In the past decade, the prevalence of mental disorders in Australia, the number of individuals with identifiable mental health disorders who do not seek help, and the level of satisfaction with mental health services have remained unchanged.1 This is despite the roll-out of mental health awareness campaigns,2-4 school-based prevention programs,5 and substantial rearrangement of primary care-based mental health services, including improved access to psychological therapies.6,7 The most important figure, however, is that in 2007, only 35% of those with a mental disorder in the previous 12 months received any care for their disorder.1 In 1997, the rate of provision of mental health treatments was 38%.8 By comparison, over 80% of people with common physical disorders receive care in any 12-month period.9
Mental health and community advocates have targeted improved access to care as the dominant theme for reform of mental health services in this country.10-13 Clearly, our reliance over recent years on restructuring existing models of primary and secondary care has failed to deliver. A variety of issues have contributed to this failure, including the relative underutilisation of traditional primary care for mental health problems by young people and those who are disadvantaged by socioeconomic or geographical factors.14-16 Presentation for mental health care through medically orientated primary health care services is often perceived as stigmatising, disempowering or irrelevant to those with mental disorders.1,17,18 In addition, other dysfunctional elements of the Australian Medicare-based system create considerable professional and service barriers.19 In particular, the fee-for-service-orientated system has not supported the development of the style of collaborative care practice that is required in mental health.20,21
Recent policy documents suggest that e-mental health services may provide improved access to evidence-based help for those who currently lack access to basic treatments.22 E-health services offer information or therapy remotely through the internet or by telephone. These services range from health promotion, early intervention for non-clinical conditions, and provision of support to those with mental health problems through chat groups, to clinical treatment provided through the internet by mental health professionals. The Fourth National Mental Health Plan called for innovative service development using new technologies.23 Additionally, the final report of the National Health and Hospitals Reform Commission called for reform in the “smart use of data, information and communication”;24 the National Primary Health Care Strategy25 supported the efficient and effective use of e-health; and the 2008 National E-Health Strategy echoed the importance of better use of technology and national health knowledge portals.26
With respect to treatment, there is increasing evidence that internet-delivered treatments are effective, efficient and cost-effective for anxiety (social anxiety, panic disorder), depression, post-traumatic stress disorder, eating disorders, and obsessive-compulsive disorder, using cognitive behaviour therapy, psychoeducation and/or exposure techniques (see Griffiths et al, ).27 Currently, the preferred model for the delivery of e-mental health programs for treatment is in partnership with existing primary care or local general practice systems (see Hickie et al, ) or through a virtual clinic environment supervised by health professionals (see Andrews and Titov, ).28,29 There is a danger in this view that the preferred model of delivery will become dominant or be considered mandatory. This promotes an overly narrow view of how e-treatment can be provided and is contrary to the evidence that automated interventions or self-help treatments can be effective (see Griffiths et al).27 Moreover, it is likely to create bottlenecks and thus unduly restrict access to care — the very problem that providing direct access to internet programs is trying to redress.
An alternate model is one where comprehensive e-health services are mounted on an internet platform and offered through free open access to a “one-stop shop” or e-health portal. Open access provides the opportunity for self-help but also for maintaining a key sense of control over one’s own health and use of health services. These features are considered to be the new tier of a more comprehensive and consolidated health system.30 They derive from the concept described in Ferguson’s pioneering contribution,31 where the consumer has a central role in managing his or her own health. If combined with useful information, timely feedback, peer support and appropriate social marketing, e-health portals (and related applications) are likely to encourage help seeking in ways that conventional health services are unlikely to emulate. The connectivity of the internet allows direct involvement in ways not previously possible.
The provision of e-health portal services is not designed to compete with or decrease the current level of face-to-face treatment. In fact, it is likely that for many users it will simply be the first step towards access to more traditional person-based services. The overt goal is to “increase participation ... among individuals who might not otherwise seek care”.32 The very nature of these applications capitalises on anonymous and easy access for people with stigmatised health problems. Groups such as young people,18 men, armed forces personnel,33 and those who have had previously stigmatising or disempowering experiences are likely to prefer not only the anonymity but also the capacity to use these services privately at home, work, school or other non-clinical settings, and will place additional value on the lack of face-to-face contact.
As has been noted previously, a lack of face-to-face contact may actually be associated with increased rates of revelation of key symptoms (eg, suicidal risk)34 or past traumatic events (eg, sexual abuse). Further, within some cultural contexts, such methods of interaction may not only be associated with less personal embarrassment or guilt but also less familial or collective shame.
