Cardiovascular disease (CVD) is the major cause of premature death among adult Aboriginal Australians, and contributes to a reduced life expectancy.1 Age-specific death rates from CVD in Aboriginal people are estimated to be four to seven times the rates in the general population.2 Despite these statistics, there is almost no information on the incidence of CVD among Aboriginal people, as there have been few opportunities to follow cohorts in longitudinal studies, especially among urban populations.3
The only sizeable study to report the incidence of coronary heart disease (CHD) in Aboriginal people comes from a remote community in the Northern Territory, where the rate of CHD events was 11.0 per 1000 person-years among participants for whom a Framingham score could be calculated.4 To investigate whether those findings were applicable to other Aboriginal populations, we measured cardiovascular events in the Perth Aboriginal Atherosclerosis Risk Study (PAARS) cohort, an urban-dwelling population.5 Our aim was to determine the incidence of cardiovascular events in a cohort of urban adult Aboriginal people without known CHD.
The PAARS has been described in detail previously.5 Briefly, an atherosclerosis risk factor study was conducted in 1998–1999 among 998 residents of Perth, Western Australia, who identified themselves as Aboriginal Australians. The mean age of participants was 40 years (range, 18–80 years).
Perth is a city of 1.6 million people, of whom less than 2% are Aboriginal.6 At the time of initial assessment (1998–1999), the PAARS cohort was representative of the broader adult Aboriginal population of Perth in age structure, but with a higher proportion of employed people.
Outcome data were obtained through record linkage to population-based administrative databases, facilitated by the WA Data Linkage System. The external dataset (the PAARS cohort data) was electronically linked to a range of databases that included hospital morbidity data for public and private hospitals in WA (1980–2006) and deaths recorded in the WA Registry of Births, Deaths and Marriages (1998–2006). Probabilistic matching of records was based on name, date of birth, sex, and last known residential address. The validity of the matching for hospital morbidity in the general population has been assessed, with false positives and false negatives each estimated to be 0.11%.7
After excluding the records of unmatched participants, we divided the cohort into those with and without a history of CHD. Using the Kaplan–Meier method, the cumulative incidence of CHD to 9 years was estimated for participants with no history of CHD. The cohort was stratified by age at baseline into four groups (< 35, 35–44, 45–54 and ≥ 55 years) for comparison with the event rate reported from a remote community.4 The incidence of CHD events per 1000 person-years was calculated, with follow-up time assigned proportionally for those who were in two age groups during the study period. (For instance, if a person followed up for 7 years was 43 years of age at baseline, they would contribute 2 person-years to the 35–44-year age group and 5 person-years to the 45–54-year age group, if they did not have a CHD event.) Sex-specific rates were also calculated.
Finally, the age-group and sex-specific rates were compared with summary data published by Wang and Hoy from their investigations in a remote NT Aboriginal community in 1992–1995.4 The study participants from the community were followed to December 2003, with first CHD events (fatal or non-fatal) identified from hospital and death records.
Perth lies within the traditional lands of the Nyoongar people of south-western WA. The PAARS was conducted in collaboration with the Derbarl Yerrigan Health Service Inc (formerly Perth Aboriginal Medical Services) and in accordance with National Health and Medical Research Council (NHMRC) criteria for health and medical research among Indigenous Australians.9 All participants in the PAARS study provided written informed consent using a form of consent developed in consultation with community representatives.
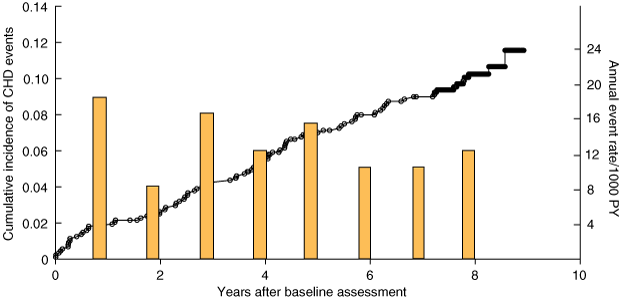
The annual CHD event rate was highest in the first year after assessment (18/1000 person-years) and varied between 8 and 16 per 1000 person-years in subsequent years (Box 1). The cumulative hazard estimate for a first CHD event to 9 years was 12.6/1000 person-years in the PAARS cohort, compared with 11.0/1000 person-years in the remote community (Box 2). The incidence of CHD increased with age, and was little different for men and women. Analysis by age group showed a tendency towards a higher CHD event rate in the PAARS cohort than the remote community in the 35–44-year age group (especially for men), but the opposite pattern in the ≥ 55-year age group. However, the confidence intervals were large and the differences not statistically significant (Box 2).
