To the Editor: Bronchiolitis, most often associated with respiratory syncytial virus (RSV), is a major cause of hospitalisation in young children. Those with chronic lung and congenital heart disease (the latter affecting about 192 births annually in Western Australia) are at particularly high risk.2 Immunoprophylaxis with the RSV monoclonal antibody palivizumab is effective in reducing severe RSV-related hospitalisations, and monthly immunoprophylaxis is recommended in high-risk children.2,3 Monthly immunoprophylaxis is costly; therefore, the most cost-effective schedule follows the times of peak RSV activity4 — usually the winter months, May to October.
Using the Western Australian Data Linkage System,5 we investigated the seasonality of bronchiolitis hospitalisations (International Classification of Diseases-10 code J21) from 1996 to 2005 as a proxy for RSV-related illness. Data specifically for RSV-related illness were considered unreliable because some children may not have been tested for RSV, test results may not have been documented on hospital discharge notes, or RSV immunofluorescence tests may have given false negative results. Furthermore, RSV codes (B97.4, J12.1, J20.5, J21.0) were not used by hospitals in WA until July 1999.
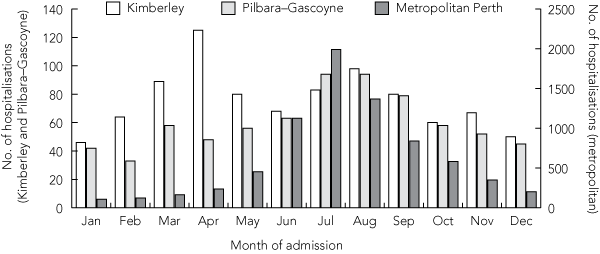
We identified 11 988 hospitalisations for bronchiolitis throughout WA among 245 249 births. Most bronchiolitis admissions (81%) were in children younger than 12 months. In the Perth metropolitan region, there was a clear winter seasonal pattern, with hospitalisations peaking in July. However, in the Kimberley region in northern WA, there was a sustained bimodal seasonality, with a peak in April and second peak in August (Box). Moreover, only 51.5% (469) of bronchiolitis admissions in the Kimberley and 61.5% (444) in the Pilbara–Gascoyne (located in mid-north WA) occurred between May and October, as opposed to 84.3% (6354) in the metropolitan region. These data support an earlier implementation and longer dosing schedule with palivizumab for high-risk children in the Kimberley and Pilbara–Gascoyne than for those in Perth.
- 1. Bower C, Ramsay JM. Congenital heart disease: a 10 year cohort. J Paediatr Child Health 1994; 30: 414-418.
- 2. The IMpact-RSV Study Group. Palivizumab, a humanized respiratory syncytial virus monoclonal antibody, reduces hospitalization from respiratory syncytial virus infection in high-risk infants. Pediatrics 1998; 102: 531-537.
- 3. Bolisetty S, Wheaton G, Chang AB. Respiratory syncytial virus infection and immunoprophylaxis for selected high-risk children in Central Australia. Aust J Rural Health 2005; 13: 265-270.
- 4. Panozzo CA, Fowlkes AL, Anderson LJ. Variation in timing of respiratory syncytial virus outbreaks: lessons from national surveillance. Pediatr Infect Dis J 2007; 26 (11 Suppl): 41S-45S.
- 5. Holman CD, Bass AJ, Rouse IL, et al. Population-based linkage of health records in Western Australia: development of a health services research linked database. Aust N Z J Public Health 1999; 23: 453-459.





Acknowledgement: Hannah Moore and Deborah Lehmann are currently funded by a National Health and Medical Research Council program grant (No. 353514).