Two months before the Armistice, the Egyptian Expeditionary Force, an Allied army containing many Australian Light Horse regiments, launched one of the last great cavalry campaigns and defeated the Turkish Army in Palestine. With the capture of Damascus, Amman, Beirut and Aleppo, comprehensive victory followed.1 It was fortunate that victory was quickly gained, as twin epidemics of falciparum malaria and pandemic influenza ended most military operations within weeks of the start of the final offensive on 19 September 1918.2,3
The final phase of the campaign was launched from what is now Israel, north of Jerusalem.1,2 No one who could avoid spending the summer in the Jordan River valley stayed there; besides being extraordinarily hot and dusty, it was also a very malarious area.1,2 Horses require large amounts of water, which linked military operations to the same river areas where mosquito breeding facilitated malaria infections.4 The Desert Mounted Corps under Lieutenant General Chauvel was consciously committed to the Jordan River valley, as one of the traditional invasion routes that had to be covered, despite the probability of large numbers of disease casualties.1 Because malaria infection was a well known risk, great efforts were made to define and eliminate the numerous mosquito breeding areas.4-6 Large drainage works, requiring extensive labour forces, were undertaken to control malaria, often in preference to defensive emplacements. Malaria infection was relatively well controlled when static positions allowed these extensive environmental modifications to stop mosquito breeding.
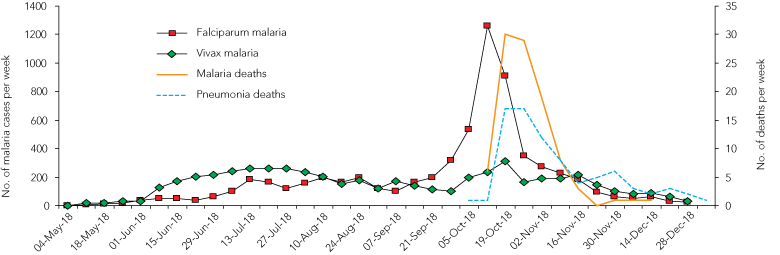
By the 12th day after the offensive began, the incidence of falciparum malaria infection in the Allied forces was rapidly increasing.4 Box 1 shows the course of the malaria epidemic and the number of malaria cases and deaths among the Desert Mounted Corps in Palestine.3,4,7,8 By mid October more than 1200 cases of malaria, largely due to Plasmodium falciparum, were occurring in a single week, with nearly 8% of the force requiring evacuation because of malaria. During the 2 months of the offensive before the Armistice, the Desert Mounted Corps (about 40 000 men) evacuated 19 652 men sick, with 6347 of these having blood-smear-positive malaria infection.2 Such attrition largely halted combat operations. Deaths lagged the peak malaria incidence by about 2 weeks (Box 1), as severely ill men were slowly brought back along the extended line of advance created by the rapid movement of cavalry up the Plain of Esdraelon. The Australian Light Horse regiments had outdistanced all their supporting logistics, including most of their medical support.1,2
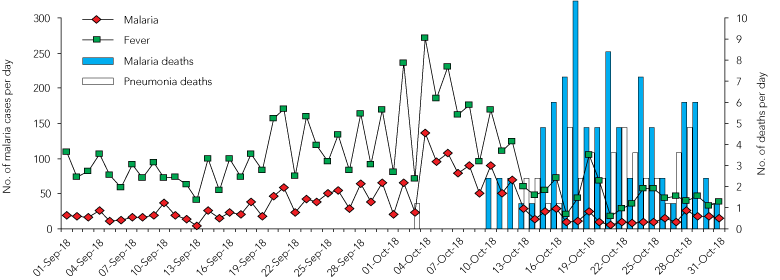
In the Australian and New Zealand Army Corps (ANZAC) Mounted Division (about 7000 men) deployed in the Jordan River valley, malaria incidence could be directly related to where the units had camped before moving into the hills. Malaria cases reached nearly 500 per week and were concentrated in the 1st Light Horse and New Zealand brigades that had spent 21–23 September in an area of known transmission.7-9 This was nearly three times the rate in the 2nd Light Horse Brigade, which had moved directly into the hills from a previously protected area.4 The daily malaria casualties in the ANZAC Mounted Division are shown in Box 2, which also shows deaths lagging peak infection by about 1–2 weeks.7,8
As this malaria epidemic had been anticipated, it was one of the best ever documented. A junior officer, Captain Philip Manson-Bahr (Distinguished Service Order), who later became a leading figure in tropical medicine in the United Kingdom, designed a malaria prevention plan in mid 1918.10 Mosquito breeding was aggressively controlled by limiting breeding areas along the front line. After the offensive began, mobile malaria diagnosis units were to follow behind the cavalry to ensure rapid treatment of febrile infections. No other interventions were possible given the military operational constraints. Quinine is foul-tasting and daily prophylactic doses are unlikely to be used in the absence of compulsion. Furthermore, the cavalry would not carry mosquito nets on combat operations.