After adjustment for age (sex was not associated with the risk factors assessed), factors associated with risk of a cardiac event in the PAARS cohort were a history of diabetes, overweight or obesity (indicated by BMI), smoking, and hypertension, but not waist circumference (Box 3). PAARS cohort participants with no history of CHD at baseline (which includes those who either did or did not experience a CHD event during follow-up) were characterised by a high proportion of overweight or obesity, with more than three-quarters having a BMI > 25 kg/m2. Compared with Aboriginal people from the remote community, they were older and had a higher proportion of reported diabetes, as well as higher mean blood pressure (especially among the women). However, rates of current smoking were significantly lower in the PAARS cohort than the remote community. Over 35% of men and 40% of women in the PAARS cohort had never smoked. The main risk factors present at baseline are shown in Box 4.
Our results showed that the CHD event rate was similar in PAARS participants (12.6/1000 person-years) to the rate in the remote NT population (11.0/1000 person-years). However, the overall rate for those living in the remote community would be higher than this figure, as it did not include the 202 participants (23%) who had insufficient data to calculate a Framingham risk score. For those excluded, the rate was estimated to be 17.8/1000 person-years (95% CI, 11.9–26.6/1000 person-years).4
Risk factors for cardiovascular disease (especially smoking, diabetes and obesity) were highly prevalent in both cohorts. Although some studies have found waist circumference to be a better predictor of diabetes among Aboriginal people than BMI,10 our results showed that higher BMI, but not waist circumference, was associated with a higher incidence of CHD events.
Although the city-dwellers were less likely to be current smokers, blood pressure, prevalence of diabetes and measures of obesity were higher in this group. The higher blood pressure and greater prevalence of obesity may reflect the higher mean age of the PAARS cohort. Lower smoking rates in the PAARS cohort may be related to several factors, including greater exposure to anti-smoking messages in the city, legislation precluding smoking in the workplace (the PAARS cohort contained a higher proportion of employed people than the broader Perth Aboriginal population), and higher levels of education. It is possible that a sedentary lifestyle and easier access to a greater variety of food (including take-away food) are related to the greater prevalence of obesity among city-dwellers, although the higher average age of the PAARS participants may be sufficient explanation. Also, there were some years between the baseline data collections: the data reported by Wang and Hoy were collected between 1992 and 19954 and those for the PAARS cohort in 1998–1999. The 3–7-year gap may have encompassed social changes that influenced health behaviours such as smoking habits, diet and exercise in one or both settings. The risk factors for the PAARS cohort were measured only at baseline, and so there is no information on their progression, regression or treatment over the intervening 7 years.
1 Cumulative incidence of CHD events since baseline assessment (line) and annual event rate per 1000 person-years (PY) (bars) for the PAARS cohort
 | |||||||||||||||
|
CHD = coronary heart disease. PAARS = Perth Aboriginal Atherosclerosis Risk Study. | |||||||||||||||
2 Incidence of CHD events in the PAARS cohort compared with incidence in a remote Aboriginal community in the Northern Territory, by age group and sex*
PAARS cohort without previous CHD (n = 891) |
|||||||||||||||
3 Comparison of CHD event rates per 1000 person-years for PAARS participants with and without common risk factors for CHD
- Pamela J Bradshaw1
- Helman S Alfonso1
- Judith C Finn1,2
- Julie Owen1
- Peter L Thompson1,2
- 1 School of Population Health, University of Western Australia, Perth, WA.
- 2 Sir Charles Gairdner Hospital, Perth, WA.
