis) and adjusted (multivariate analysis) rate ratios of visits to general practitioners from negative binomial regression analysis
8 Adjusted rate ratios of visits to general practitioners from multivariate analysis, stratified by locational disadvantage
Received 22 August 2009, accepted 22 November 2009
- Qun Mai1
- C D’Arcy J Holman2
- Frank M Sanfilippo3
- Jonathan D Emery4
- Louise M Stewart5
- University of Western Australia, Perth, WA.
We thank both the federal and Western Australian Departments of Health and Medicare Australia for providing the datasets that made this project possible. We also thank to the Data Linkage Branch at the Western Australian Department of Health for selecting study cohorts, linking and extracting associated linked records. The access and extraction of crossjurisdictional linked data required for this study was supported by a National Health and Medical Research Council (NHMRC) grant on chronic disease management in primary care, obtained by C D’Arcy J Holman. The remainder of this study was supported by Qun Mai’s PhD scholarship.
- 1. Lawrence D, Holman CD, Jablensky AV, et al. Excess cancer mortality in Western Australian psychiatric patients due to higher case fatality rates. Acta Psychiatr Scand 2000; 101: 382-388.
- 2. Lawrence D, Holman CDJ, Jablensky AV. Preventable physical illness in people with mental illness. Perth: University of Western Australia, 2001.
- 3. Lawrence DM, Holman CD, Jablensky AV, Hobbs MS. Death rate from ischaemic heart disease in Western Australian psychiatric patients 1980–1998. Br J Psychiatry 2003; 182: 31-36.
- 4. Lawrence D, Holman CD, Jablensky AV, et al. Increasing rates of suicide in Western Australian psychiatric patients: a record linkage study. Acta Psychiatr Scand 2001; 104: 443-451.
- 5. Lawrence DM, Holman CD, Jablensky AV, Fuller SA. Suicide rates in psychiatric in-patients: an application of record linkage to mental health research. Aust N Z J Public Health 1999; 23: 468-470.
- 6. Starfield B. Is primary care essential? Lancet 1994; 344: 1129-1133.
- 7. Druss BG. The mental health/primary care interface in the United States: history, structure, and context. Gen Hosp Psychiatry 2002; 24: 197-202.
- 8. Australian Government Department of Health and Ageing. Medicare benefits schedule book. Canberra: Department of Health and Ageing, 2004. http://www.health.gov.au/internet/mbsonline/publishing.nsf/Content/7B8 C8DCCFD5FCF3FCA2574F8007327A3/$File/2004-11-MBS.pdf (accessed Mar 2010).
- 9. Australian Health Ministers. National mental health policy. Canberra: Australian Government Department of Health and Ageing, 1992. http://www.health.gov.au/internet/main/publishing.nsf/Content/BF4CF02AE1033BF1CA 25722200119A23/$File/policy.pdf (accessed Mar 2010).
- 10. Cradock-O’Leary J, Young AS, Yano EM, et al. Use of general medical services by VA patients with psychiatric disorders. Psychiatr Serv 2002; 53: 874-878.
- 11. Druss BG, Rosenheck RA. Use of medical services by veterans with mental disorders. Psychosomatics 1997; 38: 451-458.
- 12. Folsom DP, McCahill M, Bartels SJ, et al. Medical comorbidity and receipt of medical care by older homeless people with schizophrenia or depression. Psychiatr Serv 2002; 53: 1456-1460.
- 13. Desai MM, Rosenheck RA, Kasprow WJ. Determinants of receipt of ambulatory medical care in a national sample of mentally ill homeless veterans. Med Care 2003; 41: 275-287.
- 14. Australian Bureau of Statistics. Information paper. Census of population and housing. Socio-economic indexes for areas, Australia 2001. Canberra: ABS, 2003. (ABS Cat, No. 2039.0.) http://www.ausstats.abs.gov.au/Ausstats/free.nsf/Lookup/AFF5E8542B58B9 4ECA256DD5007A3DF8/$File/20390_2001.pdf (accessed Mar 2010).
- 15. Australian Bureau of Statistics. Information paper. ABS views on remoteness. Canberra: ABS, 2001. (ABS Cat, No. 1244.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/papersbyTopic/667365C4D13BCF72CA2570AF00 42A9EB?OpenDocument (accessed Mar 2010).
- 16. Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373-383.





Abstract
Objective: To compare rates of visits to a general practitioner between users and non-users of mental health services (MHS).
Design, participants and setting: Population-based retrospective cohort study of 204 727 users and 294 076 matched non-users of MHS in Western Australia from 1 January 1990 to 30 June 2006, based on linked records of the use of MHS, hospital admissions, Medicare claims for GP and specialist services, electoral roll registration and deaths.
Main outcome measures: Adjusted rate ratios (ARRs) for the number of visits to GPs by users of MHS relative to non-users, and for different categories of mental disorders.
Results: Relative to non-users of MHS, the ARR of visits to GPs by users of MHS was 1.622 (95% CI, 1.613–1.631) overall, and was elevated in each separate category of mental illness. ARRs were highest for alcohol/drug disorders, schizophrenia and affective psychoses (2.404, 1.834 and 1.798, respectively). The results were not changed by location (metropolitan, rural or remote addresses). However, the 4% of MHS users with no fixed address had a very low ARR of visits to GPs (0.058; 95% CI, 0.057–0.060).
Conclusions: Users of MHS visit GPs substantially more often than non-users, with the exception of those with no fixed address who seldom see a GP at all.