To prepare for the expected increase in malaria infection, each division in the Desert Mounted Corps was assigned a mobile malaria diagnosis unit consisting of a specially trained medical officer, two medical orderlies, two microscopes, four horses and a horse-drawn wagon.1-4 Their mission was to bring specific malaria diagnosis, in the form of microscopically examined blood smears, as close to the leading units as possible.11 No. 5 Malaria Diagnosis Station was assigned to the 5th Australian Light Horse Clearing Station of the ANZAC Mounted Division and is shown at work in Box 3. The official report of the malaria epidemic reads:
The origin of the 1918–19 influenza virus, now thought to be an A/H1N1 strain, is uncertain. Influenza appeared in Palestine in May 1918 in a mild form and then in September as a much more severe disease, with many cases of pneumonia.12 Influenza particularly affected two groups, Turkish prisoners and medical personnel. The collapse of all medical facilities in Damascus occurred between the evacuation by the Turks and the occupation by the Allies. Cases of influenza added to the massively crowded hospitals where between 3000 and 4000 of about 20 000 Turkish prisoners of war (POWs) died.1 Seventy to 170 POWs were being buried each day in a continuous trench.1,2 Medical officers who were in constant contact with the sick soon became ill with influenza; most were unable to perform their duties. The medical evacuation system collapsed, with 900 seriously ill soldiers collected in Jericho without a means to move them.2
Initially, it was not understood that two epidemics of febrile disease were present in Palestine in late 1918. Both malaria and influenza can kill rapidly, and there were instances of soldiers found dead on the march after a halt, and others dying within hours of reaching medical care.3 The similarity of the severe form of both these diseases, in mechanism and outcome, is now understood in terms of an excess release of inflammatory cytokines.13 Postmortem examinations played an important role in defining the overlap between malaria and influenza. Captain Manson-Bahr described a series of 67 consecutive autopsies: he found that 35 soldiers died of falciparum malaria while another 32 died of malaria complicated by influenza–bronchopneumonia.3 Lieutenant Colonel N Hamilton Fairley, an Australian physician, who also became a noted figure in tropical medicine after the war, was conducting autopsies at the 14th Australian General Hospital in Egypt.14 In his series of 80 cases, only 16% were found to have died of uncomplicated malaria infection; 84% had malaria, but death was due to a secondary infection, often bronchopneumonia (59%).14
In the Egyptian Expeditionary Force (about 315 000 soldiers), disease casualties outnumbered those due to combat by more than 37 to 1. A total of 773 deaths from malaria infection were recorded during the last 3 months of the campaign. Another 934 soldiers from all ranks, private to regimental commanding officer, died of influenza–pneumonia during the same period.2,15 This is in comparison with the combat casualties of 198 killed or missing and 438 wounded for the entire Desert Mounted Corps of about 40 000 men.1
Textbooks describe single diseases under pathogen-specific chapters. Unfortunately, reality often involves multiple interacting agents whose symptoms overlap. The Australian Army in Palestine in 1918 is a striking example of why accurate diagnosis remains vital, even when health facilities are overwhelmed with patients. No one could do much about pandemic influenza in the pre-antibiotic era, except provide simple nursing care. Malaria infection, however, could be treated with quinine, although it was not a perfect chemotherapeutic agent, and identifying those with falciparum malaria and giving them quinine saved many lives.4,10,11 Concentrating on what one can do with the tools available is a sound principle during mass casualty events and will undoubtedly still apply when the next influenza pandemic arrives.
