To the Editor: Cardiovascular disease (CVD) and mental disorders are the top two contributors to the total burden of disease in Indigenous Australians and make a substantial contribution to the excess morbidity and mortality in this group.1 There is increasing evidence that mental disorders are risk factors for, or consequences of, CVD.2 Awareness and better understanding of the intertwined relationship between mental disorders and CVD in Indigenous populations can provide opportunities for coordinated and seamless management of these conditions in health care systems.
We investigated the association between mental disorders due to substance use and CVD in a remote Indigenous community in the Northern Territory. A cohort of 897 Aboriginal adults aged 20–74 years (85% of the community’s total adult population) was established through a population-based renal disease screening program in the community between 1992 and 1995.3 We followed up 784 participants, who were free of CVD at baseline, to 31 May 2005, using hospital and death records. The study was approved by the Behavioural and Social Sciences Ethical Review Committee of the University of Queensland.
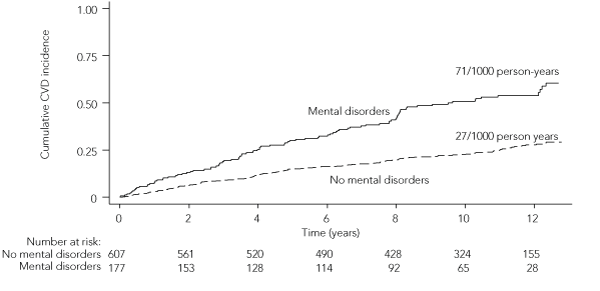
During a median follow-up period of 10 years, 177 of the 784 participants (23%) had clinically diagnosed mental disorders due to substance use (mainly alcohol: 140 participants), and 243 (31%) developed CVD. Incidence rates of CVD were 71 (95% CI, 58–87) and 27 (95% CI, 23–32) per 1000 person-years for those with and without substance use-related mental disorders, respectively (Box). Participants with substance use-related mental disorders were 2.6 (95% CI, 2.0–3.3) times more likely to develop CVD than those without. After adjusting for CVD risk factors measured at baseline (age, sex, body mass index, smoking status, alcohol use, blood pressure, serum cholesterol level, diabetes and albuminuria status), the association remained statistically significant, with an adjusted hazard ratio of 2.6 (95% CI, 1.9–3.5).
Traditional health care systems tend to separate services and treatment for mental disorders from those for physical health problems such as CVD.4 This separation is even more evident in remote Indigenous settings, where primary health care practitioners are already overwhelmed in providing general medical care to community members, with mental health services being delivered infrequently by visiting psychiatrists.5 The observed intertwined relationship between these two common conditions calls for integration of mental health services into routine primary health care, and enhanced collaboration between primary care practitioners, cardiologists and psychiatrists, in an effort to curb the huge burden imposed by these diseases.
The emerging Aboriginal mental health worker program in the NT has the potential to be an effective service model to bridge the gap between mental health care and day-to-day primary health care.5 Dedicated financial resources and ongoing support for recruitment, training and retention of Aboriginal mental health workers will be required for sustained integration of mental health care with primary care in Indigenous communities.
- 1. Vos T, Barker B, Stanley L, Lopez A. The burden of disease and injury in Aboriginal and Torres Strait Islander peoples 2003. Brisbane: School of Population Health, University of Queensland, 2007.
- 2. Prince M, Patel V, Saxena S, et al. No health without mental health. Lancet 2007; 370: 859-877.
- 3. Wang Z, Hoy WE. Hypertension, dyslipidemia, body mass index, diabetes and smoking status in Aboriginal Australians in a remote community. Ethn Dis 2003; 13: 324-330.
- 4. World Health Organization. The world health report 2001 — mental health: new understanding, new hope. Geneva: WHO, 2001.
- 5. Nagel T, Thompson C. Aboriginal mental health workers and the improving Indigenous mental health service delivery model in the ‘Top End’. Australas Psychiatry 2006; 14: 291-294.





We thank the Aboriginal community and people who participated in this study, and the local clinics for their help and support. The baseline data were collected by the renal research team at the Menzies School of Health Research, Darwin. This work was supported by a National Health and Medical Research Council Research Fellowship. The funder had no influence on study design, data collection and analysis, or writing of this letter.