Recent widely reported commentaries have questioned the necessity and appropriateness of the Australian Government’s whole-of-community approach to the prevention of overweight and obesity in children and adolescents.1-3 Opposition to the current childhood obesity prevention strategy is diverse and not consistent among commentators, but it does have some general underlying themes. Some question whether the current prevalence of childhood and adolescent obesity warrants the degree of concern and the language used to describe the problem. They also question whether the presence of overweight or even obesity in children and adolescents represents any real threat to health, and suggest that intervention for children and young adults at a population level may contribute to increasing the levels of eating disorders among young people. Others acknowledge the extent of the problem, but insist that any response should only be directed at those at highest risk; others dismiss the efficacy of any programs attempting to prevent obesity at a whole-of-community level. While it is usual and healthy for academics to debate the interpretation of research findings, there is a tendency for the more controversial views to get greater media attention purely because they are contrary.
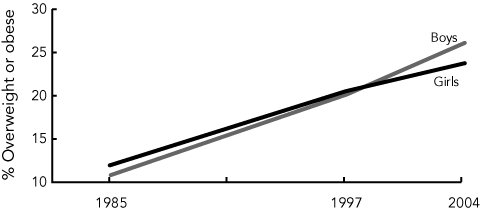
Although systems for monitoring the weight status of Australian children are limited, all of the available data (including those quoted by dissenters) show strong and consistent increases in the rates of combined overweight and obesity over the past 20 years, such that these now affect around one in every four schoolchildren4-8 (Box 1). It has been suggested that children who are classified as obese rather than overweight represent only a small proportion of Australian children, and that the proportion of obese children has stabilised in recent years. It is plausible that the rates of childhood obesity are levelling out, although it is not possible to say this with any degree of confidence, given the small number of data points that currently define the trends. In fact, a flattening in the level of increase in childhood obesity is apparent in data from other countries,9,10 and might be expected after such a rapid rise in recent decades. However, to suggest that a condition that currently affects 6%–8% of Australian schoolchildren is of little concern is hard to defend, as this equates to well over 260 000 school-aged children, based on 2005 census data. In addition, the 1.8% increase in the past 5 years, which is dismissed as insignificant by some commentators,1,3 equates to an additional 65 000 schoolchildren becoming obese.
Some commentators downplay the health implications of childhood and adolescent obesity,8,11 but there is considerable evidence that obesity results in immediate and longer-term health consequences in children, and especially adolescents. These range from orthopaedic complications, sleep apnoea and hepatic steatosis to more common manifestations of cardiovascular disease risk factors, type 2 diabetes and psychosocial problems, including low self-esteem and depression.12 There are also the problems associated with the common pattern of obesity progressing into adulthood, leading to earlier development of chronic diseases such as type 2 diabetes.13 More recent data have indicated clearly that many of these ill-health consequences of excessive weight are present in children and adolescents who are defined as overweight.14 As a consequence, early intervention in overweight children and adolescents appears justified, and highlighting the extent of the problem of overweight should not be dismissed as an attempt to exaggerate the level of weight problems in children and adolescents.
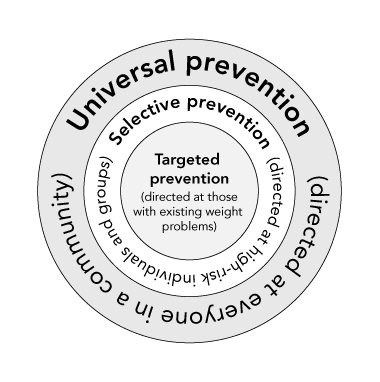
Despite widespread discussion over the past few decades, fundamental misunderstandings remain about the complementary nature of the whole-of-population and high-risk-group approaches in the prevention of chronic diseases.15 It is not possible to reduce the total burden of a weight-related disease in the community effectively by focusing solely on those at high risk, as the greatest contribution to overall burden of disease comes from those at moderate or low risk.16 Nor is it possible to deliver an appropriate and equitable solution to the obesity problem without addressing the needs of groups and individuals at high risk of weight-related illness. Neither strategy should be delivered at the expense of the other. Rather, a multilayered approach to prevention that includes less intense but broader-reaching programs needs to be combined with intensive programs to reach those at highest risk as well as those with an existing weight problem (Box 2).