In addition to treatment goals, there is a wider recognition that current mental health policy goals must also include a focus on health promotion and primary and secondary prevention. Web-based technologies are uniquely placed to deliver primary prevention, early intervention and secondary prevention services to whole populations. Recent studies indicate that prevention using e-applications is effective.35 E-health technologies have enormous advantages in population-based approaches designed to reduce disease burden primarily because they permit widespread dissemination of effective programs at low cost. Given that 75% of major mental health problems commence before the age of 25 years and 50% are evident before the age of 15 years,36 e-health applications have the clear benefit of being attractive to and easily accessed by young people. Young people already use the internet as a major source of health information and, as described elsewhere in this Supplement (see Burns et al, ),37 Australian youth readily report that they use a wide variety of internet-based services to meet their mental health needs.
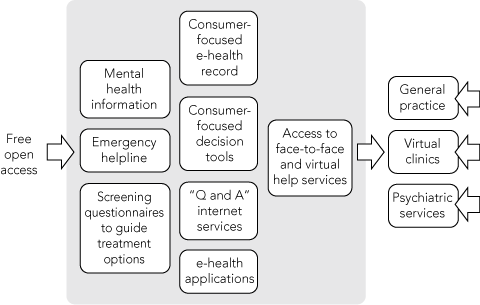
One new model to provide health promotion, prevention, access to services and direct help involves the use of an e-health portal. The e-mental health portal model shown in Box 1 is based on an earlier model developed by the e-mental health sector.22 The central features of the portal are entry to a range of services and referral to appropriate face-to-face and e-health services, once relevant information and opportunities for self-help have been offered.
The portal firstly provides an entry point to: explore the nature of mental health problems through the provision of quality information; determine levels of mental health symptoms through the use of screening questionnaires; make use of consumer-focused decision tools (by which to establish self-help or professional health care routes); and provide direct access to evidence-based, online software programs that offer treatment or prevention programs. The portal also provides access to “question and answer” email or telephone services, with replies offered immediately or within a set period such as 24 or 48 hours. Thirdly, the portal incorporates an emergency helpline, through which individuals can receive counselling services or be directed to “bricks and mortar” services such as general practices, regional headspace centres, private medical services, hospitals and so on. (There are currently 30 headspace centres in Australia, offering a youth-friendly service provided by youth workers, with access to psychologists, general practitioners and psychiatrists.) The portal might also offer access to a consumer-generated (as opposed to institutionally generated) electronic health record. The ability to create consumer-generated records is already being offered directly to people — examples include Google Health (http://www.google.com/health) and HealthSpace (http://www.healthspace.nhs.uk), developed by the National Health Service in the United Kingdom. These software applications allow people to keep track of personal health information, which can then be shared with doctors and other providers. Because of its focus on prevention as well as treatment, the e-health portal is designed to target high-prevalence disorders such as anxiety and depression, while also providing a pathway to more specialist services for those with psychosis or severe depression disorders.
Importantly, the portal is not seen to be the exclusive pathway to care for mental health disorders. Consumers and patients will continue to access health care in general practice and through hospital departments (represented in Box 1 by the reverse arrows on the right). However, the portal provides an entry point for consumers to information, self-help, counselling and other services, and the opportunity to choose from a range of traditional and other health services. The portal will also have efficiencies, allowing (at least in principle) a better distribution of higher-risk patients into general practice or psychiatry settings. The portal will be manned by health professionals and volunteers offering appropriate services. For example, crisis intervention services will be provided by volunteer counsellors. Psychiatrists might be called on to make critical decisions regarding treatment options, particularly for people in crisis or at risk. Potentially, sets of checks can be programmed to ensure that individuals do not “get lost in the system”. Appropriate monitoring can be built in to reconnect with individuals who provide contact details. The aim is to provide timely, evidence-based assistance to all portal users whether they are browsing for information, in urgent need of help, reconnecting with mental health services, or seeking help for friends or family. The portal can also proactively check that individuals are helped, or at the very least followed up, if they have requested this or in some cases where they have been assessed as needing services urgently. The processes and the software underpinning these health pathways will need to be secure and ethical, reach standards of practice, and be monitored regularly.
