Each year, there are about 5 million new vertebral fractures worldwide.1 Only 20%–30% of these are experienced as a discrete clinical event. Patients present with pain, and frequently require hospital admission for analgesia, bed rest and physical support (bracing). While their back pain may last for 6–12 weeks, complications such as pneumonia, decubitus ulcers, venous thromboembolism and even death may occur.2 Percutaneous vertebroplasty has become an alternative to conservative treatment of acute osteoporotic vertebral fractures.3-15 To date there are no published comparative studies with a conservatively treated control group to verify the benefits of percutaneous vertebroplasty. Moreover, concerns about the safety of the procedure have been raised,12,16,17 as well as the possibility that it increases the incidence of new compression fractures in adjacent vertebrae.6,18,19
To examine these issues, we performed a 2-year prospective study of 88 patients with osteoporosis treated by percutaneous vertebroplasty and 38 patients who declined percutaneous vertebroplasty and were managed conservatively, comparing clinical outcomes, fracture rates and survival.
We have published an interim 1-year analysis previously,20 and report here the completed 2-year intention-to-treat analysis. We chose a priori to define the benefits of percutaneous vertebroplasty with respect to pain and efficacy at 1 year, and safety and refracture risk at 2 years. The cohort comprised 126 consecutive patients with osteoporotic vertebral fracture presenting to St George Hospital from November 2000 to December 2002; 72 patients were managed as outpatients and 54 as inpatients.
Recruited patients satisfied the inclusion criteria of acute vertebral fracture pain (occurring within 1–6 weeks of the event and not relieved by oral analgesia) and imaging criteria of acute fracture activity. Patients were excluded if there was evidence of a pathological fracture (caused by myeloma or metastasis), osteomyelitis, major retropulsion of bony fragments into the spinal canal, or coagulopathy.
Data on patient demographics, osteoporotic risk factors such as a smoking history, alcohol intake, corticosteroid use (> 5 mg of prednisone equivalent per day), vitamin D status, parathyroid hormone activity and bone densitometry were recorded as previously described.20
All patients meeting the inclusion criteria were offered percutaneous vertebroplasty.20,21 Patients who declined vertebroplasty and agreed to longitudinal evaluation constituted our control group. Among the main reasons for declining vertebroplasty was the lack of published data on the safety of the procedure.
All patients were offered similar analgesia. Pain management was titrated according to individual need. All patients also received anti-osteoporotic medications such as oral alendronate 70 mg weekly (n = 57) or intravenous pamidronate 60 mg 6 monthly (n = 69), together with elemental calcium 1200 mg daily and ergocalciferol 0.25 μg daily (if vitamin D deficient). Pamidronate was given to patients with corticosteroid-induced osteoporosis or those who refused or were intolerant to alendronate.
Compliance with follow-up was encouraged throughout the study.
Fracture-related complications, visual analogue pain score,22 and the level of function (using the Barthel Index)23 were assessed on presentation, at 24 hours, 6 weeks, 6–12 months and 24 months after therapy. These times were calculated from the day of vertebroplasty or the day of enrolment into the study.
The total number of hospital bed-days was recorded for both groups.
Causes of death were ascertained from the patients’ hospital records and from death certificates, and classified as either all cause-related, or fracture-related if occurring within 6 months of the fracture (eg, pneumonia, thromboembolus, septicaemia and sudden unexplained cardiorespiratory arrest).
Semiquantitative vertebral morphometry was obtained from review of thoraco-lumbar spinal radiographs (T4 – L5) performed at baseline and at 12 and 24 months after enrolment. The radiographs were evaluated by an independent observer (C B) and used to determine the degree of vertebral compression24 and the presence of new compression fractures.25
New (incident) vertebral fractures were defined as a decrease (compared with baseline radiographs) of 20% or more, and at least 4 mm, in any of the three vertebral heights (anterior, middle or posterior) on follow-up.
We arbitrarily defined a new clinical event as recurrent back pain occurring more than 6 weeks after initial presentation.
