Although major depression is the leading cause of health-related disability in Australia, access to appropriate forms of psychological treatment remains low.1 Cost-effective mental health interventions can now be delivered via the internet to broad sectors of society, including people who have limited access to clinical services due to geographic, economic or social barriers.2,3 MoodGYM, an Australian innovation, is an internet-based cognitive behaviour therapy (CBT) intervention designed to treat and prevent depression and anxiety.4 MoodGYM has been shown to reduce symptoms of depression and anxiety in people in the community and in school settings.5-7
We have previously demonstrated the lack of access to skilled psychological treatments in primary care settings.8 There is an urgent need to evaluate the potential effectiveness of internet-based therapies in clinical settings, including primary care. About 85% of adult Australians visit a general practitioner in any year, and GPs are most likely to be the first point of professional contact for most individuals with mental health problems.9 Although there is evidence that use of the internet to treat mental health problems is acceptable to both patients and doctors,10 internet-based programs have not been widely used to deliver mental health interventions in conjunction with traditional general practice. Since the introduction in 2001 of the federal government’s Better Outcomes in Mental Health Care (BOiMHC) initiative, greater emphasis has been placed on delivery of more sophisticated psychological assessment and active management by Australian GPs.11 Although the introduction of Medicare-based support for psychological services in late 2006 also increased access to professionally delivered mental health services, most people still rely largely on their GP to manage their psychological difficulties.12
GPs were trained using the introductory component of the SPHERE training program (run by Educational Health Solutions and sponsored by Pfizer Pharmaceuticals), coordinated through the Central Sydney Division of General Practice. The introductory component (“Depression and anxiety: an introductory training program for general practitioners”) provides GPs with the knowledge and skills required to effectively identify, treat and manage depression, anxiety and somatic distress in their practice.13,14 This highly interactive and discussion-based training program includes three seminars that focus on: psychological distress in general practice; diagnosis of specific psychological disorders; and management of depression and anxiety. More than 9000 GPs have had access to some aspect of the SPHERE training program over the past decade.
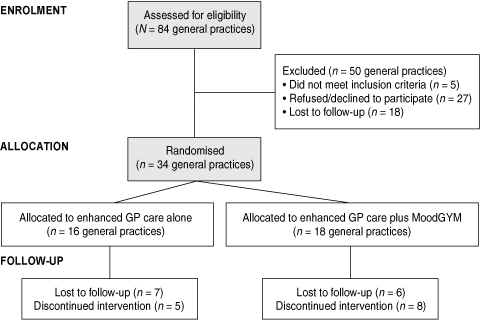
General practices were identified for participation in the study through the Central Sydney Division of General Practice, the national SPHERE database and advertising in relevant trade journals. Of 84 general practices (90 GPs) who participated in the initial assessment, 34 were randomly assigned to offer enhanced GP care plus MoodGYM or enhanced GP care alone. The cluster randomised trial design is shown in Box 1.
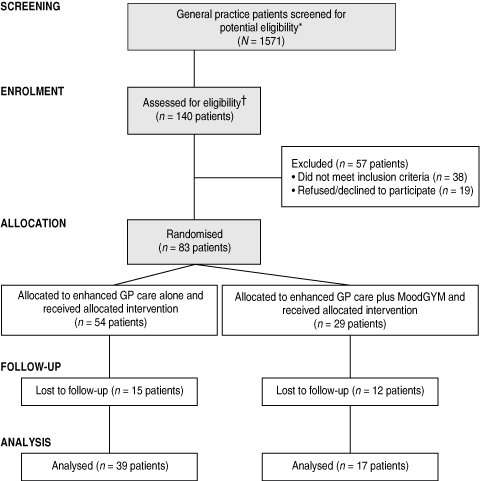
A research nurse was present within each practice on specific days and offered screening questionnaires to all patients before their appointment with the GP. In some practices, the practice manager was able to assist. Only those patients who scored positive for psychological distress (using an arbitrary cut-off score of at least 20 on the Kessler Psychological Distress Scale [K10],15 to capture all patients with high to very high levels of distress) and self-reported that they met other trial criteria were offered a follow-up appointment, and had their records flagged to alert the GP to their potential participation in the trial (Box 2). GPs then made a final determination of whether these patients were eligible for inclusion. The trial criteria included: age between 16 and 50 years (the upper age limit was used to eliminate potential confounding from patients presenting with age-related cognitive and behavioural decline); English as a first language; depressive symptoms not due to grief, and duration of less than 2 years; access to the internet; not currently enrolled in any other research project or receiving psychological or pharmacological care; and not having a major medical illness, psychomotor agitation, neurological impairment, head injury, lifetime alcohol or drug dependence or misuse, or a mixed depressive episode.
