Although there is a widespread belief that there has been an increase in babies’ birthweight in the past decade, there is a lack of Australian research to confirm this. The postulated increase in birthweight has been reported emotively in the media, with comments such as “. . . the weight of new mothers and babies rockets to record levels . . .”,1 “Fatter babies mean more c-sections” and “Babies are being born bigger than ever . . .”.2
Increases in birthweight have been reported overseas. In Canada, the proportion of babies born large for gestational age (LGA) increased from 8% in 1978 to 11.5% in 1995.3 This increase was principally attributed to increases in maternal body mass index (BMI), gestational weight gain, and height and a decrease in smoking during pregnancy.3 Similar findings from Sweden demonstrated an increase from 3.7% to 4.6% in the proportion of newborns weighing over 4500 g between 1992 and 2001, with the increase attributed to increased maternal BMI and reduced prevalence of smoking.4
The outcome of size at birth was assessed in three ways: i) mean birthweight, ii) proportion of babies weighing over 4000 g and/or over 4500 g and iii) proportion of babies born LGA. LGA was defined as > 90th centile for sex and gestational age, based on published Australian birthweight centiles for 1991–1994.5 The explanatory variables available for analysis included infant sex, maternal age, parity, smoking during pregnancy, pre-existing diabetes, gestational diabetes, hypertensive disorders during pregnancy, and maternal region of birth and year of birth. Babies were excluded from the analysis if their sex was indeterminate or unknown, their birthweight was missing or a probable outlier as defined by the Tukey method,6 and/or their gestational age was ≥ 43 weeks.
To investigate the association between LGA and the proposed explanatory variables over time, we used logistic regression analysis on the 1994–2005 data because smoking status was only collected in the MDC from mid 1993. Crude odds ratios (ORs) with 95% confidence intervals were estimated for all explanatory variables. Adjusted ORs were calculated by entering all significant explanatory variables, including year of birth, into the logistic regression model. Each variable entered the model if the likelihood-ratio test for its coefficient was significant (P < 0.01), apart from infant sex, which was included a priori.
A predictive logistic regression model was similarly established using all significant explanatory variables from the 1994 data alone (n = 79 125). The coefficients from the equation for this fitted model were then applied to data from subsequent years to calculate the predicted number of LGA babies, thus allowing for the changing frequency of the explanatory variables.7 The expected proportion of LGA babies was plotted against time and compared with the observed trend. If the observed and predicted values over time were not significantly different, this would suggest that the available explanatory variables account for all of the increase in LGA. Conversely, any difference between the observed and predicted proportions would be due to factors not included in the model.
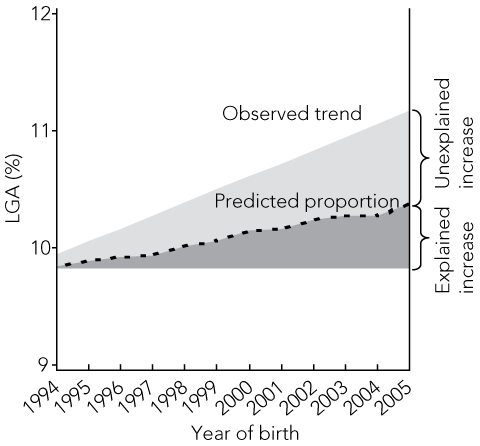
From 1990 to 2005, 1 273 924 singleton babies were born alive at term in NSW, after excluding 3858 due to missing, indeterminate or unknown sex, birthweight or gestational age. Over the 16-year study period, the mean birthweight increased significantly — by 23 g for boys and 25 g for girls (P for trend < 0.001, Box 1). The percentage of male infants with birthweight > 4000 g increased from 14.3% to 15.8% (10.5% increase), and the percentage with birthweight > 4500 g increased from 2.2% to 2.4% (9.0% increase); male infants born LGA increased from 9.2% to 10.8% (17.9% increase). The percentage of female infants with birthweight > 4000 g increased from 8.3% to 9.5% (15.2% increase), and the percentage with birthweight > 4500 g increased from 1.0% to 1.2% (20.0% increase); female infants born LGA increased from 9.1% to 11.0% (21.0% increase).
A number of maternal characteristics also changed significantly over time (Box 2). The proportion of women who reported smoking during pregnancy decreased over the study period, from 22.0% in 1994 to 13.8% in 2005. The proportion of women with reported gestational diabetes increased from 1.1% in 1990 to 4.6% in 2005, and the mean maternal age at delivery increased from 28.4 years to 30.4 years. There were no significant changes in maternal region of birth over time. The trend in mean birthweight for babies of women who underwent elective caesarean section and induction of labour was similar to the trend for those without these interventions.
