Australian Aboriginal people have survived and continue to adapt to rapid changes imposed on them by a dominant mainstream culture. A legacy of this disruption is a high incidence of cardiovascular disease (CVD).1-3 For Aboriginal populations in Central Australia, CVD is the leading cause of morbidity and mortality.1,4
Much of the disparity in CVD between Aboriginal people and the wider Australian population is likely attributable to social, environmental, behavioural and biological determinants that stem from a history of systemic social disadvantage.3 Dyslipidaemia (disruption of blood lipid concentrations) is a biological determinant that is known to accelerate atherosclerosis and CVD development.5-7 Aboriginal people in Central Australia have a propensity to atherosclerosis, owing to an atherogenic lipid profile characterised by low high-density lipoprotein cholesterol (HDL-C) concentration and small low-density lipoprotein cholesterol (LDL-C) particle size.6
Clinical management of dyslipidaemia using lipid-modifying therapy, such as statins (HMG-CoA [hydroxymethylglutaryl-coenzyme A] reductase inhibitors), is a common approach to primary and secondary prevention.8,9 Under the Australian Pharmaceutical Benefits Scheme (PBS), access to subsidised lipid-modifying therapy depends on individuals meeting eligibility criteria. These criteria were amended in 2006 and now include Aboriginal-specific criteria guided by different lipid thresholds and diabetes status (Box 1).8 The revised treatment eligibility criteria were developed using an evidence-based review of the Heart Protection Study, the United Kingdom Prospective Diabetes Study (UKPDS) and the Australian National Diabetes Information Audit (ANDIAB), as well as expert consultation.10 The studies informing the criteria are based largely on results from relatively privileged populations of European origin. Traditional absolute CVD risk calculators such as the Framingham equation have previously demonstrated poor translation in Aboriginal contexts.11
In 1995, CVD risk factor surveys were conducted in three Central Australian Aboriginal communities, with 68%–85% of the eligible population screened.6,12,13 Participants’ ages at baseline ranged from 15 to 82 years (mean, 36 years), and 42% of participants were male. Results were returned to communities, and individual participants were informed of their risk factor status after the baseline survey.
Collection of clinical data (anthropometry; plasma glucose, lipid and fibrinogen concentrations; LDL-C particle size; urinary albumin–creatinine ratio [ACR]; blood pressure) has been described elsewhere.5,6,12 Routine immunonephelometry (Boehringer Mannheim, Germany) was used for measuring levels of apolipoprotein B. LDL-C concentrations were estimated using the Friedewald equation in subjects with triglyceride levels < 4 mmol/L.14
Outcomes were defined as follows, based on information in hospital, PHC or death records:
Atherosclerotic CVD: clinically diagnosed ischaemic heart disease, ischaemic stroke or peripheral vascular disease (International classification of diseases, 10th revision [ICD-10] codes I20–I25, I63–I69, I70–I89; or ICD-9 codes 410–414, 433–438, 440–459). Hospital admissions and emergency presentations coded as cardiovascular signs and symptoms were investigated further, as was evidence of CVD provided from pathology test results, angiograms, stress tests and other radiology reports.
Diabetes: ICD-10 codes E10–E15 or ICD-9 code 250, two or more blood glucose readings ≥ 11.1 mmol/L, or prescription of hypoglycaemic medication.
Hypertension: ICD-10 codes I10–I15 or ICD-9 codes 401–405, three or more blood pressure readings ≥ 140/90 mmHg, or prescription of antihypertensive medication.
Chronic kidney disease: ICD-10 code N18 or ICD-9 code 585, two or more glomerular filtration rate estimates < 60 mL/min/1.73 m2, or three or more ACR measurements ≥ 3.4 mg/mmol.
Smoking: self-reported from baseline survey and subsequent PHC records.
Participants were stratified by their eligibility for lipid therapy according to the 2006 PBS criteria (Box 1), on the basis of baseline data and subsequent diagnoses in medical records during follow-up (preceding any first CVD event). As familial hypercholesterolaemia, family history of CVD and postmenopausal status were not known, the proportions eligible may be underestimated. For simplicity, 50 years was used as a surrogate age for menopause.
According to the 2006 PBS criteria, 334 of the 659 Aboriginal participants without CVD at baseline (50.7%) were eligible for PBS-subsidised lipid therapy by the end of follow-up in 2004–2005 (Box 1). Those who fit the PBS criteria were almost five times more likely to have a CVD event than those who did not (relative risk, 4.87; 95% CI, 2.19–10.80), with 35 PBS-eligible and seven ineligible individuals experiencing an event. Sensitivity of the Aboriginal-specific criteria was high, while specificity was moderate. Compared with the general PBS criteria (under which 37.5% of Aboriginal participants would be eligible), inclusion of Aboriginal-specific criteria made the guidelines more sensitive (83% v 74%) but less specific (52% v 65%) (Box 1).
