Arecent editorial in the Journal stated that percutaneous vertebroplasty is not an effective therapy for acute osteoporotic vertebral fractures.1 The natural history of acute osteoporotic vertebral fractures is that most heal spontaneously, with pain gradually subsiding over 6–12 weeks after the fracture. A select group of patients with acute osteoporotic vertebral fracture may present with severe back pain, often requiring narcotic analgesia and hospitalisation. We argue that vertebroplasty is effective for this group of patients. These patients are very different from those sampled by two recent randomised controlled trials (RCTs)2,3 that were the focus of the recently published editorial.1 We believe that neither the editorial nor the two cited RCTs are relevant to the patients that we treat with vertebroplasty. Here, we closely analyse the trials and argue against the editorial’s opinion that the two trials represent “the best evidence we have to date on the value of vertebroplasty”.
The vertebroplasty programs in southern and south-western Sydney provide the largest clinical experience in Australia. We have collectively treated more than 2500 cases over the past 9 years. Our indication to perform vertebroplasty is very different to that of either of the recent RCTs.2,3 We select patients with the most severe pain caused by an acute osteoporotic fracture that is less than 6 weeks old. We treat patients in whom the pain is not controlled adequately with medical therapy or in whom the pain results in hospitalisation. Patients are advised that most fractures will heal with conservative therapy, but for those cases when the pain is very severe or mobility is severely impaired, vertebroplasty can provide almost immediate relief. Vertebroplasty advances the analgesia afforded by fracture union by about 6 weeks. A secondary benefit may be reduced volume loss in the fractured vertebra, which may reduce kyphosis.4
Most of the fractures that we treat are not simple crush fractures, but have more complex architecture. These more complex fracture types are associated with more severe pain. Axial transections of the vertebral body (Box 1) seem far more painful than simple crush fractures. Acute fractures adjacent to old, deformed, healed fractures are also associated with amplified pain, presumably because there is abnormal biomechanical stress through the fracture line. Osteonecrotic fracture clefts develop in some patients with osteoporosis (Box 2), and are often associated with severe and more prolonged pain. We observe that vertebroplasty provides early pain relief and mobilisation in patients struggling to cope in the acute situation.
A study by Diamond et al sampled 126 consecutive patients from the St George Public and Private Hospitals in Southern Sydney within a 2-year interval (November 2000 to December 2002).5 All patients had fractures less than 6 weeks old and were considered appropriate for vertebroplasty by both the attending physician and interventional radiologist. The study was a non-randomised, prospective controlled trial. Eighty-eight patients receiving vertebroplasty were compared with 38 who refused vertebroplasty and received best medical therapy; 43% of those enrolled were hospital inpatients. The study showed a 60% reduction in pain at 24 hours in the vertebroplasty group. There was a 41% reduction in hospital length-of-stay in the inpatient vertebroplasty group. This enrolment pattern is dramatically different from that of either of the recent RCTs. A comparison of enrolment criteria in the Diamond et al study compared with the two recent trials is shown in Box 3.
The timing of fracture treatment is critical because, in our opinion, vertebroplasty provides internal fixation. This fixation prevents the pain of fracture fragment motion — in a similar manner to the way plaster casts act in acute forearm fractures. To extend this analogy, it would be absurd to routinely apply a plaster cast to a fractured radius at 9.5 weeks or at 16 weeks (as in these two cited RCTs2,3) to obtain palliation of pain. The fixation must normally be applied acutely, before fracture union, to be effective. Osteoporotic fractures involve the vertebral bodies (predominantly trabecular bone) while sparing the posterior elements (predominantly cortical bone). The structure of the vertebral body lends itself to cementoplasty. The surrounding cortical plate constrains the bone cement within the trabecular compartment, consolidating the fractured trabecular fragments of the vertebral body into a single unit.
The average duration of fracture pain at time of intervention in our programs is 3 weeks. The average duration of pain in the Buchbinder et al trial was 9.5 weeks3 and in the Kallmes et al trial was 18 weeks.2 This timeline suggests that most patients in both trials had “healed” fractures. Beyond 8 weeks, most patients have united (clinically healed) vertebral fractures, and pain should no longer be generated from fracture fragment motion. Vertebroplasty will less commonly be efficacious in this group. The exception is in patients whose fractures progress to osteonecrosis rather than fracture healing, resulting in a plane of “non-union” containing gas and fluid, which separates the superior from the inferior end-plates of the vertebral body.