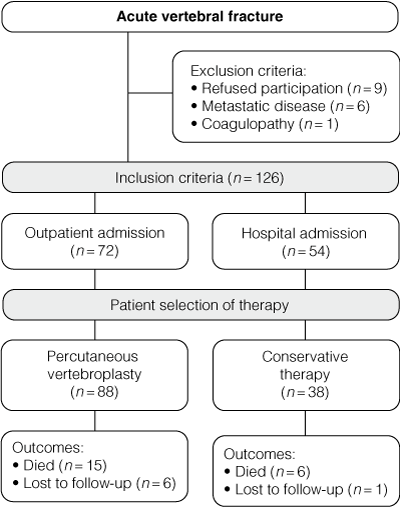
Percutaneous vertebroplasty was performed in 88 (70%) patients and conventional therapy was chosen by 38 (30%) patients. Thirty-nine men and 87 women, aged 51–95 years were followed up for a mean of 629 days (range, 42–730). Of these, 21 (17%) died during the study and 7 (6%) were lost to follow-up (Box 1).
Box 2 compares the demographic characteristics, osteoporotic risk factors, the results of bone densitometry and spinal radiography of the two groups. All patients had severe osteoporosis. The groups were similar with respect to their mean ages, height, weight, and pattern of referral, osteoporotic risk factors, serum biochemistry and mean period of observation. Vitamin D deficiency (defined as serum levels of 25-hydroxyvitamin D < 50 nmol/L) was common in both groups (49%–66%). Of the 54 hospital inpatients, 41 were treated by percutaneous vertebroplasty and 13 conservatively.
Percutaneous vertebroplasty was performed on 133 vertebrae, comprising 80 thoracic (T5 = 4; T6 = 9; T7 = 10; T8 = 12; T9 = 18; T10 = 9; T11 = 4 and T12 = 14) and 53 lumbar vertebrae (L1 = 18; L2 = 9; L3 = 14; L4 = 6 and L5 = 6). One vertebra was injected in 57 patients, two vertebrae in 21 patients, three in 10 patients and 4 in one patient.
The number of pre-existing vertebral fractures, their distribution and the degree of vertebral compression were similar in both groups. There were 58 patients (66%) in the vertebroplasty group compared with 22 controls (58%) who had radiological evidence of two or more adjacent vertebral fractures on baseline radiographs (χ2 = 0.73, P = 0.39).
Box 3 gives data for fracture outcome in patients treated by percutaneous vertebroplasty compared with conservative measures. A 60% reduction in pain scores (P < 0.001) and a 29% improvement in physical functioning (P < 0.001) were noted at 24 hours after percutaneous vertebroplasty, with no significant changes recorded in the patients treated conservatively (P < 0.01, compared with the changes after percutaneous vertebroplasty). Lower pain scores persisted in the vertebroplasty-treated group at 6 weeks (P < 0.01), but no differences between groups were evident at 6–12 and 24 months. Men showed significantly greater improvement in pain scores at 24 hours after vertebroplasty compared with women (+57% versus +37%, P < 0.01). No significant changes were seen between hospital inpatients versus outpatients, vitamin D-deficient versus vitamin D-replete patients, corticosteroid- versus non-corticosteroid-treated patients and pamidronate- versus alendronate-treated patients.
There were three minor complications in the vertebroplasty group (two fractured transverse processes and one psoas muscle haematoma). There were no major complications. The mean number of hospital bed-days for patients treated by percutaneous vertebroplasty (10.4 days; 95% CI, 8–13 days) was on average 43% less than for patients treated conservatively (17.5 days; 95% CI, 11–24 days).
Forty new vertebral fractures occurred in 30 patients. Eighteen were symptomatic and 11 of these were treated by further percutaneous vertebroplasty. Twenty-nine new vertebral fractures were noted in 21 patients (24%) treated by percutaneous vertebroplasty and 11 new vertebral fractures in nine patients (24%) treated conservatively. The hazard ratio for new vertebral fractures for those treated by percutaneous vertebroplasty (compared with the control group) was 1.13 (95% CI, 0.52–2.46; P = 0.76) (Box 4). There was no significant difference in the risk of new vertebral fractures in the two groups. No specific risk factors were identified by either univariate or multivariate analysis (data not shown). Nine patients (43%) in the vertebroplasty group and four control patients (44%) had radiological evidence of a new vertebral fracture adjacent to the initial acute osteoporotic fracture (χ2 = 0.41; P = 0.52).