PBS eligibility was associated with older age and male sex (Box 2). Glycaemic status and lipid characteristics at baseline reflect the PBS criteria, which selected for individuals with diabetes and dyslipidaemia. Total cholesterol, triglyceride, and apolipoprotein B (LDL-C particle number) concentrations were elevated in the eligible group, while HDL-C concentration was lower and LDL-C particle size smaller. HDL-C concentrations were characteristically low across both groups, with 86.2% of all participants free of CVD at baseline recording a concentration below 1 mmol/L.
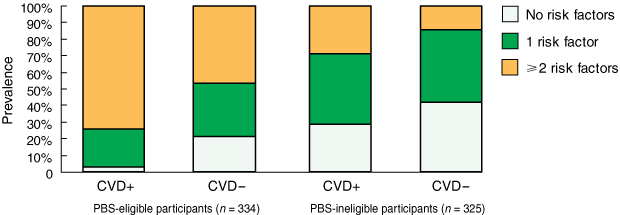
We examined other risk factors to identify clinical characteristics that might better recognise people at risk of primary CVD. The number of coexisting non-lipid risk factors (hypertension, microalbuminuria or macroalbuminuria, smoking, and elevated fibrinogen concentration) that were diagnosed in individuals at baseline or any time prior to first CVD event was examined. Of the PBS-eligible population who experienced CVD events, 74% had two or more of these risk factors, whereas of the eligible population who did not have a CVD event, 47% had two or more risk factors (Box 3).
We investigated the effect of adding further conditions to improve the specificity of the PBS criteria. These conditions were: i) age > 35 years; ii) two or more coexisting non-lipid risk factors; and iii) age > 35 years and two or more coexisting non-lipid risk factors. Individuals with total cholesterol > 6.5 mmol/L (suggestive of familial hypercholesterolaemia) were included regardless of whether they satisfied the other conditions, as the benefit of statins is uncontested in these people. All three sets of conditions improved the specificity of the current guidelines, with sensitivity reduced but not significantly so (Box 4). The incidence of CVD events and the relative risk of the eligible population experiencing CVD using any of the three proposed criteria are greater than those found when using the original guidelines because of exclusion of those at least risk.
Lipid-lowering therapy is important in primary and secondary prevention of CVD. For secondary prevention, it plays an uncontested role in reducing CVD irrespective of lipid characteristics. In this study, the inclusion of people with previous CVD in the analysis revealed a higher incidence, increased relative risk and greater sensitivity for the PBS-eligible population. This reiterates the notion that those with a prior history of CVD have a higher absolute risk of subsequent CVD and will benefit most from statin therapy.7,15 Our results demonstrate that current PBS lipid treatment guidelines identify a group of Central Australian Aboriginal people at high risk of primary and secondary CVD events, albeit with low specificity.
A high proportion of individuals in this community-based cohort had characteristically low HDL-C concentrations and small LDL-C particle size, reflective of a strongly pro-atherogenic dyslipidaemia. Low HDL-C concentrations may be indicative of insulin resistance, given that markers of the metabolic syndrome were also prevalent. Further investigation is required to establish the relationship between HDL-C, insulin resistance and CVD development in this population. However, given that there is an established link between high HDL-C levels and reduced CVD risk, the importance of treatment regardless of total cholesterol levels is evident, as low HDL-C is presumably an element contributing to increased absolute risk.16
Lipid treatment criteria need to be sensitive enough to cover high-risk individuals, but also specific so those with low absolute risk are not medicated unnecessarily. Primary prevention strategies need to account for absolute risk rather than lipid threshold criteria alone.17 The older PBS criteria for Aboriginal people prior to the 2006 amendment were less sensitive, as known risk factors required patients to have prerequisite threshold lipid levels, and the presence of diabetes did not automatically confer eligibility. Review of the UKPDS and ANDIAB studies by the Pharmaceutical Benefits Advisory Committee revealed that older people with long-term diabetes are considered a high-risk population.10 Diabetes is a major disease among Aboriginal people, affecting nearly a third aged over 55 years, and with a lower age of onset — Aboriginal people aged 25–34 years are 7.2 times more likely than other Australians to have diabetes.18 Before 2006, there was not strong evidence to support lipid therapy for young Aboriginal people with diabetes. The inclusion of all Aboriginal people with diabetes in the 2006 PBS criteria identifies a high-risk group, as do the different lipid threshold criteria centred on low HDL-C concentrations. Both these additional criteria have improved sensitivity, with 83% of participants in our cohort who experienced CVD events for the first time during the study period being PBS-eligible.
