Health literacy, which enables patients to understand and to act in their own interest, has been described as “a neglected, final pathway to high-quality health care”.1 Functional health literacy (FHL), a more limited concept, involves the ability to read, calculate and act on oral and written information in health care settings.1 Studies (predominantly from the United States) have shown that limited FHL is associated with premature mortality, higher health care costs, adverse health outcomes, lower health status, less frequent preventive health behaviour and less active self-management of chronic conditions.2,3
With increasing demands being made of people to maintain their own health and manage their own chronic conditions, competency to participate in decisions is a critical clinical and policy issue. The National Health and Hospitals Reform Commission identified improving health literacy as a national health reform direction for Australia.4 However, there are few population data on health literacy in Australia to estimate the magnitude of this task. Studies are limited by the complexity of the tools used5 or by low response rates.6 Recently, well validated screening tools have become available that reduce the time required to assess FHL (a limitation of previous instruments7); one such tool is the Newest Vital Sign (NVS).8
Data were obtained from the South Australian Health Omnibus Survey (SAHOS) during September and October 2008. Within each Australian Bureau of Statistics collector district, a random starting point was selected and 10 households were sampled using a fixed skip interval. In a non-replacement sample, one adult aged 15 years or older, whose birthday was next, was selected for interview in their home by trained health interviewers. The SAHOS methodology has been described in detail elsewhere.9
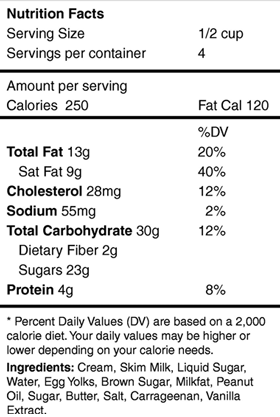
Respondents completed the NVS as a measure of FHL. The NVS is a screening tool developed specifically for use in primary care (Box 1).8 Compared with the most commonly used health literacy instrument, the Test of Functional Health Literacy in Adults (TOFHLA),10 the NVS has high sensitivity for detecting limited FHL,11 beyond that of education and age alone.8 Compared with the TOFHLA, the specificity of the NVS may produce overestimates of limited FHL.7,8 The NVS is scored out of 6, with a score of 4–6 almost always indicating adequate FHL (described as “adequate” in this article), 2–3 indicating the possibility of limited FHL (“at risk”), and 0–1 indicating a high likelihood (50% or greater) of limited FHL (“inadequate”).8
General health status was assessed by asking respondents to rate their general health on a five-point scale, from excellent to poor. Single-item measures have demonstrated good reproducibility, reliability, and strong concurrent and discriminant scale performance with an established health status measure (the 12-item Short Form Health Survey).12 Respondents were asked what health services they had accessed in the previous 12 months, and whether a doctor had diagnosed them with any of nine specified chronic conditions. Demographic data collected included sex, education level, employment status, household income, country of birth and area of residence (metropolitan or regional).
Data were analysed using SPSS version 15.0 (SPSS Inc, Chicago, Ill, USA) and weighted to the individual’s probability of selection and to Australian Bureau of Statistics population estimates.13 Bivariate associations of FHL with demographics, chronic conditions and health service use were determined using the χ2 test. Multiple logistic regression models were developed for outcome variables of inadequate FHL compared with those with adequate FHL, and also for adequate FHL compared with those either at-risk or with inadequate FHL (NVS score, 0–3).
The 2008 SAOHS population sample comprised 2824 respondents from 4614 households contacted (61.2% participation rate), and the sociodemographic distribution of participants corresponded to SA population estimates.13
Of the 2824 participants, 1358 (48.1%) were male and 2158 (76.4%) resided in the metropolitan area of Adelaide. Almost a quarter (24.0%) were at risk of limited FHL, and 21.0% had a high likelihood of inadequate FHL. Inadequate and at-risk FHL were associated with increasing age and markers of social disadvantage (Box 2). However, less than adequate FHL was found in around 20% of those reporting an annual income of greater than $100 000 or a bachelor degree and higher. Respondents with self-reported fair or poor general health were twice as likely to have inadequate FHL as those reporting very good or excellent health (31.8% v 16.9%).
In multivariable analyses, inadequate FHL was significantly associated with older age, lower education, lower income, being born outside Australia, New Zealand, the United Kingdom and Ireland, and poorer health status (Box 2).
