An accurate medication history potentially reduces the risk of adverse drug events such as interactions or inadvertent ceasing of essential medications.1-7 Obtaining such a history in an emergency department (ED) can be challenging, and patients’ own medications (POM), if available, may give the earliest indication of the drug regimen taken before presentation. The label on each medication container provides information such as the name, strength and the frequency with which it is to be taken. POM may be particularly valuable when there are communication barriers, and after hours, when community records are unavailable.
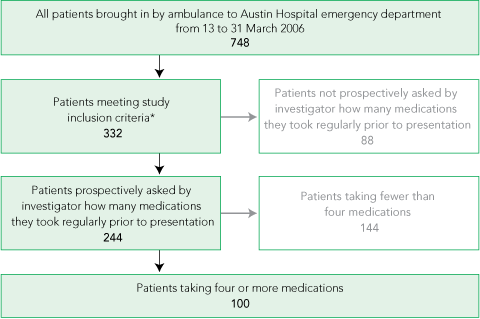
Of 748 patients brought in by ambulance to the Austin Hospital ED from 13 to 31 March 2006, 100 fulfilled our selection criteria and were recruited into the study (Box 1). No patients were referred to a pharmacist prior to the medication chart being written. Box 2 shows baseline characteristics of the 100 patients.
All, some, or none of patients’ regular medications were brought in for 30%, 37% and 33% of patients, respectively. Paramedics were often able to bring in POM for patients in high-acuity triage categories, or those transported from a public place, relative or friend’s home or doctor’s clinic. The most prevalent error type was omission, occurring on 61 occasions (Box 3). Most prescribing errors were of moderate significance (Box 4). One medication (insulin) that was brought in was lost, requiring redispensing before discharge.
Omissions were the most prevalent errors, and this is consistent with findings of previous studies.10-13 Medications that were not in tablet form were commonly omitted, including injections (particularly of insulin) and eye drops for glaucoma, highlighting that questions about such medications are routinely required during history taking. Another common error was prescription of wrong dosages; these were commonly charted for inhalers and cardiovascular medications.
If paramedics are to bring POM to EDs routinely, some procedural issues need to be managed. The risk of losing POM in transit or in hospital must be minimised. To achieve this, medications must not be sent back home before discharge as having these available at the time of hospital discharge can be of great assistance for many reasons, including educating patients about changes made in hospital and disposing of medications that the patient should no longer take. Many EDs currently use distinctive bags to store POM, and this may minimise the risk of medications being lost.14
One paramedic station in New South Wales has increased the number of patients arriving at their local ED with their own medications. Paramedics store a blood pressure sphygmomanometer in a large, clear, zip-locked bag, which is then placed inside the case of a portable resuscitator. As paramedics always carry both pieces of equipment, the plastic bag serves both as a reminder to bring patients’ medications to hospital, and as a receptacle in which to transport them.15
A comprehensive medication history is more likely when multiple sources of information are used,16,17 in conjunction with active communication with the patient or carer involved in organising the medications. POM should be used as prompts for patients to articulate their usual routine of medication administration.
3 Nature and number of the 151 prescribing errors identified
4 Occurrence and examples of prescribing errors of differing levels of significance
Received 16 December 2008, accepted 15 July 2009
- Esther W Chan1,2
- Simone E Taylor1
- Jennifer L Marriott2
- Bill Barger3
- 1 Austin Health, Melbourne, VIC.
- 2 Department of Pharmacy Practice, Centre for Medicine Use and Safety, Monash University, Melbourne, VIC.
- 3 Ambulance Victoria, Melbourne, VIC.
We gratefully acknowledge Kirstie Galbraith (Monash University) for her support and advice during the study period, and David Taylor (Austin Health) for advice on statistical issues and for reviewing the manuscript.
None identified.
- 1. The Society of Hospital Pharmacists of Australia. Committee of Specialty Practice in Clinical Pharmacy. SHPA standards of practice for clinical pharmacy. J Pharm Pract Res 2005; 35: 122-146.
- 2. The Society of Hospital Pharmacists of Australia. Committee of Specialty Practice in Emergency Medicine. SHPA standards of practice in emergency medicine pharmacy practice. J Pharm Pract Res 2006; 36: 139-142.
- 3. Rodehaver C, Fearing D. Medication reconciliation in acute care: ensuring an accurate drug regimen on admission and discharge. Jt Comm J Qual Patient Saf 2005; 31: 406-413.