There were 21 deaths (17%) during the 2-year study period, with 15 occurring in patients treated by percutaneous vertebroplasty. The hazard ratio for death in those who were treated by percutaneous vertebroplasty compared with the control group was 1.07 (95% CI, 0.42–2.76; P = 0.89) (Box 5). There was no significant difference in the risk of deaths in the two groups.
Specific risk factors identified in relation to all-cause mortality included patients’ age, history of corticosteroid therapy, and hospital admission (Box 6). Eight patients died from haematological or solid organ malignancies. There were five fracture-related deaths (4%), with four occurring in patients treated conservatively (χ2 = 5.95; P = 0.014). Considering only those patients whose death was fracture-related (with deaths due to other causes treated as censored), the hazard ratio for those who were treated by percutaneous vertebroplasty compared with the control group was 0.11 (95% CI, 0.01–0.96, P = 0.046); this was significantly different. In addition, there were other risk factors related to fracture death such as age and vitamin D deficiency (data from univariate analysis not shown).
While there are numerous published studies reporting the efficacy of percutaneous vertebroplasty,3-15 ours is the only prospective study to date which includes a control group.
We found that vertebroplasty-treated patients had better outcomes at 24 hours and at 6 weeks after the procedure, and experienced a rapid return to normal function as assessed by the Barthel Index. Although both treatment groups reached the near maximal Barthel score of 20 beyond 6 weeks, the vertebroplasty-treated patients achieved this score sooner.
Similar benefits in outcomes have been reported in a vertebroplasty-treated cohort of 97 patients followed up for 6–44 months,10 and a number of studies have shown both short < 6 months5,13,15 and mid-term (< 2 years)4,6,10,14,20 benefits of percutaneous vertebroplasty.
Between 2%–10% of all patients with vertebral fractures require hospitalisation. We elected to treat patients by percutaneous vertebroplasty early after their acute event. This led to a dramatic response and resulted in a significant reduction in analgesia use (data previously published),20 and a 43% reduction in the total number of hospital bed-days.
The benefit of percutaneous vertebroplasty is largely dependent on patient selection, operator skills and complication rates. The recent Guidelines for percutaneous vertebroplasty published by the Society of Interventional Radiology Standards of Practice Committee give the indications and contraindications.12 We elected to perform vertebroplasty as early as 1–2 weeks after the fracture, whereas other centres perform vertebroplasties after 3–9 months of failed conservative management.8,10-13
Percutaneous vertebroplasty for acute osteoporotic fractures is not without risk. In our study, three patients (3.4%) experienced minor complications. There were no major complications.
The effect of vertebroplasty on future fracture incidence is contentious.6,18,19 Legroux-Gerot and colleagues have reported a non-significant 3.1-fold (95% CI, 0.51–19.6) increase in risk of new vertebral fractures adjacent to vertebroplasty in 16 patients followed up for 35 months.14 On the other hand, Grados et al26 in a retrospective series also claimed a small (1.4-fold) but non-significant increase in vertebral fracture in the vicinity of a previous cemented vertebra. As neither study had a control group, it was not possible to determine whether the new fractures reflected the natural history of the disease or were related to the vertebroplasty procedure. Our study suggests that fracture incidence is not increased by vertebroplasty.
Vertebral fractures are predictive of other vertebral fractures.27 The 1-year risk of a second vertebral fracture (incident) after a first documented fracture is almost 20%.28 Forty new vertebral fractures were noted in 30 of our patients over the 2-year period. The risk of new vertebral fractures for those treated by percutaneous vertebroplasty was not significantly different from the risk in the conservatively treated group (hazard ratio, 1.13; 95% CI, 0.52–2.46). Vitamin D deficiency, multiple pre-existing vertebral fractures and very low lumbar spine bone density T-scores were evident in our cohort, but no specific risk factors could be identified. Future long-term controlled trials with sufficient statistical power are required to determine the fracture risk associated with percutaneous vertebroplasty.
