Health professionals need to be able to work in teams, but, paradoxically, students receive little training in how to function within an interprofessional teamwork context. Competent patient care increasingly requires practitioners to know how each of the different professions contributes its skills and expertise to optimise health outcomes.1,2 Practitioners also need to respect the contribution of each profession to patient care.
International and domestic policy agencies are urging fundamental reform of the health workforce to place interprofessional competencies on an equal footing with profession-centred expertise.3-6 Employers are demanding that universities provide team-ready graduates who have been exposed to the principles of interprofessional education (IPE) and practice.7-9 Universities face significant logistical problems in aligning curriculum across multiple professions to provide the requisite IPE training opportunities. In this article we present an overview of the University of Queensland Health Care Team Challenge (UQ HCTC), which was designed to respond to the demands for workforce reform and to provide an authentic IPE teamwork experience.
University curricula are primarily devoted to producing graduates who are competent in their professional domain. Traditional approaches to curriculum organisation and clinical education severely limit the time and format that students from different professions can spend together, learning about and from each other. IPE is essential to break down the barriers between professions that undermine the quality of cross-profession communication and patient care. A recent Best Evidence Medical Education systematic review reported that IPE activities had a positive impact on learners’ capacity to work together and on the quality of service provided to clients. Evidence of improved client satisfaction was also noted.10
The challenge is to embed opportunities for IPE and interprofessional practice within university structural frameworks that traditionally emphasise a profession-centred educational process. Not least among these challenges is developing IPE programs capable of competing with the student focus on profession-related education. Further, university staff expertise in IPE is limited, and resistance to non-profession-centred activities needs to be sensitively and imaginatively managed.8
UQ offers a range of interprofessional learning opportunities within its curriculum. In 2005, an IPE fellowship was established by the Faculty of Health Sciences. It sought innovative proposals capable of stimulating multilevel cultural change to accelerate acceptance of IPE philosophies and practices.1,11 The fellowship project, jointly awarded to two of us (R A B and M C M), proposed to implement an HCTC at UQ and explore the potential for a national competition.
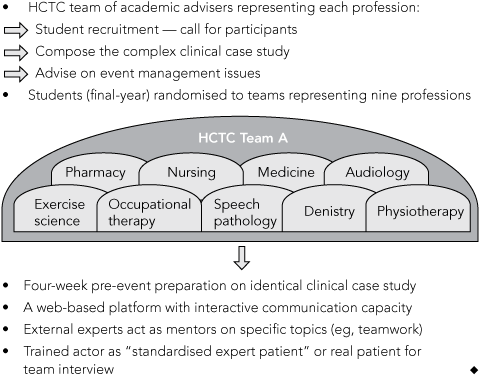
The inaugural UQ HCTC event was held in 2007 (Box 1). It is a voluntary extracurricular learning activity for final-year students to demonstrate best practice in clinical care and interprofessional teamwork in an authentic patient-centred context.12 It culminates in a lively annual public competition between interprofessional student teams. Each team is comprised of nine students, each representing one of the nine professions within the Faculty of Health Sciences. Students are recruited from a widely publicised call for participants and then randomly assigned to a team. The academic panel that supports the event collaborates with an external interprofessional team working in a health service to identify a patient (and carers) willing to be interviewed by the student teams and participate as a part of the judging panel. The academic panel devises the formal case study that has been structured to ensure that there is material relevant to all professions. The panel is also responsible for designing the extension questions, which are revealed for the first time at the competition event.
The UQ HCTC offers “real-life” practice in team-based problem solving, and competition between teams stimulates student motivation and engagement. The extracurricular design of the project helps to overcome some of the impediments faced by other pre-registration IPE projects.8,13-16 These barriers include:
Incompatible alignment of teaching blocks;
Student absence on clinical placements at different times;
Staff and student focus on professional identity; and
Differing professional requirements for IPE competencies.
