In Australia, nearly a third of the population reside in rural and remote areas.1 Australians living in rural and remote regions are significantly over-represented in road transport-related injury and fatality figures.1-3 There is limited published information about the cost of rural road crashes in Australia. The Bureau of Transport Economics conservatively estimates that the cost of all Australian road crashes in 1996 totalled $15 billion.4 The largest portion of this cost is attributed to loss of life and permanent disability.4,5 Inpatient rehabilitation costs are a significant expense.6
Evidence suggests that road crashes in rural and remote areas cost significantly more than urban road crashes. In New Zealand, about 60% of the total cost of road injuries relates to crashes that occur in rural areas,5 even though only 22% of the NZ population live in rural areas.7 A fatal crash in rural NZ costs about NZ$4 million, compared with NZ$3.5 million for an urban fatal crash.5
Similar evidence of higher costs of road crashes in rural and remote Australia is not yet available because Australian crash costs have most often been estimated based on severity of injury type.8 These costs do not take into account the retrieval and transport costs of rural and remote road crash victims. As retrieval is often performed by fixed and rotary wing services, this is likely to be an underestimated element of road crash costs. In the 2006–07 financial year, the Queensland Emergency Medical System Coordination Centre (QCC) coordinated and tasked nearly 14 000 aeromedical retrievals and interhospital transfers (Statewide Clinical Coordination and Retrieval Service [SCCRS], Queensland Health, unpublished data).
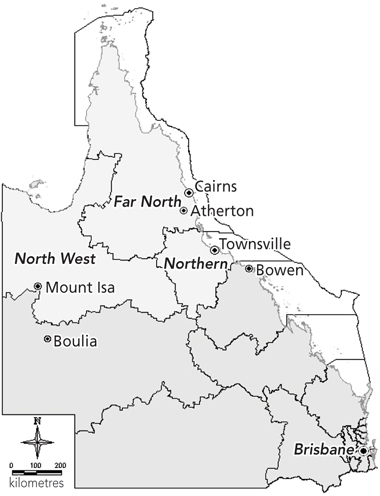
The Rural and Remote Road Safety Study was an in-depth examination of factors present in non-urban road crashes that led to the hospitalisation of at least one road user aged 16 years or older for a period of 24 hours or longer in Atherton, Cairns, Mount Isa and Townsville public hospitals. The study area was defined as the area of Queensland north of hospital Bowen in the east and Boulia in the west, including Gulf of Carpentaria and Torres Strait islands, but excluding the urban centres of Cairns and Townsville. It comprised a total land area of about 650 000 km2 (Box 1).
Tasking of road or air emergency retrieval was performed by the QCC based on factors including severity of the patient’s condition, flight priority, access to remote locations, and availability of local definitive care.9 QAS road ambulances were used if the crash scene was less than 30 minutes or 30 km away by road for critical-care patients, or less than 2.25 hours’ travelling time in non-critical cases.9
For rotary wing aircraft, the estimated cost was $5164/engine hour.10 The Bell 412 helicopters used by Emergency Management Queensland fly at about 200 km/h; straight-line distances were used to determine the duration of each flight in hours. Additionally, over 95% of rotary wing retrievals have a doctor and paramedic on board, costing $1800 and $800, respectively, per trip (SCCRS, unpublished data). These costs are added separately to the total engine hour costs for each flight because (i) they are based on proportion of shift (hourly basis), and (ii) not all flights require a paramedic and doctor on board — this decision is made at the discretion of the on-duty QCC medical coordinator.
There were 696 admitted casualties meeting the study criteria, and retrieval transport data were available for 614 (88%) of these (Box 2). QAS road ambulances provided initial emergency retrieval for most casualties (73%), followed by private transport, then rotary wing and fixed wing aircraft.
Due to the nature of the injuries incurred and the limited services available in small rural hospitals, 413 casualties (67%) were transferred from the first hospital to one of the region’s major hospitals (primarily Cairns or Townsville). A larger proportion of these services were provided by fixed wing and helicopter services (Box 2).