Providing support only for programs and procedures that have a sufficiently strong evidence base to indicate their efficacy has been the mantra of health care expenditure for some time. Population-based prevention programs are not exempt from this principle. Some commentators have suggested that the current evidence for public health interventions in obesity is too limited to support their funding and implementation, especially when compared with clinical interventions.2 The nature of evidence that defines effective public health interventions and the timeframes and methods for collecting evidence make it meaningless to compare the efficacy of clinical and population interventions. In addition, the lack of past investment in community-based obesity strategies has meant that the number of studies on which to base assessments of evidence is sparse. However, the evidence base is growing as more reports on well designed and evaluated Australian17 and overseas18 studies are published. Given the potential reach and uptake of population-based strategies for preventing obesity, there is enough evidence to identify promising strategies that have the potential to contribute in a cost-effective manner to obesity prevention in children.19
It is important to recognise that an undue emphasis on thinness is a factor associated with the development of eating disorders. Not surprisingly, some commentators have raised concerns that interventions to prevent obesity at a population level may have unintended negative consequences, particularly in susceptible children and adolescents, and have advised against such an approach.20 However, a recent Cochrane review could find no evidence linking the increased focus on obesity prevention in children with increasing rates of eating disorders.21 Recent professional discussions have explored the utility of combined prevention programs that target both overweight and underweight. Despite some research suggesting that rates of disordered eating and dieting in teenage girls may be increasing,22 there are no data showing significant increases in the rates of true clinical eating disorders in Australia.23 While it would be appropriate to be cautious in defining the content of obesity prevention programs, it is important to be mindful that to do nothing is to put the health of children at greater risk. If anything, existing federally funded projects could be accused of being too cautious by focusing on sports participation and selective aspects of healthy eating without seeking to identify clear means of reducing the overall energy intake of children or increasing their overall energy expenditure.
- Timothy P Gill1
- Louise A Baur2
- Adrian E Bauman3
- Kate S Steinbeck4
- Leonard H Storlien1
- Maria A Fiatarone Singh2
- Jennie C Brand-Miller1
- Stephen Colagiuri1
- Ian D Caterson1
- 1 Institute of Obesity, Nutrition and Exercise, University of Sydney, Sydney, NSW.
- 2 Faculty of Medicine, University of Sydney, Sydney, NSW.
- 3 School of Public Health, University of Sydney, Sydney, NSW.
- 4 Royal Prince Alfred Hospital, Sydney, NSW.
None identified.
- 1. Childhood obesity epidemic “exaggerated”. Sydney Morning Herald 2008; 31 May. http://news.smh.com.au: 80/national/childhood-obesity-epidemic-exaggerated-20080531-2k3k.html (accessed Jun 2008).
- 2. Proietto J. Surgery will do more than education to fix the obesity epidemic. The Age (Melbourne) 2008; 19 Feb. http://www.theage.com.au/news/opinion/surgery-will-do-more-than-education-to-fix-the-obesity-epidemic/2008/02/18/1203190737640.html (accessed Jun 2008).
- 3. Duffy M. Don’t fall for the big fat lie when the proof of the padding is thin. Sydney Morning Herald 2008; 31 Dec. http://www.smh.com.au/news/opinion/dont-fall-for-the-big-fat-lie-when-proof-of-the-padding-is-thin/2007/12/14/1197568262871.html?page=fullpage (accessed Jun 2008).
- 4. Booth M, Okely AD, Denney-Wilson E, et al. NSW Schools Physical Activity and Nutrition Survey (SPANS) 2004. Summary report. Sydney: NSW Department of Health, 2006. http://www.health.nsw.gov.au/pubs/2006/pdf/spans_report.pdf (accessed Dec 2008).
- 5. Vaska VL, Volkmer R. Increasing prevalence of obesity in South Australian 4-year-olds: 1995–2002. J Pediatr Child Health 2004; 40: 353-355.
