Aboriginal Australians, compared with the general Australian population, have high rates of premature mortality from preventable chronic diseases.1 The association between higher morbidity and mortality rates from preventable chronic diseases and lower socioeconomic status is well established.2 In remote areas of the Northern Territory, just over half (52.7%) the Aboriginal and Torres Strait Islander people are in the lowest income quintile;3 government pensions and allowances are their main source of income.
Socioeconomic factors have a big impact on food and nutrient intakes and food purchasing patterns;4-6 material and economic constraints are recognised as key determinants of dietary intake.7 High-quality nutrition is known to protect against chronic diseases,8 but energy-dense, nutrient-poor foods cost much less than nutrient-rich foods.9,10 Applying incrementally increasing cost constraints to a typical French diet resulted in a diet high in refined carbohydrates and low in fresh meat, fruit and vegetables.11 These findings led to the “economics of food choice” theory — that people’s dietary decisions, when made within the context of sustained budgetary constraints, are driven by maximising energy value for money (dollars per megajoule [$/MJ]), resulting in energy-dense, nutrient-poor diets.12
Our study was conducted in an island community (population, about 1700 people,13 of whom 93% are Indigenous) located 550 km from a major urban centre. At the time, community food outlets included a community store, two convenience shops (takeaway outlets), a school canteen and a government-sponsored, aged-care program providing weekly fresh food parcels to 16 community residents.14 Alcoholic beverages were prohibited. Foods acquired through subsistence procurement were not included in our analysis.
Data for all food outlets were combined (community food supply). Food and beverage weights were expressed per edible fraction and their energy and nutrient contents were obtained from the Australian Food and Nutrient Database (AUSNUT 1999).15 Volumes were converted to standard weight using the AUSNUT conversion factor. Food items were aggregated into major food groups and subgroups, as defined by the AUSNUT Food Grouping System.15 The percentage contribution of each major food group and subgroup to total energy available through the community food supply was determined.
An aggregated daily energy requirement for the study population was determined, based on age- and sex-distribution, anthropometric data and estimated physical activity level. The mean height and weight for adult age-groups between 19 and > 70 years (19–30; 31–50; 51–70; > 70 years) were determined from available anthropometric data.16 For those < 18 years in the population, the mid-point of the estimated energy requirement range for each of the categories of age and sex was used to determine an estimated energy requirement. For all age-groups a physical activity level of 1.6 was applied.17
Energy available through the community food supply on an estimated per person daily basis of 9.45 MJ was comparable with the estimated average daily requirement for this population of 9.42 MJ, and comparable with the 9.07 MJ daily requirement reported for the Australian population.18
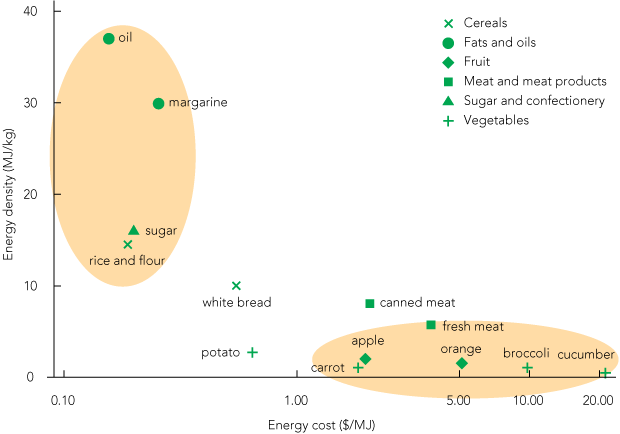
As illustrated in Box 1, cereal and cereal products, sugar and confectionery, and fats and oils contributed most to dietary energy relative to dietary cost. In contrast, nutrient-dense foods, such as meat and meat products, fish and seafood, fruit and vegetables, contributed least energy relative to cost. Energy costs (in $/MJ) of a range of foods found in the community store are given in Box 2. Sugar, cooking oil, rice, margarine and white flour are the lowest-cost options, providing dietary energy at minimal cost (< 0.26 $/MJ), compared with fresh vegetables, meat and fruit, which provided energy at a much higher cost. Box 3 highlights the up-to-100-fold range in energy costs of foods in this community store.
The most important finding in our study was the marked gradient in cost per MJ between low-quality foods, rich in refined carbohydrates and fats, and the high-quality, nutrient-dense foods recommended in the Australian guide to healthy eating,19 illustrating the inverse relationship between energy density and energy cost, consistent with published data.
