The demand for emergency department (ED) services is increasing in most developed countries.1 It has been claimed that a significant cause of this increasing demand is “general practice patients” attending the ED rather than their general practitioner.2 The demand has led to experimentation with alternative sources of care, including after-hours general practice clinics at or near EDs.3 Many health services are working to have a general practice clinic in or near public hospitals. Literature on the quantitative effect of general practice clinics is equivocal,4-13 particularly in Australia.
We used regression time series analysis (Box 1) to examine the clinic’s impact on the number of low-urgency patients presenting to the ED. Patients were considered low-urgency if they were assigned an Australasian Triage Scale (ATS) category of 4 (potentially serious) or 5 (less urgent).15 De-identified hospital data for the period January 1998 to October 2008 were retrieved from the NSW Health Emergency Department Information System.
Multiple linear regression using Cochrane–Orcutt transformation16 was performed in Intercooled Stata 9.0 for Windows (StataCorp, College Station, Tex, USA). The following dependent variables were examined in turn: daily ATS category 4 and 5 presentations to the ED at any time of day, daily ATS category 4 and 5 presentations to the ED during the hours the AHC was open (the AHC was open a total of 27 hours a week), and daily ATS category 1, 2 and 3 (immediately, imminently and potentially life-threatening) presentations to the ED at any time of day.
Explanatory variables coding for a linear trend, day of the week, and month of the year were included. To this statistical model we added an abrupt permanent change intervention variable and then a two-parameter gradual permanent intervention.17 The abrupt permanent change assumes the number of daily ED presentations changes to a new level from the moment the clinic opens, whereas the gradual permanent intervention model assumes a gradual change to reach the same level as observed in the abrupt permanent change.
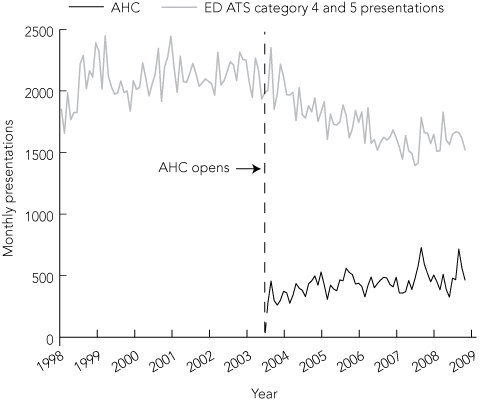
During the study period, there were 345 465 presentations to the ED. After the opening of the AHC in March 2003, monthly low-urgency presentations appeared to decline, while the number of consultations at the AHC appeared to grow (Box 2).
The mean and range of daily presentations to the ED before and after the opening of the AHC are shown in Box 3. On average, there were 67.9 presentations to the ED per day of patients triaged as ATS category 4 or 5 before the clinic opened, and 56.0 presentations per day after it opened.
After adjusting for the long-term trend and weekly and annual cycles, daily presentations to the ED at any time of day of patients triaged as ATS category 4 and 5 fell by 7.04 patients a day (95% CI, 5.39–8.70) (Box 4) after the opening of the AHC. This represents an 8.2% reduction in total ED presentations (95% CI, 6.2%–10.2%).
The magnitude of the observed change is similar to the 8.9% observed in the Netherlands7 but greater than the modelled estimates of 2%–3% in Fremantle, Western Australia,2 and 2.5% (95% CI, 2.4%–2.6%) across the Perth metropolitan area.5 The larger impact observed in Wagga Wagga could be associated with the antecedent conditions, as a larger impact is likely where there is limited existing after-hours GP access. Before the clinic opened, after-hours general practice services in Wagga Wagga were extremely limited and the GP to patient ratio relatively low (1 : 1401). Many low-urgency patients may therefore have attended the ED because it was the only available option. Hence, our estimates are likely to be closer to the maximal response that may be expected from AHCs.