Given the economic, medical and social implications of medicating such a large proportion of people (50.7% of this population and about 20% of all Australians aged 30–74 years19), consideration of additional eligibility criteria may be warranted. Age of primary CVD event was dramatically younger in this Aboriginal cohort than in the general Australian population, and this must be recognised in indentifying at-risk individuals. In this cohort, 24% of people who experienced atherosclerotic CVD events were aged less than 35 years. Three of these 10 individuals had baseline cholesterol levels higher than 7 mmol/L (the other seven were above 5 mmol/L), suggesting familial hypercholesterolaemia. Notwithstanding the possibility of familial hypercholesterolaemia in younger people, limiting treatment on the basis of age > 35 years or number of non-lipid risk factors, or both, would result in a two- to threefold decrease in the number of eligible people and improved specificity, with a non-significant reduction in sensitivity.
Medical intervention with lipid-modifying therapy is only one aspect of CVD prevention. Both the National Heart Foundation of Australia and Cardiac Society of Australia and New Zealand guidelines and the PBS guidelines recommend lifestyle interventions such as physical activity and healthy eating before commencing lipid therapy.16,18 It should be acknowledged that social determinants are strong drivers of health, and that socioeconomic restrictions and access to and supply of fresh produce can make adherence to lifestyle interventions difficult. Policies and structures need to be conducive to such changes so CVD management and prevention do not rely solely on pharmaceutical therapies.
1 PBS eligibility criteria for lipid-lowering treatment,8 and cardiovascular disease (CVD) outcomes in 659 participants, stratified by their eligibility status
2 Baseline characteristics of PBS-eligible* and PBS-ineligible populations
3 Prevalence of coexisting non-lipid risk factors,* by participants’ PBS eligibility and cardiovascular disease (CVD) event status
 | |||||||||||||||
- Joanne N Luke1
- Alex Brown2
- David N O’Neal3
- Kerin O’Dea4
- Alicia J Jenkins3
- Margaret Kelaher5
- James D Best3
- Kevin G Rowley1
- 1 Onemda VicHealth Koori Health Unit, Centre for Health and Society, School of Population Health, University of Melbourne, Melbourne,
- 2 Centre for Indigenous Diabetes and Vascular Disease Research, Baker IDI Heart and Diabetes Institute, Alice Springs, NT.
- 3 Department of Medicine (St Vincent’s Hospital), University of Melbourne, Melbourne, VIC.
- 4 Sansom Institute, University of South Australia, Adelaide, SA.
- 5 Centre for Health Policy and Program Evaluation, School of Population Health, University of Melbourne, Melbourne, VIC.
We thank the Elders, community members and medical service providers of the Central Australian communities involved in the project; and Peter Howard, Leah Johnston, Zaimin Wang, Zhiqiang Wang and Andrea Neale for expert assistance. This study was funded by a National Health and Medical Research Council (NHMRC) “HOMELANDS” Program grant. Kevin Rowley is supported by an NHMRC Senior Research Fellowship.
Alex Brown received support from Alphapharm to attend the Cardiac Society of Australia and New Zealand Conference in Adelaide in 2008. There was no associated impact or influence on the development of this article.
- 1. Li SQ, Guthridge SL. Mortality in the Northern Territory: 1981–2000. Darwin: NT Department of Health and Community Services, 2004.
- 2. Australian Bureau of Statistics and Australian Institute of Health and Welfare. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples, 2008. Canberra: Commonwealth of Australia, 2008. (ABS Cat. No. 4704.0, AIHW Cat. No. IHW 21.)
- 3. Brown AD, Morrissey MJ, Sherwood JM. Uncovering the determinants of cardiovascular disease among Indigenous people. Ethn Health 2006; 11: 191-210.
- 4. Dempsey KE, Condon JR. Mortality in the Northern Territory, 1979–1997. Darwin: Territory Health Services, 2000.
- 5. de Backer G, de Bacquer D, Kornitzer M. Epidemiological aspects of high density lipoprotein cholesterol. Atherosclerosis 1998; 137 Suppl: S1-S6.
- 6. O’Neal DN, Piers LS, Iser DM, et al. Australian Aboriginal people and Torres Strait Islanders have an atherogenic lipid profile that is characterised by low HDL-cholesterol levels and small LDL particles. Atherosclerosis 2008; 201: 368-377.