- 6. Goodman S, Lewis PR, Dixon AJ, Travers CA. Childhood obesity: of growing urgency [letter]. Med J Aust 2002; 176: 400-401. <MJA full text>
- 7. Magarey A, Daniels L, Boulton TJC. Prevalence of overweight and obesity in Australian children and adolescents: reassessment of 1985 and 1995 data against new standard international definitions. Med J Aust 2001; 174: 561-564. <MJA full text>
- 8. O’Dea JA. Gender, ethnicity, culture and social class influences on childhood obesity among Australian schoolchildren: implications for treatment, prevention and community education. Health Soc Care Community 2008; 16: 282-290.
- 9. New Zealand Ministry of Health. A portrait of health – key results of the 2006/07 New Zealand Health Survey. Wellington: New Zealand Ministry of Health, 2008. http://www.moh.govt.nz/moh.nsf/indexmh/portrait-of-health (accessed Dec 2008).
- 10. Sjöberg A, Lissner L, Albertsson-Wikland K, Mårild S. Recent anthropometric trends among Swedish school children: evidence for decreasing prevalence of overweight in girls. Acta Paediatr 2008; 97: 118-123.
- 11. Flegal KM, Tabak CJ, Ogden CL. Overweight in children: definitions and interpretation. Health Educ Res 2006; 21: 755-761.
- 12. World Health Organization. Obesity: preventing and managing the global epidemic. Report of a WHO Consultation. WHO Technical Report Series 894. Geneva: WHO, 2000. http://whqlibdoc.who.int/trs/WHO_TRS_894.pdf (accessed Dec 2008).
- 13. Dietz WH. Health consequences of obesity in youth: childhood predictors of adult disease. Paediatrics 1998; 101: 518-525.
- 14. Denney-Wilson E, Hardy LL, Dobbins T, et al. The association between BMI, waist circumference and chronic disease risk factors in Australian adolescents. Arch Pediatr Adol Med 2008; 162: 566-573.
- 15. Joffe M, Mindell J. A tentative step towards healthy public policy. J Epidemiol Community Health 2004; 58: 966-968.
- 16. Rose G. The strategy of preventive medicine. Oxford: Oxford University Press, 1992.
- 17. Sanigorski AM, Bell AC, Kremer PJ, et al. Reducing unhealthy weight gain in children through community capacity-building: results of a quasi-experimental intervention program, Be Active Eat Well. Int J Obesity 2008; 32: 1060-1067.
- 18. Taylor RW, Mcauley KA, Williams SM, et al. Reducing weight gain in children through enhancing physical activity and nutrition: the APPLE project. Int J Pediatr Obesity 2006; 1: 146-152.
- 19. Swinburn B, Gill T, Kumanyika S. Obesity prevention: a proposed framework for translating evidence into action. Obesity Rev 2005; 6: 23-33.
- 20. O’Dea JA. Prevention of child obesity: first, do no harm. Health Educ Res 2004; 20: 259-265.
- 21. Carter FA, Bulik CM. Childhood obesity prevention programs: how do they affect eating pathology and other psychological measures? Psychosom Med 2008; 70: 363-371.
- 22. Gonzalez A, Kohn MR, Clarke SD. Eating disorders in adolescents. Aust Family Physician 2007; 36: 614-619.
- 23. Ben-Tovim DI, Gilchrist PN, Walker MK. Evolving evidence and continuing uncertainties for eating disorders [editorial]. Med J Aust 2001; 175: 238-239.





Abstract
Recent reports have suggested that the problem of childhood and adolescent obesity has been exaggerated in Australia, and that community-wide obesity prevention initiatives are not warranted; we argue that this is not an accurate reflection of the situation.
Available data indicate that obesity affects 6%–8% of Australian schoolchildren, and that the proportion has continued to increase in recent years.
Childhood and adolescent obesity is associated with a wide range of immediate health concerns, as well as increasing the risk of disease in adulthood. Some weight-related health problems are also found in overweight children.
A range of strategies, including whole-of-community obesity prevention programs, will be required to tackle this problem.
Concerns about disordered eating in children and adolescents should not preclude appropriate action on childhood obesity.