- 4. The Joint Commission. Sentinel event alert. Issue 35. Using medication reconciliation to prevent errors. 2006, 25 Jan. http://www.jointcommission.org/SentinelEvents/SentinelEventAlert/sea_35.htm (accessed Aug 2009).
- 5. Institute for Healthcare Improvement. Improvement stories. Accuracy at every step: the challenge of medication reconciliation. 2006; 20 Mar. http://www.ihi.org/IHI/Topics/PatientSafety/MedicationSystems/ImprovementStories/AccuracyatEveryStep.htm (accessed Aug 2009).
- 6. Rogers G, Alper E, Brunelle D, et al. Reconciling medications at admission: safe practice recommendations and implementation strategies. Jt Comm J Qual Patient Saf 2006; 32: 37-50.
- 7. Gleason KM, Groszek JM, Sullivan C, et al. Reconciliation of discrepancies in medication histories and admission orders of newly hospitalized patients. Am J Health Syst Pharm 2004; 61: 1689-1695.
- 8. Hepler CD, Strand LM. Opportunities and responsibilities in pharmaceutical care. Am J Health Syst Pharm 1990; 47: 533-543.
- 9. Australasian College for Emergency Medicine. Policy on the Australasian Triage Scale. Last reviewed 2006. http://www.acem.org.au/media/policies_and_guidelines/P06_Aust_Triage_Scale_-_Nov_2000.pdf (accessed Aug 2009).
- 10. Cornish PL, Knowles SR, Marchesano R, et al. Unintended medication discrepancies at the time of hospital admission. Arch Intern Med 2005; 165: 424-429.
- 11. Tam VC, Knowles SR, Cornish PL, et al. Frequency, type and clinical importance of medication history errors at admission to hospital: a systematic review. CMAJ 2005; 173: 510-515.
- 12. Nicholls M, Horler K, Campbell D, et al. Medicines. Peace in a POD (patients’ own drug). Health Serv J 2001; 111: 35.
- 13. Drewett NM. Stop regular medicine errors. Pharm in Pract 1998; 8: 193-196.
- 14. Chan EW, Taylor SE, Marriott JL, Barger B. Exploration of attitudes and barriers to bringing patient’s own medications to the emergency department: a survey of paramedics. J Emerg Primary Health Care 2008; 6 (4). Article 990313. http://www.jephc.com/uploads/990313EC1.pdf (accessed Aug 2009).
- 15. Australian Resource Centre for Healthcare Innovations. TABLETS — Tablets are bagged letting emergency treat safely. 2007. http://www.archi.net.au/e-library/awards/awards06/safety/tablets (accessed Aug 2009).
- 16. Carney SL. Medication accuracy and general practitioner referral letters. Intern Med J 2006; 36: 132-134.
- 17. Varkey P, Cunningham J, O’Meara J, et al. Multidisciplinary approach to inpatient medication reconciliation in an academic setting. Am J Health Syst Pharm 2007; 64: 850-854.





Abstract
Objective: To determine whether the availability of patients’ own medications (POM) in emergency departments (EDs) results in decreased prescribing errors of patients’ usual medications on admission.
Design, participants and setting: Observational study of patients presenting by ambulance to the ED of Austin Hospital, a Melbourne metropolitan teaching hospital, between 13 and 31 March 2006. Patients were enrolled if they were brought to the ED by ambulance, aged 18 years or older, taking four or more regular medications, admitted to hospital, and not referred to a pharmacist before the admission medication chart was written. ED pharmacists determined patients’ regular medications and details of medications brought in by ambulance. Admission medication charts were assessed and discrepancies were recorded as prescribing errors if a change was made after a pharmacist discussed the discrepancy with the prescriber.
Main outcome measures: Percentage of medications correctly prescribed when POM were brought in to the ED compared with when they were not; the nature and frequency of prescribing errors on admission.
Results: 100 patients were enrolled; they were taking 4–17 regular medications (mean, 8.0; SD, 3.7). Among the 428 POM that were brought to the ED, 56 errors occurred (13.1%); and among the 372 regular medications taken by patients for whom POM were not brought in, 95 errors occurred (25.5%) (difference in percentages, 12.4%; 95% CI, 6.7%–18.0%; P < 0.001). The most prevalent prescribing errors were omissions (40.4%), and most errors (72.8%) were classified as of “moderate” clinical significance.
Conclusions: When POM were brought to the ED by paramedics, significantly fewer errors occurred on admission medication charts. An intervention program to encourage paramedics to bring POM to the ED is indicated.