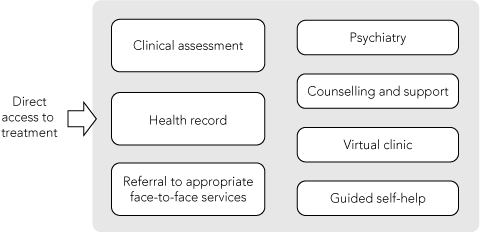
A potential model for such specialised services is illustrated in Box 2. The key characteristic here is the willingness of specialised providers to enter into an online treatment relationship with consumers who have complex, severe or ongoing disorders, and also to accept that these people may never present in person for conventional care. Such systems may be able to work with a wider network of locally based health service providers to enhance care, but should not rely on such partnerships to deliver care. Consequently, all aspects of care need to be adapted to the e-health environment, including issues related to adequacy of assessment, provision of personalised health information, access to emergency care, provision and monitoring of medications, monitoring of responses to treatments, engagement of family and carers, and promotion of long-term health and social outcomes. While challenging in scope, it may well be the case that the combination of a concentration of health experts in such environments and enhanced web-based technologies translates into a more attractive and more functional treatment service than our current place-based models.
- Helen Christensen1
- Ian B Hickie2
- 1 Centre for Mental Health Research, Australian National University, Canberra, ACT.
- 2 Brain & Mind Research Institute, University of Sydney, Sydney, NSW.
Helen Christensen is funded by National Health and Medical Research Council (NHMRC) Fellowship 525411. Ian Hickie holds an NHMRC Australia Fellowship.
None identified.
- 1. Meadows GN, Burgess PM. Perceived need for mental health care: findings from the 2007 Australian Survey of Mental Health and Wellbeing. Aust N Z J Psychiatry 2009; 43: 624-634.
- 2. Hickie IB. Preventing depression: a challenge for the Australian community. Med J Aust 2002; 177 (7 Suppl): S85-S86. <MJA full text>
- 3. Pirkis J, Hickie I, Young L, et al. An evaluation of beyondblue, Australia’s national depression initiative. Int J Ment Health Promot 2005; 7: 35-53.
- 4. Highet NJ, Luscombe GM, Davenport TA, et al. Positive relationships between public awareness activity and recognition of the impacts of depression in Australia. Aust N Z J Psychiatry 2006; 40: 55-58.
- 5. Wyn J, Cahill H, Holdsworth R, et al. MindMatters, a whole-school approach promoting mental health and wellbeing. Aust N Z J Psychiatry 2000; 34: 594-601.
- 6. Hickie IB, Pirkis JE, Blashki GA, et al. General practitioners’ response to depression and anxiety in the Australian community: a preliminary analysis. Med J Aust 2004; 181 (7 Suppl): S15-S20. <MJA full text>
- 7. Morley B, Pirkis J, Sanderson K, et al. Better outcomes in mental health care: impact of different models of psychological service provision on patient outcomes. Aust N Z J Psychiatry 2007; 41: 142-149.
- 8. Henderson S, Andrews G, Hall W. Australia’s mental health: an overview of the general population survey. Aust N Z J Psychiatry 2000; 34: 197-205.
- 9. Andrews G, Carter GL. What people say about their general practitioners’ treatment of anxiety and depression. Med J Aust 2001; 175 (2 Suppl): S48-S51.
- 10. Hickie IB, Groom GL, McGorry PD, et al. Australian mental health reform: time for real outcomes. Med J Aust 2005; 182: 401-406. <MJA full text>
- 11. Hickie IB, McGorry PD. Increased access to evidence-based primary mental health care: will the implementation match the rhetoric? Med J Aust 2007; 187: 100-103. <MJA full text>
- 12. McGorry PD, Tanti C, Stokes R, et al. headspace: Australia’s National Youth Mental Health Foundation — where young minds come first. Med J Aust 2007; 187 (7 Suppl): S68-S70. <MJA full text>
- 13. Rosenberg S, Hickie IB, Mendoza J. National mental health reform: less talk, more action. Med J Aust 2009; 190: 193-195. <MJA full text>
- 14. Hickie IB, Davenport TA, Scott EM, et al. Unmet need for recognition of common mental disorders in Australian general practice. Med J Aust 2001; 175 (2 Suppl): S18-S24.
- 15. Hickie IB, Davenport TA, Naismith SL, et al. Treatment of common mental disorders in Australian general practice. Med J Aust 2001; 175 (2 Suppl): S25-S30.
- 16. Hickie IB, Fogarty AS, Davenport TA, et al. Responding to experiences of young people with common mental health problems attending Australian general practice. Med J Aust 2007; 187 (7 Suppl): S47-S52. <MJA full text>
- 17. Hickie IB, Luscombe GM, Davenport TA, et al. Perspectives of young people on depression: awareness, experiences, attitudes and treatment preferences. Early Interv Psychiatry 2007; 1: 333-339.