The Kallmes et al trial describes “our previous finding that the fracture age is not associated with the response to vertebroplasty”.2 To suggest that the use of an internal fixation technique will be equally efficacious at 2 weeks after a fracture and 12 months later defies all principles of fracture fixation. The failure of Kallmes et al to demonstrate a benefit from vertebroplasty in this trial may reflect the incorrect timing of the intervention and a misunderstanding of the mechanics of vertebroplasty.
Both recent trials included patients with back pain for up to 12 months, which is far too long for a trial of acute fractures. For vertebroplasty, we select patients with the most severe pain who have “fresh” fractures less than 6 weeks old. This patient group was inadequately included in either recent RCT. Buchbinder et al3 included only 25 patients (32% of the total) who had pain for less than 6 weeks, which is far too small a number for separate statistical analysis as defined by the authors’ own calculations.6 Kallmes et al2 does not disclose how many patients had fractures less than 6 weeks old. It is likely to be few, as the trial protocol excluded patients with fractures less than 4 weeks old (Clinical protocol IDE #G030091/S2 as presented to the St George Hospital Ethics Committee), and the mean age of fractures was 16 weeks at the time of random allocation.
Correct patient selection is primarily a clinical decision and requires input from both the referring clinician and interventional radiologist. The interventional radiologist was excluded from patient selection in the Buchbinder et al trial,3 which is not normal clinical practice and may have further compromised patient selection.
Magnetic resonance imaging (MRI) is considered an important adjunct in patient selection as it verifies the fracture as recent. Our patients all undergo MRI unless they have contraindications. Clinical experience correlating bone oedema apparent on MRI with vertebroplasty in more than 2000 cases has taught us that oedema can persist for several months beyond fracture consolidation. Some bones, still appearing bright on fat-suppressed MRI, are extremely hard at vertebroplasty and the fracture has clearly united. The duration of MRI-apparent bone oedema and alterations in the pattern of oedema after osteoporotic vertebral fracture remain unquantified in the literature. Fracture healing should be assessed clinically by character of pain and time from fracture. The contention in Box 1 of the Buchbinder et al editorial that bone oedema apparent on MRI itself confirms a fracture to be unhealed1 is, in our opinion, incorrect. The MRI confirms a recent fracture, but, beyond 6 weeks, fracture duration does not itself indicate a failure of bony union unless a fluid-filled cleft is demonstrated within the bone.
The trial of Kallmes et al2 required neither an MRI scan nor a bone scan for enrolment. We do not accept this as appropriate for proper patient selection.
Inpatients were excluded from the Kallmes et al trial by protocol. This important omission was not disclosed in the published report of the trial.2 We regard this as a major shortcoming because many of the patients we treat with vertebroplasty are inpatients. There is no mention of inpatients in Buchbinder et al,3 which also appears to be an outpatient trial.
Both recent RCTs had difficulties with patient recruitment. The published protocol of the Kallmes et al trial aimed to enrol 250 patients,7 but was completed with 131 patients after 4 years.2 The refusal rate of 70% may have caused selection bias and may have reduced the statistical power. There is no reported follow-up of the patients who refused to participate.
The published protocol of the Buchbinder et al trial aimed to enrol 200 patients6 but the trial recruited only 78 patients over 4.4 years.3 This trial was affected by the early withdrawal of two of the four participating centres. The third centre had no previously existing vertebroplasty program, and enrolled 15 patients over 4.4 years. The remaining 53 patients (68% of the trial’s enrolment) were followed at a single centre, with the interventions performed by one radiologist. The Buchbinder et al trial was, in effect, more a single-centre, single-radiologist study and not, as reported, a multicentre trial of vertebroplasty. The rate of patient refusal at point of enrolment was 64%.