There is an intense 4-week preparation period for the teams before the public event. The crucial output of the pre-event phase is a management plan developed by each team based on a clinical case study scenario. Each case is developed by a team of clinicians from a range of professional backgrounds and based on a complex real-life scenario reflecting a chronic health problem. The case is layered to acknowledge the challenges faced by an individual and his or her family and community. Complications are embedded to challenge students to look beyond their own single-profession sphere of interest and to explore evidence-based and real-world standards of practice. To increase the authenticity of the learning experience, a genuine patient or “standardised patient” (a trained actor) is available for a team interview to assist in the development of the management plan (Box 2).
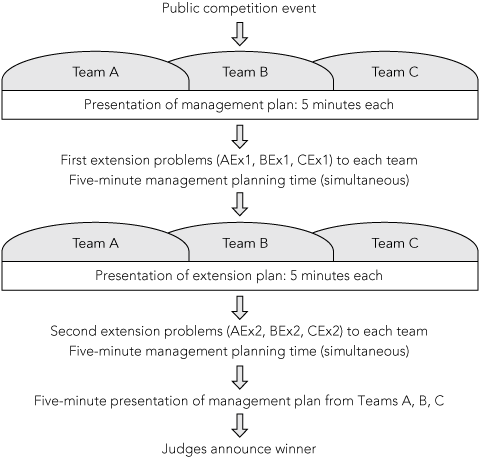
The teamwork skills developed in the pre-event phase are fundamental to success at the public event play-off, when each team is challenged with two rounds of previously unseen extension scenarios related to the case (Box 3). The judging panel is comprised of the patient and an external interprofessional team practising in the field relevant to the case study. The teams are assessed on multiple criteria: teamwork, collaboration, communication skills, prioritising professional input, understanding of different professional roles, and the degree to which the patient’s needs are integrated into management planning.
Partnership with the University of British Columbia, the home of the only other HCTC in existence. Access to the University of British Columbia’s HCTC event management know-how accelerated the concept-to-implementation phase at UQ;
A clear focus on sustainability through external sponsorship;
Establishment of a UQ HCTC alumni organisation to encourage student IPE leaders to carry their skills into the workplace;
Research on changes in student knowledge and attitudes to IPE, longitudinal behavioural change after graduation, and impact on the audience viewing the live event;
Authentic client involvement by recruiting a patient and carers to be interviewed by students and to be members of the judging panel; and
Ministerial support for the HCTC from Queensland Health as partners in health workforce reform and IPE.
The key challenges to implementing an HCTC at an institutional level are:
Obtaining seed funds;
Ensuring support from top management;
Recruiting the support of all the professions;
Inspiring final-year students to volunteer for an extracurricular event;
Managing a large performance event; and
Sustainability.
Experience conducting the 2007 and 2008 UQ HCTCs has demonstrated that these challenges have been comfortably overcome. Essential communication strategies for promoting expansion are an informative website (http://www.HealthCare TeamChallenge.com) and the ubiquitous YouTube video (for 2007 HCTC student participant reflections, see http://www.youtube. com/v/tooDdfgwKik; for footage of the 2008 event, see http://au.youtube.com/watch?v=qdxMANtPlhw).
- Rosalie A Boyce1
- Monica C Moran2
- Lisa M Nissen1
- Helen J Chenery3
- Peter M Brooks3
- 1 School of Pharmacy, The University of Queensland, Brisbane, QLD.
- 2 School of Health and Rehabilitation Sciences, The University of Queensland, Brisbane, QLD.
- 3 Faculty of Health Sciences, The University of Queensland, Royal Brisbane and Women’s Hospital, Brisbane, QLD.
We acknowledge the significant contribution of Emma Poulsen, Project Officer for the UQ HCTC; the academic advisory panel that supports the event; the student participants; and our partners and sponsors from industry, the professions, and the University of British Columbia. The UQ HCTC project has been funded by a UQ Faculty of Health Sciences IPE fellowship and the UQ Teaching and Learning Strategic Grants (large grants) scheme, including partnership funds from Queensland Health.
None identified.