- 18. Cohen A, Medlow S, Kelk N, et al. Young people’s experiences of mental health care: implications for the headspace: National Youth Mental Health Foundation. Youth Stud Aust 2009; 28: 13-20.
- 19. Hickie I, Davenport T, Luscombe G, et al. Is real reform of the Medicare Benefits Schedule for psychiatrists in Australia economically, socially or professionally desirable? Australas Psychiatry 2006; 14: 8-14.
- 20. Scott E, Naismith S, Whitwell B, et al. Delivering youth-specific mental health services: the advantages of a collaborative multi-disciplinary system. Australas Psychiatry 2009; 17: 189-194.
- 21. Board on Health Care Services, Institute of Medicine (US). Improving the quality of health care for mental and substance-use conditions: quality chasm series. Washington, DC: National Academies Press, 2006.
- 22. Christensen H, Proudfoot J, Andrews G, et al. E-mental health: a 2020 vision and strategy for Australia. http://www.ehub.anu.edu.au/workshop2009_presentations/Emental_Health_2020_Vision_and_Strategy_for_Australia.pdf (accessed May 2010).
- 23. Fourth National Mental Health Plan Working Group. Fourth National Mental Health Plan: an agenda for collaborative government action in mental health 2009–2014. Canberra: Commonwealth of Australia, 2009. http://www.health.gov.au/internet/main/publishing.nsf/Content/mental-pubs-f-plan09 (accessed May 2010).
- 24. National Health and Hospitals Reform Commission. A healthier future for all Australians: final report June 2009. Canberra: Department of Health and Ageing, 2009.
- 25. Australian Government Department of Health and Ageing. Towards a National Primary Health Care Strategy: a discussion paper from the Australian Government. Canberra: Commonwealth of Australia, 2008.
- 26. Deloitte National E-Health and Information Principal Committee. National E-Health Strategy. Canberra: Department of Health and Ageing, 2008. http://www.health.gov.au/internet/main/publishing.nsf/Content/National+Ehealth+Strategy (accessed May 2010).
- 27. Griffiths KM, Farrer L, Christensen H. The efficacy of internet interventions for depression and anxiety disorders: a review of randomised controlled trials. Med J Aust 2010; 192 (11 Suppl): S4-S11. <MJA full text>
- 28. Hickie IB, Davenport TA, Luscombe GM, et al. Practitioner-supported delivery of internet-based cognitive behaviour therapy: evaluation of the feasibility of conducting a cluster randomised trial. Med J Aust 2010; 192 (11 Suppl): S31-S35. <MJA full text>
- 29. Andrews G, Titov N. Is internet treatment for depressive and anxiety disorders ready for prime time? Med J Aust 2010; 192 (11 Suppl): S45-S47. <MJA full text>
- 30. Coiera E. Four rules for the reinvention of health care. BMJ 2004; 328: 1197-1199.
- 31. Ferguson T. Online patient-helpers and physicians working together: a new partnership for high quality health care. BMJ 2000; 321: 1129-1132.
- 32. Ruggiero KJ, Resnick HS, Acierno R, et al. Internet-based intervention for mental health and substance use problems in disaster-affected populations: a pilot feasibility study. Behav Ther 2006, 37: 190-205.
- 33. Wilson JAB, Onorati K, Mishkind M, et al. Soldier attitudes about technology-based approaches to mental health care. Cyberpsychol Behav 2008; 11: 767-769.
- 34. Barak A. Emotional support and suicide prevention through the Internet: a field project report. Comput Human Behav 2007; 23: 971-984.
- 35. Cuijpers P, van Straten A, Smit F, et al. Preventing the onset of depressive disorders: a meta-analytic review of psychological interventions. Am J Psychiatry 2008; 165: 1272-1280.
- 36. Kim-Cohen J, Caspi A, Moffitt TE, et al. Prior juvenile diagnoses in adults with mental disorder: developmental follow-back of a prospective-longitudinal cohort. Arch Gen Psychiatry 2003; 60: 709-717.
- 37. Burns JM, Davenport TA, Durkin LA, et al. The internet as a setting for mental health service utilisation by young people. Med J Aust 2010; 192 (11 Suppl): S22-S26. <MJA full text>





Abstract
Traditional clinic-based service delivery systems remain inaccessible to many Australians with mental health problems.
If we are to substantially reduce the burden of mental illness, we need to develop more accessible, empowering and sustainable models of mental health care.
E-health technologies have specific efficiencies and advantages in the domains of health promotion, prevention, early intervention and prolonged treatment.
It is timely to use the best features of these technologies to start to build a more responsive and efficient mental health care system.