Vertebral fractures are associated with a 16% reduction in expected 5-year survival.29 In a prospective study of women with clinical vertebral fractures, the age-adjusted relative risk of death (with 4 years follow-up) was 8.6.30 There were 21 deaths (17%) in our 2-year study, with no significant increases noted in the vertebroplasty-treated patients. While percutaneous vertebroplasty appeared to significantly reduce the risk of dying from fracture-related complications, the numbers were small, with only five fracture-related deaths occurring. Larger studies are required to verify this potential benefit of percutaneous vertebroplasty.
The drawbacks of our study include the non-randomised design, with patients recruited on the basis of consenting or refusing to have vertebroplasty. Clinical demographic and risk factors were similar in both groups, and both were evaluated longitudinally over the same period and all patients received the same medical care. Currently, randomised, prospective, controlled trials are in progress in Australia, the Netherlands and North America, comparing percutaneous vertebroplasty with a controlled intervention (“sham vertebroplasty”).31 All are having difficulty in recruiting patients because of the perceived benefit of the vertebroplasty procedure.32
We await new data from these trials to provide level-I evidence for the benefits of percutaneous vertebroplasty.
1 Study recruitment, treatment selection and outcomes of patients treated by either percutaneous vertebroplasty or conservative therapy
2 Clinical demographics, osteoporotic risk factors and bone densitometry data for patients with acute vertebral fractures, by type of therapy (data are expressed as mean ± 1 SD or as percentages)
|
Vertebroplasty (n = 88) |
Conservative therapy (n = 38) |
P |
||||||||||||
Sex ratio (men : women) |
32 : 56 |
7 : 31 |
0.08 |
||||||||||||
Inpatients* |
41 (47%) |
13 (34%) |
0.27 |
||||||||||||
Age (years) |
76.8 ± 8.7 |
76.1 ± 10.0 |
0.66 |
||||||||||||
Weight (kg) |
63.7 ± 12.1 |
65.2 ± 16.4 |
0.55 |
||||||||||||
Height (cm) |
159.9 ± 8.2 |
157.1 ± 7.0 |
0.09 |
||||||||||||
Smokers |
11 (13%) |
4 (11%) |
0.73 |
||||||||||||
Alcohol excess |
15 (17%) |
6 (16%) |
0.87 |
||||||||||||
Corticosteroid therapy |
25 (28%) |
9 (24%) |
0.70 |
||||||||||||
Vitamin D deficiency |
43 (49%) |
25 (66%) |
0.12 |
||||||||||||
Secondary hyperparathyroidism |
29 (33%) |
19 (50%) |
0.08 |
||||||||||||
Lumbar spine T-score |
− 3.9 ± 1.1 |
− 3.3 ± 1.5 |
0.01 |
||||||||||||
Femoral neck T-score |
− 2.6 ± 1.1 |
− 2.4 ± 1.0 |
0.32 |
||||||||||||
Pre-existing fractures† |
3.5 ± 1.8 |
3.1± 1.6 |
0.23 |
||||||||||||
Vertebral compression |
44 ± 16% |
45 ± 17% |
0.98 |
||||||||||||
* Includes patients admitted to hospital with back pain. † Calculated from the sum of the pre-existing vertebral fractures per patient. |