The results of our study highlight the importance of modelling the food supply available to Indigenous people in remote areas to identify practical modifications that can be achieved at minimum cost. Achieving nutritional recommendations at minimum cost, however, is a challenge, as often taste and convenience are compromised,20 and the resulting diet is markedly changed from the typical diet, with much less fresh produce.21 On the basis of self-selected diets, it has been shown that, under normal circumstances, high-quality diets cost more.22
A primary motive for our study was to better understand why the poor-quality dietary patterns of remote Indigenous communities23 have changed little over more than two decades. This dietary pattern has been attributed to conservative food preferences resulting from the historical government policy, from the time of early European settlement through to the early 1970s, of providing rations for Indigenous Australians.24 This pattern is reinforced by contemporary issues of limited availability of healthy food choices, high food costs and limited household-storage and food-preparation capacity.25
Our study shows that low income is a powerful driver of food choice — a factor compounded in remote communities by high costs of perishable foods, such as meat, fruit and vegetables.26 Our study focuses on one large, remote community, but similar socioeconomic conditions and disparities in food costs exist across all Indigenous communities in Australia.
This is the first demonstration of the relationship between energy density, energy cost and dietary patterns for an economically marginalised Indigenous population in Australia. By placing nutritional improvement in an economic, rather than an individual behavioural change framework, our study highlights the investment that improving nutrition for Indigenous people in remote communities will require.
1 Community food supply — percentage energy and cost contributions to total energy and total diet cost, and dietary energy cost, for each of the major food groups
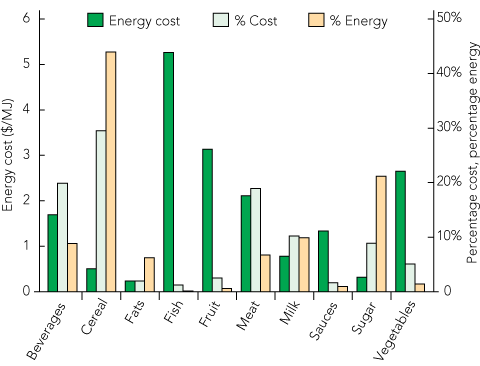
- Julie K Brimblecombe1
- Kerin O’Dea2
- 1 Preventable Chronic Diseases, Menzies School of Health Research, Royal Darwin Hospital Campus, Darwin, NT.
- 2 Sansom Institute of Health Research, University of South Australia, Adelaide, SA.
We thank the Arnhem Land Progress Association, the community school principal, the community health centre, and the proprietor of the convenience store for providing access to store sales and invoice data; Yalu’Marnggithinyaraw (particularly Elaine Maypilama, Joanne Garnggulkpuy, Dorothy Bepuka and Dorothy Yunggirrnga) for supporting and facilitating this study in the community, and for bringing to our attention the primary importance of cost of food and income in determining food choices for community members; Robyn Liddle for expertise in database design and application, and Joseph McDonnell for statistical expertise. Julie Brimblecombe was funded by the National Health and Medical Research Council (NHMRC) (Grants 124319; 320860); the National Heart Foundation (PhD scholarship); and the Co-operative Research Centre for Aboriginal Health (PhD scholarship).
None identified.
- 1. Australian Bureau of Statistics. The health and welfare of Australian Aboriginal and Torres Strait Islander peoples, 2003. Canberra: ABS, 2003. (ABS Cat. No. 4704.0.)
- 2. Turrell G, Mathers C. Socioeconomic inequalities in all-cause and specific-cause mortality in Australia: 1985-1987 and 1995-1997. Int J Epidemiol 2001; 30: 231-239.
- 3. Australian Bureau of Statistics. National Aboriginal and Torres Strait Islander social survey, Northern Territory, 2002. Canberra: ABS, 2004 (ABS Cat. No. 4714.7.55.001.)
- 4. Irala-Estevez JD, Groth M, Johansson L, et al. A systematic review of socio-economic differences in food habits in Europe: consumption of fruit and vegetables. Eur J Clin Nutr 2000; 54: 706-714.
- 5. Martikainen P, Brunner E, Marmot M. Socioeconomic differences in dietary patterns among middle-aged men and women. Soc Sci Med 2003; 56: 1397-1410.
- 6. Turrell G, Hewitt B, Patterson C, et al. Socioeconomic differences in food purchasing behaviour and suggested implications for diet-related health promotion. J Hum Nutr Diet 2002; 15: 355-364.
- 7. Drewnowski A, Darmon N. Food choices and diet costs: an economic analysis. J Nutr 2005; 135: 900-904.
- 8. Iqbal R, Anand S, Ounpuu S, et al. Dietary patterns and the risk of acute myocardial infarction in 52 countries: results of the INTERHEART study. Circulation 2008; 118: 1929-1937.
- 9. Darmon N, Briend A, Drewnowski A. Energy-dense diets are associated with lower diet costs: a community study of French adults. Public Health Nutr 2004; 7: 21-27.
- 10. Drewnowski A, Darmon N, Briend A. Replacing fats and sweets with vegetables and fruits — a question of cost. Am J Public Health 2004; 94: 1555-1559.
