* This article is based on a presentation given by Graham Brown at the Clinical Research Excellence Conference 2007 (CRX07) in Melbourne.
Australia has achieved health indices that are among the best in the world, with a mixed public–private system and a health workforce trained predominantly with substantial government support of education and health. It is essential to ensure that the excellent past performance is sustained through appropriate attention to training of the next generation, who will translate knowledge into improved patient outcomes. The almost exclusive emphasis that is now being placed on service provision in hospitals, without accompanying attention to education and research, could put that record at risk.1 It is, however, reassuring that the nation is showing determination to address the major exception to a good report in health — Indigenous health.
The 10-year health trends for Australia and the developed world suggest that we are likely to be managing large numbers of older patients with chronic diseases, with more demand for “personalised” medicine and information that enables patients and families to participate in management. There will be increased use of very expensive technology, and practitioners without full medical training (eg, psychologists, practice nurses, nurse practitioners and physician assistants) will take more active roles. Hospitals will promote shorter stays, greater efficiencies, more open displays of outcome data, and a response to community demand for quality and safety (Box 1). If societal pressure leads to increasing emphasis on community, more attention will be given to areas of extreme need for under-served populations, particularly Indigenous populations.
In Australia, the first clinical academic departments of universities were established in the mid 20th century,1 some 50 years after their counterparts were promoted in Europe and North America.2 Until the late 1970s, it was generally accepted that the public hospitals had an important role to play in training the medical workforce of the future. With increasing trends towards payment based solely on the services delivered, public hospitals are seen by some as business units of state health service delivery units, with minimal acknowledgement that education and research are essential for improved health outcomes.
Clinical academics are the “threatened species” of medicine.3 Perhaps extinction of this species is an unintended consequence of assets being stripped from public health and education, but not compensated for by research and educational training programs such as those in the United States. The effects of weakening and undermining these foundations are not immediately visible, but they weaken the system in the long term. A strong case has been put forward in the United Kingdom for the National Health Service to promote research and an environment that enables people to undertake research.4 It has further been argued that academic centres that provide service delivery contribute to improved health outcomes in the short and longer term. Application of the philosophy of “no service without research” facilitates the process of researchers and practitioners co-creating relevant knowledge to improve health outcomes.
Better patient outcomes are achieved in academic clinical settings because of closer attention to protocols, delivery of better care in a clinical trial setting, and ready access to new interventions provided by health care practitioners with experience in their benefits or side effects.5 In an environment that facilitates interaction between research and clinical practice, collaborative projects and programs can be developed. These allow patient-focused questions to be addressed and research translation that takes local health care settings into account. Furthermore, it has been clearly shown that Australia has benefited in economic terms from investment in medical research.5
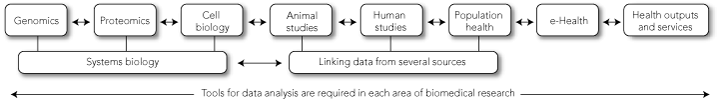
Biomedical research is a spectrum — from genetics through to protein products, laboratory-based cell biology, animal studies, human studies, population health and individualised medicine — that continually undergoes transition, most recently with the advent of “e-health” (Box 2). Translational research is an iterative process, from molecules to medicines to millions, but discovery and application are just as important in the other direction, from populations to patients to genetics. It is a high priority to develop systems for linking datasets from different areas of research and service, to allow the best decisions to be made for patient care and to facilitate research. Integrating a research culture into patient management must be acknowledged by both hospital managers and government bodies as a vital component of good patient care.
The initiative of the National Health and Medical Research Council (NHMRC) in creating Centres of Clinical Research Excellence has been an important mechanism for enhancing the quality of clinical research in Australia and mentoring a new generation of clinical academics. The intent of the program is to reward successful clinical researchers and expand their potential to produce high-quality research, provide high-quality clinical research training, and translate research findings into health policy and improved health outcomes (Box 3).6 The Centres provide career-based training in patient-oriented research for investigators, support staff, trial managers, and leaders in disciplines including nursing, pharmacy, physiotherapy and social sciences. They have already enriched local academic environments, provided initial funding for investigators to develop autonomy and independence, and contributed to developing the capacity of the Australian pharmaceutical industry to conduct trials initiated by investigators and industry. The mentoring role for students has been important, and funding has enabled increased investment, and improvements in study design and analysis.
1 Changes in emphasis for hospitals1
Shorter hospital stays
Greater focus on costs
Less emphasis on capacity building
Research can be considered an extra
No financial incentives to be world leaders in clinical services, or to provide conditions to attract world’s best practitioners
Possible increases in privatisation
Quality and safety focus
Safety and service framework
Clinical governance
Open display of outcome data
Requirement for evidence to lead change
Need for “health services research”
Received 3 August 2008, accepted 19 January 2009
- Graham V Brown2
- Tania C Sorrell3
- 1 University of Melbourne, Royal Melbourne Hospital, Melbourne, VIC.
- 2 Nossal Institute for Global Health, University of Melbourne, Melbourne, VIC.
- 3 Centre for Infectious Diseases and Microbiology, Western Clinical School, University of Sydney, Sydney, NSW.
Graham Brown has served on NHMRC committees and is on the Management Committee of BioGrid (a platform for sharing life science information). Tania Sorrell has sat on advisory boards for antifungal drugs for Pfizer, Merck, Gilead and Schering-Plough, and received investigator-initiated grants and travel assistance from Pfizer, Merck and Gilead.
- 1. Penington DG. Rediscovering university teaching hospitals for Australia. Med J Aust 2008; 189: 332-335. <MJA full text>
- 2. Flexner A. Medical education in the United States and Canada: a report to the Carnegie Foundation for the Advancement of Teaching. New York: Carnegie Foundation for the Advancement of Teaching, 1910.
- 3. The death of the US academic medical centre [editorial]? Lancet 2007; 369: 532.
- 4. Cooksey D. A review of UK health research funding. London: Her Majesty’s Stationery Office, 2006.
- 5. Grant J (Chairman). Sustaining the virtuous cycle for a healthy, competitive Australia: investment review of health and medical research. Final report, Dec 2004. Canberra: Commonwealth of Australia, 2004.
- 6. National Health and Medical Research Council. Centres for Clinical Research Excellence funding policy. Canberra: NHMRC, 2008. http://www.nhmrc.gov.au/grants/apply/ccre/_files/CCRE_Funding_Policy_2008.pdf (accessed Apr 2009).





Abstract
Integration of research and education into health care delivery leads to improved outcomes and facilitates rapid translation of results into policy and practice.
Australia is at great risk of losing the important contribution of clinical research conducted in our public hospital system. This risk is increasing as research and educational training are targeted for expenditure reduction in the current business models of health service delivery, which focus only on short-term outcomes.
The Centres of Clinical Research Excellence Scheme — initiated by the National Health and Medical Research Council (NHMRC) — is an excellent step towards redressing this problem, but it cannot succeed in isolation.
We must improve and optimise care through promotion of attractive sustainable career pathways to provide strong clinical and translational research capabilities in hospital settings that address current health priorities and new disciplines.
Targeted investment in talented people is the greatest long-term contribution that governments can make to guarantee quality in national systems of health.