In Australia, the effect of AHCs is often examined in the context of their ability to reduce access block, where their value is often considered limited.3,4 This approach may undervalue AHCs, if the benefits of diverting low-urgency and general practice patients to primary care are not also considered. In a comparison of the costs and quality of care between primary and specialist care, populations using primary care as their first source of care had lower health expenditures than other groups.18,19 This is further demonstrated by the observation that employing GPs within the ED to attend to low-acuity patients reduced costs by around 40% relative to hospital doctors.19,20 This reflected GPs’ less frequent requests for investigations and referrals, and was achieved with no differences in patient satisfaction or clinical outcome. General practice clinics may increase patient satisfaction, as the shorter waiting times frequently observed in general practice, compared with the ED, have been associated with increased patient satisfaction.21
The aim of this study was to examine the effect of the AHC on low-urgency ED presentations. Clearly, not all patients with an ATS category of 4 or 5 will be suitable for general practice (eg, a patient with broken digits).3 The aim is to direct the maximum number of people to the most appropriate care. Patients that chose to attend the AHC were not diverted away from care but rather offered an alternative service. As it is not a bulk-billing clinic, the patients attending the AHC showed, by their willingness to purchase the service, that they believed the net benefits were greater than the benefits of attending the ED. Even in the presence of substantial costs to patients, the AHC had an effect. All else being equal, the effect of bulk-billing clinics may be even greater.
The use of time series analysis assisted in adjusting the effect of the intervention for underlying trends and cycles. The estimate of the intervention effect depends heavily on the statistical model’s ability to remove the trends in the data and reduce the residuals to “white noise”. This is often achieved by using autoregressive integrated moving average (ARIMA) models,22 but our data could not be modelled satisfactorily by standard or seasonal ARIMA models. However, the use of indicator variables gave a high level of flexibility to the cyclical adjustment, and the Cochrane–Orcutt estimation16 adjusted the linear model for serial correlation in the error terms.
1 Time series analysis
A time series is a set of observations of the same variable through time.
Many time series, such as daily presentations to an emergency department (ED), demonstrate long-term trends, as well as weekly, seasonal and other cyclical patterns.
If no allowance is made for these underlying trends and cycles, then pre- and post-intervention testing will often detect changes that may have occurred irrespective of the intervention.14
2 Monthly low-urgency presentations to Wagga Wagga Base Hospital emergency department (ED), and monthly presentations to the after-hours clinic (AHC)
 |
3 Descriptive statistics for daily presentations to the emergency department (ED) and after-hours clinic (AHC), before adjusting for contemporaneous trends and cycles
Daily ED presentations (ATS category 4 and 5) at any time of day |
|||||||||||||||
Daily ED presentations (ATS category 4 and 5) during AHC hours |
|||||||||||||||
Daily ED presentations (ATS category 1, 2 and 3) at any time of day |
|||||||||||||||
- David J Buckley1
- Paul W Curtis2
- Joseph G McGirr3
- Greater Southern Area Health Service, Wagga Wagga, NSW.
We would like to thank Paul Locker at the Riverina Division of General Practice for providing history and information about the Wagga Wagga AHC.
None identified.
- 1. Cameron PA, Kennedy MP, McNeil JJ. The effects of bonus payments on emergency service performance in Victoria. Med J Aust 1999; 171: 243-246.
- 2. Sprivulis P. Estimation of the general practice workload of a metropolitan teaching hospital emergency department. Emerg Med (Fremantle) 2003; 15: 32-37.
- 3. Australasian College for Emergency Medicine. The relationship between emergency department overcrowding and alternative after-hours GP services. Melbourne: ACEM, 2004. http://www.webcitation.org/5VGYQM4XM (accessed Mar 2010).
- 4. Richardson DB, Mountain D. Myths versus facts in emergency department overcrowding and hospital access block. Med J Aust 2009; 190: 369-374. <MJA full text>
- 5. Nagree Y, Ercleve TNO, Sprivulis PC. After-hours general practice clinics are unlikely to reduce low acuity patient attendances to metropolitan Perth emergency departments. Aust Health Rev 2004; 28: 285-291.
- 6. Stoddart D, Ireland AJ, Crawford R, Kelly B. Impact on an accident and emergency department of Glasgow’s new primary care emergency service. Health Bull (Edinb) 1999; 57: 186-191.
- 7. van Uden CJT, Crebolder HFJM. Does setting up out of hours primary care cooperatives outside a hospital reduce demand for emergency care? Emerg Med J 2004; 21: 722-723.