Among respondents aged 65 years and over, limited FHL was more common in those with chronic conditions, although the strength of the adjusted associations with individual chronic conditions was similar across age groups. In adjusted models, inadequate or at-risk FHL was significantly associated with diabetes, ischaemic heart disease and stroke in both age groups and in arthritis among those younger than 65 years (Box 3).
Reported use of health care services varied with health literacy. Participants with inadequate or at-risk FHL had more hospital admissions and less use of services in the community, and these associations were stronger among those younger than 65 years (Box 4). Respondents aged 65 years and over with inadequate FHL were significantly more likely to report being hospitalised in the previous 12 months (odds ratio, 2.2; 95% CI, 1.1–4.5).
Limited FHL is common among adults in SA, and is associated with lower health status. Consistent with other reports, risk of limited FHL was more prevalent among people with significant chronic conditions such as diabetes, heart disease and stroke.1,2 Younger individuals at risk of limited FHL were less likely to report visiting a range of health care providers, including general practitioners. The widespread distribution of risk of less than adequate FHL across socioeconomic groups emphasises that limited FHL is unlikely to be a proxy measure of social disadvantage. Compared with the highest category of income and education, each group showed an increased risk of limited FHL. However, even among those with a bachelor degree or higher, around 20% were at risk of limited FHL.
Using educational level will misclassify a substantial proportion of people as health literate or illiterate.1,2,5,6 Clinicians are unable to correctly identify those with limited FHL,14 so some form of assessment is required in clinical practice. The NVS is quick to administer and is acceptable to patients, with over 98% of participants in one study agreeing to undergo assessment during a routine primary care visit.15 Patients with limited health literacy are less likely to ask clinicians questions,16 and most health education information is too complex for patients to understand.1 Knowledge of the scope of limited health literacy can lead clinicians to adjust their communication styles to meet the needs of patients and carers.7 Specifically tailoring communication for those with poor health literacy has been shown to improve outcomes among patients with diabetes.17 Explicitly including health literacy education in the design of chronic disease self-management programs may be an effective means of improving the outcomes achieved by such programs and minimising social inequalities in health outcomes.18
Although our survey only included households with telephones, 97% of households have telephones19 and the demographic characteristics were representative of the overall SA population profile,13 so the extent of any bias is likely to be small.
We do not know from our study the extent to which the risk of limited FHL is associated with less knowledge of chronic conditions or with unhealthy lifestyle behaviours. How individuals process and contextualise information will vary, and people can have a greater understanding of an issue than a health literacy test result might suggest. Similarly, people’s behaviour will reflect a wider range of influences, both good and ill, than can be measured by a brief screening test. However, it is clear from our data and other studies that results of FHL tests reflect the risk of having a chronic disease and the outcomes of those conditions.1-3
It is known that a small number of health behaviours account for up to 78% of the variance in the apparent risk of a serious chronic disease.20 Yet, as noted in a recent commentary, in moving from “knowledge of what most matters to health to the power of its application . . . we have miles to go before we sleep”.20 Other commentators have suggested that there is value in conceptualising health literacy as more than a risk factor requiring assessment and management in clinical care to also include the notion of health literacy as a personal asset,21,22 “focused on the development of skills and capacities intended to enable people to exert greater control over their health and the factors that shape health”.21 This takes health literacy beyond health-related reading and numeracy skills into the field of preventive health as a “resource for daily living” outside health care settings,23 and thus may be better characterised as health competency.24 We propose that health competency is a process that, in either clinical or everyday settings, involves patients:
recognising an issue or problem as personally relevant;
accepting that the issue exists and requires decisions to be made and some form of action taken;
seeking out and critically evaluating information;
undertaking actions with regard to the issue in light of knowledge gained; and
personalising the issue by monitoring the effects or outcomes over time.