Once patients were recruited to the trial, they received either enhanced GP care plus MoodGYM or enhanced GP care alone (Box 2). Both interventions were delivered over about 8 weeks, with baseline and end-of-treatment assessments conducted by the research nurse. Follow-ups were also undertaken 6 months and 12 months after the intervention.
Data were collected from all GPs who initially enrolled in the trial and all patients who were screened. At enrolment, GPs reported individual demographics and practice characteristics. Patients who were screened for entry to the trial completed a survey that recorded demographic information and measured their current level of psychological distress with the 12-item Somatic and Psychological Health Report (SPHERE-12)16 and the K10. The K10 cut-off scores used in the 2000 Health and Wellbeing Survey and the 2001 National Health Survey to estimate the prevalence of levels of psychological distress were applied.17 Patients’ self-reported disability was also measured with the Brief Disability Questionnaire (BDQ).18
GP and patient demographics and general practice characteristics were analysed using simple descriptive statistics, χ2 analysis and independent samples t tests. SPHERE-12 and K10 scores over the course of the study were examined using Kaplan–Meier curves, which estimated the time to resolution of psychological symptoms for each intervention. To test for any clinically meaningful differences between interventions over time, Cohen’s d effect size was used. Cohen defined d as the difference between the means, divided by the standard deviation, of either group (effect sizes: small, d = 0.2–0.3; medium, d = 0.4–0.5; and large, d = 0.8 to infinity).19 Paired samples t tests were used to assess the relationship between BDQ “days out of role” before treatment and immediately after treatment, and between-condition differences were assessed using independent samples t tests.
Data were analysed using SPSS 17.0 for Windows (SPSS Inc, Chicago, Ill, USA).
Characteristics of the 90 GPs who enrolled in the trial are shown in Box 3. In addition to the SPHERE training, a quarter (22/88) indicated they had received other mental health training (eg, psychiatry training, a university Masters or Diploma course in psychological medicine).
Demographic data of the 1571 patients screened for potential eligibility for the trial are shown in Box 4. Of these patients, 84% had access to the internet for personal use, and over a fifth reported significant psychological distress (25% scored as Type 1 [substantial psychological and somatic symptoms] on the SPHERE-12, and 22% scored ≥ 22 [high to very high levels of psychological distress] on the K10). A further third of patients reported some significant psychological symptoms, with just under half reporting no symptoms.
Over the four study timepoints, full SPHERE-12 and K10 data were available for 56 of the 83 recruited patients (Box 5). Of the 27 patients who dropped out, 15 were recruited to the enhanced GP care alone condition (28% of that group), and 12 to the enhanced GP care plus MoodGYM condition (41% of that group). Participants who dropped out did not differ significantly from the rest of the participants in terms of sex or age (recruited patients v drop-out patients: female, 75% v 69%, χ2 = 0.29, P = 0.59; mean age, 38.8 years v 36.0 years, t = 0.55, P = 0.58).
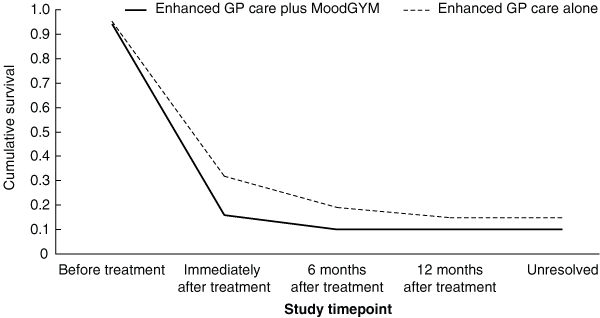
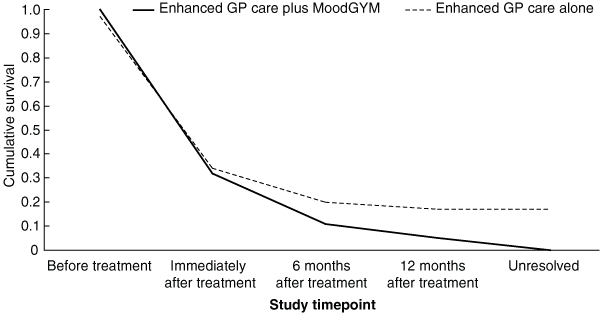
Box 6 and Box 7 illustrate the resolution of psychological symptoms over time, by condition, using survival functions. For most participants, symptoms resolved immediately after treatment, as assessed by both the SPHERE-12 and K10. More patients experienced a resolution of symptoms with enhanced GP care plus MoodGYM compared with enhanced GP care alone. This pattern was continued at 6 and 12 months after treatment.