- 7. McDermott R, Rowley KG, Lee AJ, et al. Increase in prevalence of obesity and diabetes and decrease in plasma cholesterol in a central Australian Aboriginal community. Med J Aust 2000; 172: 480-484. <MJA full text>
- 8. Australian Government Department of Health and Ageing. PBS-eligibility criteria for lipid lowering drugs fact sheet. Canberra: DoHA, 2006. http://www.health.gov.au/internet/main/publishing.nsf/content/lipid_eligibilitycriteria.htm (accessed Mar 2008).
- 9. Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of cholesterol lowering with simvastatin in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet 2002; 360: 7-22.
- 10. National Prescribing Service. Revised PBS criteria for lipid-modifying drugs (October, 2006). Sydney: NPS, 2007. http://www.nps.org.au/health_professionals/publications/nps_radar/issues/current/february_2007/pbs_lmd_criteria (accessed Apr 2008).
- 11. Wang Z, Hoy WE. Is the Framingham coronary heart disease absolute risk function applicable to Aboriginal people? Med J Aust 2005; 182: 66-69. <MJA full text>
- 12. Rowley KG, Iser DM, Best JD, et al. Albuminuria in Australian Aboriginal people: prevalence and associations with components of the metabolic syndrome. Diabetologia 2000; 43: 1397-1403.
- 13. Wang Z, Knight S, Wilson A, et al. Blood pressure and hypertension for Australian Aboriginal and Torres Strait Islander people. Eur J Cardiovasc Prev Rehabil 2006; 13: 438-443.
- 14. Friedewald WT, Levy RI, Fredrickson DS. Estimation of the concentration of low-density lipoprotein cholesterol in plasma, without use of the preparative ultracentrifuge. Clin Chem 1972; 18: 499-502.
- 15. Collins R, Armitage J, Parish S, et al; Heart Protection Study Collaborative Group. Effects of cholesterol-lowering with simvastatin on stroke and other major vascular events in 20536 people with cerebrovascular disease or other high-risk conditions. Lancet 2004; 363: 757-767.
- 16. Barter PJ, Rye KA. High density lipoproteins and coronary heart disease. Atherosclerosis 1996; 121: 1-12.
- 17. Tonkin AM, Lim SS, Schirmer H. Cardiovascular risk factors: when should we treat [editorial]? Med J Aust 2003; 178: 101-102. <MJA full text>
- 18. Australian Bureau of Statistics. National Aboriginal and Torres Strait Islander Health Survey, 2004–05. Canberra: ABS, 2006. (ABS Cat. No. 4715.0.)
- 19. Chen L, Rogers SL, Colagiuri S, et al. How do the Australian guidelines for lipid-lowering drugs perform in practice? Cardiovascular disease risk in the AusDiab Study, 1999–2000. Med J Aust 2008; 189: 319-322. <MJA full text>





Abstract
Objective: To evaluate the extent to which the current Pharmaceutical Benefits Scheme (PBS) guidelines for patient eligibility for lipid-lowering medication are applicable to Aboriginal people in Central Australia.
Design, setting and participants: A 10-year cohort study of 659 Aboriginal people who participated in population-based cardiovascular disease (CVD) risk factor surveys in 1995 and who were free of CVD at baseline, for the period from 1995 to 2004–2005 or until first CVD event. Evidence of atherosclerotic CVD (ischaemic heart disease, ischaemic stroke, and peripheral vascular disease) was sought from hospital, primary health care and death records. PBS eligibility was assigned according to the current PBS criteria, which were amended in 2006 to include Aboriginal-specific criteria, using participants’ baseline (1995) and 10-year follow-up data.
Main outcome measures: Proportions of PBS-eligible and PBS-ineligible participants who had CVD events during the study period; sensitivity and specificity of the criteria.
Results: Of 42 participants who had CVD events during the study period, 35 were PBS-eligible (incidence, 1130/100 000 person-years; relative risk compared with PBS-ineligible population, 4.87 [95% CI, 2.19–10.80]) and seven were PBS-ineligible. PBS eligibility was associated with older mean age (37 v 32 years) and male sex (48% v 37%), with 50.7% of participants (334/659) meeting eligibility criteria. The mean high-density lipoprotein cholesterol level at baseline was very low in both groups (0.81 v 0.87 mmol/L). The current PBS guidelines have low specificity (52%) in this population, which was found to improve (to 71%–82%) by incorporating additional non-lipid criteria (age and multiple non-lipid risk factors).
Conclusion: The current PBS lipid treatment criteria, which include any Aboriginal person with diabetes and less stringent cholesterol thresholds than the previous version, identify a group at very high risk of CVD. Global risk assessment may better identify those at risk.