- 11. Darmon N, Ferguson EL, Briend A. A cost constraint alone has adverse effects on food selection and nutrient density: an analysis of human diets by linear programming. J Nutr 2002; 132: 3764-3771.
- 12. Drewnowski A. Fat and sugar: an economic analysis. J Nutr 2003; 133: 838S-840S.
- 13. Australian Bureau of Statistics. Australian Bureau of Statistics 2006 Census tables. Canberra: ABS, 2007. (ABS Cat. No. 2068.0.)
- 14. Brimblecombe J, Mackerras D, Clifford P, O’Dea K. Does the store-turnover method still provide a useful guide to food intakes in Aboriginal communities? Aust N Z J Public Health 2006; 30: 444-447.
- 15. Food Standards Australia New Zealand (FSANZ): Australian Food and Nutrient Database. AUSNUT 1999. Canberra: FSANZ, 1999.
- 16. Brimblecombe J, Mackerras D, Garnggulkpuy J, et al. Leanness and type 2 diabetes in a population of Indigenous Australians. Diabetes Res Clin Pract 2006; 72: 93-99.
- 17. Australian Government Department of Health and Ageing; National Health and Medical Research Council; Ministry of Health (NZ). Nutrient Reference Values for Australia and New Zealand. Dietary energy. Canberra: DoHA, NHMRC, 2006. http://www.nrv.gov.au/energy.htm (accessed Mar 2009).
- 18. Australian Bureau of Statistics, Department of Health and Aged Care. National Nutrition Survey: nutrient intakes and physical measurements, Australia, 1995. Canberra: ABS, 1998. (ABS Cat. No. 4805.0.)
- 19. Kellet E, Smith A, Schmerlaib Y. The Australian guide to healthy eating. Adelaide: Children’s Health Development Foundation; Women’s and Children’s Hospital (South Australia); and Faculty of Health and Behavioural Sciences (Deakin University, Victoria), 1998. http://www.health.gov.au/internet/main/publishing.nsf/Content/E384CFA588B74377CA256F190004059B/$File/fd-cons-5.pdf (accessed Mar 2009, link updated May 2009)
- 20. Foley WL. How does dietary advice for diabetes management divide families? Asia Pac J Clin Nutr 2004; 13 (Suppl): S61.
- 21. Darmon N, Ferguson EL, Briend A. Impact of a cost constraint on nutritionally adequate food choices for French women: an analysis by linear programming. J Nutr Educ Behav 2006; 38: 82-90.
- 22. Cade J, Upmeier H, Calvert C, Greenwood D. Costs of a healthy diet: analysis from the UK Women’s Cohort Study. Public Health Nutr 1999; 2: 505-512.
- 23. Lee AJ, O’Dea K. Apparent dietary intake in remote Aboriginal communities. Aust J Public Health 1994; 18: 190-197.
- 24. National Health and Medical Research Council. Nutrition in Aboriginal and Torres Strait Islander Peoples: an information paper. Canberra: NHMRC, 2000: 1-267. http://www.nhmrc.gov.au/publications/synopses/_files/n26.pdf (accessed Mar 2009).
- 25. National Aboriginal and Torres Strait Islander Nutrition Working Party. National Aboriginal and Torres Strait Islander nutrition strategy and action plan, 2000-2010, and first phase activities, 2000-2003. Melbourne: National Public Health Partnership, 2001: 1-55. http://www.nphp.gov.au/publications/signal/natsinsa1.pdf (accessed Mar 2009).
- 26. Harrison MS, Coyne T, Lee AJ, et al. The increasing cost of the basic foods required to promote health in Queensland. Med J Aust 2007; 186: 9-14. <MJA full text>





Abstract
Objective: To explore the relationship between dietary quality and energy density of foods (MJ/kg) and energy cost ($/MJ) for an Aboriginal population living in a remote region of northern Australia.
Design: For a 3-month period in 2005, we collected food and non-alcoholic beverage supply data from food outlets available to the study population. From these data, we compared the energy density of foods with their energy cost.
Main outcome measures: Energy density and energy cost of food purchases.
Results: The diet of the study population was high in refined carbohydrates and low in fresh fruit and vegetables. Foods with high energy density were associated with lower costs and contributed disproportionately to energy availability.
Conclusion: The energy–cost differential between energy-dense, nutrient-poor foods and energy-dilute, nutrient-rich foods influences the capacity of Australian Aboriginal people living in remote communities to attain a healthy diet. This is consistent with the “economics of food choice” theory, whereby people on low incomes maximise energy availability per dollar in their food purchasing patterns, and has particular relevance for developing nutrition policy and strategies in Aboriginal communities, where poor nutrition is a major determinant of preventable chronic disease.