Some risks can be anticipated, and some cannot. The decision to launch a military offensive during the height of the malaria season in Palestine was made, knowing the probable consequences for the health of the troops. Malaria infection was ameliorated with the best technology of the time, which was rapid microscopic diagnosis followed by quinine chemotherapy. The influenza pandemic could not have been foreseen, and it struck when the medical evacuation system was already functioning poorly due to extensive military operations over great distances in difficult terrain.2 The campaign concluded successfully despite large numbers of disease casualties, because the Turkish forces collapsed in the face of the rapidly moving Allied assault.1 That the Turks were also hit by both malaria and influenza contributed to their military failure.2
1 Malaria incidence, and deaths from malaria and pneumonia, per week, Desert Mounted Corps, Palestine, May – December 1918
 | |||||||||||||||
- G Dennis Shanks1,2
- 1 Centre for Military and Veterans’ Health, University of Queensland, Brisbane, QLD.
- 2 Australian Army Malaria Institute, Gallipoli Barracks, Brisbane, QLD.
None identified.
- 1. Gullett HS. The Australian Imperial Force in Sinai and Palestine, 1914–1918. Sydney: Angus & Robertson, 1923: 638-791.
- 2. Downes RM. The campaign in Sinai and Palestine. 2nd ed. Sydney: Halstead Press, 1938: 698-777.
- 3. Manson-Bahr P. Experiences of malaria in the Egyptian Expeditionary Force. Lancet 1920; 1: 79-85.
- 4. Angus W. Report on malaria in the Egyptian Expeditionary Force during 1918. Cairo: Egyptian Expeditionary Force, January 1919: 1-51. Australian War Memorial, Canberra.
- 5. Sewell EP, Macgregor ASM. An anti-malaria campaign in Palestine: an account of the preventive measures undertaken in the 21st Corps area in 1918. J R Army Med Corps 1920; 34: 204-218.
- 6. Woodcock HM. Notes and comments upon my malaria experiences while with the Egyptian Expeditionary Force, 1916-1918. J R Army Med Corps 1920; 34: 385-483.
- 7. Cases of malaria, diagnosed each week in the Jordan valley by the ANZAC Field Laboratory, 1918. File 267/25. Australian War Memorial, Canberra.
- 8. Charts and graphs from ANZAC Mounted Division, Desert Mounted Corps. File 267/29. Australian War Memorial, Canberra.
- 9. Statistics of casualties Australian Imperial Force. London: Records Section, AIF Headquarters, 1919: 1-32. Australian War Memorial, Canberra.
- 10. Manson-Bahr P. War diary of malaria diagnosis stations. London: National Records Office Kew, 1918: 1-17. The National Archives, Kew, Surrey, UK.
- 11. Ferguson EW. History of the ANZAC field laboratory, 1919: 1-12. Australian War Memorial, Canberra.
- 12. Benjafield JD. Notes on the influenza epidemic in the Egyptian Expeditionary Force. BMJ 1919; 2: 167-169.
- 13. Clark J, Alleva L, Budd A, Cowden W. Understanding the role of inflammatory cytokines in malaria and related disease. Travel Med Infect Dis 2008; 6: 67-81.
- 14. Fairley NH. The causes of death from malaria in Palestine: a study in cellular pathology. Trans R Soc Trop Med Hyg 1920; 13: 121-125.
- 15. Mitchell TJ, Smith GM. Medical services: casualties and medical statistics of the Great War, 1931: 208-217. Imperial War Museum, London.






Abstract
In October 1918, an Allied army (Egyptian Expeditionary Force) in Palestine experienced simultaneous epidemics of falciparum malaria and influenza during the cavalry campaign that defeated the Turkish Army.
Malaria infection occurred 2 weeks after the advance of cavalry units into areas without environmental mosquito control. Pandemic influenza, now thought to be an A/H1N1 strain, struck at the same time.
In the Egyptian Expeditionary Force of 315 000 soldiers, 773 died from malaria and 934 from influenza–pneumonia. Disease casualties outnumbered those due to combat by more than 37 to 1.
Simultaneous infectious disease epidemics can cause mass casualties, capable of overwhelming any health service.