We studied 4569 patients admitted to the ICU of St Thomas’ Hospital, London, from 2002 to 2006. For each patient, we had the date of admission to and discharge from the ICU. We modelled the probability of discharge using a longitudinal survival model.1 Patients who died were censored. We modelled day of the week as a categorical variable, with Wednesday as the reference category. The model controlled for age, APACHE II (Acute Physiology and Chronic Health Evaluation) score, whether the patient was being filtrated or ventilated, and presence of health care-acquired infection. Software from the BUGS (Bayesian inference Using Gibbs Sampling) Project2 was used for the analysis.
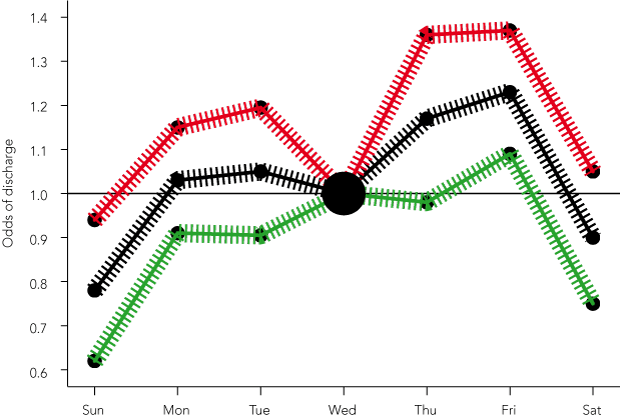
The odds of being discharged by day of the week are shown in the Box. The odds of being discharged alive were significantly lower on Sunday and significantly higher on Friday (the 95% posterior interval for these 2 days does not include 1).
- Adrian G Barnett1
- Nicholas Graves1
- Ben S Cooper2
- Rahul Batra3
- Jonathan D Edgeworth3
- 1 Institute of Health and Biomedical Innovation, Queensland University of Technology, Brisbane, QLD.
- 2 Statistics, Modelling, and Bioinformatics Department, Centre for Infections, Health Protection Agency, London, UK.
- 3 Guy’s and St Thomas’ National Health Service Foundation Trust, London, UK.
None identified.





Abstract
Objective: To estimate the effect of day of the week on the odds of being discharged alive from an intensive care unit (ICU).
Design: A longitudinal analysis of risk of discharge by day of the week.
Setting and patients: 4569 patients admitted to the ICU of St Thomas’ Hospital, London, from 2002 to 2006.
Results: The odds of being discharged alive were lowest on the weekend and literally climbed during the week.
Conclusion: Our results show a frightening pattern of discharge from an ICU ward, most likely caused by a complex web of specialist availability and patient demand.