The estimated cost of emergency retrieval and transport to the first hospital for 534 patients (excluding the 80 transported by private vehicles) was over $1 million (Box 3). Of the 413 casualties who required transfer from the first treating hospital to a major hospital, 17 were then transported to a third hospital, nearly all (16) by fixed wing at a further cost of $170 000 (Box 3). The estimated total cost of retrievals and interhospital transfers over the study period was about $3.7 million, equating to an annual cost of $1.1 million.
The actual costs of the initial acute admission for the 253 casualties admitted to TTH, including the 68 casualties admitted to the ICU, are shown in Box 4.
Across the four public hospitals within the study area, casualties occupied a total of 6360 acute bed-days. Of these, 734 were ICU bed-days. The total estimated cost of casualty hospitalisation over the study period was nearly $6.7 million (Box 5). This equates to an annual estimated cost of almost $2 million for the initial acute hospitalisation of rural and remote road crash victims requiring hospital admissions of at least 24 hours in northern Queensland.
The total estimated hospitalisation costs may be slightly overestimated because all patients with head injuries were transferred to TTH, thus inflating the average cost per bed-day. However, the retrospective nature of data collection and the composite nature of data sources mean it is likely that the overall cost has been underestimated. Obtaining more accurate and widely accessible data should be a goal for future research to better estimate road crash costs across the country, particularly in rural and remote settings. Further, no attempt has been made to address the economic and human costs of post-hospital rehabilitation (either actual or ideal) and long-term disability. The cost of this care is likely to be substantial, based on costs of inpatient rehabilitation reported from other countries.6
This study goes some way toward showing that the burden of road crash costs in rural and remote areas is substantial. Rural and remote road crashes are more likely than urban road crashes to be serious, due to faster travelling speeds, greater alcohol and drug use, lower rates of seatbelt use, and delays in emergency response and retrieval times.11,12 Additional factors are longer travelling distances, a greater variety of vehicle types, and poorer road quality.11 Although our study was based in northern Queensland, similar road crash costs may be faced by health departments in other rural and remote areas, such as western New South Wales, northern South Australia, Western Australia and the Northern Territory, that encompass large distances, sparsely populated areas and greater crash severity.5
To reduce costs associated with retrieval and transport, it may be possible to avoid or delay patient transportation from regional, rural and remote health care facilities through the use of telemedicine and teleradiology. For example, SCCRS, via the QCC in Townsville, currently provides telemedicine services to Palm Island Hospital. A 6-month evaluation of this service reported that telemedicine prevented 10 unnecessary aeromedical retrievals and six night flights, equating to an average annual saving of between $206 000 and $352 000.10
1 Northern Queensland study area
 | |||||||||||||||
|
Delineated areas are statistical divisions. Light shading indicates study area. | |||||||||||||||
2 Modes of transport to hospital from crash site and for interhospital transfers
From crash site to first hospital |
From first hospital to major hospital |
||||||||||||||
Received 23 April 2008, accepted 14 October 2008
- Teresa M O’Connor1
- Heather A Hanks1
- Mark S Elcock2
- Richard C Turner1
- Craig Veitch3,4
- 1 School of Medicine and Dentistry, James Cook University, Townsville, QLD.
- 2 Statewide Clinical Coordination and Retrieval Service, Queensland Health, Townsville, QLD.
- 3 Faculty of Health Sciences, University of Sydney, Sydney, NSW.
- 4 Community Based Health Care Research Unit, Royal Rehabilitation Centre Sydney, Sydney, NSW.
We wish to acknowledge financial assistance provided by the Motor Accident Insurance Commission, the Centre for Accident Research and Road Safety – Queensland, and the Queensland Government. Our thanks also to Queensland Health staff of hospitals in the study area and QAS staff from the Northern and Far Northern regions of Queensland.
None identified.
- 1. Australian Institute of Health and Welfare. Rural, regional and remote health: a study on mortality. Canberra: AIHW, 2007. (AIHW Cat. No. PHE 95.)
