To the Editor: Aboriginal and Torres Strait Islander people were more at risk of hospitalisation, admission to intensive care units and death during the 2009 influenza A pandemic than non-Indigenous Australians.1 We conducted a descriptive analysis of our response to the pandemic at Winnunga Nimmityjah Aboriginal Health Service (Winnunga) — an Aboriginal community controlled health service in Canberra, Australian Capital Territory, which provides comprehensive primary health care to more than 3500 patients per year. Data were sourced from the Winnunga electronic patient record system, pathology laboratories and ACT Health. The Winnunga Board approved this analysis and report for publication.
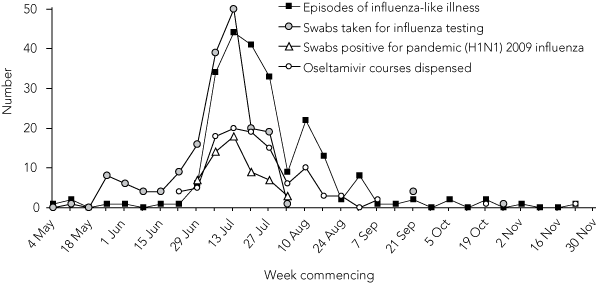
Increased testing for influenza commenced in late May. The first patient with pandemic (H1N1) 2009 influenza was identified on 1 July (Box). Of the 168 nasal swabs tested for influenza by polymerase chain reaction analysis, 52 (31%) were positive for pandemic (H1N1) 2009 influenza. In addition, six Winnunga patients tested positive at other locations. In late July, testing guidelines changed and laboratory testing was no longer recommended for most patients with influenza-like illness.2 Consequently, we did not identify test-positive cases past the beginning of August. The actual number of cases of pandemic influenza that occurred in Winnunga patients is unknown.
In July and August, 13% (204/1604) of all presenting patients at Winnunga had an influenza-like illness. There were 229 recorded episodes of influenza-like illness between May and November with a sharp peak in July and a smaller peak in August (Box).
Oseltamivir dispensing commenced 1 week before identification of the first patient who tested positive, and corresponded with episodes of influenza-like illness (Box). A total of 107 courses of oseltamivir were dispensed to 33 children and 74 adults. Clinical risk factors other than Aboriginal and Torres Strait Islander status were recorded for 47 of these patients. Oseltamivir dispensed to Winnunga patients at other locations was not included in our analysis. We do not know whether oseltamivir made a difference in reducing severity of disease or preventing hospitalisations in our patients.
- Ana Herceg1
- Peter G Sharp2
- Christine G Arthur3
- Julie A Tongs4
- Winnunga Nimmityjah Aboriginal Health Service, Canberra, ACT.
- 1. Kelly H, Mercer GN, Cheng AC. Quantifying the risk of pandemic influenza in pregnancy and Indigenous people in Australia in 2009. Euro Surveill 2009; 14 (5): pii=19441. http://www.eurosurveillance.org/ViewArticle.aspx?ArticleId=19441 (accessed Jan 2010).
- 2. Guest C. Management of suspected cases of H1N1 influenza ’09 in the ACT. Update – 21 July 2009. Canberra: ACT Health, 2009. http://www.actdgp.asn.au/content/Document/July%202009/Letter%20GP%2021%20July%20Final.pdf (accessed Apr 2010).