A total of 952 671 babies born between 1994 and 2005 met the entry criteria for the logistic regression analysis. Crude and adjusted ORs are shown in Box 3. The factors most strongly associated with LGA were pre-existing and gestational diabetes, multiparity, maternal age ≥ 35 years and Polynesia as the maternal region of birth (Box 3). All proposed explanatory variables were statistically significant and were retained in the model, including year of birth.
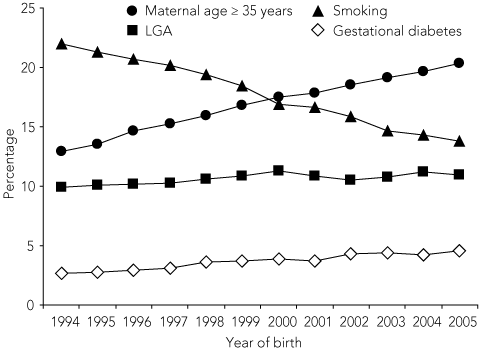
The increasing trend in the observed proportion of babies born LGA compared with the predicted proportion, adjusted for covariates, is shown in Box 4, and demonstrates that only some of the increase can be accounted for by the changing trends in maternal age, parity, smoking, diabetes, pregnancy hypertension and maternal region of birth. The increase from 1994 to 2005 in the percentage of babies born LGA was from 9.9% to 10.9%, but the percentage increase predicted by the model for the same time period was only 10.4%.
High birthweight may have important health implications for the infant, and has been shown to be associated with a high BMI in later life.8 There is evidence for a relationship between high birthweight and increased future risk of cancer,9,10 including Wilms’ tumour,11 infant and childhood leukaemia,12 osteosarcoma,13 astrocytoma,14 and breast,15,16 prostate17 and colon18 cancer. In addition, the future risk of asthma19 and type 1 diabetes20 is increased in high birthweight babies. The fetal origins hypothesis may provide an explanation for the fact that high birthweight may have lifelong health consequences.21
At the time of delivery, high birthweight may result in injury to the infant, with increased risk of shoulder dystocia and brachial plexus injury,22 or to the mother, with higher rates of caesarean section, fourth-degree perineal lacerations, prolonged hospital stay23 and postpartum haemorrhage.7,24 For these reasons, the increasing proportion of large babies is of concern. Further studies to ascertain all factors contributing to the increase in birthweight over time, including maternal pre-pregnancy BMI and weight gain during pregnancy, are warranted. In addition, estimation of the increase in high-birthweight babies is important to enable appropriate maternity health services planning. By means of illustration, 1429 more babies weighing > 4000 g were born in NSW in 2005 than in 1990.
Although a portion of the increase in babies born LGA over the 16-year study period can be attributed to variables we have studied, a larger portion is unexplained (Box 4). In other studies, increasing maternal pre-pregnancy weight and gestational weight gain have been implicated.3,4 Indeed, the prevalence of overweight or obesity among pregnant women in Australia is high.25 Data on maternal BMI or weight gain were not available. It may be important to limit gestational weight gain, although evidence for the effect of dietary intervention and physical activity to reduce gestational weight gain is conflicting.26 Randomised controlled trials investigating the limitation of weight gain during pregnancy are currently in the early stages of recruitment.27,28
Our findings are similar to the trends observed in other countries. In Sweden, the mean birthweight increased by 35 g (or an average of 3.5 g/year) between 1992 and 2001,4 and in Canada, the mean birthweight increased by 46 g (equivalent to 2.4 g/year) between 1978 and 1996.3 In comparison, an increase of 24 g between 1990 and 2005 (1.5 g/year) was observed in the NSW population studied. This lower rate of increase may in part be due to the fact that smoking among pregnant women is relatively more common in Australia (16.7% in NSW compared with 10.9% in Sweden, based on 2001 data4).
A strength of our study is the availability of a population health dataset that has been validated against the medical record. Birthweight is recorded in the MDC with high accuracy, and a 96.5% concordance with the medical record has been reported.29 Most variables have a good level of agreement with the medical record, with high κ values. For example, pregnancy hypertension as recorded in the MDC has a specificity of 99.5% and a sensitivity of 63.3%30 when compared with the medical record. The main shortcoming of our study is that we were unable to investigate several important factors, such as maternal pre-pregnancy weight and weight gain during pregnancy. In addition, there may have been changes over time, such as increased screening for gestational diabetes. Improved screening and resulting treatment for gestational diabetes over the study period could have reduced the number of infants born LGA.