Our study was supported by a grant-in-aid from the Heart Foundation of Australia. The Aboriginal Advisory Committee includes representatives from the Aboriginal Health Council of WA, Derbarl Yerrigan Health Service Inc, the Heart Foundation of Australia, Diabetes WA and the Canning Division of General Practice. The Community Reference Group members are Darryl Kickett, David Kelly, Debbie Stobie, Roz Yarran, Tracey Kickett, Sharon Bushby, Lyn Dimer, Francine Eades and Tiew-Hwa Katherine Teng.
None identified.
- 1. Trewin D, Madden R. The health and welfare of Australia’s Aboriginal and Torres Strait Islander peoples, 2005. Canberra: Australian Bureau of Statistics and Australian Institute of Health and Welfare, 2005. (ABS Cat. No. 4704.0; AIHW Cat. No. IHW 14.)
- 2. Australian Bureau of Statistics. Australian social trends 2002. Canberra: ABS, 2002. (ABS Cat. No. 4102.0.) http://www.ausstats.abs.gov.au/ausstats/subscriber.nsf/0/C0A01711EAD 911BFCA256BCD007D7F10/$File/41020_2002.pdf (accessed Mar 2009).
- 3. Grove N, Brough M, Canuto C, Dobson A. Aboriginal and Torres Strait Islander health research and the conduct of longitudinal studies: issues for debate. Aust N Z J Public Health 2003; 27: 637-641.
- 4. Wang Z, Hoy WE. Is the Framingham coronary heart disease absolute risk function applicable to Aboriginal people? Med J Aust 2005; 182: 66-69. <MJA full text>
- 5. Thompson PL, Bradshaw PJ, Veroni M, Wilkes ET. Cardiovascular risk among urban Aboriginal people. Med J Aust 2003; 179: 143-146. <MJA full text>
- 6. Australian Bureau of Statistics. 1996 census data: Perth. Basic community profile. http://www.abs.gov.au/AUSSTATS/abs@.nsf/d8874b08a9e70711ca2570960003cd61/a7966f52203c6441ca2570dd00270190!OpenDocument (accessed Mar 2009).
- 7. Holman C, Bass A, Rouse I, Hobbs M. Population-based linkage of health records in Western Australia: development of a health services research linked database. Aust N Z J Public Health 1999; 23: 453-459.
- 8. World Health Organization. Obesity — preventing and managing the global epidemic: report of a WHO consultation on obesity. Geneva: WHO, 1998.
- 9. National Health and Medical Research Council. National statement on ethical conduct in research involving humans — June 1999. Canberra: NHMRC, 1999.
- 10. Wang Z, Hoy WE. Body size measurements as predictors of type 2 diabetes in Aboriginal people. Int J Obes Relat Metab Disord 2004; 28: 1580-1584.





Abstract
Objective: To determine the incidence of coronary heart disease (CHD) events in an urban Aboriginal population.
Design, setting and participants: Cohort study of 906 Aboriginal people without CHD from 998 who had undergone risk-factor assessment in the Perth Aboriginal Atherosclerosis Risk Study (PAARS) in 1998–1999. PAARS cohort data were electronically linked to a range of databases that included Western Australian hospital morbidity data and death registry data. We analysed data from January 1980 to December 2006 to identify previous admissions for CHD from 1980 to baseline (1998–1999) and new events from baseline to 2006.
Main outcome measure: First CHD event (hospital admission or death).
Results: There were 891 linked records for the 906 participants without previous CHD. The event rate was 12.6/1000 person-years (95% CI, 10.2–15.6/1000 person-years). Annual CHD event rates ranged from 8 to 18/1000 person-years. After adjustment for age (sex was not associated with the risk factors assessed), factors associated with risk of a CHD event in the PAARS cohort were a history of diabetes, overweight or obesity (indicated by body mass index), smoking, and hypertension, but not waist circumference. People with these risk factors were 1.9–2.7 times more likely to experience a CHD event. Compared with previously published information from a remote Aboriginal community in the Northern Territory, the incidence of CHD events among urban-dwelling Aboriginal people was not significantly different (P > 0.05 overall and for subgroups defined by age and sex).
Conclusions: City-dwelling Aboriginal Australians have an incidence of CHD events comparable to that of Aboriginal people living in remote northern Australia.