Second, and much more challenging, is moving from engaging general practices in cross-sectional audits of practice to participation in complex treatment trials — even when this has been made simpler by randomising practices rather than patients (and where all patients therefore receive active and credible interventions). Even though this issue has been discussed for many years, our experience has been that conducting longitudinal or interventional mental health studies in Australian general practice remains extremely challenging. We suspect that without specific and targeted support from national health service development and evaluation agencies, such research will remain neglected.20,21
Despite these barriers, we remain committed to testing internet-based adjuncts to clinical care in real-world settings. Use of the internet provides an experience of psychological therapy between the face-to-face contacts with the practitioner. This active engagement of the subject in self-directed therapy supported by a health professional combines the recognised advantages of the internet (low cost, high availability and convenience, no limitations to volume of use, high-fidelity delivery of the structured and evidence-based content of the MoodGYM CBT program) and the non-specific treatment benefits of contact with a GP with recognised psychological assessment and management skills. The suggestion of differences between this combined therapy and practitioner-delivered therapy alone is consistent with other studies of the longer-term benefits of structured forms of CBT.3,22
Australians express a strong preference for non-pharmacological therapies as first-line treatments for common mental disorders.1 Given the current geographical, financial and other service-related difficulties that many people experience when trying to access psychological care through primary care settings,12,23 the development of internet-based therapies that may reduce such barriers is a key health-service development strategy. This preliminary study suggests that MoodGYM, when integrated with psychological care provided by a GP, may have advantages over enhanced GP care alone. This remains to be formally tested in a trial with sufficient power to detect meaningful clinical differences in long-term outcomes.
3 Characteristics of the 90 enrolled general practitioners
* Unless otherwise indicated. Denominators vary due to missing data. |
|||||||||||||||
5 Self-reported psychological symptoms over time for recruited patients*
Enhanced GP care alone (n = 39) |
Enhanced GP care plus MoodGYM (n = 17) |
||||||||||||||
- Ian B Hickie1
- Tracey A Davenport1
- Georgina M Luscombe1
- Michael Moore2
- Kathleen M Griffiths3
- Helen Christensen3
- 1 Brain & Mind Research Institute, University of Sydney, Sydney, NSW.
- 2 Central Sydney Division of General Practice, Sydney, NSW.
- 3 Centre for Mental Health Research, Australian National University, Canberra, ACT.
The MoodGYM GP trial (chief investigators: Helen Christensen, Kathleen Griffiths, Ian Hickie and Michael Moore) was funded by the Australian Government Department of Health and Ageing. The research was also supported by National Health and Medical Research Council Principal Research Fellowships 148947 and 366781. We are grateful to Zoe Richards, Wendy Rees and Andrea Fogarty for their research assistance with the study.
Helen Christensen and Kathleen Griffiths are the developers of the MoodGYM website.
- 1. Australian Bureau of Statistics. National Survey of Mental Health and Wellbeing: summary of results, 2007. Canberra: ABS, 2008. (ABS Cat. No. 4326.0.) http://www.abs.gov.au/AUSSTATS/abs@.nsf/mf/4326.0 (accessed Jun 2009).
- 2. Christensen H. Computerised therapy for psychiatric disorders. Lancet 2007; 370: 112-113.
- 3. Perini S, Titov N, Andrews G. Clinician-assisted Internet-based treatment is effective for depression: randomized controlled trial. Aust N Z J Psychiatry 2009; 43: 571-578.
- 4. MoodGYM [website]. http://moodgym.anu. edu.au (accessed Jun 2009).
- 5. Christensen H, Griffiths KM, Korten A. Web-based cognitive behavior therapy: analysis of site usage and changes in depression and anxiety scores. J Med Internet Res 2002; 4: e3.
- 6. Christensen H, Griffiths KM, Jorm AF. Delivering interventions for depression by using the internet: randomised controlled trial. BMJ 2004; 328: 265.
- 7. O’Kearney R, Kang K, Christensen H, Griffiths K. A controlled trial of a school-based Internet program for reducing depressive symptoms in adolescent girls. Depress Anxiety 2009; 26: 65-72.
- 8. Hickie IB, Davenport TA, Naismith SL, et al. Treatment of common mental disorders in Australian general practice. Med J Aust 2001; 175 (2 Suppl): S25-S30.
- 9. Burgess PM, Pirkis JE, Slade TN, et al. Service use for mental health problems: findings from the 2007 National Survey of Mental Health and Wellbeing. Aust N Z J Psychiatry 2009; 43: 615-623.