Vertebroplasty is operator dependant and proper technique is very important. The technique as described in the Buchbinder et al trial3 mandates the use of 13-gauge needles and 1 mL syringes to inject the bone cement. The average injected volume was 2.8 mL of cement which is, in our experience, too little to adequately stabilise most vertebral fractures. In our practice, lumbar fractures usually require cement volumes of up to 10 mL per treated level, necessitating the use of 11-gauge needles and more modern injecting systems. The cement distribution must be sufficient to provide internal fixation to all segments of the vertebral body, or the procedure will not be effective (Box 2). These technical failings are central problems of the study, and could also explain the relatively poor outcomes of the trial’s vertebroplasty group.
A previous publication from the same principal institution as the Kallmes et al RCT reported that cement volume was not related to clinical outcome.8 The RCT by Kallmes et al2 is the logical extension of this earlier study in its finding that the injection of zero cement is the same as cement injection. Kallmes et al state: “We previously had found that a fracture duration of up to 1 year was associated with a good response to vertebroplasty”. These publications demonstrate the futility of applying vertebroplasty to healed fractures. It is not surprising that, in patients with healed fractures, the cement volume injected (from zero to 10 mL) will not affect outcome, or that outcomes will be similar to a sham procedure. On the contrary, our experience with acute fractures less than 6 weeks old is that adequate cement volume and distribution is critical to obtaining good analgesia through internal fixation.
Both recent RCTs had very poor efficacy of their vertebroplasty interventions, with mean pain score reductions after vertebroplasty of only 2.3 cm (Buchbinder et al3) and 3.0 cm (Kallmes et al2) on a 10 cm visual analogue scale for pain. This contrasts dramatically with our own clinical experience and also with expected results based on the literature. A systematic review of 15 articles reporting results from 11 prospective, three retrospective and one controlled trial of 1136 vertebroplasty procedures showed a mean pain score reduction of 5.7 cm on a 10 cm visual analogue scale in the short term after vertebroplasty.9 Similar results were published in other meta-analyses.10-12 The authors of the trials recognise that this level of efficacy is what vertebroplasty routinely achieves. In the Buchbinder et al trial, the investigators were predicting an effect of vertebroplasty of “more than 5 points on a 10-point scale”.3 Their study did not achieve this expected outcome.
In recent correspondence in the New England Journal of Medicine,13 Buchbinder et al and Kallmes et al cite a recently published RCT of vertebroplasty14 as evidence that the procedure is ineffective in acute fractures. This study from Denmark enrolled 50 patients in 7 years with fractures less than 8 weeks old. It randomly allocated patients to vertebroplasty or best medical therapy. Only 36 of these patients had baseline pain scores measured before random allocation. MRI was optional. Pain estimates were recorded immediately after vertebroplasty and at 3 months. The trial found a reduction in pain score of 5.7 cm on a 10 cm visual analogue scale at 24 hours after vertebroplasty, and a statistically significant reduction in duration of hospitalisation in the vertebroplasty group. No significant differences in pain scores were noted at 3 months, which is not surprising given the small sample size, and the fact that most fractures in the conservative group will heal in the first 2 months after the fracture. Any persisting benefit beyond this period can only accrue from improved vertebral height and spinal mechanics, and may not be detected unless the study is powered adequately to assess this outcome.
The 12-month data from the VERTOS II trial15,16 were presented at the annual meeting of the Cardiovascular and Interventional Radiology Society of Europe (CIRSE) in Lisbon in September 2009. This study from five centres in the Netherlands enrolled 202 patients with acute fractures of less than 6 weeks’ duration, all with MRI correlation. Their patient selection, imaging and numeric enrolment were optimal. Patients were randomly allocated to vertebroplasty or conservative therapy, with 101 patients in each group. The trial findings, as presented by the principal author at CIRSE, showed a statistically significant analgesic effect of vertebroplasty with a 60% reduction in pain score at 24 hours after the procedure. The pain advantage in the vertebroplasty group compared with the conservative group progressively narrowed with time, as expected, but still remained statistically significant at 12 months. The study was also powered for cost-effectiveness.