|||||||||||||||
3 The changes in pain score and physical functioning in patients treated with acute vertebral fractures. Values are expressed as mean ± 1 SD
|
Vertebroplasty (n = 88) |
Conservative therapy (n = 38) |
P |
||||||||||||
Pain scores |
|
|
|
||||||||||||
0 hours |
20 ± 4 |
20 ± 5 |
0.77 |
||||||||||||
24 hours |
8 ± 4† |
19 ± 5 |
0.001 |
||||||||||||
Percentage change* |
− 60% |
− 5% |
0.001 |
||||||||||||
6 weeks |
5 ± 4† |
7 ± 5‡ |
0.004 |
||||||||||||
Percentage change* |
− 75% |
− 65% |
0.002 |
||||||||||||
6–12 months |
3 ± 4† |
4 ± 5‡ |
0.17 |
||||||||||||
Percentage change* |
− 85% |
− 80% |
0.36 |
||||||||||||
24 months |
2 ± 3† |
3 ± 3‡ |
0.72 |
||||||||||||
Percentage change* |
− 90% |
− 85% |
0.85 |
||||||||||||
Physical functioning |
|
|
|
||||||||||||
0 hours |
14 ± 4 |
14 ± 4 |
0.81 |
||||||||||||
24 hours |
18 ± 3† |
14 ± 3 |
0.001 |
||||||||||||
Percentage change* |
+ 29% |
0 |
0.001 |
||||||||||||
6 weeks |
19 ± 2† |
18 ± 3‡ |
0.02 |
||||||||||||
Percentage change* |
+ 36% |
+ 29% |
0.29 |
||||||||||||
6–12 months |
19 ± 1† |
19 ± 2‡ |
0.20 |
||||||||||||
Percentage change* |
+ 36% |
+ 36% |
0.22 |
||||||||||||
24 months |
19 ± 2† |
19 ± 2‡ |
0.60 |
||||||||||||
Percentage change* |
+ 36% |
+ 36% |
0.36 |
||||||||||||
* Percentage change from baseline is calculated as the difference between the baseline and recorded values (at 24 hours, 6 weeks, 6–12 and 24 months) and expressed as a percentage of the baseline value. † P < 0.001 compared with measurements before percutaneous vertebroplasty. ‡ P < 0.001 compared with measurements at 24 hours after commencing conservative therapy. |
|||||||||||||||
4 Kaplan-Meier curve showing the unadjusted fracture-free survival in patients treated by either percutaneous vertebroplasty (solid line) or conservative therapy (stippled line)
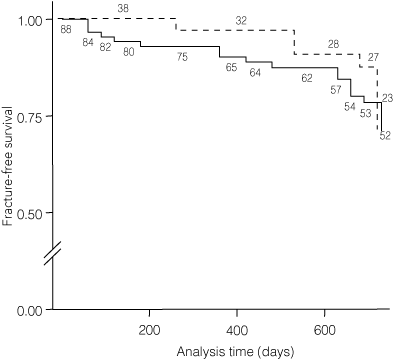
Log-rank test: χ2= 0.09, P = 0.76.
5 Kaplan-Meier curve showing the unadjusted death rates from all-cause mortality in patients treated by either percutaneous vertebroplasty (solid line) or conservative therapy (stippled line)
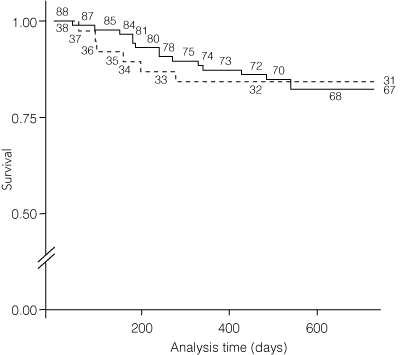
Log-rank test: χ2 = 0.02, P = 0.89.
6 Data from multivariate analysis showing the most important predictors of all-cause mortality
Variable |
Hazard ratio |
95% CI |
|||||||||||||
Age |
1.09 |
1.02–1.17* |
|||||||||||||
Corticosteroid therapy |
4.72 |
1.9–11.7* |
|||||||||||||
Hospital admission |
5.96 |
1.98–17.94* |
|||||||||||||
* P < 0.01. |
|||||||||||||||
Received 4 September 2005, accepted 25 November 2005
- 1. Melton LJ, Thamer M, Ray NF, et al. Fractures attributable to osteoporosis: Report from the National Osteoporosis Foundation. J Bone Miner Res 1997; 12: 16-23.