- 8. van Uden CJT, Winkens RAG, Wesseling G, et al. The impact of a primary care physician cooperative on the caseload of an emergency department: the Maastricht integrated out-of-hours service. J Gen Intern Med 2005; 20: 612-617.
- 9. Bolton P, Thompson L. The reasons for, and lessons learned from, the closure of the Canterbury GP After-Hours Service. Aust Health Rev 2001; 24: 66-73.
- 10. O’Keeffe N. The effect of a new general practice out-of-hours co-operative on a county hospital accident and emergency department. Ir J Med Sci 2008; 177: 367-370.
- 11. Ieraci S, Cunningham P, Talbot-Stern J, Walker S. Emergency medicine and “acute” general practice: comparing apples with oranges. Aust Health Rev 2000; 23: 152-161.
- 12. Ruffin RE, Hooper JK. Responses to access block in Australia: the Queen Elizabeth Hospital Medical Division. Med J Aust 2003; 178: 104-105. <MJA full text>
- 13. Liaw ST, Hill T, Bryce H, Adams G. Emergency and primary care at a Melbourne hospital: reasons for attendance and satisfaction. Aust Health Rev 2001; 24: 120-134.
- 14. Cable G. Enhancing causal interpretations of quality improvement interventions. Qual Health Care 2001; 10: 179-186.
- 15. Hollis G, Sprivulis P. Reliability of the National Triage Scale with changes in emergency department activity level. Emerg Med 1996; 8: 231-234.
- 16. Cochrane D, Orcutt GH. Application of least squares regression to relationships containing auto-correlated error terms. J Am Stat Assoc 1949; 44: 32-61.
- 17. Box GEP, Tiao GC. Intervention analysis with applications to economic and environmental problems. J Am Stat Assoc 1975; 70: 70-79.
- 18. Engström S, Foldevi M, Borgquist L. Is general practice effective? A systematic literature review. Scand J Prim Health Care 2001; 19: 131-144.
- 19. Dale J, Lang H, Roberts JA, et al. Cost effectiveness of treating primary care patients in accident and emergency: a comparison between general practitioners, senior house officers and registrars. BMJ 1996; 312: 1340-1344.
- 20. Murphy AW, Bury G, Plunkett PK, et al. Randomised controlled trial of general practitioner versus usual medical care in an urban accident and emergency department: process, outcome, and comparative cost. BMJ 1996; 312: 1135-1142.
- 21. Bolton P, Mira M. A comparison of waiting times, patient choice and satisfaction in three primary care settings. Aust J Prim Health 2003; 9: 68-70.
- 22. Box GEP, Jenkins GM, Reinsel GC. Time series analysis: forecasting and control. 3rd ed. Englewood Cliffs, NJ: Prentice Hall, 1994.





Abstract
Objective: To assess the impact of the opening of an after-hours general practice clinic on the number of daily low-urgency presentations to the nearby emergency department.
Design, participants and setting: Retrospective time series analysis of emergency presentation data, from the New South Wales Health Emergency Department Information System, for all patients presenting to the emergency department of Wagga Wagga Base Hospital between January 1998 and October 2008.
Main outcome measures: Daily emergency department presentations, before and after the March 2003 opening of the after-hours clinic, of patients triaged as Australasian Triage Scale (ATS) category 4 or 5 (at any time of day, and during the hours of operation of the clinic), and of patients triaged as ATS category 1, 2 or 3 (at any time of day).
Results: After adjusting for long-term trends and weekly and annual cycles, the opening of the after-hours clinic was associated with a daily reduction of 7.04 patients (95% CI, 5.39–8.70) in emergency department presentations with an ATS category of 4 or 5. This represented an 8.2% reduction in total presentations (95% CI, 6.2%–10.2%). Presentations of ATS category 1, 2 or 3 patients rose by 1.36 patients a day (95% CI, 0.36–2.35), representing 1.6% of total presentations (95% CI, 0.4%–2.7%). The impact of the after-hours clinic was best modelled by a gradual permanent change.
Conclusion: An after-hours general practice clinic was associated with a reduction in low-urgency presentations to the emergency department in Wagga Wagga.