It is our opinion that the two recent RCTs2,3 discussed in the recent editorial on vertebroplasty by Buchbinder et al1 sampled a group of patients with healed fractures who were unlikely to benefit from vertebroplasty. The patients whom we treat with vertebroplasty are very different from those sampled in these trials. The editorial by Buchbinder et al incorrectly generalised the findings of these trials to include the group with acute fractures that we treat.
1 Imaging before and after vertebroplasty of an acute osteoporotic fracture in the thoracolumbar spine of a 79-year-old patient 2 weeks after a fall
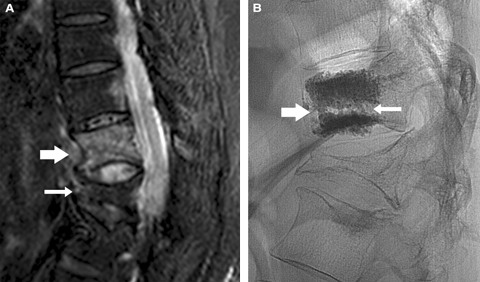
A: Sagittal short-inversion-time inversion recovery (STIR) magnetic resonance imaging (MRI) scan of the thoracolumbar spine. On this type of MRI scan, fluid provides the only bright signal. This is a midline image, with anterior to the left, showing an acute T12 fracture (broad arrow). Note the dark linear fracture line transgressing the vertebral body. This is not a “crush fracture” but rather an axial transection splitting the vertebral body into inferior and superior halves. There is an old, healed fracture of the L1 vertebral body (thin arrow) which alters the biomechanical strain through the acute T12 fracture line. The lack of bright signal in the
L1 fracture shows this to be long-standing.
B: Vertebroplasty image in the lateral projection. Note the trabecular cement filling in the superior and inferior aspects of the vertebral body, separated by the fracture line (thin arrow). There is an anterior cement column (broad arrow) bonding the two fragments together and providing internal fixation.
2 Imaging before and after vertebroplasty of an acute osteoporotic fracture in the lumbar spine of an 80-year-old patient 3 weeks after a lifting injury
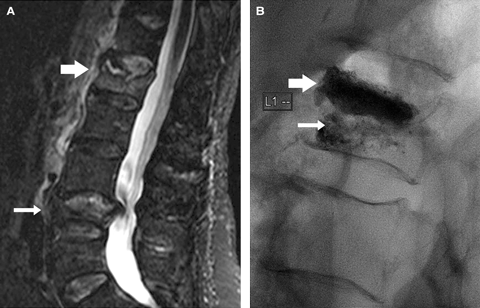
A: Sagittal short-inversion-time inversion recovery (STIR) magnetic resonance imaging scan
of the lumbar spine. The only bright signal is provided by fluid. There is an acute fracture of
L1 (broad arrow). Note the linear fluid cleft immediately below the superior end-plate of the vertebral body. This represents an osteonecrotic cleft. There is an old, healed fracture of
L4 (thin arrow). The lack of bright signal in L4 shows it to be old.
B: Vertebroplasty image of L1. The broad arrow points to the dense cement filling in the osteonecrotic cavity, which has reconstructed the superior end-plate. The thin arrow points
to the “fluffy” cement filling of the more normal trabecular bone in the inferior half of the vertebral body. It is essential to fill this inferior segment to prevent ongoing fracture and collapse. (Injected cement volume, 12 mL.)
- William A Clark1
- Terrence H Diamond2
- H Patrick McNeil2
- Peter N Gonski3
- Glen P Schlaphoff4
- John C Rouse5
- 1 Interventional Radiology, St George Private Hospital, Sydney, NSW.
- 2 University of New South Wales, Sydney, NSW.
- 3 Southcare, Sutherland Hospital, Sydney, NSW.
- 4 Liverpool Hospital, Sydney, NSW.
- 5 St George Hospital and Sutherland Hospital, Sydney, NSW.
William Clark was an expert adviser to the Medical Services Advisory Committee (MSAC) in the determination of public funding of vertebroplasty and has again been called to MSAC as an expert adviser to determine future public funding of vertebroplasty. Terrence Diamond and William Clark were investigators in the Kallmes et al trial.2
- 1. Buchbinder R, Osborne RH, Kallmes DF. Vertebroplasty appears no better than placebo for painful osteoporotic spinal fractures and has potential for harm [editorial]. Med J Aust 2009; 191: 476-477. <MJA full text>
- 2. Kallmes D, Comstock B, Heagerty P, et al. A randomized trial of vertebroplasty for osteoporotic spinal fractures. N Engl J Med 2009; 361: 569-579.