- 2. Ross P. Clinical consequences of vertebral fractures. Am J Med 1997; 103: 30S-43S.
- 3. Cotton A, Boutry N, Cortet B, et al. Percutaneous vertebroplasty: state of the art. Radiographics 1998; 18: 311-320.
- 4. Cortet B, Cotton A, Boutry N, et al. Percutaneous vertebroplasty in the treatment of osteoporotic vertebral compression fractures: an open prospective study. J Rheumatol 1999; 26: 2222-2228.
- 5. Martin JB, Jean B, Sugiu K, et al. Vertebroplasty: clinical experience and follow-up results. Bone 1999; 25 (Suppl): 11S-15S.
- 6. Grados F, Depriester C, Cayrolle G, et al. Long-term observations of vertebral osteoporotic fractures treated by percutaneous vertebroplasty. Rheumatology 2000; 39: 1410-1414.
- 7. Mathis JM, Barr JD, Belkoff SM, et al. Percutaneous vertebroplasty: a developing standard of care for vertebral compression fractures. Am J Neuroradiol 2001; 22: 373-381.
- 8. Murphy KJ, Lin DD. Vertebroplasty: a simple solution to a difficult problem. J Clin Densitom 2001; 4: 189-197.
- 9. Watts NB, Harris ST, Genant HK. Treatment of painful osteoporotic vertebral fractures with percutaneous vertebroplasty or kyphoplasty. Osteoporos Int 2001; 12: 429-437.
- 10. McGraw JK, Lippert JA, Minkus KD, et al. Prospective evaluation of pain relief in 100 patients undergoing percutaneous vertebroplasty: results and follow-up. J Vasc Interv Radiol 2002; 13: 883-886.
- 11. Kallmes DF, Jensen ME. Percutaneous vertebroplasty. Radiology 2003; 229: 27-36.
- 12. McGraw JK, Cardella J, Barr JD, et al. Society of Interventional Radiology Quality Improvement Guidelines for Percutaneous Vertebroplasty. J Vasc Interv Radiol 14(9 Pt 2): S311-S315. Available at: http://www.sirweb.org/clinical/cpg/S311.pdf (accessed Dec 2005).
- 13. Evans AJ, Jensen ME, Kip KE, et al. Vertebral compression fractures: pain reduction and improvements in functional mobility after percutaneous polymethylmethacrylate vertebroplasty: retrospective report of 245 cases. Radiology 2003; 226: 366-372.
- 14. Legroux-Gerot I, Lormeau C, Boutry N, et al. Long-term follow up of vertebral osteoporotic fractures treated by percutaneous vertebroplasty. Clin Rheumatol 2004; 23: 310-317.
- 15. McKiernan F, Faciszewski T, Jensen R. Quality of life following vertebroplasty. J Bone Joint Surg Am 2004; 86: 2600-2606.
- 16. Laredo JD, Hamze B. Complications of percutaneous vertebroplasty and their preventions. Skeletal Radiol 2004; 33: 493-505.
- 17. US Food and Drug Administration. FDA Public Health Web Notification: complications related to the use of bone cement and bone void fillers in treating compression fractures of the spine. Available at: http://www.fda.gov/cdrh/safety/bonecement.html (accessed Dec 2005).
- 18. Kim SH, Kang HS, Choi JA, Ahn JM. Risk factors of new compression fractures in adjacent vertebrae after percutaneous vertebroplasty. Acta Radiol 2004; 45: 440-445.
- 19. Anita A, Uppin MD, Joshua A, et al. Occurrence of new vertebral body fracture after percutaneous vertebroplasty in patients with osteoporosis. Radiology 2003; 226: 119-124.
- 20. Diamond TH, Champion B, Clark WA. Management of acute osteoporotic vertebral fractures: a nonrandomised trial comparing percutaneous vertebroplasty with conservative therapy. Am J Med 2003; 114: 257-265.
- 21. Diamond TH, Clarke WA. Percutaneous vertebroplasty: a novel treatment for acute vertebral fractures. Med J Aust 2001; 174: 398-400.