- 1. Greiner AC, Knebel E, editors. Health professions education: a bridge to quality. Washington, DC: National Academies Press, 2003.
- 2. Harris MF, Zwar NA. Care of patients with chronic disease: the challenge for general practice. Med J Aust 2007; 187: 104-107. <MJA full text>
- 3. Canadian Health Services Research Foundation. Listening for direction II: national consultation on health services and policy issues for 2004–2007. Ottawa: CHSRF, 2004. http://www.chsrf.ca/other_documents/listening/pdf/LfD_II_Final_Report_e.pdf (accessed Jul 2008).
- 4. Productivity Commission. Australia’s health workforce. Productivity Commission research report. Canberra: Commonwealth of Australia, 2005. http://www.pc.gov.au/__data/assets/pdf_file/0003/9480/healthworkforce.pdf (accessed Mar 2009).
- 5. World Health Organization. The world health report 2006: working together for health. Geneva: WHO, 2006. http://www.who.int/whr/2006/en (accessed May 2008).
- 6. British Columbia Competency Framework for Interprofessional Collaboration. Leading interprofessional education and research. Vancouver: University of British Columbia College of Health Disciplines, 2008. http://www.chd.ubc.ca/files/file/BC%20Competency%20Framework% 20for%20IPC.pdf (accessed Aug 2008).
- 7. Pruitt SD, Epping-Jordan JE. Preparing the 21st century global healthcare workforce. BMJ 2005; 330: 637-639.
- 8. Stone N. Coming in from the interprofessional cold in Australia. Aust Health Rev 2007; 31: 332-340.
- 9. Lewis B, Stone N. Shaping a sustainable interprofessional education program. Focus Health Prof Educ 2007; 8 (3): 27-46.
- 10. Hammick M, Freeth D, Koppel I, et al. A best evidence systematic review of interprofessional education: BEME Guide No. 9. Med Teach 2007; 29: 735-757.
- 11. Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Washington, DC: National Academies Press, 2001.
- 12. Moran M, Boyce RA, O’Neill K, et al. The Health Care Team Challenge: extra-curricula engagement in inter-professional education (IPE). Focus Health Prof Educ 2007; 8 (3): 47-53.
- 13. Barr H. Unpacking interprofessional education. In: Leathard A, editor. Interprofessional collaboration: from policy to practice in health and social care. Hove, UK: Brunner-Routledge, 2003: 265-279.
- 14. Braithwaite J, Travaglia J. Inter-professional learning and clinical education: an overview of the literature. Canberra: Braithwaite and Associates and Australian Capital Territory Health Department, 2005. http://www.med.unsw.edu.au/medweb.nsf/resources/Projects7/$file/IPL,+clinical+ed+Lit+review+AbsoluteFinal.pdf (accessed Mar 2009).
- 15. Canadian Health Services Research Foundation. Teamwork in healthcare: promoting effective teamwork in healthcare in Canada: policy synthesis and recommendations. Ottawa: CHSRF, 2006. http://www.chsrf.ca/research_themes/pdf/teamwork-synthesis-report_e.pdf (accessed Aug 2008).
- 16. Kyrkjebø JM, Brattebø G, Smith-Strøm H. Improving patient safety by using interprofessional simulation training in health professional education. J Interprof Care 2006; 20: 507-516.






Abstract
Successful transition of students to competent work-ready health professionals requires an ability to work in health care teams.
Poor communication and teamwork practice has been implicated as a contributing source of error affecting patient safety.
Traditional university curriculum structures severely limit the time that students from different professions can spend together, learning about and from each other (interprofessional education [IPE]).
IPE initiatives need to focus on whole-of-system impacts and organisational sustainability.
The Health Care Team Challenge (HCTC) is a high-profile leadership strategy that engages students, academic staff, practising professionals, policymakers and industry in a whole-of-system approach to IPE and interprofessional practice. Interprofessional student teams compete at a live public event for a cash prize for the best management plan centred on a complex clinical case study.
National and international HCTCs are planned for future years.