- 3. Buchbinder R, Osborne R, Ebeling P, et al. A randomized trial of vertebroplasty for painful osteoporotic vertebral fractures. N Engl J Med 2009; 361: 557-568.
- 4. Teng MMH, Wei C, Wei L, et al. Kyphosis correction and height restoration effects of percutaneous vertebroplasty. Am J Neuroradiol 2003; 24: 1893-1900.
- 5. Diamond TH, Bryant C, Browne L, Clark WA. Clinical outcomes after acute osteoporotic vertebral fractures: a 2-year non-randomised trial comparing percutaneous vertebroplasty with conservative therapy. Med J Aust 2006; 184: 113-117. <MJA full text>
- 6. Buchbinder R, Osborne RH, Ebeling PR, et al. Efficacy and safety of vertebroplasty for treatment of painful osteoporotic vertebral fractures: a randomized controlled trial. BMC Musculoskelet Disord 2008; 9: 156.
- 7. Gray LA, Jarvik JG, Heagerty PJ, et al. Investigational vertebroplasty efficacy and safety trial (INVEST): a randomized controlled trial of percutaneous vertebroplasty. BMC Musculoskelet Disord 2007; 8: 126.
- 8. Kaufmann TJ, Trout AT, Kallmes DF. The effects of cement volume on clinical outcomes of percutaneous vertebroplasty. Am J Neuroradiol 2006; 27: 1933-1937.
- 9. Ploeg WT, Veldhuizen AG, The B, Sietsma MS. Percutaneous vertebroplasty as a treatment for osteoporotic vertebral fractures: a systematic review. Eur Spine J 2006; 15: 1749-1758.
- 10. McGirt M, Parker S, Wolinsky J-P, et al. Vertebroplasty and kyphoplasty for the treatment of vertebral compression fractures: an evidence-based review of the literature. Spine J 2009; 9: 501-508.
- 11. Hochmuth K, Proschek D, Schwartz W, et al. Percutaneous vertebroplasty in the therapy of osteoporotic vertebral compression fractures: a review. Eur Radiol 2006; 16: 998-1004.
- 12. Eck JC, Nachtigall D, Humphreys C, Hodges SD. Comparison of vertebroplasty and balloon kyphoplasty for treatment of vertebral compression fractures: a meta-analysis of the literature. Spine J 2008; 8: 488-497.
- 13. Trials of vertebroplasty for vertebral fractures [author reply]. New Engl J Med 2009; 361: 2099-2100.
- 14. Rousing R, Andersen M, Jespersen S, et al. Percutaneous vertebroplasty compared with conservative treatment in patients with painful acute or subacute osteoporotic vertebral fractures: three-months follow-up in a clinical randomized study. Spine 2009; 34: 1349-1354.
- 15. Klazen CA, Verhaar HJJ, Lampmann LEH, et al. VERTOS II. Percutaneous vertebroplasty versus conservative therapy in patients with painful osteoporotic vertebral compression fractures; rationale, objectives and design of a multicentre randomized controlled trial. Trials 2007; 8: 33.
- 16. Klazen C, Lohle P, Jansen F, et al. 1-year results of the VERTOS II trial: vertebroplasty versus conservative therapy. Cardiovasc Intervent Radiol 2009; 32 (Suppl 2): 313.





Abstract
We use vertebroplasty for patients with the most severe pain caused by osteoporotic vertebral fractures less than 6 weeks old, and have observed dramatic pain relief in this acute setting.
A recent editorial in the Journal, written by the authors of two recent vertebroplasty trials, suggested that vertebroplasty is not an effective therapy for acute osteoporotic vertebral fractures.
The trials described in the editorial sampled a very different patient cohort to the one that we treat with vertebroplasty.
Our clinical experience and most of the published literature relating to the benefits of vertebroplasty are in striking contrast to the opinions presented in that editorial.