- 10. Titov N, Andrews G, Johnston L, et al. Shyness programme: longer term benefits, cost-effectiveness, and acceptability. Aust N Z J Psychiatry 2009; 43: 36-44.
- 11. Hickie IB, Pirkis JE, Blashki GA, et al. General practitioners’ response to depression and anxiety in the Australian community: a preliminary analysis. Med J Aust 2004; 181 (7 Suppl): S15-S20. <MJA full text>
- 12. Hickie IB, McGorry PD. Increased access to evidence-based primary mental health care: will the implementation match the rhetoric? Med J Aust 2007; 187: 100-103. <MJA full text>
- 13. Hickie I, Scott E, Ricci C, et al. Treating depression and anxiety in general practice: training manual. Sydney: Educational Health Solutions, 1998.
- 14. Naismith SL, Hickie IB, Scott EM, Davenport TA. Effects of mental health training and clinical audit on general practitioners’ management of common mental disorders. Med J Aust 2001; 175 (2 Suppl): S42-S47.
- 15. Kessler RC, Andrews G, Colpe LJ, et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol Med 2002; 32: 959-976.
- 16. Hickie IB, Davenport TA, Hadzi-Pavlovic D, et al. Development of a simple screening tool for common mental disorders in general practice. Med J Aust 2001; 175 (2 Suppl): S10-S17.
- 17. Australian Bureau of Statistics. Information paper: use of the Kessler Psychological Distress Scale in ABS health surveys, Australia, 2001. Canberra: ABS, 2003. (ABS Cat. No. 4817.0.55.001.) http://www.abs.gov.au/ausstats/abs@.nsf/mf/4817.0.55.001 (accessed Jun 2009).
- 18. Von Korff M, Ustun TB, Ormel J, et al. Self-report disability in an international primary care study of psychological illness. J Clin Epidemiol 1996; 49: 297-303.
- 19. Cohen J. Statistical power analysis for the behavioral sciences. 2nd ed. Hillsdale, NJ: Lawrence Erlbaum Associates, 1988.
- 20. Anderson WP, Papadakis EM. Research to improve health practice and policy. Med J Aust 2009; 191: 646-647. <MJA full text>
- 21. Mitchell RJ, McClure RJ, Olivier J, Watson WL. Rational allocation of Australia’s research dollars: does the distribution of NHMRC funding by National Health Priority Area reflect actual disease burden? Med J Aust 2009; 191: 648-652. <MJA full text>
- 22. Perini S, Titov N, Andrews G. The Climate Sadness program: an open trial of Internet-based treatment for depression. E-J Appl Psychol 2008; 4 (2): 18-24.
- 23. Rosenberg S, Hickie IB, Mendoza J. National mental health reform: less talk, more action. Med J Aust 2009; 190: 193-195. <MJA full text>





Abstract
Objective: To determine the feasibility of conducting a cluster randomised trial in Australia of the effectiveness of general practitioner-supported delivery of internet-based cognitive behaviour therapy (CBT) and enhanced psychological care.
Design, setting and participants: Cluster randomised trial involving patients attending general practices in Australia. Participating practices were randomly allocated to interventions. The study was conducted between January 2004 and January 2007.
Interventions: Enhanced GP care was delivered by doctors who had completed specific mental health training; the experimental condition consisted of enhanced GP care plus MoodGYM, an internet-based CBT intervention.
Main outcome measures: Demographic and behavioural characteristics of patients, and demographic and practice characteristics of GPs; time to resolution of psychological symptoms for patients involved in the longitudinal phase of the trial.
Results: 1571 patients attending 90 GPs from 84 general practices were identified as potentially suitable for recruitment. These patients had a mean age of 35 years, 76% were female, 84% had access to the internet for personal use, and 22% reported high or very high levels of psychological distress on the Kessler Psychological Distress Scale. The 90 GPs had a mean age of 49 years, 53% were female and 25% had completed formal mental health training. Of the 1571 screened patients, 340 reported high levels of psychological distress, but only 140 of these could be further assessed for eligibility in the trial. Of these 140, 83 patients with depression (attending 10 GPs in eight general practices) proceeded to randomisation. For these patients, the experimental intervention (enhanced GP care plus MoodGYM) tended to result in prompt and more sustained resolution of depressive symptoms.
Conclusion: Our capacity to conduct a definitive trial was limited by available resources. Preliminary data suggest that primary care patients with depression may derive additional benefits from an internet-based CBT program delivered in conjunction with enhanced psychological care from GPs.