Such conceptualisation involves personal skills and competencies, attitudes, motivation and the inclination to act with regard to health, and recognises these may be context-specific to situations, health conditions, and modes of social or clinical interaction. As a personal asset, health literacy so defined acknowledges individuals’ social and cultural contexts and calls for engagement in social action for health and participation in altered social norms that can enable action on the social determinants of health.21 It suggests an expanded role for the health system: patient education, improving the parameters of the health care interaction and facilitating navigation through an often labyrinthine health system, and fostering development in schools, adult learning and community development programs.21
There is, however, little empirical research evaluating the “asset” concept. This relates to a lack of consensus definition of health literacy1,21,22 and a lack of well developed instruments that can measure a broader notion of health literacy as “a distinct concept, rather than a derivative concept from literacy and numeracy skills”.21 The NVS, like the TOFHLA,11 measures reading, interpretation skills and the ability to use numbers, rather than all aspects of health literacy.21,23 Its brevity permits use in clinical settings and population surveys with acceptable responder burden, but at the potential risk of overestimating limited health literacy when compared with the TOFHLA. However, our estimates of limited FHL are similar to those obtained by other Australian surveys using much more comprehensive instruments.5 It has been suggested that none of the current FHL instruments are ideal, nor do they capture all the aspects of the definitions of health literacy or competency.21,23,24 The recently developed Swiss Health Literacy Survey comprehensively measures competencies beyond basic health-related reading skills in an attempt to align with expanded definitions and conceptual models of health literacy.25 Results from more widespread use of the Swiss Health Literacy Survey may help further understanding of health literacy or competency and ascertain whether there is a need for other measures.24 This understanding will aid further research to identify how groups with different levels of health literacy achieve different health outcomes, and to identify modifiable risk factors and potential interventions.
1 The Newest Vital Sign8
 |
|||||||||||||||
Figure reproduced with permission from Weiss et al,8 courtesy of Annals of Family Medicine Inc. |
|||||||||||||||
2 Prevalence of participants within functional health literacy categories among different demographic groups and multiple logistic regression models for comparison of inadequate* with adequate† functional health literacy
Numbers and percentages may not add to n or 100%, respectively, as data are weighted. |
|||||||||||||||
3 Prevalence of chronic conditions by functional health literacy levels and adjusted odds ratios* for inadequate or at-risk levels† of functional health literacy associated with these conditions, by age group
Numbers and percentages may not add to n or 100%, respectively, as data are weighted. |
|||||||||||||||
4 Health service use in previous 12 months within levels of functional health literacy overall and age stratified and adjusted odds ratios* for association of inadequate or at-risk functional health literacy† with health service use, by age group
Received 29 April 2009, accepted 15 September 2009
- Robert J Adams1
- Sarah L Appleton1
- Catherine L Hill1,2
- Mark Dodd3
- Christopher Findlay3
- David H Wilson1
- 1 Health Observatory, Discipline of Medicine, University of Adelaide, Adelaide, SA.
- 2 Rheumatology Unit, Queen Elizabeth Hospital, Adelaide, SA.
- 3 School of Economics, University of Adelaide, Adelaide, SA.
The University of Adelaide and the Queen Elizabeth Hospital Research Foundation fund the Health Observatory. They had no role in the study design, data collection, analysis and interpretation, and writing or publication of this article.
None identified.
- 1. Nielsen-Bohlman L, Panzer AM, Kindig DA, editors; Committee on Health Literacy, Board on Neuroscience and Behavioral Health. Health literacy: a prescription to end confusion. Washington, DC: National Academies Press, 2004.
- 2. Dewalt DA, Berkman ND, Sheridan S, et al. Literacy and health outcomes: a systematic review of the literature. J Gen Intern Med 2004; 19: 1228-1239.
- 3. Howard DH, Gazmararian JA, Parker RM. The impact of low health literacy on medical costs for Medicare managed care enrollees. Am J Med 2005; 118: 371-377.
- 4. National Health and Hospitals Reform Commission. A healthier future for all Australians — interim report December 2008. Canberra: Commonwealth of Australia, 2009. (Publications No. P3 – 4822.)
- 5. Australian Bureau of Statistics. Adult Literacy and Life Skills Survey, summary results, Australia, 2006. Canberra: ABS, 2007. (ABS Cat. No. 4228.0.)
- 6. Barber MN, Staples M, Osborne RH, et al. Up to a quarter of the Australian population may have suboptimal health literacy depending upon the measurement tool: results from a population-based survey. Health Promot Int 2009; 24: 252-261.
- 7. Weiss BD. Removing barriers to better, safer care. Health literacy and patient safety: help patients understand. A manual for clinicians. 2nd ed. Chicago: American Medical Association Foundation and American Medical Association, 2007.
- 8. Weiss BD, Mays MZ, Martz W, et al. Quick assessment of literacy in primary care: the Newest Vital Sign. Ann Fam Med 2005; 3: 514-522.
- 9. Wilson DH, Wakefield M, Taylor AW. The South Australian Health Omnibus Survey. Health Promot J Austr 1992; 2: 47-49.