- 2. National Injury Prevention Advisory Council. Directions in injury prevention. Report 1: research needs. Canberra: NIPAC, 1999. http://www.health.nsw.gov.au/public-health/health-promotion/injury-prevention/priorities/directions-in-ip-report1.pdf (accessed Nov 2008).
- 3. Henley G, Kreisfeld R, Harrison JE. Injury deaths, Australia 2003–04. Adelaide: Australian Institute of Health and Welfare, 2007. (AIHW Cat. No. INJCAT 89.)
- 4. Australian Government Bureau of Transport Economics. Road crash costs in Australia. Report 102. Canberra: Bureau of Transport Economics, 2000. http://www.bitre.gov.au/publications/47/Files/r102.pdf (accessed Nov 2008).
- 5. NZ Government Ministry of Transport. The social cost of road crashes and injuries. Wellington: Ministry of Transport, 2007. http://www.transport.govt.nz/socialcost/ (accessed Nov 2008).
- 6. Miller T, Langston E, Lawrence B, et al. Rehabilitation costs and long-term consequences of motor vehicle injury. Report No. DOT HS 810 581. Washington, DC: National Highway Traffic Safety Administration, 2006. http://www.nhtsa.dot.gov/people/injury/research/RehabCosts/ (accessed Nov 2008).
- 7. Statistics New Zealand. Demographics trends: 2007 reference report. Wellington: Statistics New Zealand, 2008. http://www.stats.govt.nz/analytical-reports/dem-trends-07/ (accessed Nov 2008).
- 8. Andreassend DC. A framework for costing accidents and accident types. Accid Anal Prev 1985; 17: 111-117.
- 9. Elcock M. Tasking considerations for aeromedical operations — standard operating procedure. Townsville, Qld: Statewide Clinical Coordination and Retrieval Service, 2006.
- 10. Mathews KA, Elcock MS, Furyk JS. The use of telemedicine to aid in assessing patients prior to aeromedical retrieval to a tertiary referral centre. J Telemed Telecare 2008; 14: 309-314.
- 11. Veitch C, Sheehan M, Turner R, et al. The economic, medical and social costs of road traffic crashes in rural north Queensland: a 5-year multi-phase study. In: Proceedings of the 8th National Rural Health Conference; 2005 Mar 10–13; Alice Springs, NT. http://www.abc.net.au/rural /events/ruralhealth/2005/papers/8nrhcfinal paper00466.pdf (accessed Nov 2008).
- 12. Veitch C, O’Connor T, Steinhardt D, et al. Rural and remote road crashes: piecing together the story. In: Proceedings of the 9th National Rural Health Conference; 2007 Mar 7–10; Albury, NSW. http://9thnrhc.ruralhealth.org.au/program/docs/papers/oconnor_C3.pdf (accessed Nov 2008).





Abstract
Objective: To estimate costs of retrieval, transport and acute medical services associated with road crashes in northern Queensland from March 2004 to June 2007.
Design, setting and participants: Case study of 696 people aged 16 years or older who had been involved in a road crash in the study area (all areas north and west of Bowen, excluding the urban areas of Townsville and Cairns) and had been admitted to hospital for a minimum of 24 hours after the crash. Data on mode of retrieval, acute care provided and total costs were obtained for each patient.
Main outcome measures: Method of retrieval or transport; length of stay in intensive care unit (ICU) and/or hospital for each patient; costs of retrieval, transport and inhospital care.
Results: Retrieval data were collected for 614 of the 696 study participants (88%). Most primary retrievals (446; 73%) occurred by road. More than half of interhospital transfers were undertaken by fixed or rotary wing services. Casualties in the study occupied a total of 6360 bed-days, of which 734 were ICU bed-days. The total retrieval, transport and acute hospital care costs of road crash victims in northern Queensland over the study period were calculated to be approximately $10.4 million.
Conclusion: The costs associated with rural and remote road crashes in northern Queensland represent a considerable economic burden.