1 Mean birthweight and 95% confidence intervals for male and female live-born, term singletons in New South Wales, 1990–2005
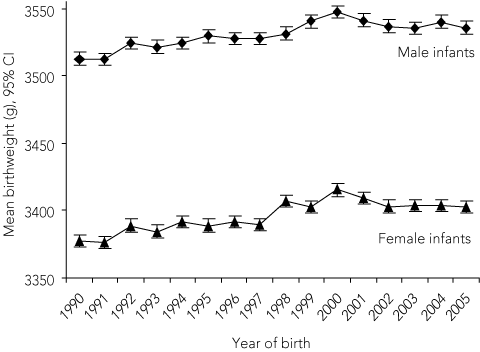
2 Trends over time for babies born large for gestational age (LGA) and the variables of maternal age, smoking and gestational diabetes
3 Crude and adjusted odds ratios (ORs) of being born large for gestational age (LGA) for 952 671 live-born, term singleton births in New South Wales, 1994–2005
Data are from the NSW Midwives Data Collection (1994–2005, n = 952 671). * LGA was defined as > 90th percentile based on published percentiles for sex and gestational age.5 † Adjusted for all characteristics shown and year of birth. ‡ Data for this characteristic were missing for 1379 records. § Data for this characteristic were missing for 1738 records. | |||||||||||||||
- Ruth M Hadfield1
- Samantha J Lain1
- Judy M Simpson2
- Jane B Ford1
- Camille H Raynes-Greenow1
- Jonathan M Morris3
- Christine L Roberts1
- 1 Perinatal Research and Population Health, Kolling Institute of Medical Research, University of Sydney, Sydney, NSW.
- 2 School of Public Health, University of Sydney, Sydney, NSW.
- 3 Department of Obstetrics and Gynaecology, Northern Clinical School, University of Sydney, Sydney, NSW.
We thank the hospital staff who collect these data. Ruth Hadfield and Camille Raynes-Greenow are funded by National Health and Medical Research Council (NHMRC) Post-doctoral Training Research Fellowships. Jane Ford is supported by the Health Research and Outcomes Network and an NHMRC Capacity Building Grant in population health research. Christine Roberts is supported by an NHMRC Senior Research Fellowship.
None identified.
- 1. Weaver C. SIDS risk for fat babies. Daily Telegraph (Sydney) 2007; 19 Aug. http://www.news.com.au/dailytelegraph/story/0,22049,22267780-5006010,00.html (accessed Feb 2009, link updated March 2009).
- 2. Schliebs M. Fatter babies mean more c-sections. The Australian 2008; 11 Jun. http://www.theaustralian.news.com.au/story/0,25197,23845721-26103,00.html (accessed Feb 2009).
- 3. Kramer MS, Morin I, Yang H, et al. Why are babies getting bigger? Temporal trends in fetal growth and its determinants. J Pediatr 2002; 141: 538-542.
- 4. Surkan PJ, Hsieh CC, Johansson AL, et al. Reasons for increasing trends in large for gestational age births. Obstet Gynecol 2004; 104: 720-726.
- 5. Roberts CL, Lancaster PA. Australian national birthweight percentiles by gestational age. Med J Aust 1999; 170: 114-118. <MJA full text>
- 6. Tukey JW. Exploratory data analysis. Reading, Mass: Addison Wesley, 1977: 44.
- 7. Ford JB, Roberts CL, Simpson JM, et al. Increased postpartum hemorrhage rates in Australia. Int J Gynaecol Obstet 2007; 98: 237-243.
- 8. Parsons TJ, Power C, Manor O. Fetal and early life growth and body mass index from birth to early adulthood in 1958 British cohort: longitudinal study. BMJ 2001; 323: 1331-1335.
- 9. Ross JA. High birthweight and cancer: evidence and implications. Cancer Epidemiol Biomarkers Prev 2006; 15: 1-2.
- 10. Ahlgren M, Wohlfahrt J, Olsen LW, et al. Birth weight and risk of cancer. Cancer 2007; 110: 412-429.
- 11. Puumala SE, Soler JT, Johnson KJ, Spector LG. Birth characteristics and Wilms tumor in Minnesota. Int J Cancer 2008; 122: 1368-1373.
- 12. Roman E, Simpson J, Ansell P, et al. Perinatal and reproductive factors: a report on haematological malignancies from the UKCCS. Eur J Cancer 2005; 41: 749-759.
- 13. Troisi R, Masters MN, Joshipura K, et al. Perinatal factors, growth and development, and osteosarcoma risk. Br J Cancer 2006; 95: 1603-1607.