- 10. Parker RM, Baker DW, Williams MV, Nurss JR. The Test of Functional Health Literacy in Adults: a new instrument for measuring patients’ literacy skills. J Gen Intern Med 1995; 10: 537-545.
- 11. Osborn CY, Weiss BD, Davis TC, et al. Measuring adult literacy in health care: performance of the Newest Vital Sign. Am J Health Behav 2007; 31 Suppl 1: S36-S46.
- 12. DeSalvo KB, Fisher WP, Tran K, et al. Assessing measurement properties of two single-item general health measures. Qual Life Res 2006; 15: 191-201.
- 13. Australian Bureau of Statistics. Population by age and sex, Australian states and territories Jun 2007. Canberra: ABS, 2008. (ABS Cat. No. 3201.0.)
- 14. Kelly PA, Haidet P. Physician overestimation of patient literacy: a potential source of health care disparities. Patient Educ Couns 2007; 66: 119-122.
- 15. Ryan JG, Leguen F, Weiss BD, et al. Will patients agree to have their literacy skills assessed in clinical practice? Health Educ Res 2008; 23: 603-611.
- 16. Katz MG, Jacobson TA, Veledar E, Kripalani S. Patient literacy and question-asking behavior during the medical encounter: a mixed-methods analysis. J Gen Intern Med 2007; 22: 782-786.
- 17. Schillinger D, Piette J, Grumbach K, et al. Closing the loop: physician communication with diabetic patients who have low literacy. Arch Intern Med 2003; 163: 83-90.
- 18. Fayter D, Main C, Misso K, et al. Population tobacco control interventions and their effects on social inequalities in smoking. York: Centre for Reviews and Dissemination, University of York, 2008. (CRD Report 39.)
- 19. Australian Bureau of Statistics. Census of Population and Housing: selected social and housing characteristics for statistical local areas South Australia, 2001. Canberra: ABS, 2002. (ABS Cat. No. 2015.4.)
- 20. Katz DL. Life and death, knowledge and power: why knowing what matters is not what’s the matter. Arch Intern Med 2009; 169: 1362-1363.
- 21. Nutbeam D. The evolving concept of health literacy. Soc Sci Med 2008; 67: 2072-2078.
- 22. Protheroe J, Wallace LS, Rowlands G, DeVoe JE. Health literacy: setting an international collaborative research agenda. BMC Fam Pract 2009; 10: 51. doi: 10.1186/1471-2296-10-51.
- 23. Peerson A, Saunders M. Health literacy revisited: what do we mean and why does it matter? Health Promot Int 2009; 24: 285-296.
- 24. Baker DW. The meaning and the measure of health literacy. J Gen Intern Med 2006; 21: 878-883.
- 25. European Health Literacy Survey. University of Maastricht. http://inthealth.eu/research/health-literacy-survey/ (accessed Aug 2009).





Abstract
Objective: To measure the level of functional health literacy (FHL) in an Australian population, and to explore the level of risk associated with level of FHL.
Design, setting and participants: Cross-sectional, random population survey administered to 2824 South Australians aged ≥ 15 years, September – October 2008.
Main outcome measures: Newest Vital Sign as a measure of FHL, self-reported general health status, and use of health services.
Results: 24% of respondents were at risk of limited FHL, and 21% had a high likelihood of inadequate FHL; this increased with age (≥ 65 years, 50% v 25–44 years, 11%). In multiple logistic regression models, a high likelihood of inadequate FHL was significantly more common among those with lower education (left school ≤ 15 years of age, odds ratio [OR], 8.1; 95% CI, 4.8–13.6); with lower annual income (< $20 000, OR, 4.1; 95% CI, 2.3–7.4); who were born in countries other than Australia, New Zealand, the United Kingdom and Ireland; and with poorer health status (OR, 1.6; 95% CI, 1.2–2.2). Inadequate FHL was significantly less common among females (OR, 0.6; 95% CI, 0.5–0.8). People with inadequate or at-risk FHL were significantly more likely to report having diabetes, cardiac disease or stroke, and significantly less likely to have recently attended a doctor. Respondents aged ≥ 65 years with inadequate FHL were more likely to have been admitted to hospital (OR, 2.2; 95% CI, 1.1–4.5).
Conclusion: Many Australians are likely to have limited health literacy, and this is a risk to effective health care delivery and health improvement across the community.