- 22. Melzack R. The McGill Pain Questionnaire: major properties and scoring methods. Pain 1975; 1: 277-299.
- 23. Mahoney FI, Barthel DW. Functional evaluation: the Barthel Index. Md State Med J 1965; 14: 61-65.
- 24. Genant HK, Wu CY, Van Kuijk C, Nevitt MC. Vertebral fracture assessment using a semiquantitative technique. J Bone Miner Res 1993; 8: 1137-1148.
- 25. Nevitt MC, Cummings SR, Stone KL, et al. Risk factors for first-incident radiographic vertebral fracture in women > 65 years of age: the study of osteoporotic fractures. J Bone Miner Res 2005; 20: 131-140.
- 26. Grados F, Depriester C, Cayrolle G, et al. Long-term observations of vertebral osteoporotic fractures treated by percutaneous vertebroplasty. Rheumatology 2000; 39: 1410-1414.
- 27. Klotzbeucher CM, Ross PD, Landsman PB, et al. Patients with prior fracture have an increased risk of future fracture: summary of the literature and statistical synthesis. J Bone Miner Res 2000; 15: 721-727.
- 28. Lindsay R, Silverman SL, Cooper C, et al. Risk of new vertebral fracture in the years following a fracture. JAMA 2001; 285: 320-323.
- 29. Cooper C, Atkinson EJ, Jacobsen SJ, et al. Population-based study of survival after osteoporotic fractures. Am J Epidemiol 1993; 137: 1001-1005.
- 30. Cauley JA, Thompson DE, Ensrud KC, et al. Risk of mortality following clinical fractures. Osteoporos Int 2000; 11: 556-561.
- 31. Vertebroplasty for the treatment of fractures due to osteoporosis. National Institutes of Health. Available at: http://www.clinicaltrials.gov/ct/show/NCT00068822?order=2 (accessed Dec 2005).
- 32. Kolata G. Spinal cement draws patients and questions. The New York Times 2005; 28 Aug. Available at: http://select.nytimes.com/gst/abstract.html?res=FA0E11F8345A0C7B8EDDA10894DD404482 (accessed Dec 2005).





Abstract
Objective: To assess the safety and efficacy of percutaneous vertebroplasty for the treatment of acute osteoporotic vertebral fractures.
Design: A prospective, non-randomised, “intention-to-treat” 2-year study.
Patients and setting: 126 consecutive patients (39 men and 87 women, aged 51–95 years) with acute osteoporotic vertebral fractures presenting to St George Hospital from November 2000 to December 2002. They comprised 88 patients treated by percutaneous vertebroplasty and 38 by conservative therapy.
Main outcome measures: Primary outcomes — changes in patients’ pain score and level of function recorded at 24 hours, 6 weeks, 6–12 months and 24 months after therapy. Secondary outcomes — occurrence of new clinical or radiological vertebral fractures and survival at 2 years.
Results: Three minor complications (fractured pedicle and psoas muscle haemorrhage) occurred in the vertebroplasty group during the first year of the study. Outcomes in vertebroplasty-treated patients (60% reduction in visual analogue pain scores from 20 to 8; P < 0.001), a rapid return to normal function (29% improvement in physical functioning from 14 to 18; P < 0.001) and lower rates of hospitalisation (43% reduction in the mean number of hospital bed-days occupied) were better than those treated conservatively (P < 0.001 for the comparison of all variables at 24 hours). Lower pain scores persisted in the vertebroplasty-treated group at 6 weeks (P < 0.001), but no differences between the two groups were evident at 12 and 24 months. In the vertebroplasty-treated group compared with the control group, the rates of new vertebral fractures (clinically and by radiographic assessment) (hazard ratio, 1.13; 95% CI, 0.52–2.46; P = 0.76) and death (hazard ratio, 1.07; 95% CI, 0.42–2.76; P = 0.89) showed no significant difference.
Conclusion: The analgesic benefit of percutaneous vertebroplasty and the low complication rates suggest that it is a useful therapy for acute painful osteoporotic vertebral fractures.