- 14. Von Behren J, Reynolds P. Birth characteristics and brain cancers in young children. Int J Epidemiol 2003; 32: 248-256.
- 15. McCormack VA, dos Santos Silva I, Koupil I, et al. Birth characteristics and adult cancer incidence: Swedish cohort of over 11,000 men and women. Int J Cancer 2005; 115: 611-617.
- 16. Michels KB, Xue F. Role of birthweight in the etiology of breast cancer. Int J Cancer 2006; 119: 2007-2025.
- 17. Nilsen TI, Romundstad PR, Troisi R, Vatten LJ. Birth size and subsequent risk for prostate cancer: a prospective population-based study in Norway. Int J Cancer 2005; 113: 1002-1004.
- 18. Nilsen TI, Romundstad PR, Troisi R, et al. Birth size and colorectal cancer risk: a prospective population based study. Gut 2005; 54: 1728-1732.
- 19. Flaherman V, Rutherford GW. A meta-analysis of the effect of high weight on asthma. Arch Dis Child 2006; 91: 334-339.
- 20. Haynes A, Bower C, Bulsara MK, et al. Perinatal risk factors for childhood Type 1 diabetes in Western Australia — a population-based study (1980–2002). Diabet Med 2007; 24: 564-570.
- 21. Barker DJ. Fetal origins of coronary heart disease. BMJ 1995; 311: 171-174.
- 22. Raio L, Ghezzi F, Di Naro E, et al. Perinatal outcome of fetuses with a birth weight greater than 4500 g: an analysis of 3356 cases. Eur J Obstet Gynecol Reprod Biol 2003; 109: 160-165.
- 23. Stotland NE, Caughey AB, Breed EM, Escobar GJ. Risk factors and obstetric complications associated with macrosomia. Int J Gynaecol Obstet 2004; 87: 220-226.
- 24. Ford JB, Roberts CL, Bell JC, et al. Postpartum haemorrhage occurrence and recurrence: a population-based study. Med J Aust 2007; 187: 391-393. <MJA full text>
- 25. Callaway LK, Prins JB, Chang AM, McIntyre HD. The prevalence and impact of overweight and obesity in an Australian obstetric population. Med J Aust 2006; 184: 56-59. <MJA full text>
- 26. Guelinckx I, Devlieger R, Beckers K, Vansant G. Maternal obesity: pregnancy complications, gestational weight gain and nutrition. Obes Rev 2008; 9: 140-150.
- 27. Maternal Perinatal Clinical Trials Unit, University of Adelaide. Limiting weight gain in overweight and obese women during pregnancy to improve health outcomes: a randomised trial. http://www.health.adelaide.edu.au/og/research/mpctu.html#obesity (accessed Oct 2008).
- 28. Maternal Perinatal Clinical Trials Unit, University of Adelaide. Dietary and lifestyle advice for women with borderline gestational diabetes mellitus. http://www.health.adelaide.edu.au/og/research/mpctu.html#obgt (accessed Oct 2008).
- 29. Taylor L, Pym M, Bajuk B, et al. Part 8: validation study NSW Midwives Data Collection 1998. New South Wales Mothers and Babies 1998. NSW Public Health Bulletin Supplementary Series (State Publication no. (EPI) 000029) 2000; 11 (1): 97-99. http://www.publish.csiro.au/nid/227/issue/5090.htm (accessed Feb 2009).
- 30. Roberts CL, Bell JC, Ford JB, et al. The accuracy of reporting of the hypertensive disorders of pregnancy in population health data. Hypertens Pregnancy 2008; 27: 285-297.





Abstract
Objective: To determine whether the proportion of babies born large for gestational age (LGA) in New South Wales has increased, and to identify possible reasons for any increase.
Design and setting: Population-based study using data obtained from the NSW Midwives Data Collection, a legislated surveillance system of all births in NSW.
Participants: All 1 273 924 live-born singletons delivered at term (≥ 37 complete weeks’ gestation) in NSW from 1990 to 2005.
Main outcome measures: LGA, defined as > 90th centile for sex and gestational age using 1991–1994 Australian centile charts; maternal factors associated with LGA were assessed using logistic regression.
Results: The proportion of babies born LGA increased from 9.2% to 10.8% (18% increase) for male infants and from 9.1% to 11.0% (21% increase) for female infants. The mean birthweight increased by 23 g for boys and 25 g for girls over the study period. Increasing maternal age, higher rates of gestational diabetes and a decline in smoking contributed significantly to these increases, but did not fully explain them.
Conclusions: There is an increasing trend in the proportion of babies born LGA, which is only partly attributable to decreasing maternal smoking, increasing maternal age and increasing gestational diabetes.